Materials and Methods
Four replants were carried out in three patients during 6 months. All patients were building worker. The oldest of them was 54 years.
The first patient was building worker. He was 35 years old. His finger stuck in elevator and just a narrow skin strip was connected in dorsal area. The strip was sectioned by surgeon before the beginning of finger replantation. Debridement skin was shortened. Patient had smoking background.
It took 9 h from the time when trauma induced till the beginning of replantation operation and the finger was roughly dressed. Replantation was carried out in metacarpophalangeal joint. There were two skin incisions in the dorsal area of finger. The same area slightly bled after replantation till 24 h.
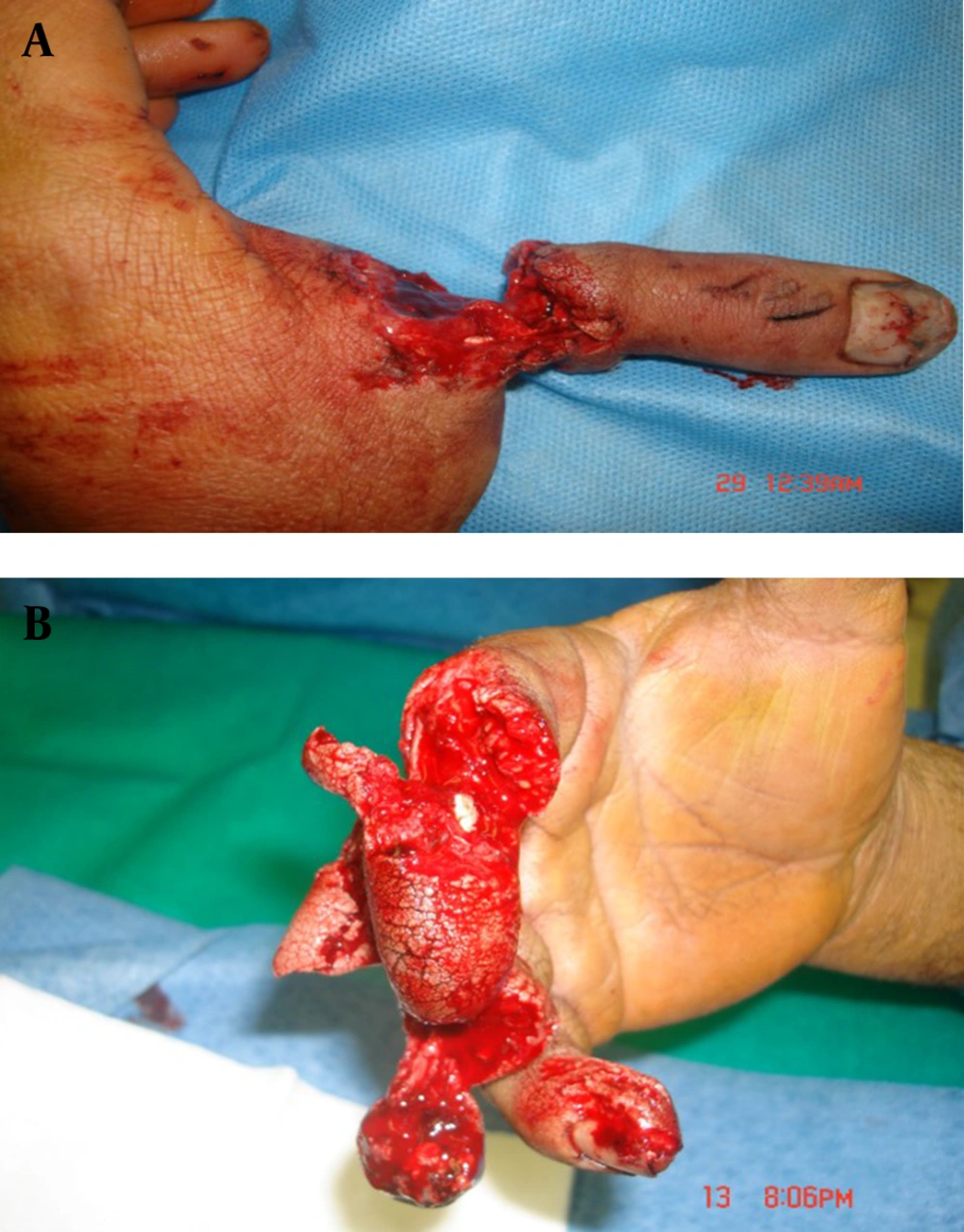
The second patient was a wood worker. He had 2-4 serious injuries as the result of sectioned ting wood. The third finger could not been replanted due to serious injury (Fig. 1). After suitable debridement, the stump was sutured. The second and fourth fingers were replanted.
