1. Background
Urolithiasis stands as one of the most prevalent urological disorders, with percutaneous nephrolithotomy (PCNL) emerging as the standard treatment for renal stones larger than 2cm. Consequently, PCNL ranks among the most frequently performed urological procedures. In the United States, the cost of each PCNL procedure (1)ranges from 9000 to 16000 USD, significantly impacting the healthcare system's finances (2).In Iran, while PCNL costs comparatively less, concerns over healthcare bed occupancy persist, potentially compromising healthcare outcomes (3, 4). Recent studies have linked higher bed occupancy rates with increased mortality, even in developed countries (5). Therefore, adopting ambulatory PCNL practices could enhance patient outcomes and reduce mortality rates, irrespective of cost reduction concerns.
Post-surgical complications of PCNL, including bleeding, sepsis, surgical site injury, loss of kidney function, urinoma, and urinary leakage, necessitate careful post-surgical management, often requiring prolonged hospitalization (6, 7). However, advancements in surgical techniques have contributed to a decline in PCNL complication rates in recent years. Consequently, ambulatory PCNL may be viable for selected patients with reduced risk of complications and stable post-surgical conditions (8-10).
Ambulatory PCNL was initially described by Preminger et al. Moreover, amidst the COVID-19 pandemic, hospital space constraints have necessitated prioritizing patient discharge post-surgery (11). In this context, outpatient PCNL with same-day discharge could be considered for selected patients meeting strict criteria (10)
Recent studies have demonstrated that patients in stable post-surgical conditions, characterized by appropriate blood creatinine levels, urine volume, absence of urinary leakage, and normal post-operative physical examinations, can be discharged on the same day as surgery without significant changes in surgical outcomes or complication rates (10, 12)Notably, most studies on ambulatory PCNL have been conducted in developed countries.
2. Objectives
This study aims to evaluate the safety and efficacy of outpatient PCNL in a developing country setting.
3. Methods
The prospective cohort study received approval from the Iran University of Medical Sciences ethics committee (IR.IUMS.FMD.REC.1401.294). The study and control groups comprised urolithiasis patients selected from a pool of 142 individuals who underwent PCNL by a single surgeon (BS) at Firoozgar Hospital between June 2022 and March 2023. Among the 142 patients, 32 met the study's inclusion criteria and exhibited suitable post-operative conditions for discharge. All 32 patients were briefed on the study criteria and informed about the risks and benefits of same-day discharge. They were assured that non-participation would not affect their treatment. Consent was obtained from all 32 patients who volunteered to participate. Subsequently, all 32 patients were discharged within 12 hours post-PCNL without an overnight hospital stay, constituting the ambulatory PCNL group. To compare surgical outcomes and complications, a control group of 32 patients who did not undergo same-day discharge (with a post-operative observation period of 48 hours) was randomly selected from the remaining 110 patients presenting to Firoozgar Hospital during the same period.
Pre-operative imaging was conducted using non-contrast abdominal and pelvic computed tomography for all patients. Prior to surgery, patients underwent laboratory evaluations, including urine analyses (UA), urine culture (UC), complete blood count (CBC) with differential, blood urea nitrogen (BUN), serum creatinine, serum sodium (Na), serum potassium (K), prothrombin time (PT), partial thromboplastin time (PTT), and international normalized ratio (INR).
3.1. Inclusion and Exclusion Criteria
Patients over 18 years old planning to undergo PCNL for renal stones larger than 2 cm (1.5 cm in lower-pole stones), multiple renal stones, or kidney stones resistant to extracorporeal shock wave lithotripsy (ESWL) were included if they met the study criteria. Exclusion criteria encompassed patients with coagulation disorders (e.g., low platelet count, abnormal PT, PTT, and INR), abnormal renal anatomy, renal failure, active urinary tract infection (positive UC two weeks before surgery, or evidence of infection in urine analysis), single kidney patients, high-risk anesthesia candidates, and those with any abnormal pre-operative laboratory test results.
