1. Background
Volumetric modulated arc therapy (VMAT) has been adopted by many centers for the curative treatment of locally advanced head and neck (H&N) cancer. This relatively modern technique is still in its infancy concerning the long-term follow-up data of patient-related outcomes and quality of life (QOL) studies. The greatest benefit is achieving a steep dose gradient, which is translated into a better therapeutic ratio (1-3), thereby reducing the side-effects like xerostomia and dysphagia.
2. Objectives
This prospective observational study was carried out to ascertain the impact of dysphagia on the QOL of patients undergoing radiation therapy for H&N cancer with curative intent. The same was assessed by MD Anderson dysphagia inventory (MDADI) (4), which is a dysphagia-specific QOL questionnaire for patients with H&N cancer.
3. Methods
3.1. Patient Selection
This prospective observational study was conducted at a tertiary care hospital in India from January 2017 to January 2018. Patients with a histopathological diagnosis of squamous cell carcinoma of the H&N, aged 18 years and older, treated by definitive/adjuvant VMAT with curative intent were enrolled in this study. Those with lymphomas and/or alternate histologies, metastatic or recurrent disease, and Karnofsky performance score < 60 were excluded. Furthermore, patients, who did not complete their treatment or lost the follow-up, were excluded from the analysis. Non-random sampling was used and consecutive patients receiving VMAT meeting the inclusion criteria were enrolled. All the participants provided written informed consent.
3.2. Treatment
All patients were treated on multi-energy ELEKTA Versa HD linear accelerator with external beam radiation therapy, using VMAT to a dose of 60 Gy to 70 Gy delivered in 30 to 35 fractions over 6 to 7 weeks with or without concomitant chemotherapy. As per institutional protocol, the emphasis was placed on optimum coverage of the primary tumor (V95 of the planning target volumes ≥ 95%) over the sparing of normal tissues. When indicated, chemotherapy was administered weekly once concurrently with RT; cisplatin (40 mg/m2) was the drug of choice as the chemosensitizer. The dose constraints for organs at risk (OARs) were set-pharyngeal constrictors (mean < 45 - 50 Gy), larynx (mean < 40 Gy), and cervical esophagus (mean < 45 - 50 Gy) (5).
3.3. Target Volume Delineation
Gross tumor volume (GTV) consisted of all the grossly visible disease by clinical examination and/or by imaging. Clinical target volume (CTV) included the GTV with an expansion to account for subclinical disease. The regions at high risk were included in the CTVhigh risk. The regions were assumed to be at a lesser risk of harboring disease and were included in the CTVintermediate risk/low risk. The planning target volumes (PTVs) were generated by giving an isometric expansion of 5 mm to all CTVs. PTVs high risk/intermediate-risk/low risk were prescribed to a dose of 66 Gy to 70 Gy, 59.4 Gy, and 56 Gy, respectively, using simultaneous integrated boost single-phase technique with 5 fractions weekly. The neck node levels were contoured as per DAHANCA 2013 consensus guidelines (6).
3.4. Contouring of Dysphagia and Aspiration Related Structures (DARS)
The superior, middle, and inferior constrictors were contoured as a single structure labeled as pharyngeal constrictors, cranially starting from the pterygoid plates extending caudally up to the inferior edge of cricoid cartilage (7). The larynx was contoured starting cranially from the top of the pyriform sinus going downward up to the inferior edge of the cricoid cartilage with the lumen excluded (8). Contouring of the cervical esophagus began cranially from the inferior edge of the cricoid cartilage until the level of the superior extent of the aortic arch (7).
3.5. Assessment of Dysphagia
Dysphagia was assessed and graded according to the common terminology criteria for adverse events (CTC-AE version 4.03) scoring system before starting the treatment, at the completion of treatment, and 3 to 6 months after the completion of RT.
The evaluation of dysphagia associated QOL was done with the help of a questionnaire known as MDADI. It comprises 4 subscales-global, emotional, functional, and physical with a total of 20 questions.
