1. Introduction
Crush injuries of upper extremity always disable patients and might involve many organs such as finger arm hand or might involve all of them together.
Mangling injuries effect daily activities of patients; such injuries may also affect the family members of the patients (1).
Priorities in treating mangling injuries include treating the life threatening injuries, preserving the injured limb and restoring of its function (2).
The life threatening injuries in other parts of body such as hands, neck, or abdomen can be cured. Then the wound excision skeletal fixation tendon, neurovascular reconstruction and soft tissue coverage are made for limb (3-5); crushed intrinsic muscle should be debrided to prevent contracture. Routinely repairing both the flexor digitorum sublimis and flexor digitorum profundus is made unless gliding is comprised of case repairing only flexor digitorum profondus is done (6). If primary repair is not possible, two-stage reconstruction by tendon rod is done. For soft tissue, the coverage of joint, tendon, bone and neurovascular with local flap, regional flap, distant flap or free tissue transfer should be considered (7-9).
2. Case Presentation
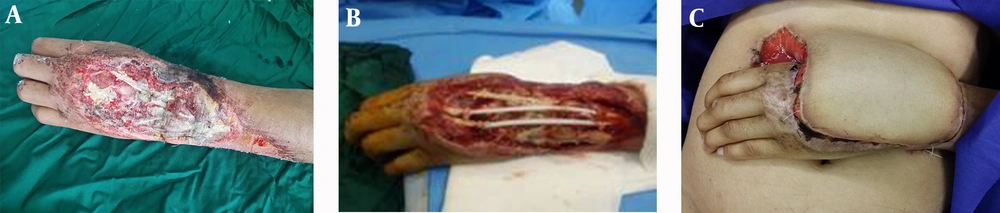
Here is the case of a 37-year-old female with crushed hands injury in dorsal hand due to accident. In primary evaluation, she had no life threatening injury; in the past medical history, she had allergic asthma and hyperthyroidism (Figure 1A).
In the physical exam, there was a soft tissue defect in dorsal hand. She could not extend the left 3rd, 4th and 5th fingers. Distal pulse and capillary refill were normal. There was no bone injury; there were extensor tendons defect about 6 cm length and soft tissue defect about 6 - 12 cm. The wound was dirty and full of debris. After serial irrigation and debridement of necrotic tissue and foreign body, the injection of antibiotic and tetanus prophylaxis, the patient was scheduled for flap. There are two options to reconstruct extensor tendons: covering soft tissue alone and postponing tendon reconstruction, extensor tendon reconstruction with silicon rod and soft tissue coverage concurrently (10).
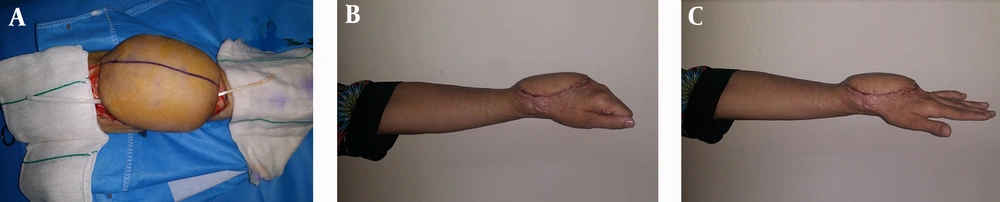
Although the latter method had a few proponents, the second method was employed. Therefore, silicon rod was inserted for extensor tendons and then random pattern abdominal flap was inserted (Figure 1B and 1C); three weeks later the pedicle of flap was separated and three months later silicon rods were removed. Therefore, extensor tendons with palmaris longus and plantaris tendon graft were reconstructed (Figure 2A). Silicon produces pseudosheet around flexor sheet to prevent subsequent adhesion.
3. Discussion
There are many options such as regional flap, distant flap or free flap to cover the dorsal hand soft tissue. Some of them need microsurgery skills and take a long time (11-14). Regional forearm flap causes extensive scar in the donor site.
It was not accepted by the patient, and on the other hand regional forearm flap is used for small soft tissue defect (15). Totally, there was a concern about risk of infection due to silicon rod in acute setting; the second method was employed to lessen several surgeries and avoid adhesion.
Advantages of this method are: no need to microsurgery skills, no need to long time operations, no need to extensive scars in upper limb and prevention of extra operation for extensor reconstruction. Disadvantages of this method are: possibility of infection, possibility of need to debulking.
The first stage for debulking was made three months later, a half of flap was debulked and then three months later the other half was debulked again.
Finally, the patient could extend her fingers and gradually, the range of motion increased (Figure 2B, 2C).