3.2. Surgical Technique and Post-operative Considerations
Prophylactic antibiotics, specifically 3rd generation cephalosporin (ceftriaxone 1 g), were administered to all patients before the operation. As outlined in our recent study, all patients underwent general anesthesia. Subsequently, patients were positioned in lithotomy, and a cystoscope inserted a 4-Fr or 5-Fr ureteral catheter. Surgery was conducted under fluoroscopy guidance using a rigid 24-Fr nephroscope and a pneumatic lithotripter. The primary technique employed was the tubeless approach. However, in cases where double J stents or nephrostomy were necessary, they were inserted (13)
Hemoglobin (Hb), serum creatinine, sodium, and potassium levels were reassessed six hours post-surgery. Ureteral and Foley catheters were removed within 6 to 12 hours post-surgery.
Patients in the study group were discharged if they exhibited normal post-operative laboratory results, were catheter-free for 6 to 12 hours after surgery, and did not require overnight hospitalization. Patients with double J stents were scheduled for clinic visits 14 days after discharge for stent removal. Following PCNL, vital signs, physical examinations, level of consciousness, food and fluid tolerance, and pain levels were evaluated. Patients were permitted same-day discharge if they demonstrated stable vital signs, adequate food and fluid tolerance, mobility, and normal post-operative laboratory findings. All patients were assured of suitable home care conditions and access to medical facilities. Conversely, patients in the control group were discharged two days post-PCNL after Foley and ureteral catheter removal.
3.3. Post-operative Exclusion Criteria
Post-operative exclusion criteria comprised patients with more than one renal access, complications such as urinary leakage from the nephrostomy site, necessitating red blood cell transfusion intra or post-surgery, a Hb drop exceeding two mg/dL within 6 hours post-surgery, fever (axillary temperature ≥ 37.6°C), hematuria, urosepsis, surgical site damage, abnormal chest x-ray (e.g., pneumothorax) in cases of upper calyx access, and those lacking suitable discharge conditions including loss of consciousness, uncontrolled pain with nonsteroidal anti-inflammatory drugs (NSAIDs), food and liquid intolerance, inadequate access to emergency care, and abnormal gait. Such patients were not discharged and were excluded from the study.
All 64 patients underwent follow-up assessments, including ultrasound, kidney-ureter-bladder X-ray (KUB), CBC, and serum creatinine level measurements 14 days post-surgery.
3.4. Statistics
Statistical Package for the Social Sciences (SPSS) software version 22 was utilized for data analysis. Quantitative variables were presented as mean and standard deviation (SD), while qualitative variables were expressed as frequency and percentage. The normality of quantitative data was assessed using the Kolmogorov-Smirnov test. For normally distributed data, the means were compared using independent sample t-tests and ANOVA tests, while non-normally distributed data were analyzed using the Mann-Whitney U and Kruskal-Wallis H (one-way ANOVA) tests. Qualitative data were compared using the chi-square and Fisher's exact tests. A P-value < 0.05 was considered statistically significant.
4. Results
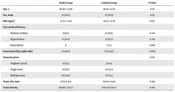
A total of 64 patients were included in the study. The mean age was 46.68 (SD: 11.45), with a mean body mass index (BMI) of 28.39 (SD: 6.26). Of the total, 36 out of 64 (56.3 %) patients were male, while the remaining 28 were female. Multiple stones were present in 45.3% of cases, with 37.5% having pelvis stones and 4.7% having calyx renal stones. Additionally, 7.8% had staghorn calculi. The mean stone size was 32.81 mm (SD: 11.96), with renal stones located on the left side in 40 patients (62.5%). A history of hypertension was reported in 35.9% of patients, and 14.1% had diabetes mellitus. Furthermore, 21.9% had undergone prior ESWL, and 9.4% had a history of PCNL. Thirty-two patients were assigned to the study group, while the remaining 32 comprised the control group. There were no significant differences in patient characteristics, including age (P-value = 0.771), BMI (P-value = 0.141), gender (P-value = 0.131), surgical history (P-value = 0.406), and medical history between the two groups. Moreover, stone laterality (P-value = 0.606), location (P-value = 0.731), size (P-value = 0.334), and density (P-value = 0.065) did not significantly differ between the study and control groups. Eight patients in the study group and ten in the control group had double J stents placed, with no statistically significant difference observed (P-value = 0.232) (Table 1).