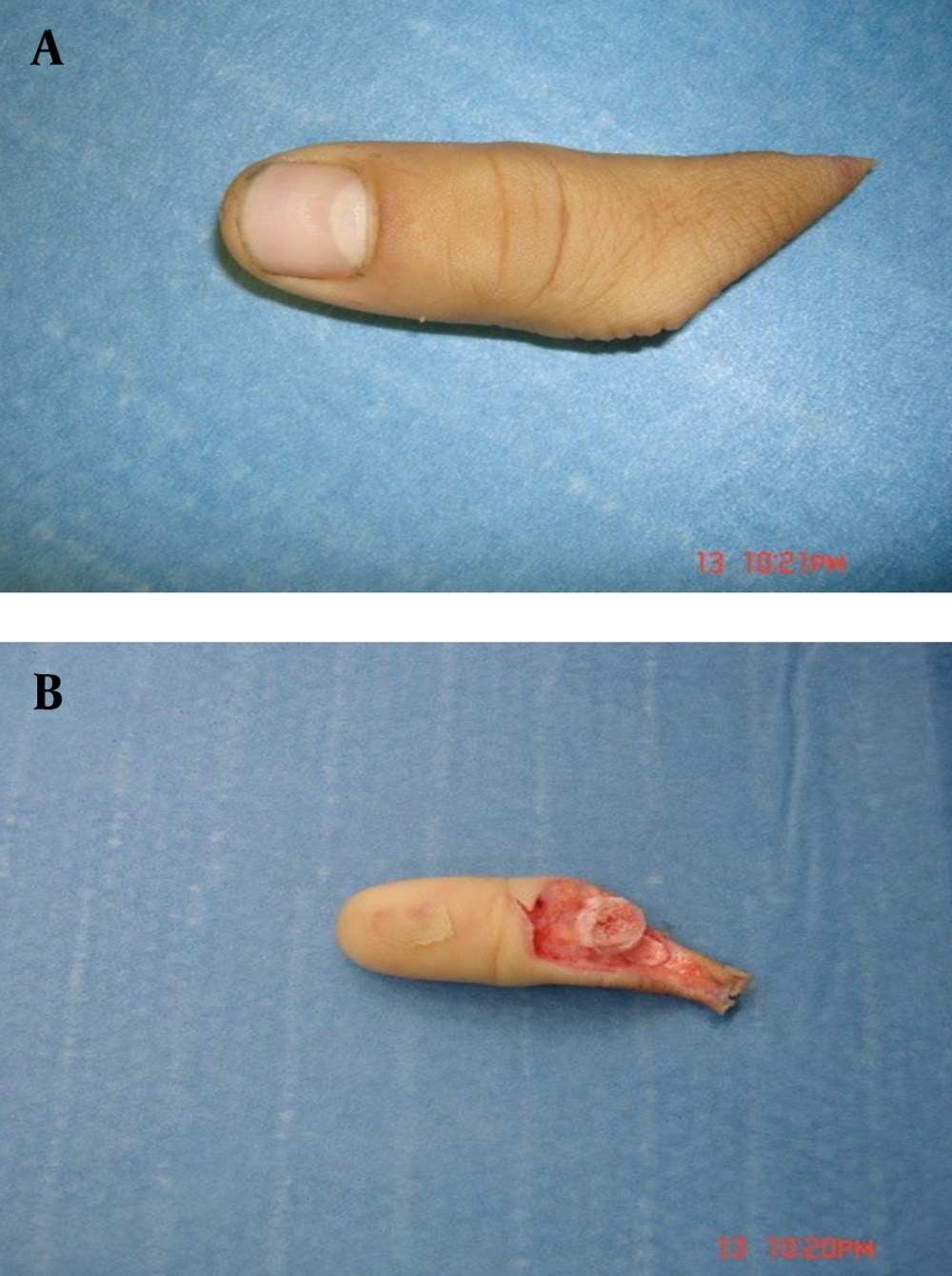
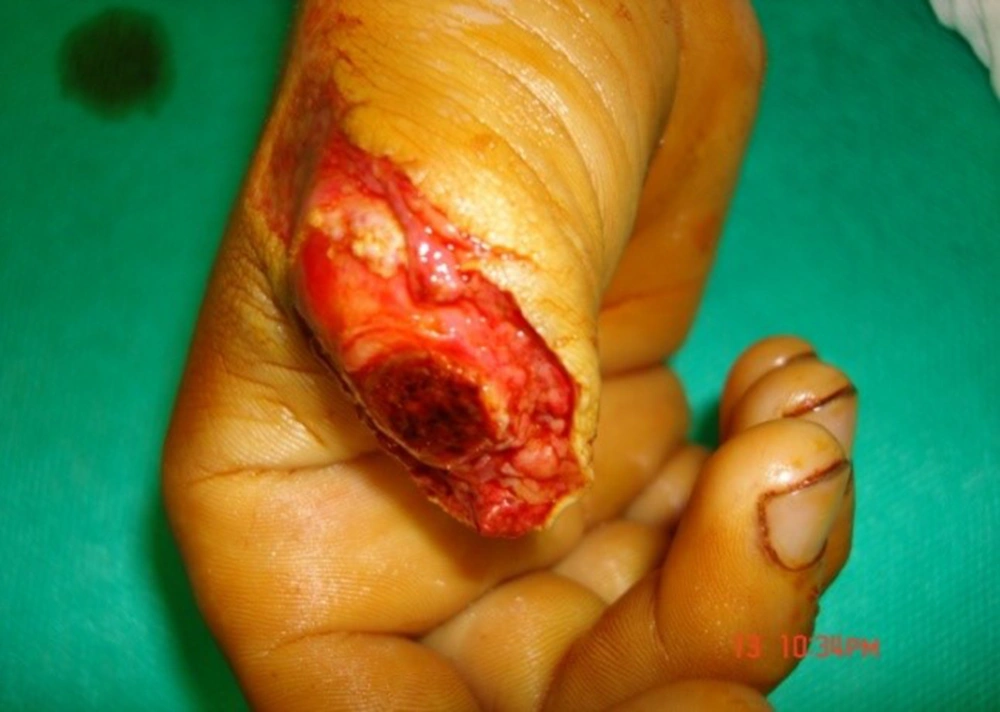
The third patient was carpenter worker. He was 27 years old. His thumb was obliquely sectioned from proximal to interphalangeal joint in right hand. There was deep injury in thumb cartilage. It bled till two days after replantation. The patient had smoked 10 cigarettes a day for 10 years, before admission (Fig. 2 and 3).
Since in all surgeries, patients were hospitalized in other center than the primary place, it took 7 h between the induction of trauma and the beginning of replant. Amputation was carried out in thumb (in two patients) and the second, third and fourth fingers (in one patient). Concerning the patient’s condition, the second and fourth fingers were replanted.
In the present report, we incorporated two maneuvers to avoid extra incisions in the dorsal skin of distal fragment and to find dorsal veins: in early step, we employed moderate pressure in soft tissues on the surface and velar of thumb. Then, we made attempt to find dorsal vein by bleeding toward the end of vein amputated fragment (magnification=12×). In all three cases, this action was successful. In the fourth case, the abovementioned maneuver failed. After arterial anastomosis and the establishment of blood flow in distal fragment, we found dorsal veins by controlling the finger’s dorsal level in bleeding area. Then, we softly separated dorsal vein from surrounding tissues and delivered to surgical wound. Replantation operation was carried out under anesthesia. Before entering the patient into operation room, work was done on amputated fragment. In this step, no extra incision was employed. Bilateral digital artery was separated from digital neuron and surrounding tissues till reaching intact intima (delivery).
Bilateral artery and bilateral neuron were respectively marked by 10-0 and 9-0 nylon string. In the next step, we employed mild pressure on the soft and velar tissue and found the slight blood drainage of vein 2 of dorsal vein. Then, we marked it by 10-0 nylon string. Since we intended to not to induce any extra incisions in dorsal area, we postponed vein desection from surrounding tissues to the step after osteosynthesis.
