1. Introduction
The majority of the tumors arisen from the epididymis, are benign. Malignant epididymal lesions are rare, accounting for 0.03% of all male cancers. Both primary and metastatic cancers of the epididymis are rare (1). Epididymal metastatic carcinoma has been extremely rare and to the best of our knowledge only 13 cases have been reported (1-13). There has been just one reported case of cholangiocarcinoma metastatic to the epididymis and ours will be the second reported case.
Therefore, in this case report, we will describe our experience with a case of metastatic cholangiocarcinoma to the epididymis.
2. Case Presentation
A 36-year-old man presented with chief complaint of right scrotal swelling and tenderness. Physical examination showed an emaciated middle-aged gentleman with jaundice. His pulse rate, blood pressure, respiratory rate and temperature were normal. His laboratory findings were as below:
ALT (alanine aminotransferase) = 120 IU/L, AST (aspartate aminotransferase) = 100 IU/L, Alkaline phosphatase: 150 IU/L, Bilirubin = 8.5 mg/dL (Total), direct bilirubin = 2.2 mg/dL and lactate dehydrogenase (LDH) was normal.
Complete blood count (CBC) showed mild anemia, otherwise was normal. Tumor markers including HCG (human chorionic gonadotropin), and AFP (alpha fetoprotein) were negative. CA19-9 was elevated, 130 U/mL (normal = 37 U/mL).
All the imaging studies including chest and abdominopelvic CT scans were normal.
Testicular examination revealed right scrotal swelling and tenderness. In physical examination, a right testicular mass was palpated.
Past medical history revealed history of liver transplant 2 years prior to current admission with the diagnosis of hilar cholangiocarcinoma (stage I). The patient refused to receive any type of chemotherapy. Also, a year after liver transplantation, he developed a mass in mesocolon which had been operated on and showed metastatic cholangiocarcinoma.
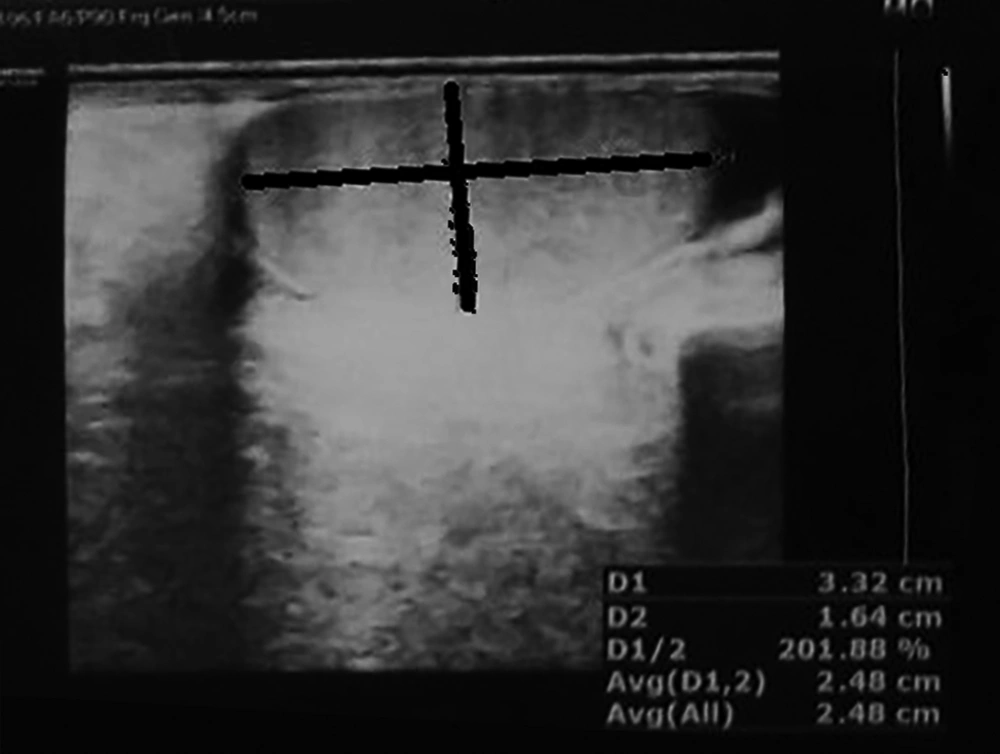
Ultrasonography of the testis showed a hypoechoic mass in upper pole of the right testis (Figure 1).