The global subscale consists of one question, which asks how the overall daily routine of an individual is affected as a result of swallowing difficulty. The emotional component of MDADI consists of 6 statements assessing a patient's affective responses to dysphagia. The functional subscale represents the impact of a swallowing problem on a person’s daily activities. Questions in the physical subscale indicate the self-perceptions of swallowing difficulty. For each question, 5 possible options are given in the MDADI (strongly agree, agree, no opinion, disagree, and strongly disagree) and scored on a scale of 1 to 5 (1 for strongly agree and 5 for strongly disagree). One question in the emotional (I do not feel self-conscious when I eat) and another in the functional section (I feel free to go out to eat with my friends, neighbors, and relatives) are scored as 5 for strongly agree and 1 for strongly disagree. All the questions in a single subscale are summed up and, then, a mean score is obtained, which is multiplied by 20 to derive a score, which lies between 0 (extremely low functioning) and 100 (high functioning). Thus, the higher the MDADI scores, the better is the QOL.
3.6. Data Analysis
The data were analyzed, using Microsoft Excel 2017 and SPSS version 20 (Statistical Package for Social Sciences, IL, Chicago). The chi-square test and Independent-samples t-test were applied for the analysis. A value of 0.05 was taken as a level of significance in our study. Spearman correlation coefficients were calculated between the MDADI scores and mean OAR doses.
4. Results
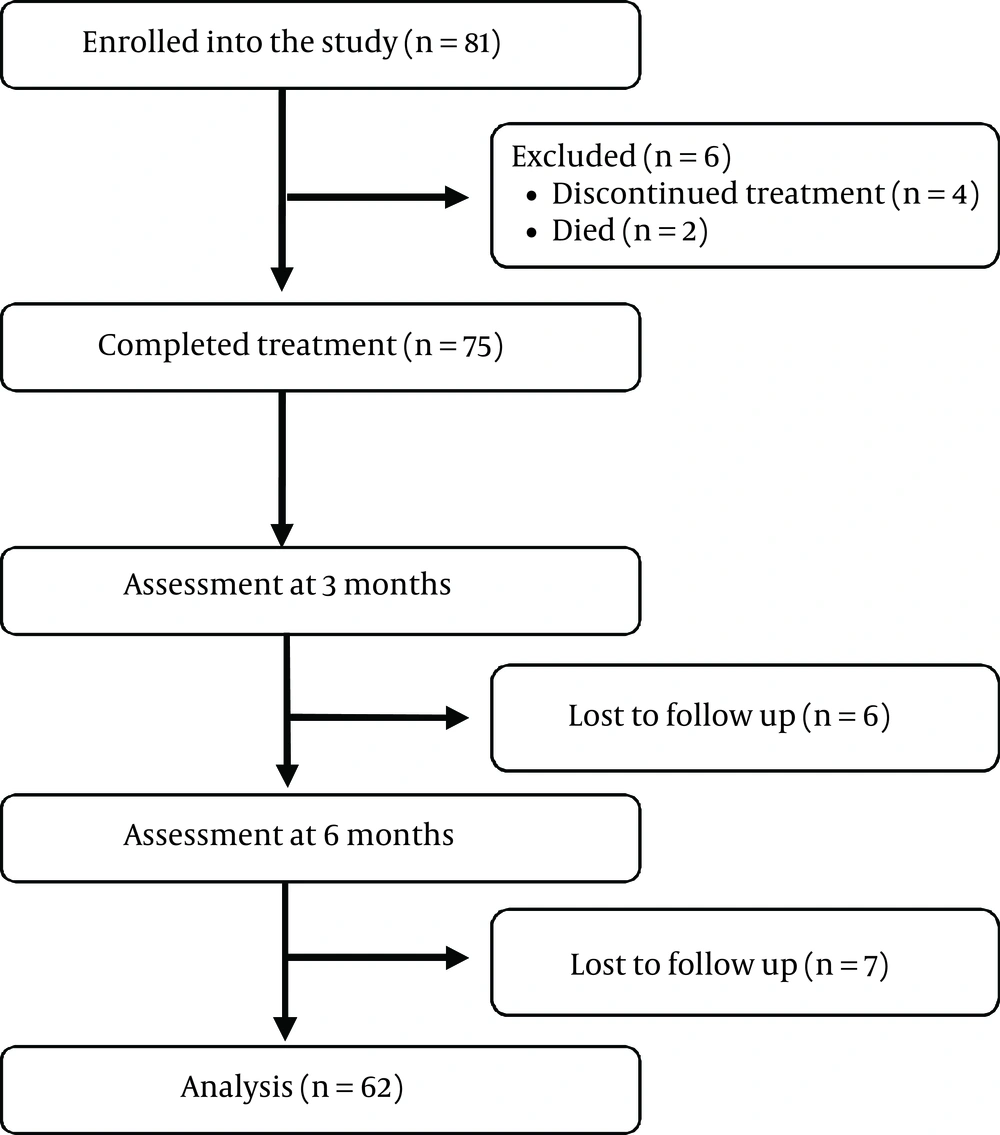
Out of the 81 patients initially enrolled for the study, 62 patients were included for the final data analysis (Figure 1).
