1. Background
The coronavirus (COVID-19) outbreak has changed into a public health crisis that brought huge challenges to people's mental health (1). The first case of COVID-19 was officially identified in Wuhan (China) in late 2019 (2), and by January 24, 2020, it was spread to 13 countries (3). In Iran, the growing trend of the disease was such that 987 people were infected, and 54 died on March 1, 2020 (4). By early April, 50,468 cases were infected and 3,160 died (5). The rapid spread of the COVID-19 outbreak, which have claimed many lives in two months, indicates the power of this virus (6). Restrictions, quarantine, the fear of infection, the depression that people experience as a result of losing friends and family members, and the anxiety of losing loved ones are among the mental challenges of COVID-19 (7). It seems that fear is one of the consequences of mass quarantine (8). According to the literature, there is a significant correlation between the duration of quarantine and post-traumatic stress disorder (PTSD) (9).
The COVID-19 pandemic has created emotional problems and anxiety in the general population, mostly in severely affected countries (10). Indeed, emotional traumas, such as natural disasters, global pandemic diseases, wars, social problems, etc. can cause huge stress disorders (11). There are several studies that support the correlation between the COVID-19 outbreak and mental and emotional problems, especially depression and anxiety (1, 12-14). COVID-19 has led to various psychological problems such as depression (15), violence (16), hysteria (17), suicide (18), emotional distress, and anxiety in the general population (19), even in people who are not at a high risk of infection (17). In Asia, Iran and China are two countries severely affected by COVID-19 (5). This virus has influenced all aspects of human life, with extensive psychological and emotional impacts on human societies. Meanwhile, several consequences will appear in the future.
2. Objectives
This study aimed to investigate the psychological impacts of COVID-19 on the general public's emotional state in Iran.
3. Methods
3.1. Study Design
This study is approved by the Research Committee of the Islamic Azad University (code: 14/11/5/9381). The study was conducted in Iran from March 24-26, when the number of COVID-19 cases increased. Because the Iranian government has asked people to limit face-to-face contacts and stay home since early March, this study used an online survey to assess the impact of COVID-19 on the emotional general public's emotional state in Iran. The respondents were invited to participate in this online survey. A snowball sampling technique focused on the general population in various provinces and cities during the COVID-19 pandemic was used. Initially, the online survey was posted on the university websites and distributed among students. Then, the respondents were asked and encouraged to pass it on to others. Participants completed the online questionnaires in Persian through an online survey platform. All respondents provided their informed consent. Besides, the principles of the Helsinki Declaration were observed in the present study. The collected data were anonymous and remained confidential. Some of the results obtained from this study were presented to students in various workshops.
3.2. Statistical Analyses
Statistical analyses were performed using SPSS version 21.0. To calculate the association between the independent variable, i.e., the impact of COVID-19, and the dependent variable, i.e., emotional states, a linear regression analysis was used.
3.3. Research Tools
The Impact of Event Scale-Revised (IES-R) (Weiss and Marmar, 1997) was used to assess the psychological impact of COVID-19 (20). This scale consists of 22 items and three dimensions. Its dimensions include intrusion (eight items), avoidance (eight items), and hyper-arousal (six items). Hence, the IES-R scale score is formed for three subscales. The total score ranges from 0-23 (normal), 24-32 (low psychological impact), 33-36 (medium psychological impact) to > 37 (severe psychological impact). The cut-off point is ≥ 33, which indicates PTSD. In Iran, the Cronbach’s alpha coefficient of the total scale was 0.83 (21).
The emotional states were measured using the Positive and Negative Affect Schedule (PANAS) (Watson, Clark, and Tellegen, 1988) (22). This schedule is designed in two ten-item mood subscales that consist of both positive and negative effects. The responses are scored based on a six-point Likert-type ranging from one to five. The validity of the positive (α= 0.88) and negative (α =0.87) effects is investigated. In Iran, its internal consistency is reported as 0.87 (23).