| Study Group | Control Group | P-Value | |
|---|---|---|---|
| Age, y | 46.06 ± 11.40 | 46.91 ± 11.67 | 0.771 |
| Sex, male | 21 (65.6) | 15 (46.9) | 0.131 |
| BMI, kg/m2 | 27.25 ± 5.59 | 29.53 ± 6.76 | 0.147 |
| Past medical history | |||
| Diabetes mellites | 3 (9.4) | 6 (18.8) | 0.474 |
| Hypertension | 11 (34.4) | 12 (37.5) | 0.794 |
| Renal failure | 0 | 1 (3.1) | 1.000 |
| Stone laterality (right side) | 13 (40.6) | 11 (34.40) | 0.606 |
| Stone location | 0.731 | ||
| Staghorn calculi | 4 (12.5) | 3 (9.4) | |
| Single stone | 9 (28.1) | 12 (37.5) | |
| Multiple stone | 19 (59.4) | 17 (53.1) | |
| Stone size, mm | 33.30 ± 9.71 | 32.29 ± 14.14 | 0.334 |
| Stone density | 519.00 ± 137.57 | 856.54 ±278.41 | 0.065 |
Patients’ Characteristics a
The post-surgical observation period in the study group (7.88 hours) was significantly shorter than that in the control group (62 hours) (P-value < 0.001). As illustrated in Table 2, the stone-free rate, transfusion requirement, and perioperative complications did not show significant differences between the two groups. Likewise, there was no significant variation in the need for re-admission.
| Study Group | Control Group | P-Value | |
|---|---|---|---|
| Hospitalization time | 7.88 ± 1.33 | 62.00 ± 39.35 | < 0.001 |
| Access site | 1.000 | ||
| Superior calyx | 3 (9.4) | 4 (12.5) | |
| Middle calyx | 5 (15.6) | 5 (15.6) | |
| Inferior calyx | 24 (75) | 21 (65.6) | |
| Stone free rate, % | 84.4 | 87.5 | 1.000 |
| Transfusion | 0 | 1 (3.1) | 1.000 |
| Re-admission | 3 (9.3) | 4 (12.5) b | 0.113 |
| Double J placement | 8 (25.0) | 10 (31.2) | 0.232 |
| Mean hemoglobin change, mg/dL | 1.48 | 1.31 | 0.482 |
| Mean creatinine change, mg/dL | 0.13 | 0.23 | 0.096 |
Peri-operative Data a
Changes between pre-operative and post-operative laboratory test results were analyzed. The mean Hb level change was 1.48 mg/dL (SD: ± 1.02) in the study group and 1.31 mg/dL (SD: ± 0.91) in the control group. Additionally, the creatinine change was 0.13 ± 0.04 in the study group and 0.23 ± 0.03 in the control group. Three patients from the study group were re-admitted to the emergency department due to post-surgical complications. One patient had an axillary temperature of 38.1°C and was admitted for 48 hours while being prescribed Ciprofloxacin for fever. The second patient required placement of a Double J stent due to surgical site urinary leakage, but the issue was resolved after 24 hours of observation without intervention. The third patient experienced pain and was discharged after receiving Paracetamol.
Furthermore, four patients from the control group required an observation period of more than 48 hours due to peri-operative complications. One patient developed sepsis and remained admitted for eight days, while another experienced colon damage and underwent four days of conservative management. A third patient was prescribed Ciprofloxacin for urinary tract infection and discharged after three days, and the fourth patient required two additional days of conservative management for surgical site urinary leakage before being discharged following Double J stent placement.
5. Discussion
The present study demonstrates that PCNL can be safely performed in outpatient settings without increasing the rate of perioperative complications. However, conducting PCNL in an outpatient setting can significantly reduce hospital stay durations and costs.