4.1. Demographics
The baseline characteristics of all participants were recorded from the patient records (Table 1).
| Factors | Frequency, No. (%) |
|---|---|
| Age (median), y | 54 |
| Gender | |
| Males | 57 (91.9) |
| Females | 5 (8.1) |
| Performance score (ECOG) | |
| 1 | 51 (82.3) |
| 2 | 11 (17.7) |
| Subsite | |
| Oral cavity | 21 (33.9) |
| Oropharynx | 15 (24.2) |
| Hypopharynx | 10 (16.1) |
| Larynx | 12 (19.4) |
| Nasopharynx | 2 (3.2) |
| Sinonasal | 2 (3.2) |
| Stage | |
| Early-stage (I & II) | 13 (21) |
| Advanced stage (III, IVA, & IVB) | 49 (79) |
| Histological grade | |
| Well differentiated | 32 (51.6) |
| Mod. Differentiated | 23 (37.1) |
| Poorly differentiated | 4 (6.5) |
| Others | 3 (4.8) |
| Intent of RT | |
| Definitive | 32 (51.6) |
| Adjuvant | 30 (48.4) |
| Chemotherapy | |
| Yes | 37 (59.7) |
| No | 25 (40.3) |
4.2. Dose-Volume Characteristics
The overall mean doses to the constrictors, larynx, and cervical esophagus have been reported along with the individual subsites-based doses in Tables 2 and 3.
| Mean Dose (Gy) | |
|---|---|
| Constrictors | |
| Mean | 51.2 |
| Range | 16.8 - 69.5 |
| Larynx | |
| Mean | 49.5 |
| Range | 5.5 - 72.5 |
| Cervical esophagus | |
| Mean | 50.0 |
| Range | 0.3 - 71.2 |
| Subsite | Mean doses (Gy) | ||
|---|---|---|---|
| Constrictors | Larynx | Cervical Oesophagus | |
| Oropharynx (n = 15) | 55.9 | 48.0 | 48.6 |
| Oral Cavity (n = 21) | 40.9 | 38.3 | 40.1 |
| Hypopharynx (n = 10) | 57.0 | 68.3 | 62.3 |
| Larynx (n = 12) | 54.5 | 69.5 | 59.9 |
| Nasopharynx & sinonasal (n = 4) | 49.3 | 33.8 | 40.1 |
4.3. Acute Dysphagia
Dysphagia was assessed and graded according to CTC-AE V. 4.03 before the treatment, at completion, and 3 months after the treatment. The same has been depicted in Table 4.
| Before Starting Treatment | At Completion | At 3 Months | |
|---|---|---|---|
| No dysphagia | 32 (51.6) | 7 (11.2) | 34 (54.8) |
| Grade I dysphagia | 25 (40.3) | 23 (37.1) | 23 (37.1) |
| Grade II dysphagia | 5 (8) | 15 (24.2) | 5 (8) |
| Grade III dysphagia | 0 | 17 (27.4) | 0 |
| Laryngeal edema grade I | 0 | 15 (24.2) | 9 (14.5) |
| Laryngeal edema grade II | 0 | 11 (17.7) | 5 (8.1) |
aValues are expressed as No. (%).
