1. Background
Benign prostatic hyperplasia (BPH) affects almost 210 million men worldwide (1, 2); Hence, it is the leading cause of lower urinary tract symptoms (LUTSs) in aging men (2). The prevalence of BPH increases by 70% and 90% in individuals aged 61 - 70 and 81 - 90 years, respectively (3). About 50% of such individuals reveal clinically significant symptoms (4), including micturition, urgent urination, dysuria, and obstruction symptoms such as residual urine and urinary retention (5, 6). In this regard, surgery is the most effective therapy in treating patients with moderate and severe prostatic hyperplasia (6). Studies have recently introduced TURP as a gold standard for the surgical treatment of patients with BPH (7) since more favorable clinical results are achieved for BPH patients (7).
Post-TURP bacteremia and severe sepsis are the side effects in these patients (8). TURP seems to be a clean-contaminated method requiring antibiotic prophylaxis (9). The efficacy of prophylactic antibiotics in these patients has been reported in previous studies (10). The prevalence of post-TURP bacteremia decreases by 1% with antimicrobial prophylaxis (11).
Some patients use a catheter before surgery because of urinary obstruction (11), causing bacteriuria (9). Catheter-related bacteremia may be caused by a broad spectrum of gram-positive and gram-negative bacteria (12). Although antibiotics decrease postoperative bacteremia, bacteriuria, and symptomatic urinary tract infection (13), urinary tract infection is more prevalent in these patients than in patients with no catheter (14).
Recently, various compounds have been used to prevent and treat urinary tract infections (15). Chlorhexidine as a disinfectant and antiseptic component (16) has been applied to treat many post-surgical infections (17). Studies have suggested that the long-term use of chlorhexidine against gram-positive and gram-negative microorganisms, yeast cells, viruses, and mycoplasma is effective (15). It may be beneficial for the prevention of urinary infection following a transurethral operation (18).
A catheter in patients with urinary obstruction undergoing TURP leads to bacteriuria. TURP is performed on patients who have already had bladder colonization with bacteria, increasing the probability of bacteremia and sepsis in spite of consuming prophylaxis antibiotics.
2. Objectives
The present study aimed to evaluate the effect of chlorhexidine 0.2% on pre-TURP bladder washing to reduce postoperative bacteremia.
3. Methods
3.1. Sample of the Study
This clinical trial study was conducted in the urology department of Al-Zahra Hospital, Isfahan, Iran from 2017 to 2018 on BPH patients who were candidate for TURP. Because of urinary retention in these patients, all the patients had a catheter before surgery. After receiving their informed consent, the study was approved by the Ethics Committee of Isfahan University of Medical Sciences (IR. MUI.MED.REC 1397.073)
3.2. Inclusion and Exclusion Criteria
In this study, inclusion criteria were male patients with BPH who were candidate for TURP. All the patients had urinary catheters and were diagnosed with bacteriuria. Moreover, patients with symptomatic bacteriuria were excluded from the study.
3.3. Classification of Patients and Antibiotic Administration
In this study, antibiotics were administered to all patients one hour before surgery according to the guidelines. Sixty participants were randomly assigned into two groups (case and control groups). In the case group, the bladder was rinsed with 50 cc chlorhexidine 0.2% for 10 min, and the bladder in the control group was rinsed with 50 cc distilled water for 10 min. Then, the two groups underwent the TURP surgery.
3.4. Blood and Urine Analysis
Six hours after surgery, blood samples were collected safely from all patients and sent to the laboratory immediately. After separating serum using a centrifuge (Eppendorf, 5702), Biomerieux kit, France was used to evaluating procalcitonin (PCT). The PCT level was classified into three groups (low level: 0 - 0.5 ng/ml, medium level: > 0.05 - 0.5 ng/mL, and high level: > 0.5 ng/mL)
Before treatment, eosin-methylene blue agar medium (EMB agar) was used to determine urine culture. The urine culture method was performed by placing a sterile wire loop in the urine plate. Then urine culture was incubated at 37°C for 24 - 48 hours. Colony counts > 100 CFU/mL and < 100 CFU/mL as positive and negative cultures, respectively.
