1. Background
2. Objectives
3. Methods
3.1. Drugs
3.2. Cells and Cell Culture
3.3. MTT Test
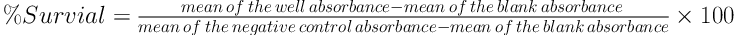
Zahedan Journal of Research in Medical Sciences
Image Credit:
There are many strategies to cure cancer, therefore, many drugs have been evaluated in this field. Albendazole (ABZ), derivative of benzimidazole, has a wide range of anti human and animal worm effects. The anti tumor effect of ABZ in both animal and human clinical trials has been reported.
In the present study, the cytotoxic effect of ABZ on breast cancer cell lines, MDA-MB-231 and MCF7, and on the melanoma cell line, B16F10, were evaluated with MTT assay for the first time.
Different doses of ABZ for two breast cancer cell lines and the melanoma cell line were investigated. ANOVA was employed to analyze the data. Mean comparisons were carried out by Dunnett’s test in SPSS (version 18.0) statistical software.
The results showed that ABZ (0.1, 1, 10, 100µM) significantly reduced the viability of MCF7, the percent of declines to different concentrations of ABZ, 0.1, 1, 10, and 100 µM, were 15, 32, 38, and 44 accordingly, indicating enhancement ABZ toxicity effect towards its rising concentration (P value ≤ 0.001). However, significant toxicity effect of ABZ on the MDA-MB-231 was only apparent at concentration of 100 µM with approximately 27% reduction in viability (P value ≤ 0.05). In addition, this effect on B16F10 in all ABZ concentration levels was significant, resulting in 34%, 18%, and 27% reduction in cell viability for ABZ concentrations 100, 10, and 1µM accordingly, indicating the higher impact at the first and third concentrations than second concentration (P value ≤ 0.001).
According to the cytotoxic effects of ABZ on breast cancer and melanoma cells, it can be used as a promising adjuvant along with other chemotherapy drugs.
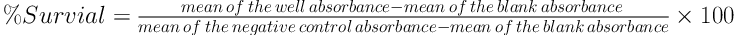
Copyright © 2018, Zahedan Journal of Research in Medical Sciences. This is an open-access article distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/) which permits copy and redistribute the material just in noncommercial usages, provided the original work is properly cited
Purchasing Reprints
Author(s):