1. Introduction
Eye injuries in military service have a major economic impact each year throughout the lives of members of the armed services. While it costs millions of dollars a year to treat extraordinary eye injuries, it is comparable to the cost of replacing and retraining service members to replace people with vision loss (1).
Contact lens wear is important factor for contagious corneal ulcers in the world (2). Every year, around two million new corneal ulcers grow in Asia and Africa (3). Unless treated when in the acute stage, this clinical disorder is vision-threatening (4). Effective treatment of corneal ulcers is related on the identification of the origin's problem. Nowadays, there are more reports of clinical failures to treat infectious (bacterial) corneal ulcers (5). In this report, a bioresonance-based complementary treatment for corneal ulcers is described in order to determine whether an electromagnetic frequency complements can improve intractable corneal ulcers. They are currently used to treat chronic wounds and have been reported to be an effective treatment for corneal wound healing (6-9).
2. Case Presentation
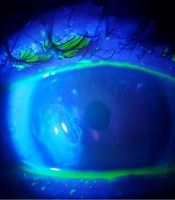
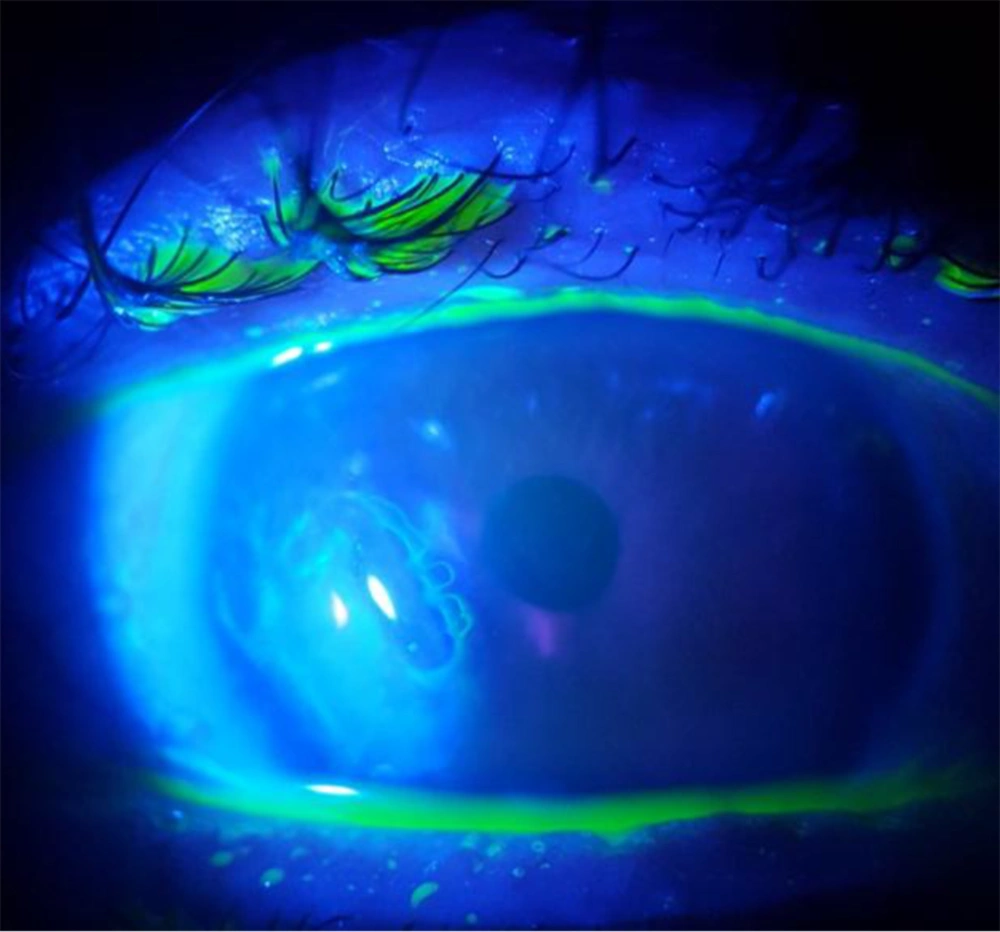
The patient was a 65-year-old man who was referred to an ophthalmologist for cataract treatment. The lens was scratched during the eye operation as a result of a medical error. Following that, the patient experienced a problem with light reflection on vision. His lens was replaced in the second operation, and a corneal ulcer developed. He has a foreign body sensation in one of his eyes, which is accompanied by severe pain and tears. His visual acuity has remained constant. An examination with a slit lamp revealed a central corneal ulcer with diffuse corneal edema (Figure 1).