In 1986, Preminger et al. first introduced ambulatory PCNL in a cohort of 10 young patients with stones measuring less than 1.5 cm (11). Subsequently, with advancements in surgical techniques and decreased complications, ambulatory PCNL became more common. In 2023, Thakker et al. reported the largest population of ambulatory PCNL in the United States, with a study group comprising 53 patients (10). However, in their study, the percentage of mini PCNL surgeries was significantly higher in the study group than in the control group, which could have influenced the results. Schoenfeld et al. included 54 patients who underwent ambulatory PCNL and compared them with a control group matched for age, gender distribution, and BMI. They reported better surgical outcomes, including fewer residual stones and re-admissions (14). Hosier et al. included high-risk patients (age > 75 years and BMI > 30) but reported similar surgical outcomes and complications compared to the control group (12). El-Tabey et al. employed a tubeless technique and Double J stent insertion. They reported that ambulatory PCNL was performed in approximately 72% of cases, with a stone-free rate of about 91% and a mean postoperative pain score of 4.4 on the visual analog scale (VAS) (15). Beiko et al. documented 50 cases of ambulatory PCNL with a mean hospital stay of only 208 minutes and 12% of patients requiring emergency department visits within seven days (16).
The selection criteria are among the most critical considerations when performing PCNL in an outpatient setting. Thakker et al. suggested inclusion criteria such as appropriate levels of consciousness, adequate pain control, tolerance to intake, and baseline mobility while excluding patients exhibiting post-surgical signs of hemorrhage and sepsis (10). Singh et al. included patients with an American Society of Anesthesiologists (ASA) score of 1, minimal stone burden (< 2 cm), short procedure duration, and stone location in the middle or inferior calyx (17). Schoenfeld et al. outlined discharge protocols in their study, including ambulation, liquid tolerance, and one episode of self-voiding (14). Shahrour and Andonian did not discharge patients with an ASA score ≥ 3, single or transplanted kidney patients, patients with encrusted stents, or those lacking appropriate home support. Additionally, they did not discharge patients requiring more than three punctures to obtain access, multiple tracts, or second-look nephroscopy. Their post-operative exclusion criteria included inadequate pain control (18). As mentioned previously, patients with coagulation disorders, abnormal renal anatomy or function, active urinary tract infection, and any abnormal pre-operative laboratory test were excluded from the study. Patients experiencing perioperative complications, requiring red-packed cell transfusion, or exhibiting more than a two mg/dL drop in Hb during the six hours after surgery were also excluded. Those lacking suitable discharge conditions, such as loss of consciousness, uncontrolled pain with NSAIDs, intolerance to liquids and food intake, or abnormal gait, were not discharged and were excluded from the study. Performing PCNL in an outpatient setting necessitates precise and stringent patient selection criteria. However, factors related to the patient's home care, such as family support and convenient access to medical centers, should also be considered (18). Based on the present study's inclusion criteria, only 32 out of 142 (22.53%) patients who underwent PCNL could be discharged.
Based on the findings of the present study, patients in the standard group experienced more significant complications because, in cases of perioperative complications, patients were not allowed to be discharged on the same day.
In developed countries such as the United States, performing feasible procedures in an ambulatory setting can significantly reduce costs. However, cost reduction is not the only advantage of ambulatory PCNL. In a developing country such as Iran, performing PCNL in an outpatient setting does not significantly alter expenditures due to low treatment costs. Nevertheless, hospital admission capacity is limited. Furthermore, increased bed occupancy can directly raise the mortality rate and impact patient outcomes. Thus, performing PCNL in an ambulatory setting can enhance hospital capacity, ultimately improving patient outcomes.
The present study has several limitations. The study population is limited. Therefore, further studies with larger populations are required to determine the precise criteria for ambulatory PCNL. Nonetheless, the present study has both pre and post-operative inclusion and exclusion criteria.
5.1. Conclusions
PCNL can be performed in ambulatory settings in patients with accurate pre-operative risk assessments and can significantly reduce costs without altering surgical outcomes and complications. Further studies with larger populations are needed to assess the optimal hospital stay duration based on the patient's status.