In this step, patient was transferred to operation room. Proximal stamp was probed under anesthesia and tourniquet control (100 mmHg over patient’s systolic pressure and maximum up to 300 mmHg). Then, deep flexor tendon, bilateral digital artery, two dorsal veins, and bilateral digital neuron were found and marked separately. Osteosynthesis was done using KW (Kirshner Wire) No. 0.35 inch. Digital artery was discontinuously anastomosed by 10-0 nylon string under double microvascular clamp with 12× magnification.
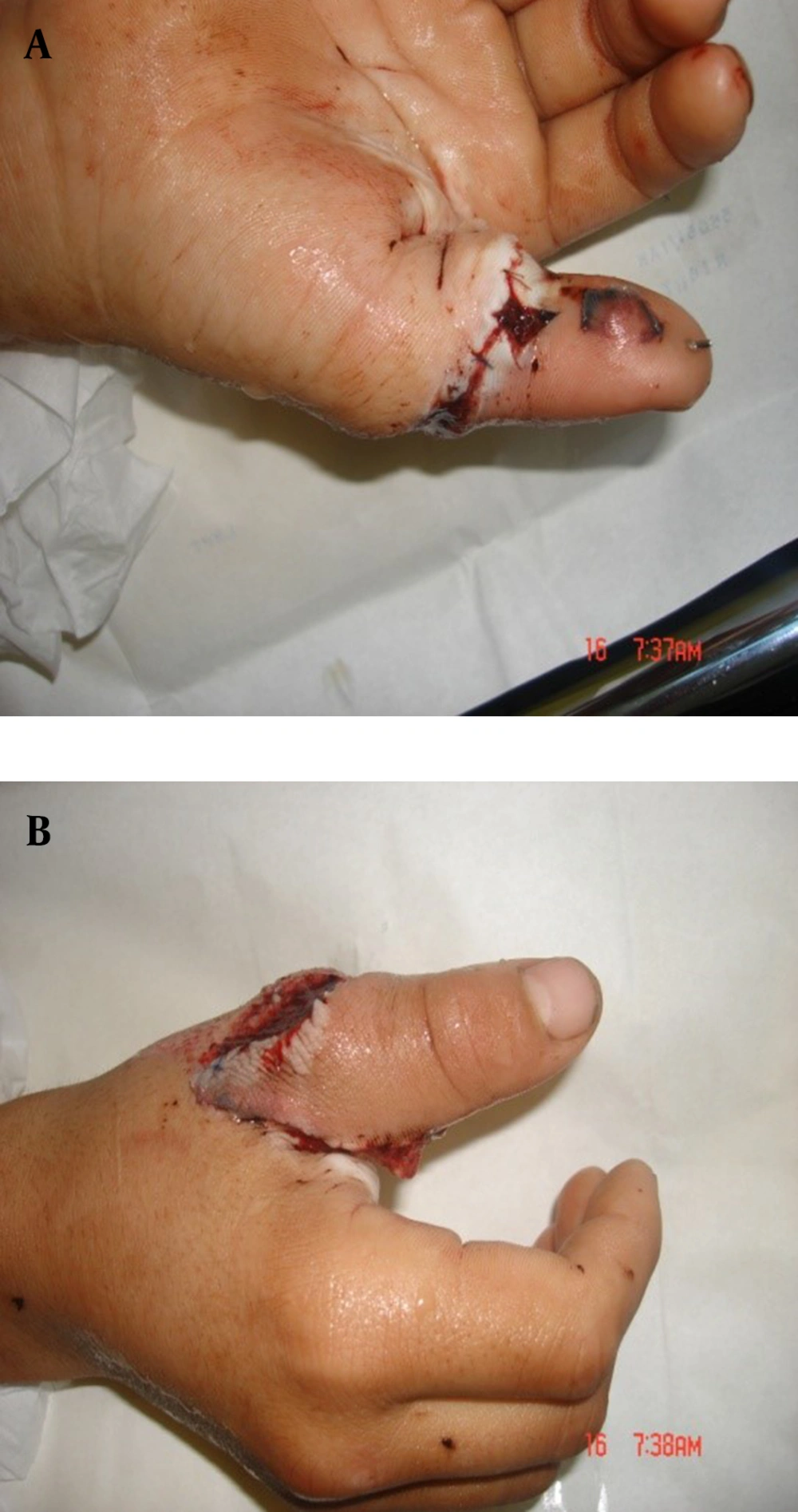
In the end, the arterial anastomosis of vascular clamp was opened. In case of distal bleeding, the openness of anastomosis was approved. In none of the cases, arterial anastomosis revision was required. In anastomosis, surgery area and two ends of artery were rinsed drop by drop using heparin (1000 unit in 100 mL) by means of syringe and iota No. 28. In one case, due to the artery spasm, we put cotton saturated by papaverine on the area of artery anastomosis. Then, we tended to restore deep flexor tendon and extensor system. Dorsal veins’ anastomosis was done exactly the same as arterial one. During the anastamosis of the first vein, vascular blood flow kept on via the second vein. In the end, distal blood flow was controlled for 15 min while the area of surgery was coated by cotton saturated by warm papaverine. Skin was restored by 4-0 nylon string. Dorsal splint was placed above elbow and in zero degree wrist flexion. A trained nurse controlled the openness of anastomosis in ward using oximetry pulse. After 48 h from surgery, the wound was undressed and rinsed by warm saline. The patients were dismissed by splint. He had on-patient visits till 15 days later (Fig. 4). The patient was recommended to absolutely avoid smoking. Next visits were in the third and sixth weeks after surgery. From the sixth week on, physiotherapy was begun by removing KW.