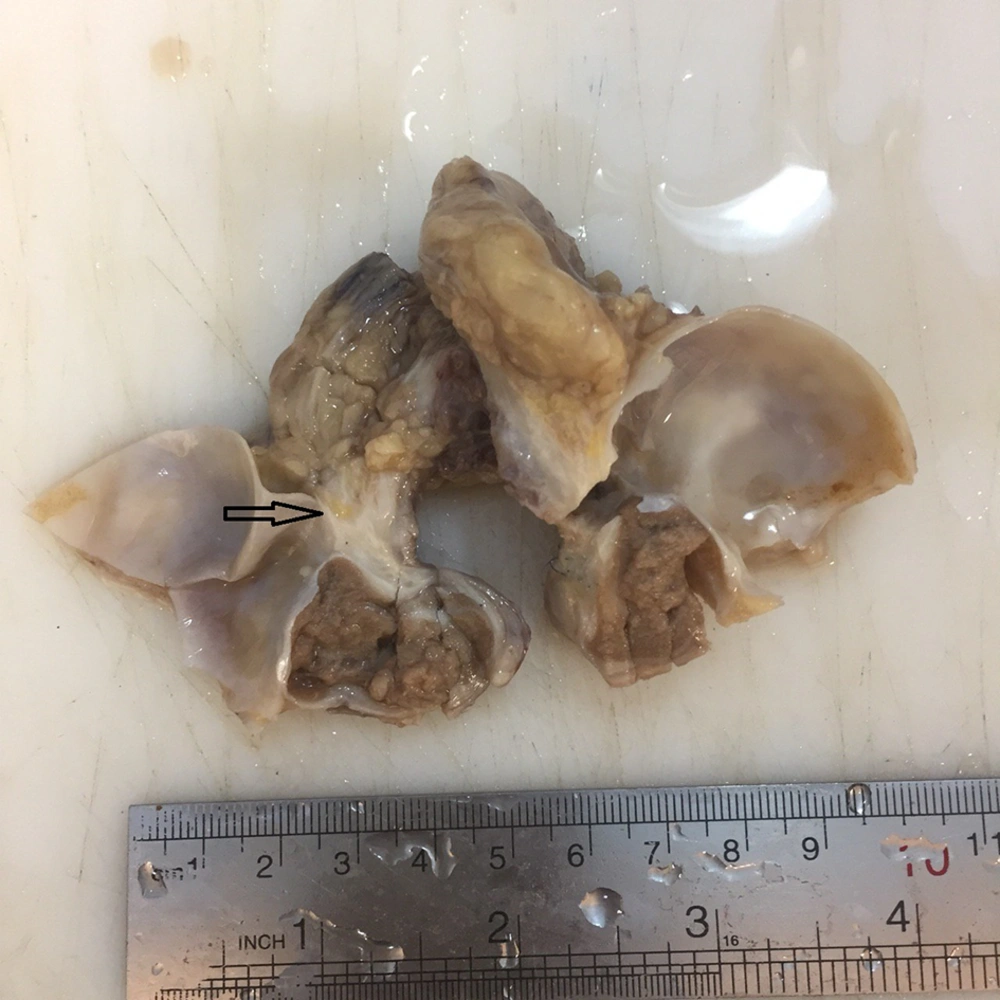
The patient underwent orchiectomy and the right testis and epididymis were removed. Figure 2 shows the gross pathology of the orchiectomy specimen, the arrow shows the tumor in the epididymis.