There were no patients with grade IV or higher dysphagia.
Laryngitis manifested as hoarseness of voice and dry cough was observed in 15 patients (24.2%) having grade I and 11 patients (17.7%) with grade II laryngitis.
At 3 months after the treatment, 34 patients (54.8%) had no dysphagia, whereas 23 patients (37.1%) had grade I dysphagia and 9 patients (14.5%) had grade I laryngitis.
4.4. Late Toxicities
Late toxicities were assessed at 6 months after the treatment. Then, 13 patients lost the follow-up (Table 5).
| Dysphagia Grade | At 6 Months |
|---|---|
| No dysphagia | 49 (79) |
| Grade I dysphagia | 10 (16.1) |
| Grade II dysphagia | 3 (4.8) |
| No laryngeal edema | 41 (66.1) |
| Grade I laryngeal edema | 14 (22.6) |
| Grade II laryngeal edema | 5 (8.1) |
| Grade III/IV laryngeal edema | 2 (3.2) |
aValues are expressed as No. (%).
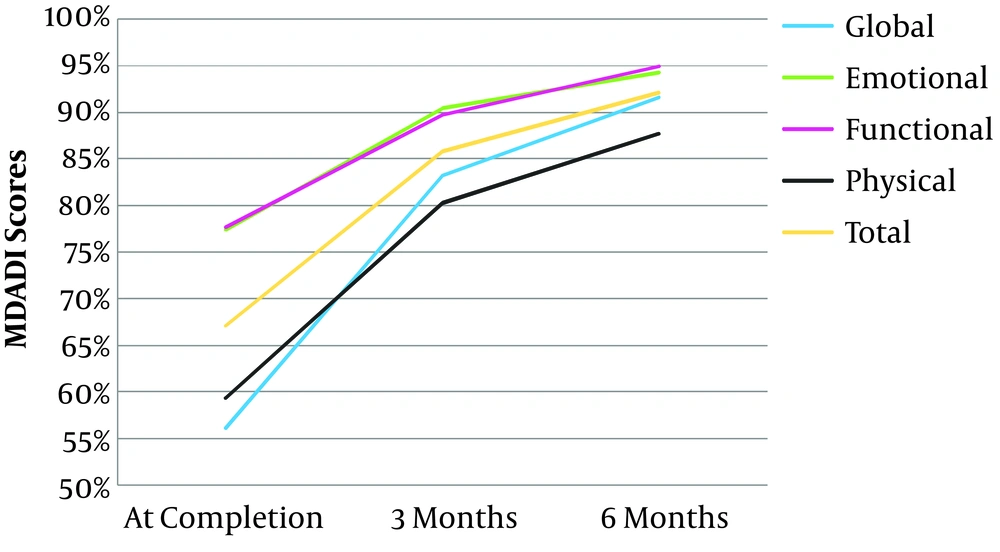
The MDADI questionnaire was administered at 3 points of time to assess the impact of dysphagia on the QOL of patients. The average total score at the completion of treatment was 67.11 (range 43-94), which improved on subsequent visits. Similarly, there was an improvement in the individual average sub-scores, especially in the global and physical components, showing a marked increment in average scores at 6 months. This trend of improvement in QOL is depicted in Figure 2 and Table 6.