Results
In all three cases replantation was successfully done. The dressing change was done by attending surgeon and on a regular basis every other day. Twelve hours after replantation in case one there was a mild bleeding which was controlled by gently applying adrenalin moisture fine mesh gauze. Suture removal was planned in day 14 and splint removed 4 weeks after the operation. Active physiotherapy was scheduled in 4 courses each was 10 consecutive days. The full course of therapy was 4 months.
Discussion
Although the replantation of amputated limb is a normal and accepted surgery, it has still its own specific technical precision and sensitivity. The only absolute ban of this surgery is the patient’s adverse condition. That is, he cannot stand long complicated surgery [1]. Mean surgery time in our patients was 5.5 h for each finger. The amputated finger must be placed in a container of ice (no direct touch) after being cleansed by cotton saturated with saline and being placed in a plastic sterile bag. This can be replanted up to 56 h later [6, 7]. The tolerance time of warm ischemia is shorter in most proximal fragments of the limb. Although digital artery anastomosis is the key step of replant success, the main problem is related to ability to make vascular drainage [8-10]. Vein narrow wall enhances its susceptibility, in one hand, and it is permanently in collapse mode during anastomosis. It brings about further technical challenges. There are reports where semi-distal replantation of distal phalanx is successfully done by the anastomosis of one artery yet no vein anastomosis (in this case, suitable vein is not found for anastomosis) using leech replantation [11].
Another problem with vascular system is that no exact anatomic status is defined for dorsal veins. In dorsal area, we deal with a vascular network. Hence, dissection, detection, and separation of vein is considerably more difficult than artery. As a result, during the delivery of tissues to find suitable vein, harms or iatrogenic of vascular network is probable. The same damages can be highly risky. This is because, after the establishment of blood flow, they can lead to blood drainage and hematoma and pressure on the susceptible anastomosis of vascular system. Blood drainage of finger dorsal veins can be stopped by the least pressure. It is inevitable due to the vascular congestion of replantation failure. Based on several reports, the most prevalent cause of replantation failure is vascular congestion after surgery [12].
The main difference between our patients and the normal method of finger replantation is that no extra incisions were done to search for thumb artery and vein. Regarding the matter that the location of the artery and vein is completely defined, the searching step was not required for all patients. Omitting more incisions means imposing lower risk to veins which must be anastamosed by microsurgery technique and it is considered to be an advantage. Yet, since it limits surgeon’s access to veins’ stump, naturally the surgery will become longer and need the surgeon’s further patience. However, vascular anastomosis was done with further accuracy and longer time yet no extra incisions and flapping for dorsal veins exposure. Little blood drainage around the area of anastomosis means the presence of platelets. These platelets can result in the failure of replantation due to the vasoactive amines they release. These vasoactive amines are capable of contracting veins and can reverse the replantation. That is why the accurate homeostasis of wound in the end of replantation surgery is emphasized [1]. The number of patients reported is small. Nevertheless, this surgical method will be continued regarding repletion in finger due to the group’s positive response to this technique regarding the survival of replantation.