1. Background
Soft tissue sarcomas (STS) are classified as a group of relatively rare heterogeneous tumors with a non-osseous origin accounting for approximately 0.7% of all cancers (1-4). Primary sarcoma originating from the genitourinary (GU) tract accounts for 2.1% of all the STSs and between 1% and 2% of all GU cancers (5-8). As a result of the exceeding rarity of this group of malignancies, there are few published articles about GU sarcomas and their characteristics. Furthermore, the sample size of previously conducted literature is often small, as the largest published series comprised of 131 patients treated over a span of 25 years in the Memorial Sloan Kettering Cancer Center, New York, USA (6).
Previous studies established the impact of ethnicity, racial, and geographic factors on the prevalence and prognosis of STSs (9, 10). Multi-institution studies conducted in different social and geographical settings may benefit both researchers and clinicians in providing patients suffering from GU sarcomas with proper intervention and care.
2. Objectives
The current study aimed at presenting a descriptive analysis of GU sarcoma among the Iranian population from April 2009 to June 2014 registered in the Cancer Research Center (CRC) database, providing data regarding patients’ clinicopathological characteristics, tumor location, grading, and histology.
3. Methods
The population sample for this retrospective study was composed of all known cases of STS across the country from April 2009 to June 2014, registered in the CRC database. Patients with pathologically and microscopically confirmed sarcomas originating from the urogenital tract were included in the analysis. Patients’ medical history was extracted from the CRC database, subjects with a history of metastatic cancers, and patients with a history of drastic GU surgical operations, such as radical nephrectomy before their diagnosis were excluded from the study to avoid analytical discrepancies. Out of 1534 STS patients in CRC records, 337 met our inclusion criteria and were enrolled in the study.
Basic patient variables, including age, gender, city, and the province of residence, as well as data regarding tumor anatomical location, morphology, and grading were also recorded. As CRC is a subsection of the Iranian Ministry of Health, the retrieved data provided sufficient coverage across nearly the entire geographical provinces of Iran. Tumor grading was confirmed by reviewing pathology records, and tumor histological grade was defined as low or high, depending on the degree of cellularity and nuclear pleomorphism, mitosis quantity, and cell differentiation. The design and methodology of this study were reviewed and approved through the Ethics Committee of Shahid Beheshti University of Medical Sciences.
IBM’s Statistical Package for Social Sciences (SPSS) version 22 was utilized for statistical analysis. Chi-square test was used in determining a possible relationship between basic patient data and the tumor characteristics. P value ≤ 0.05 was considered statistically significant. Analysis of domains with values too small to be assessed through Pearson’s Chi-Square test was performed through the Likelihood Ratio Chi-Square test. P value ≤ 0.05 was considered statistically significant.
4. Results
During the timeframe for this study, 337 patients with sarcoma of the GU tract were diagnosed across the country. Although the majority of the subjects originated from the capital city of Tehran (19.0%), a notable percentage of patients were referred from the north-western (12.5%) and north-eastern (13.1%) provinces of the country. Table 1 presents the basic demographics for the subjects and tumor characteristics.
| Variable | No. of patients, No. (%) (total=337) |
|---|---|
| Age Categories, yr | |
| 0-14 | 55 (16.3) |
| 15-64 | 181 (53.7) |
| ≥ 65 | 101 (30) |
| Gender | |
| Female | 91 (27.0) |
| Male | 246 (73.0) |
| Tumor Histological Morphology | |
| Liposarcoma | 65 (19.2) |
| Leiomyosarcoma | 53 (15.7) |
| Rhabdomyosarcoma | 52 (15.4) |
| Spindle cell sarcoma | 32 (9.5) |
| Malignant fibrous histiocytoma | 15 (4.5) |
| Clear cell sarcoma of the kidney | 15 (4.5) |
| Kaposi sarcoma | 11 (3.3) |
| Other | 94 (27.8) |
| The primary organ of involvement | |
| Kidney | 106 (31.5) |
| Bladder | 74 (22.0) |
| Testis / Paratesticular region | 65 (19.3) |
| Prostate | 34 (10.1) |
| Penis | 10 (3.0) |
| Ureter | 5 (1.5) |
| Unspecified male organ | 43 (12.8) |
| Tumor Grade | |
| Low | 50 (14.9) |
| High | 52 (15.4) |
| Undetermined | 235 (69.7) |
A male predominance was observed among the subjects with 246 (73%) patients being male and 91 (27%) female. When comparing gender to the other patient parameters, no notable relationship was found between gender and tumor morphology or grading. However, as Table 2 shows, a positive association was noted between gender and the primary anatomical site of the tumors (P < 0.001).