Furthermore, blood samples were inoculated to BACTEC blood culture vials, and then the vials were incubated in BACTEC 9120 instrument for seven hours. The vials, which were declared positive by the machine, were re-cultivated.
3.5. Statistical Analysis
Data were imported to SPSS version 18. Independent t-test and chi-square test were used for the data analysis. P< 0.05 was set as the significance level.
4. Results
In the present study, 60 patients with BPH were assigned into two groups (n = 30). The participants’ mean age in the control and case groups was 67.46 ± 7.85 and 70.16 ± 6.23 years, respectively. In terms of age, the two groups revealed no significant difference (P = 0.14). Furthermore, the urine culture results revealed the positive urine culture for all the patients.
Table 1 shows the results of BACTEC blood culture in the case and control groups.
| Groups | BACTEC Blood Culture | P-Value | |
|---|---|---|---|
| Positive, No (%) | Negative, No (%) | ||
| Case | 0 (0) | 30 (100) | 0.076 |
| Control | 3 (10) | 27 (90) | |
The results of BACTEC blood culture showed positive BACTEC blood culture in 3 (10%) and 0 (0%) patients in the control and case groups, respectively. Moreover, no significant difference was noticed between the two groups in terms of BACTEC blood culture (P = 0.076). Table 2 shows the frequency of patients in terms of procalcitonin level.
| Procalcitonin Level a | Control, Frequency (%) | Case, Frequency (%) | P-Value |
|---|---|---|---|
| Low | 2 (6.66) | 12 (40) | 0.000 |
| Medium | 14 (46.6) | 16 (53.3) | |
| High | 14 (46.6) | 2 (6.66) | |
| Total | 30 (100) | 30 (100) |
aLow: 0-0.5 ng/mL, Medium: >0.05 - 0.5 ng/mL, High: > 0.5 ng/mL.
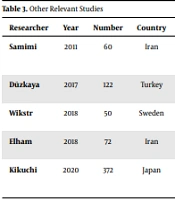
As shown in Table 2, 6.6 % and 46.6 % of the patients in the control group have low and high PCT levels, respectively. Moreover, 40 % and 6.66 % of the patients in the case group have low and high PCT levels, respectively. A significant difference was noticed between the two groups in terms of calcitonin level (P < 0.01). Table 3 presents some other relevant studies.
| Researcher | Year | Number | Country | Age | Sex | Outcome |
|---|---|---|---|---|---|---|
| Samimi | 2011 | 60 | Iran | 50 | M | A significant difference was detected between chlorhexidine (30%) and saline (77.3%) groups in terms of infection. Bladder irrigation with chlorhexidine 0.2% seems to decrease infection because of catheterization (19) |
| Duzkaya | 2017 | 122 | Turkey | 37 - 48 | F, M | Chlorhexidine0.05%; povidone-iodine10%, or sterile water had no significantly different effects on catheter-associated urinary tract infections (CAUTI) in the three groups (20) |
| Wikstrom | 2018 | 50 | Sweden | 43.7 | M, F | Bladder irrigation with chlorhexidine, using intermittent self-catheterization, reduced bacteriuria in most patients with bacteriuria (21) |
| Elham | 2018 | 72 | Iran | - | M | Chlorhexidine gluconate 2% reduced bacteriuria in catheterized patients compared to povidone-iodine 10%; however, the difference was not significant (22) |
| Kikuchi | 2020 | 372 | Japan | 74.6 | M | Maintenance antisepsis with chlorhexidine 1% decreased the risk of developing catheter-related bloodstream infection in more than 20 days after central venous catheter insertion, indicating the effectiveness of chlorhexidine 1% (23) |
5. Discussion
TURP is a common surgery in urology. Foley catheter and bacteriuria in patients lead to bacteremia. Moreover, sepsis is a systematic response to infection by microbial organisms. The diagnosis of infection caused by bacteria or other microbial organisms is essential for effective treatment and prognostic assessment. There is no specific clinical laboratory method in the diagnosis of bacterial infection. PCT is a favorable biomarker for the recognition of bacterial infections and sepsis (24), which is superior to other biomarkers in predicting the severity of disease (24). Reinhart et al. reported that PCT is a valuable marker for host inflammatory responses (25). Jin et al. also claimed that PCT exhibits greater specificity than other pro-inflammatory markers in identifying patients with sepsis and diagnosing bacterial infections (26).