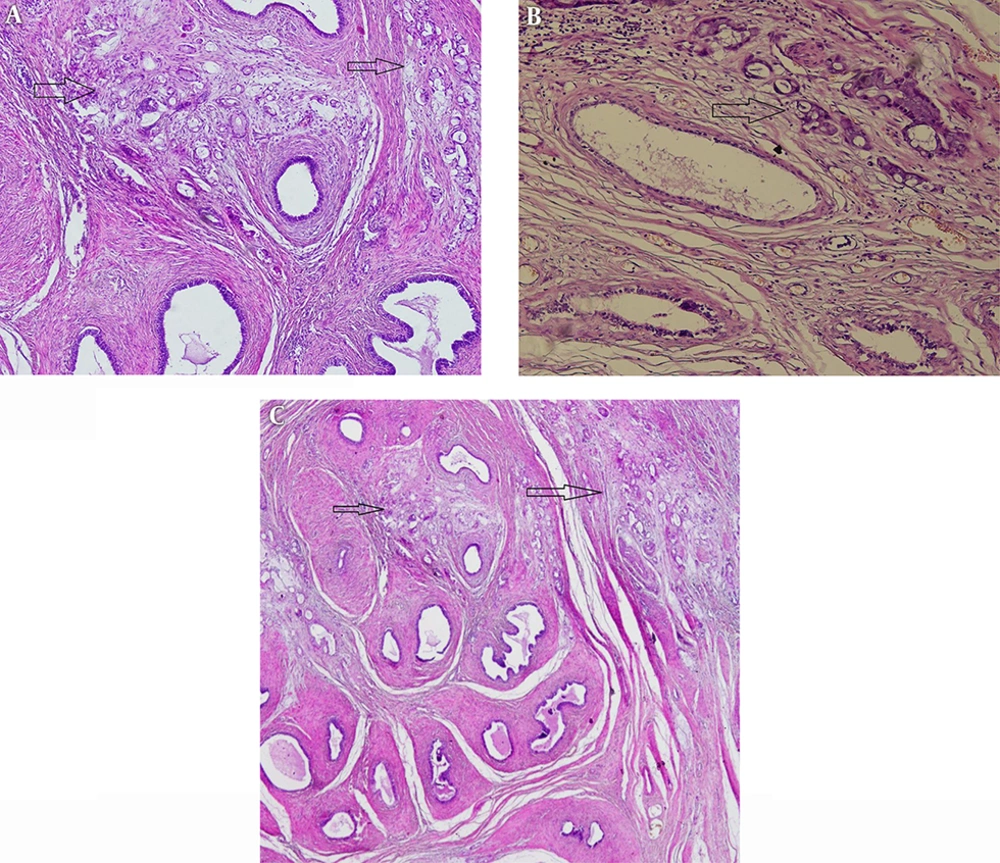
Histopathologic sections from the testis and epididymis showed adenocarcinoma within the epididymis (Figure 3A - B). The histopathology was compatible with metastatic cholangiocarcinoma and exactly the same histopathologic picture as the previous tumor in the liver. The diagnosis of metastatic epididymal cholangiocarcinoma was made, however the patient refused to be treated by chemotherapy. Now after 3 months he is still alive and doing relatively well.
3. Discussion
Benign and malignant tumors of the epididymis are very rare. More than 94% of the tumors in epididymis are benign and malignant tumors are very rare. Metastatic carcinomas to epididymis have been extremely rare (14). Table 1 shows the details of the 13 previously reported cases of metastasis to the epididymis as well as the current case. The age range of the reported cases have been 50 - 77 years (65.7 ± 10.3). Our case is the youngest reported case (36 years of age). There has not been any preference for the right and left epididymis. In 5 cases metastases have been to the left epididymis, right in 4 cases and it has been bilateral in 3 cases. In our case, the tumor has been in the right epididymis. In one of the previous cases, the side of the metastasis has not been reported (1-13).