| At Completion | At 3 Months | At 6 Months | |
|---|---|---|---|
| Global | |||
| Mean ± SD | 56.1 ± 23.9 | 83.2 ± 22.1 | 91.6 ± 18.3 |
| Range | 20 - 100 | 40 - 100 | 20 - 100 |
| Emotional | |||
| Mean ± SD | 77.4 ± 11.0 | 90.4 ± 7.7 | 94.3 ± 7.4 |
| Range | 50 - 100 | 73 - 100 | 71 - 100 |
| Functional | |||
| Mean ± SD | 77.7 ± 14.5 | 89.7 ± 9.2 | 94.9 ± 5.9 |
| Range | 36 - 100 | 55 - 100 | 74 - 100 |
| Physical | |||
| Mean ± SD | 59.4 ± 13.7 | 80.3 ± 14.1 | 87.7 ± 11.7 |
| Range | 38 - 95 | 50 - 98 | 53 - 100 |
| Total | |||
| Mean ± SD | 67.1 ± 13.2 | 85.8 ± 11.2 | 92.1 ± 9.3 |
| Range | 43 - 94 | 59 - 99 | 60 - 99 |
4.5. Association Between Dysphagia and Quality of Life
Independent-samples t-test was applied to test the correlation between the patient-reported QOL scores and the severity of dysphagia and a strong association was found between the same. Total MDADI scores were lower for those who had significant dysphagia than those who did not (P < 0.001). The scores of the individual components (i.e. global, emotional, functional, and physical sub-scores of the questionnaire) also correlated with the grade of dysphagia. The same has been depicted in Table 7.
| < Grade 2 (N = 30) | ≥ Grade 2 (N = 32) | P Value | |
|---|---|---|---|
| At completion | |||
| Global | 70.7 ± 17.2 | 42.5 ± 21.4 | < 0.001 |
| Emotional | 84.2 ± 9.7 | 71.0 ± 7.9 | < 0.001 |
| Functional | 85.4 ± 8.9 | 70.4 ± 15.0 | < 0.001 |
| Physical | 69.5 ± 10.1 | 50.0 ± 9.2 | < 0.001 |
| Total | 77.2 ± 8.4 | 57.7 ± 9.4 | < 0.001 |
| AT 3 months | Grade 0 (N = 34) | ≥ Grade 1 (N = 28) | P Value |
| Global | 96.5 ± 7.7 | 67.1 ± 23.2 | < 0.001 |
| Emotional | 95.7 ± 3.2 | 83.9 ± 6.4 | < 0.001 |
| Functional | 93.8 ± 6.7 | 84.7 ± 9.4 | < 0.001 |
| Physical | 90.8 ± 6.1 | 67.5 ± 9.7 | < 0.001 |
| Total | 94.0 ± 4.1 | 75.7 ± 8.6 | < 0.001 |
| AT 6 months | Grade 0 (N = 49) | ≥ Grade 1 (N = 13) | P Value |
| Global | 97.5 ± 6.6 | 69.2 ± 29.0 | < 0.004 |
| Emotional | 97.3 ± 3.6 | 82.9 ± 7.0 | < 0.001 |
| Functional | 96.2 ± 4.2 | 90.0 ± 8.7 | 0.026 |
| Physical | 92.4 ± 6.1 | 70.1 ± 10.9 | < 0.001 |
| Total | 95.8 ± 3.1 | 78.1 ± 11.5 | < 0.001 |
aValues are expressed as mean ± SD.
4.6. Association of Quality of Life and Mean Doses to OARs
The correlation of MDADI scores with mean doses to OARs was analyzed, using the Independent-samples t-test. At the completion of treatment, the total MDADI score was significantly related to the constrictor mean dose (P = 0.035) and larynx mean dose (P = 0.050). Also, there was a statistically significant correlation with some individual sub-scores of the questionnaire (Table 8).
