It is suggested to perform a sperm DFI assay in addition to routine tests in evaluating male fertility (
17). The association between lifestyle factors and the DFI has been widely reported (
14). The authors of the present study believed that if a strong link was confirmed between these factors and sperm DFI, public health strategies could be made to prevent and eliminate these habits among the general population; therefore, this study was conducted to evaluate these potential risk factors.
In the current study, the mean age of patients was 37.45 ± 5.99 years, and 73.4% of patients were younger than 35 years. Previous studies have shown a mean age ranging from 27.83 to 46.6 years among male partners of couples suffering from infertility (
18,
19). The discrepancy observed in the mean age of infertile men from different regions can be justified by differences in genetic and environmental factors between populations. In some areas, low health insurance coverage can also play a role as it might make it financially infeasible for some individuals, particularly younger couples, to seek fertility care. Traditionally, aging is believed to play a principal role in diminishing sperm quality. Different factors, such as the degeneration of the urogenital tract, a decrease in the number of Leydig cells, and more exposure to exogenous toxicants, can contribute to lower semen quality in older men (
20).
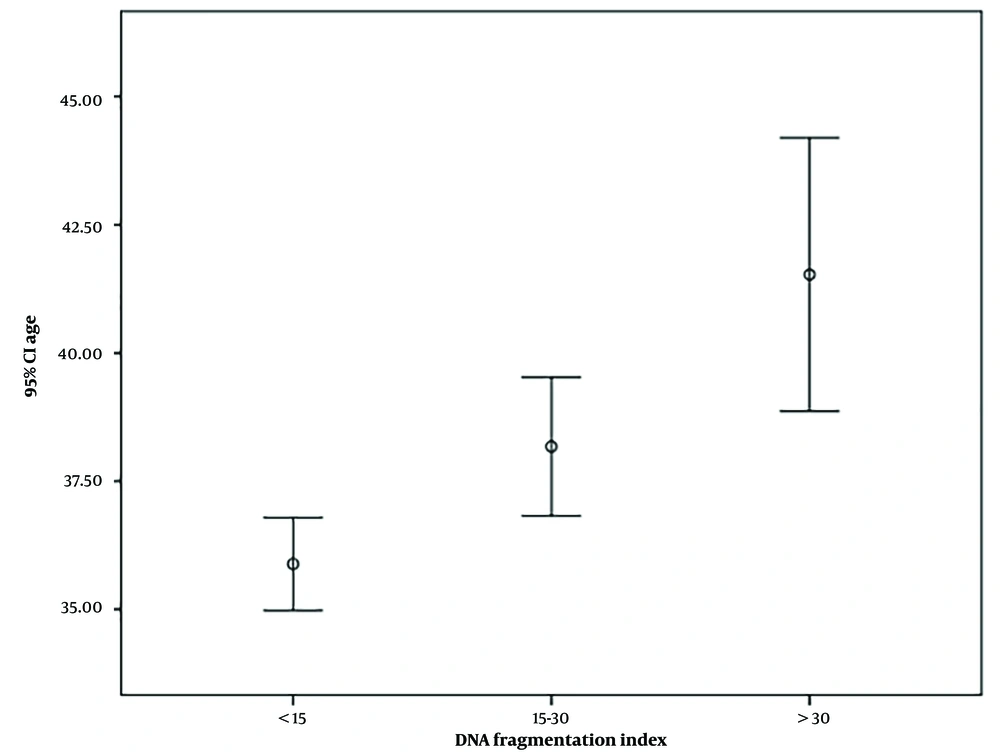
In the current study, 15.3% of the subjects had a DFI of more than 30%. Al Omrani et al. reported that 13.83% of infertile men had high DFI in the Saudi population (
21). The present study demonstrated a significant difference between the mean age in the three studied groups. The group with a higher mean age had a higher DFI. Radwan et al. showed that the age category of older than 40 years was correlated with a higher DFI (
11). The underlying causes of sperm DNA impairment in older men are unclear. However, some mechanisms, such as oxidative stress and impaired sperm chromatin packaging, have been suggested (
22). Oxidative stress associated with paternal aging results in inflammation and endocrine dysfunction and subsequently hinders spermatogenesis (
20).
In the present study, 51.8% of the patients had a normal BMI. The mean BMI was 27.01 in an analysis performed by Ajayi et al. Additionally, they reported lower semen volume, sperm count, and motility in obese men than those with normal weight (
23). The current study’s results showed no significant relationship between BMI and DFI in the studied population. Bandel et al. performed a cross-sectional study on 1503 men in the general population. They did not confirm a positive relationship between high BMI and sperm DNA damage (
14). On the other hand, Kort et al. showed a positive relationship between BMI and DFI; as the subjects’ BMI increased beyond 25 kg/m
2, the DFI also rose (
24).
In the present study, no noticeable relationship was observed between smoking and DFI. Sepaniak et al. showed that smokers had a significantly higher DFI than non-smokers (32% versus 25.9%) (
25). This finding is inconsistent with the findings of the current study and a study performed by Radwan et al., where they showed no association between smoking and sperm DNA damage (
11).
In the current study, there was no considerable correlation between alcohol consumption and DFI. Similarly, Rios et al. demonstrated no relationship between increased sperm DFI and alcohol use in a study on 147 infertile men (
26). In addition, Shi et al. showed that the alcohol drinking index was not significantly correlated with any of the evaluated sperm parameters in their study (
15). The aforementioned results differ from the results of Komiya et al.’s study. They concluded that in those with chronic alcohol use, sperm DFI is higher than in nondrinkers (
27).
Based on the present study’s results, age is the only demographic variable that affects male fertility, and lifestyle factors might not have an influential role in the occurrence of infertility. Therefore, theoretically, lifestyle modification might not be effective in the prevention or treatment of male infertility. At the clinical level, the findings of the present study insinuate the potential benefits of the DFI measurement in the evaluation of infertile men aged over 35 years.
5.1. Limitations
This study has specific strengths, including evaluating both unmodifiable factors (i.e., age) and modifiable factors (i.e., BMI, smoking, and alcohol consumption) in a relatively large sample size. At the same time, most similar studies studied fewer variables or had smaller sample sizes. However, there were also some limitations to this study. The first one is the couples’ reluctance to participate, particularly men denying infertility due to cultural misconceptions. Furthermore, as many infertile couples had been referred to various practitioners before participating in this study, it was challenging to convince them to give a detailed history over again.
5.2. Conclusions
There was no significant relationship between lifestyle factors and DFI. However, large-scale studies are required to evaluate the role of these factors, as if their role in infertility is proven, lifestyle modification might be a potential method for managing infertility.