In this study, the bladder was rinsed with 50 cc distilled water and chlorhexidine 0.2%, and findings revealed the higher PCT level of and the high risk of sepsis in the control group, compared to the case group. Accordingly, bladder washing with chlorhexidine in patients with foley catheters reduces the probability of bacterial infection during and after surgery. Mimoz et al. noted that chlorhexidine-based solutions could be used to prevent catheter-related infection (27). In this regard, PCT threshold < 0.25 ng/mL is a strong predictor of the absence of urinary tract infection (25). Elham et al. documented that, compared to povidone-iodine 10%, chlorhexidine 2% further decreased bacteriuria in catheterized patients (22); however, Ball et al. stated that bladder irrigation with chlorhexidine used to prevent urinary infection did not eliminate pre-existing infection (28). To sum up, the findings are not consistent in this regard.
Moreover, we administered antibiotics for all the patients one hour before surgery according to the guidelines, resulting in a high level of antibiotics in the blood and preventing the conversion of bacteremia to symptomatic bacteremia. According to Bose et al., the early identification of bacteremia is necessary to prevent infection progression to a more severe form (29). Qiang et al. assessed the effect of antibiotics on TURP and observed that antibiotic prophylaxis reduced the infection rate in such patients. They observed a remarkable difference between individuals receiving antibiotic prophylaxis versus placebo in terms of post-TURP bacteriuria (26.2 to 9.2%). Moreover, they declared that antibiotic prophylaxis decreased high fever and bacteremia in these patients (30). In Grabe et al.’s study, antibiotic prophylaxis was used to prevent bacterial growth in urine (31). According to these researchers, antibiotic use is associated with clean and clean-contaminated operations (31). Other studies have also suggested a decrease in the infection rate in the presence of antibiotics (30). Hence, PCT evaluation may be used to motivate or hinder antibiotic therapy in patients with systemic infections (18). Levin et al. reported that procalcitonin measurement improves the diagnosis of bacterial infections and decreases the unnecessary consumption of antibiotics (32).
The results of BACTEC blood culture also revealed positive BACTEC blood culture in three patients in the control group and no patient in the case group. The findings indicated that the frequency of bacterial contamination was higher in the control group than in the case group. However, no significant difference was noticed between the two groups in terms of the BACTEC blood culture system. Riedel et al. proposed BACTEC 9240 and BACT/Alert blood culture systems to detect bacterial contamination. They also reported that the BACTEC system is an appropriate method to screen bacterial contamination in microbiology laboratories (33). This finding was not in line with those of the present study. The most meaningful difference between the two studies seemed to be raised by sample size. Sixty patients were included in the present study, while Riedel et al. conducted a study on 113 patients. Gokbolat et al. evaluated the BACTEC 9240 automated blood culture system in detecting Candida species. They showed the low sensitivity rate of blood culture tests (34). Cuenca-Estrella et al. also achieved the same findings and stated that blood culture as a critical diagnostic test was associated with low sensitivity (35). According to the findings of the present study and many other studies, the BACTEC blood culture system may not be an effective test to detect bacterial contamination.
5.1. Conclusions
According to the findings of this study, the frequency of patients with a high level of procalcitonin after TURP was higher in the control group than in the case group, indicating that chlorhexidine in catheterized patients undergoing TURP decreases the number of bacteria in the bladder. In other words, the probability of bacteremia is lower in the case group. It seems that procalcitonin level can be considered as a strong biomarker to predict bacteria in such patients.