1. Background
Control of pain after open-heart surgery in patients in the intensive care unit (ICU) is a major concern of healthcare providers. Pain is a subjective and personal experience that affects most body systems and can result in prolonged hospital stays (1-3). Many procedures performed by nurses in the ICU, such as patient repositioning, catheter and drain removal, endotracheal suctioning, and wound care, have been identified as painful for patients. However, verbal communication is altered in patients with endotracheal intubation or a reduced level of consciousness due to sedative or paralyzing drugs; therefore, pain assessment in such situations is crucial and difficult (4, 5).
For adequate pain assessment and proper treatment in intubated or unconscious patients, some valid observable behavioral scales and physiological indicators, such as the Critical-care pain observation tool (CPOT), are used (6). The CPOT is a feasible, easy-to-complete, and simple-to-understand tool that includes an evaluation of four different behaviors (facial expressions, body movements, muscle tension, and compliance with the ventilator for mechanically ventilated patients or vocalization for non-intubated patients) (7). However, in some situations, such as when the patient is receiving high doses of sedative drugs or neuromuscular blockers, the use of CPOT is less valuable due to inhibition of motor function (8).
Another criterion used to assess pain in ICU patients is vital signs. Although vital signs are easily accessible in the ICU, their validity for pain assessment is not strongly confirmed. Moreover, vital signs are not recommended indicators for pain assessment in nonverbal patients, based on the American society for pain management nursing (ASPMN) guidelines (9). Also, administration of various drugs, such as beta-blockers, calcium-channel blockers, and other drugs that affect blood pressure and heart rate (HR), can modulate the cardiovascular response to pain.
On the other hand, because there is a significant relationship between pain and the sensory system, the cortical arousal response is a known pain indicator. BIS monitoring is used for this purpose as a potential tool for the detection of pain (10, 11). BIS is a non-invasive technology with the main purpose of quantifying changes in the brain’s electrophysiological state during sedation and anesthesia by measuring different indices, including the BIS value, electromyographic (EMG) activity, electroencephalographic (EEG) data, and the density spectral array (DSA) (6).
2. Objectives
The aim of this study was to evaluate BIS for pain assessment in sedated and mechanically ventilated adult ICU patients after cardiac surgery. The CPOT and vital signs, such as mean arterial pressure (MAP) and HR, were assessed during painful procedures, then compared with each other and with BIS.
3. Materials and Methods
Seventy consecutive patients who underwent cardiac surgery (coronary artery bypass graft or valvular surgery) and were admitted to the intensive care unit at Rajaie cardiovascular medical and research center (Tehran, Iran) from April to October 2015 were enrolled in the study.
The inclusion criteria were age > 18 years, inability to use verbal communication due to an endotracheal tube, having undergone coronary artery bypass surgery or valve replacement/repair via median sternotomy, a sedation-agitation scale (SAS) (12) score of 2 or 3, and no history of neurological disease or drug abuse. The exclusion criteria were the use of narcotics, sedatives, or neuromuscular relaxants after surgery during the study period, cardiac arrest and CPR in the operating room or ICU, ischemic or hemorrhagic neurological events, encephalopathy, and prolonged intubation time (> 8 hours).
This study was approved by the local ethics committee according to the Helsinki declaration of the world medical association (2000). All patients were informed about the study and provided written consent prior to being enrolled. After surgery, all patients were transferred to the ICU with an endotracheal tube. During the first hours after admission to the ICU, when the effects of the anesthetics, neuromuscular relaxants, and opioid drugs used during the operation disappeared but the patients were still intubated and under mechanical ventilation, their pain was assessed.
Pain evaluations using the two different pain tools (BIS and CPOT) were independently performed at the same time. The pain assessments were done three times: 1) at baseline (immediately before any painful procedure, including tracheal suctioning or change in position), 2) during the painful procedure, and 3) five minutes after the procedure (recovery time). All patients were assessed for pain scores by one investigator.