| Characteristics | Kidney | Bladder | Testis | Prostate | Penis | Ureter | Unspecified male organ | Total | P value |
|---|---|---|---|---|---|---|---|---|---|
| Age Categories, yr | 0.015 | ||||||||
| 0-14 | 23 | 16 | 9 | 4 | 0 | 0 | 3 | 55 | |
| 15-64 | 65 | 35 | 31 | 19 | 3 | 3 | 25 | 181 | |
| ≥ 65 | 18 | 23 | 25 | 11 | 7 | 2 | 15 | 101 | |
| Gender | 0.02 | ||||||||
| Male | 45 | 46 | 65 | 34 | 10 | 3 | 43 | 246 | |
| Female | 61 | 28 | 0 | 0 | 0 | 2 | 0 | 91 | |
| Grading | 0.031 | ||||||||
| Low | 14 | 4 | 8 | 6 | 0 | 3 | 15 | 50 | |
| High | 19 | 18 | 5 | 6 | 0 | 0 | 4 | 52 | |
| Undetermined | 73 | 52 | 52 | 22 | 22 | 2 | 24 | 235 |
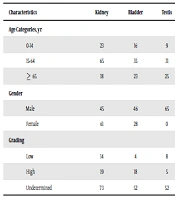
The incidence of GU sarcomas was also assessed in the three designed subgroups of patients based on age. The highest rate of GU sarcomas was observed among the age group of 15 to 64 years (53.7%), followed by the ≥ 65 year age group (30.0%). Of all the tumors, 50 (14.9%) were reported as low-grade, 52 (15.4%) were classified as high-grade, while the remaining 235 (69.7%) were designated as pathologically undetermined. The most commonly reported histological subtype of tumors was Liposarcoma (19.2%), followed by Leiomyosarcoma (15.7%) and Rhabdomyosarcoma (15.4%). The predominant sites of involvement were the kidney (31.5%), bladder (22.0%), and the testis/paratesticular region (19.3%). Table 2 reveals a statistical association between the anatomical location of the tumors and the rest of the characteristics of the subjects. As mentioned above, a notable relationship was witnessed between age and tumor location. The gender of the patients and the grading of the tumors were shown to be similarly associated with the primary organ of involvement (P < 0.05).
Table 3 demonstrates the relationship between the histological morphology of the tumors and patients’ characteristics, as well as the primary organ of involvement. A significant statistical association was noted between tumor morphology and all of the assessed characteristics including the age and the gender of the patients, tumor grading, and the primary anatomical site of the tumors (P < 0.05).
| Characteristics | Liposarcoma | Leiomyo sarcoma | Rhabdomy sarcoma | Spindle cell sarcoma | Malignant fibrous histiocytoma | Clear cell sarcoma of the kidney | Kaposi sarcoma | Other | Total | P value |
|---|---|---|---|---|---|---|---|---|---|---|
| Age Categories, yr | 0.02 | |||||||||
| 0-14 | 1 | 2 | 30 | 1 | 0 | 9 | 0 | 12 | 55 | |
| 15-64 | 40 | 34 | 20 | 26 | 8 | 4 | 3 | 46 | 181 | |
| ≥ 65 | 24 | 17 | 2 | 5 | 7 | 2 | 8 | 36 | 101 | |
| Gender | 0.03 | |||||||||
| Male | 47 | 37 | 39 | 19 | 12 | 8 | 11 | 73 | 246 | |
| Female | 18 | 16 | 13 | 13 | 3 | 7 | 0 | 21 | 91 | |
| Grading | 0.021 | |||||||||
| Low | 20 | 18 | 0 | 3 | 0 | 1 | 2 | 6 | 50 | |
| High | 12 | 5 | 2 | 8 | 7 | 0 | 0 | 18 | 52 | |
| Undetermined | 33 | 30 | 50 | 21 | 8 | 14 | 9 | 70 | 235 | |
| Primary Tumor Site | 0.01 | |||||||||
| Kidney | 22 | 15 | 5 | 11 | 3 | 15 | 0 | 35 | 106 | |
| Bladder | 8 | 9 | 18 | 6 | 4 | 0 | 0 | 29 | 74 | |
| Testis | 15 | 13 | 16 | 4 | 2 | 0 | 1 | 28 | 65 | |
| Prostate | 7 | 0 | 6 | 6 | 0 | 0 | 2 | 21 | 34 | |
| Penis | 0 | 0 | 0 | 1 | 0 | 0 | 8 | 9 | 10 | |
| Ureter | 1 | 2 | 0 | 0 | 1 | 0 | 0 | 4 | 5 | |
| Unspecified Male Organ | 12 | 12 | 7 | 4 | 5 | 0 | 0 | 3 | 43 |
5. Discussion
Primary sarcomas involving the GU tract are rare. As mentioned before, they comprise about 2% of the entire urological cancers and 2% of STSs (5, 6, 11). While tumor registry centers across the world often provide population-based data regarding general characteristics of cancers in a regional scope, the influence of ethnic and racial factors on patients’ characteristics demonstrates the importance of such analyses in different geographical settings. Studies like those conducted by Martinez et al. (10) and DiGiovanna et al. (9) confirm the influence of ethnicity and race on the properties of STS patients, and henceforth the need for conducting national-based studies independently for each type of tumors. The main goal of this study is to provide a detailed descriptive analysis of GU sarcomas among the Iranian population according to the CRC registry from 2009 to 2014, thus providing a national reference for future literature.