| First Author | Year | Primary Origin of the Tumor | Age, y | Greatest Diameter of Epididymal Tumor, cm | Side of the Involvement | Presenting Sign and Symptom | Duration of Disease Before Epididymis Metastasis, y | Other Metastases | Outcome |
|---|---|---|---|---|---|---|---|---|---|
| Anastasiadis (1) | 1998 | Prostate | 73 | 4 | Right | Lower back pain | 8 | Colon | Alive after 13 months |
| Ozdal (2) | 2002 | Stomach | 55 | 1 | Left | Painless testicular swelling | Simultaneously | - | NR* |
| Gaskin (3) | 2003 | Prostate | 65 | NR* | Bilateral | NR* | NR* | - | NR* |
| Heman-Ackah (4) | 2004 | Prostate | 77 | 0.9 | Left | Scrotal mass | 4 | - | NR* |
| Moreno Anton (5) | 2005 | Colon | 74 | 2.2 | Right | Tenderness | 1 | Testis and spermatic cord | NR* |
| Xu (6) | 2013 | Stomach | 50 | NR* | Bilateral | Urinary symptoms | 4 | Testis and spermatic cord | NR* |
| Serfling (7) | 2016 | Prostate | 73 | NR* | NR* | Asymptomatic (high PSA) | 4 | - | Well and alive |
| Zhang (8) | 2016 | Prostate | 69 | NR* | Right | Tenderness | 5 | - | Well after 24 months |
| Bennett (9) | 2017 | Cholangiocarcinoma | 72 | 4 | Right | Tenderness and mass | Simultaneously | - | Died |
| Mittal (10) | 2017 | Prostate | 75 | NR* | Bilateral | Lower Urinary tract infection | Simultaneously | Bone | NR* |
| Agarwal (11) | 2018 | Jejunum | NR* | 5 | Left | Scrotal mass | Simultaneously | Liver and peritoneum | Alive |
| Di Franco (12) | 2018 | Pancreas | 70 | 2 | Left | Scrotal mass | Simultaneously | - | Alive |
| Santos-Lopes (13) | 2019 | Prostate | 69 | 1.8 | Left | Asymptomatic (high PSA) | 5 | - | Alive |
| Current case | Cholangiocarcinoma | 36 | 6 | Right | Scrotal swelling | 2 | Meso-colon | Alive |
All of the metastatic carcinomas to the epididymis were small (less than 5 cm). In five cases, the size has not been reported. In the remainder, the size has been 0.9 - 4 cm (2.73 ± 1.4) (1-13). Our case has been the largest reported case with 6 cm diameter.
Clinical presentation of epididymal metastatic tumors have been nonspecific. In 2 patients, metastasis from prostate has been incidentally found by investigation of the source of high PSA (prostatic specific antigen) (7, 13). In other patients the presenting symptoms have been scrotal mass, swelling, and tenderness (2, 4, 5, 7-9, 11). Other more uncommon signs and symptoms have been urinary tract infection (6, 9) and low back pain (1).
In 5 patients epididymal metastasis had been detected at the same time of the diagnosis of the primary cancer (2, 9-11, 13). In others, this interval between the diagnosis of the primary tumor and the epididymal metastasis had been between one to 8 years (2.6 ± 2.4). Our case was detected 2 years after liver transplant and resection of the cholangiocarcinoma.
The most common primary carcinoma metastatic to epididymis has been prostate in 7 cases (40%) (1, 3, 4, 7, 8, 10, 13). Other less common primary tumors have been stomach in 2 cases (2, 6), and colon (5), jejunum (13), pancreas (12) and cholangiocarcinoma (9) each in one patient.
As the table shows, in the last 20 years, only one case of metastatic cholangiocarcinoma to the epididymis has been reported (9) and our patient is the second case.
In most of the previous cases, the primary method of diagnosis has been clinical, which was confirmed by pathologic diagnosis. In a few patients, tumor markers have been helpful especially PSA in prostate adenocarcinoma (7, 13). However, in a few cases, imaging studies have been the primary method of diagnosis. Radiologic methods were ultrasonography (US), computed tomography scan (CT scan), magnetic resonance imaging (MRI) and even PET (positron emission tomography) scans (7). US findings had been reported as a homogenous, well-defined and hypoechoic mass (1, 11, 14). CT scan of epididymal metastasis revealed a solid mass (1). MRI had shown a heterogeneous nodule, with arterial vascularization (5). In the majority of the cases there has been no definite diagnosis by radiology, so orchiectomy had been performed (13). Needle biopsy has also been performed in cases with primary presentation of epididymal tumor and no prior diagnosis such as a reported case of metastatic gastric cancer which was primarily diagnosed based on histologic features of metastasis in the epididymis (2).
For confirming the metastatic nature of a carcinoma in the epididymis, history of primary tumor, comparison of the histologic features of the primary and metastatic cancer have been very important and immunohistochemistry has been reported to help confirming the primary origin, such as PSA for prostatic cancer. However, no specific marker has been reported in primary cancers of epididymis (15).
As a conclusion, metastatic carcinoma to the epididymis is a very rare event, and metastatic cholangiocarcinoma is extremely rare.