3.1. Bispectral Index (BIS)
BIS was recorded continuously with the portable Bispectral index monitor (Model A-2000 software version 3.20, Aspect Medical System). The BIS uses a sensor (Denmetere A/S Kildemosevej 13, Denmark) that is placed on the patient’s forehead (frontal, left temporal, and left mastoid bone). The sensor sends different signals, including the BIS index score, EMG activity, and electroencephalographic data (EEG). The range of BIS values is from 0 (complete suppression of EEG or coma) to 100 (fully awake) (13).
3.2. Critical-Care Pain Observation Tool (CPOT)
The CPOT has four sections, each containing items scored from 0 to 2 (for a possible total score of 0 - 8). The four sections are facial expressions, body movements, muscle tension, and compliance with the ventilator for intubated patients. The levels of pain intensity based on CPOT scores are: 0 - 2 (no pain or mild pain), 3 - 5 (moderate pain), and 6 - 8 (severe pain) (9).
3.3. Vital Signs
MAP and HR were assessed at baseline and during painful procedures.
3.4. Statistical Analyses
Statistical analyses were performed with SPSS 21.0 for Windows (SPSS Inc., Chicago, IL, USA). All variables were tested for normal distribution with the Kolmogorov-Smirnov test. Repeated-measures ANOVA followed by the Bonferroni post-hoc test was used to assess changes in numerical variables over time. The correlations between pain-assessment-tool scores were assessed by Spearman’s correlation test. P values of ≤ 0.05 were considered statistically significant.
4. Results
The study sample included 70 patients who underwent cardiac surgery; 46 (65.7%) of the patients had coronary artery bypass graft (CABG) surgery and 24 (34.3%) underwent valvular surgery. The mean age of the study population was 56.02 ± 14.2 years; 44 (62.9%) were male and 26 (37.1%) were female.
The mean values of the changes in CPOT, BIS, MAP, and HR at the three times (baseline, during painful stimulation, and at recovery time) are shown in Table 1. The mean CPOT, BIS, and MAP values were significantly changed over time, increasing during suctioning or repositioning, and decreasing at recovery time (five minutes after the procedure) (P < 0.05). Changes in HR were not significant over time (P = 0.34).
| Baseline | During Painful Stimulation | At RECOVERY Time | P Value | |
|---|---|---|---|---|
| CPOT | 0.94 ± 0.52 | 3.98 ± 1.65 | 1.31 ± 1.07 | < 0.001 |
| BIS | 60.78 ± 10.95 | 84.94 ± 10.52 | 63.48 ± 12.17 | < 0.001 |
| MAP, mmHg | 87.65 ± 15.00 | 92.88 ± 15.37 | 89.77 ± 14.72 | 0.003 |
| HR, bpm | 94.04 ± 16.73 | 95.68 ± 16.78 | 93.61 ± 16.56 | 0.346 |
Abbreviations: BIS, bispectral index; CPOT, critical-care pain observation tool; HR, heart rate; MAP, mean arterial pressure.
The correlations between CPOT and BIS with vital signs and other parameters of pain assessment are depicted in Tables 2 - 4. CPOT had a significant positive correlation with BIS at baseline, during painful stimulation, and after recovery time, but it was not correlated with HR and MAP (except at baseline). The BIS scores were significantly correlated with MAP, but not with HR.
| BIS (Baseline) | HR (Baseline) | MAP (Baseline) | ||||
|---|---|---|---|---|---|---|
| r | P Value | r | P Value | r | P Value | |
| CPOT | 0.666 | < 0.001 | -0.015 | 0.902 | 0.268 | 0.025 |
| BIS | - | - | -0.025 | 0.835 | 0.321 | 0.007 |
Abbreviations: BIS, bispectral index; CPOT, critical-care pain observation tool; HR, heart rate; MAP, mean arterial pressure.
| BIS | HR | MAP | ||||
|---|---|---|---|---|---|---|
| r | P Value | r | P Value | r | P Value | |
| CPOT | 0.612 | < 0.001 | -0.190 | 0.116 | 0.211 | 0.080 |
| BIS | - | - | -0.025 | 0.835 | 0.321 | 0.007 |
Abbreviations: BIS, bispectral index; CPOT, critical-care pain observation tool; HR, heart rate; MAP, mean arterial pressure.
| BIS (Recovery Time) | HR (Recovery Time) | MAP (Recovery Time) | ||||
|---|---|---|---|---|---|---|
| r | P Value | r | P Value | r | P Value | |
| CPOT | 0.738 | < 0.001 | -0.122 | 0.1314 | 0.211 | 0.079 |
| BIS | - | - | 0.0175 | 0.147 | 0.231 | 0.054 |
Abbreviations: BIS, bispectral index; CPOT, critical-care pain observation tool; HR, heart rate; MAP, mean arterial pressure.