4. Results
The data analysis was conducted in both descriptive and inferential levels. In the descriptive level, means, standard deviations, and percentages were used, and in the inferential level, to answer the main research question, the linear regression analysis was applied. A total of 721 citizens from 62 cities in Iran participated in this study, and 293 respondents did not complete the questionnaires. Hence, in total, 428 subjects (284 females and 141 males) completely responded to the questionnaires.
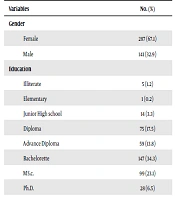
The mean age of participants was 32 years. Most of the participants had a bachelor's degree. Moreover, 249 were married. The average time at home of participants during the COVID-19 outbreak was 21 hours (Table 1). The linear regression analysis showed a significant association between the COVID-19 outbreak and the general public's negative emotional state in Iran (B =0.251, 95% CI: 0.207 to 0.295) (Table 2).
| Variables | No. (%) |
|---|---|
| Gender | |
| Female | 287 (67.1) |
| Male | 141 (32.9) |
| Education | |
| Illiterate | 5 (1.2) |
| Elementary | 1 (0.2) |
| Junior High school | 14 (3.3) |
| Diploma | 75 (17.5) |
| Advance Diploma | 59 (13.8) |
| Bachelorette | 147 (34.3) |
| MS.c. | 99 (23.1) |
| Ph.D. | 28 (6.5) |
| Employment status | |
| Student | 21 (4.9) |
| Unemployed | 15 (3.5) |
| Housewife | 32 (7.5) |
| Retired | 25 (5.8) |
| Employed | 191 (44.6) |
| University Student | 144 (33.6) |
| Marital status | |
| Single | 179 (41.8) |
| Married | 249 (58.2) |
| Age | |
| 10 -19 years | 75 (17.5) |
| 20-29 years | 127 (29.7) |
| 30-39 years | 96 (22.4) |
| 40-49 years | 90 (21) |
| 50-59 years | 27 (6.3) |
| 60 and more years | 13 (3) |
| Staying at home | |
| 0-5 hour | 13 (3.0) |
| 6-10 hour | 17 (4) |
| 11-15 hour | 16 (3.7) |
| 16-19 hour | 37 (8.6) |
| 20-24 hour | 345 (80.5) |
5. Discussion
According to the best knowledge of the authors, this is the first study in Iran that has investigated the psychological impacts of COVID-19 on the general public's emotional state at the peak of the pandemic. The results indicated that the rapid spread of the virus has influenced the general public's emotional state.
A similar study demonstrated that the distress rate among Iranian adults was higher than that in the Chinese population (24). The final impact of the COVID-19 pandemic is still unclear; however, its psychological effects are certain, including worry about getting infected, fear of death, disappointment, job burnout, and negative emotions, all of which affect the physical and emotional health of society (16). Additionally, depression, PTSD, insomnia, anxiety, anger, and even suicide in patients and their families are other psychological consequences of the COVID-19 prevalence (25). In Italy, research showed a high percentage of PTSD symptoms during the COVID-19 pandemic in the community, which resulted in sleep problems (26). Moreover, the COVID-19 outbreak has created huge problems for educational systems all around the world (27). In China, women, compared to men, experience higher levels of PTSD and sleep issues (28). COVID-19 has increased anxiety among many of us, as we know little about it (29), and experts are using sophisticated techniques to control its spread (30). Therefore, psychologists and psychiatrists should look for novel techniques to decrease the impacts of the COVID-19 outbreak. As an instance, during this global crisis, spirituality is useful for staying calm (25). As a result, it can be argued that the COVID-19 outbreak has influenced important aspects of our lives, particularly through negative emotions, so mental health teams should be formed to improve the general public's emotions by providing online or in-person psychological services with complete and updated treatment information and programs.
The current study had strengths, including being an online survey, which facilitates participation. Secondly, the present study was a large-scale research that collected data from all regions of the country at the peak of the pandemic. On the other hand, the researcher could not collect any information from some of the respondents who were not eager to participate in the online survey.