The subjects of this study were distributed in 3 sub-domains based on their age. As stated before, our analysis found the prevalence of GU sarcoma higher in the age group of 15 to 64 years compared to the other age domains. Previous descriptive studies on GU sarcomas confirmed these findings, as GU sarcomas are demonstrated to be more common among adults younger than 65 years old (5, 6, 12, 13). Similar to the study conducted by Dotan et al., we found the subjects’ age to correlate with the primary location of tumors across all 3 sub-domains (P < 0.05). Male predominance was noted across all of the age groups and among the subjects in general, comprising 73.0% of the total subjects.
GU sarcomas share several histologic and pathologic characteristics with other STSs. The previously published literature establishes liposarcoma as the most commonly found histological subtype of STS, followed by malignant histiocytoma and leiomyosarcoma (11). While the data on primary GU sarcomas are scarce, prior studies suggested similar histologic findings in the GU sarcoma with leiomyosarcoma and liposarcoma reported as the most commonly found histologic subtypes, respectively (5, 6, 14-18). Our analysis found liposarcoma as the most frequently seen histologic subtype (19.2%), followed by leiomyosarcoma (15.7%), rhabdomyosarcoma (15.4%), spindle cell sarcoma (9.5%), and malignant fibrous histiocytoma (4.5%). Although leiomyosarcoma is generally regarded as the most prevalent histological subtype in the GU sarcoma, an analysis conducted by Zhang et al. regarded liposarcoma as the primary histological finding (19). This relative discrepancy may be related to leiomyosarcoma often involving the GU tract and end-organs, while liposarcoma has a greater tendency toward retroperitoneal involvement (6, 19).
The data on the pathological grading of the tumors were retrospectively retrieved from the CRC database, with the majority of the tumors’ grading defined as pathologically undetermined. Of those with diagnosed grading, 52 (15.4%) were designated high-grade, while 50 (14.9%) were recorded as low-grade. Our analysis demonstrated a notable statistical association between tumors’ grading and their primary anatomical location (P < 0.05). A similar association was observed between age and grading (P < 0.05), with high-grade tumors predominantly seen in older subjects. As mentioned by the previous literature, both age and grading are independent factors of survival in patients with the GU sarcoma (5, 6). Nevertheless, a comparison of gender and tumor grading parameters yielded no significant statistical relationship (P = 0.728). Overall, our findings confirmed the established data by previously published articles, as we demonstrated that GU sarcomas predominantly occurred in the Iranian adult population, with the most common histologic subtypes similar to those witnessed by the other studies. However, several limitations must be addressed.
Firstly, the data provided by CRC did not include patients’ survival rate, existing metastasis, undergone treatment, and disease relapse. Prospective follow-up was not performed; therefore, analysis of these variables and their association with the available subject characteristics were beyond the scope of this study. Secondly, the data were retrospectively provided, and the predominance of the pathologically undetermined GU sarcoma might affect the analysis of the subjects’ tumor grading.
5.1. Conclusions
Primary sarcomas originating from the GU tract are a relatively rare class of tumors, accounting for around 2% of all urological malignancies. Our study aimed at providing descriptive data on this spectrum of tumors in the Iranian population between 2009 and 2014. Similar characteristics were observed among Iranian GU sarcoma patients compared to the prior studies conducted in different geographical settings.