5. Discussion
The BIS index and CPOT scores were found to be higher during painful procedures. CPOT, BIS, and MAP were significantly correlated at baseline, during painful stimulus, and at recovery time. The BIS index and CPOT scores seemed to be more sensitive indicators of pain than the vital signs, which remained quite stable.
In the current study, CPOT scores peaked during suctioning or repositioning, and declined five minutes after the onset of the painful stimulus. The trends of these changes were significant. These results are quite similar to those obtained in a report by Gelinas et al. (6), who showed that CPOT scores were increased during painful procedures, such as turning and endotracheal suctioning, compared with rest. In another study by the same authors (8), 113 unconscious ICU patients with different diagnoses were evaluated. The average CPOT score during repositioning, with or without endotracheal suctioning, was 2.23.
In our study, the BIS scores were increased during repositioning and endotracheal suctioning compared with baseline. Brocas et al. (14) showed that in patients who had not received analgesia prior to procedures such as suctioning, the BIS scores increased during the painful stimulation and decreased significantly five, 10, and 15 minutes later. They suggested that the BIS variations reflected cortical reactivity to painful intervention in critically-ill sedated and ventilated patients. The BIS index may help to optimize analgesia during invasive events. However, in a study by Li et al. (15), the BIS index was increased during endotracheal suctioning, but remained unchanged three and five minutes after the painful stimulation.
In the current study, the trend of changing MAP values was significant; during the painful situation, MAP was increased, and then began to decline over time. On the other hand, the changes in HR were not significant. This may indicate that vital signs alone cannot be used to assess pain in patients who are unable to express pain. Several studies show that vital signs, including MAP and HR, were increased significantly during painful procedures in conscious or unconscious sedated and ventilated patients (16, 17). However, Gelinas et al. showed that vital signs for pain