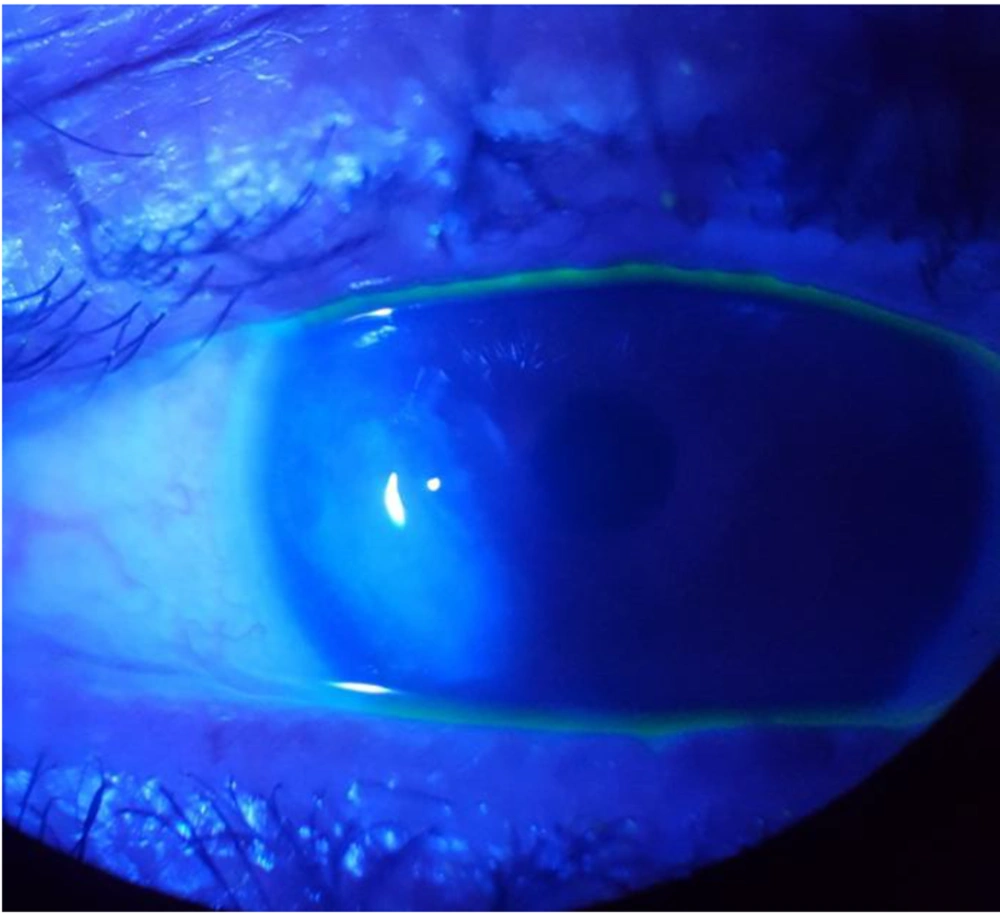
The patient regularly uses sodium chloride and tetracycline eye drops. The wound was burned five times with laser surgery due to a lack of healing; however, there was no significant improvement in the patient's condition. He had never had bacterial keratitis before. He referred to the Bioresonance Center, where he had been treated with electromagnetic frequency (E.M.F) complements for one year. According to the final optician's report, lens bandage was removed also the ulcer is stable without any fluid (Figure 2).
Now, he not only has not worn contact lens for a long time but also has not experienced of severe pain or sensitivity to light in recent weeks.
3. Discussion
Corneal ulcers are frequently caused by a variety of factors, including infective keratitis or trauma. Treatment consists of topical and, in some cases, systemic medications, as well as surgical procedures (10). It has been proposed that EMFs, by changing or augmenting preexisting endogenous electrical fields, may trigger specific, measurable cellular responses such as DNA synthesis, transcription, and protein synthesis (11).
Magnetic therapy with an extremely low-frequency electromagnetic frequency complements is a non-invasive, safe, and simple method for healing injuries from a variety of causes (6). Ghaffarieh et al. discovered that magnetic treatment of corneal chemical burns significantly reduced the ulcerative area when compared to control groups, particularly in the first week of therapy, and that its effectiveness was comparable to medical therapy (12). The success of a single case report is, of course, limited, and it is critical to confirm the current findings with additional findings from additional studies. The authors express their gratitude to the patient for their cooperation and permission to publish the report.