assessment in ICU patients are not recommended, and that vital signs must be used concomitantly with other valid pain-assessment tools (18). Vital signs are not considered valid indicators for pain assessment because the majority of ICU patients receive sympathetic-system-suppressing drugs, beta blockers, calcium-channel blockers, and angiotensin-converting enzyme inhibitors. These factors can all inhibit the physiological responses to some extent (19, 20).
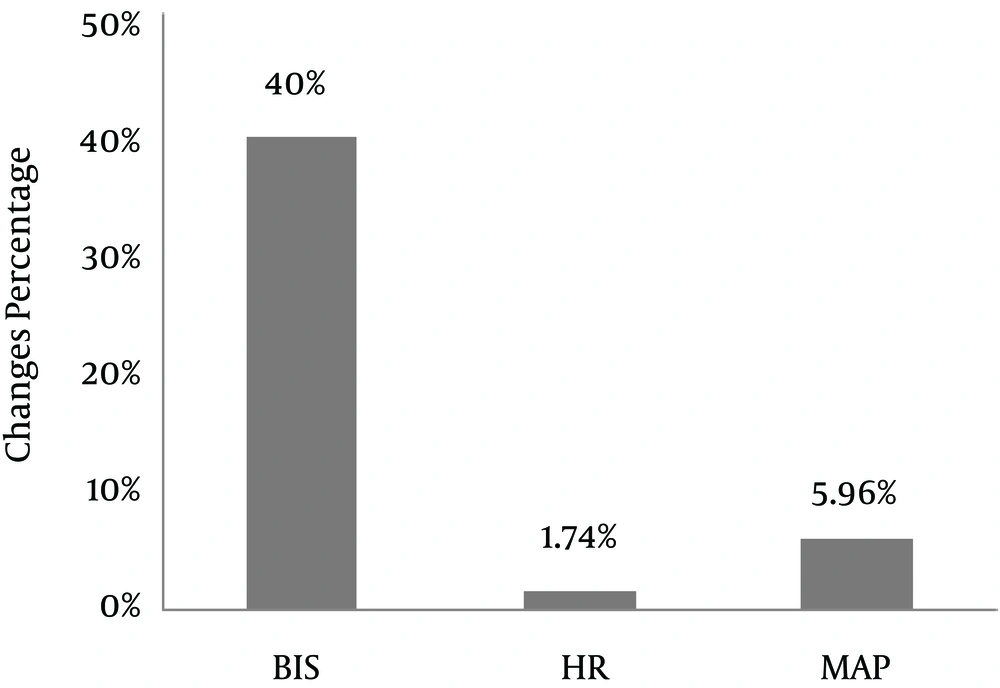
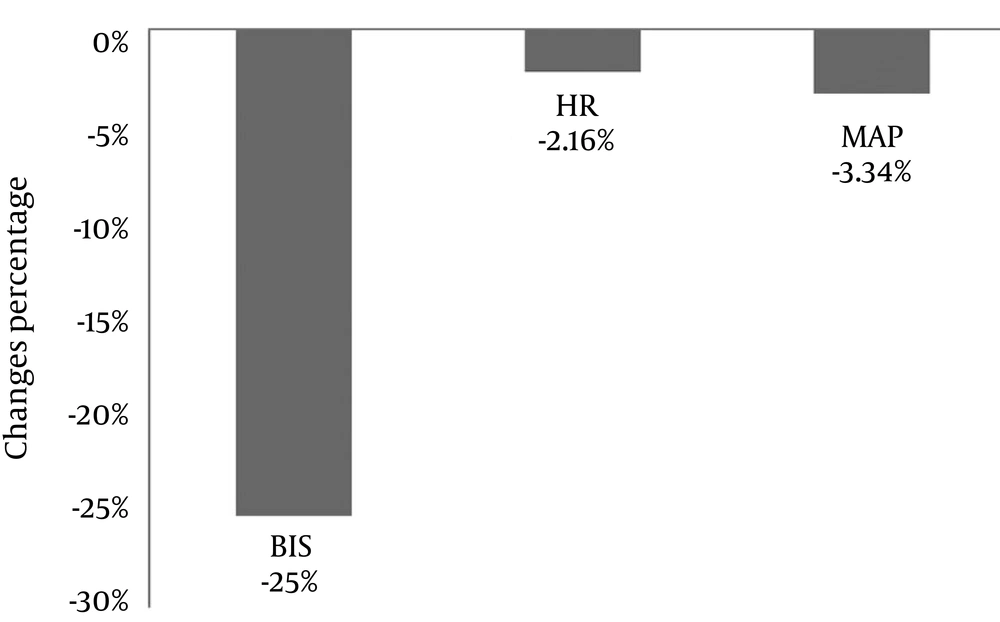
Compared to baseline values, the BIS scores increased more than 39% during patient-turning and endotracheal suctioning, and decreased approximately 25% by the recovery time (Figures 1 and 2). In the study by Li et al. (18), the BIS index increased approximately 10% during painful situations compared to baseline. It should be noted that in that study, all patients received analgesia prior to the procedure, and they were under deep sedation. It is clear that opioids play a significant role in modulating the sensitivity of BIS monitoring (21). Brocas et al. (14) demonstrated that a bolus dose of alfentanil reduced BIS scores in response to painful stimulation, so significant changes in BIS were not seen. Also, in the control group that had not received alfentanil, a significant increase was observed in the BIS scores during the painful stimulation, with an average increase from 60 to 88.
In a study by Gelinas et al. (6), the BIS index increased 20% - 30% and vital signs decreased approximately 10% during turning and endotracheal suctioning. That study concluded that vital signs, in comparison with BIS and CPOT, have a low sensitivity for pain assessment in ill ICU patients. Our findings are also in line with these (Figures 1 and 2).
5.1. Conclusions
According to the results of this study, as pain sensation has an influence on brain arousal status, BIS monitoring can be used for pain assessment along with the CPOT in intubated and sedated patients, and it is much more sensitive than hemodynamic changes. It appears that BIS monitoring can be used more efficiently in patients under deep sedation or those who have received muscle relaxants, in whom the physical symptoms of pain sensation are depressed.