| Constrictor Mean Dose | P Value | Larynx Mean Dose | P Value | Cervical Esophagus Mean Dose | P Value | ||||
|---|---|---|---|---|---|---|---|---|---|
| < 50Gy | ≥ 50Gy | < 45Gy | ≥ 45Gy | < 45Gy | ≥ 45Gy | ||||
| Scores at completion | |||||||||
| Global | 58.5 | 54.3 | 0.495 | 60.7 | 52.6 | 0.186 | 55.0 | 56.5 | 0.669 |
| Emotional | 82.5 | 73.5 | 0.001 | 82.8 | 73.2 | <0.001 | 81.4 | 76.0 | 0.634 |
| Functional | 81.9 | 74.5 | 0.045 | 78.4 | 77.1 | 0.507 | 75.5 | 78.4 | 0.094 |
| Physical | 63.2 | 56.5 | 0.048 | 62.3 | 57.2 | 0.147 | 60.5 | 59.0 | 0.006 |
| Total | 70.7 | 64.3 | 0.035 | 70.8 | 64.3 | 0.050 | 67.6 | 66.9 | 0.469 |
| Scores at 3 months | |||||||||
| Global | 87.4 | 80.0 | 0.341 | 89.6 | 78.3 | 0.044 | 80.0 | 84.4 | 0.502 |
| Emotional | 92.4 | 88.8 | 0.003 | 92.4 | 88.8 | 0.048 | 88.3 | 91.1 | 0.205 |
| Functional | 92.0 | 87.9 | 0.115 | 91.8 | 88.0 | 0.106 | 89.7 | 89.7 | 0.990 |
| Physical | 83.4 | 77.9 | 0.072 | 84.2 | 77.3 | 0.058 | 77.6 | 81.2 | 0.373 |
| Total | 88.6 | 83.6 | 0.010 | 89.3 | 83.0 | 0.028 | 83.8 | 86.5 | 0.411 |
| Scores at 6 months | |||||||||
| Global | 91.1 | 92.0 | 0.807 | 96.3 | 88.0 | 0.077 | 92.5 | 91.3 | 0.824 |
| Emotional | 94.6 | 94.0 | 0.863 | 96.2 | 92.7 | 0.065 | 93.9 | 94.4 | 0.824 |
| Functional | 95.5 | 94.5 | 0.968 | 96.6 | 93.7 | 0.060 | 96.0 | 94.6 | 0.412 |
| Physical | 88.5 | 87.1 | 0.476 | 91.5 | 84.7 | 0.022 | 87.6 | 87.7 | 0.959 |
| Total | 92.6 | 91.7 | 0.952 | 95.0 | 89.9 | 0.029 | 92.5 | 91.9 | 0.849 |
This association was maintained 3 months after the treatment by the constrictors and larynx mean doses (P < 0.05). Keeping the dose constraints for constrictors < 50 Gy and larynx < 45 Gy resulted in a better QOL. The mean doses to the cervical esophagus did not statistically correlate with the questionnaire scores.
At the time of 6 months after the treatment, a correlation was seen only with the larynx mean doses (P < 0.05).
Spearman’s rank correlation analysis was used to find the correlation between the MDADI scores and mean doses to the DARS. The mean dose to constrictors was significantly correlated to the total as well as individual MDADI score values. The correlation coefficient values indicate that, as the mean doses increased, the MDADI scores dropped resulting in a poorer QOL. The same has been depicted in Table 9.
| Constrictors | Larynx | Cervical Esophagus | ||||
|---|---|---|---|---|---|---|
| R2 | P Value | R2 | P Value | R2 | P Value | |
| Global | -0.203 | 0.114 | -0.220 | 0.086 | -0.289 | 0.023 |
| Functional | -0.482 | < 0.001 | -0.440 | < 0.001 | -0.309 | 0.015 |
| Emotional | -0.329 | 0.009 | -0.144 | 0.265 | -0.106 | 0.412 |
| Physical | -0.298 | 0.018 | -0.200 | 0.119 | -0.180 | 0.162 |
| Total | -0.319 | 0.011 | -0.250 | 0.050 | -0.244 | 0.056 |
4.7. Improvement in Quality of Life Associated with Dysphagia
The trend of improvement/worsening of MDADI scores and, hence, the QOL was studied at the end of the study period. It was observed that 50 out of 62 patients (80.6%) had shown improvement, 10 patients (16.1%) were status quo in terms of score values, and 2 patients (3.2%) had worsening of QOL because of recurrence/development of new primary. A total of 13 patients had lost the follow-up and their status was unknown.
5. Discussion
MDADI is the first validated and extremely reliable self-administered questionnaire that specifically intends to evaluate the impact of dysphagia on the QOL of patients with H&N cancer. The MDADI scores represent an individual’s perception of their swallowing abilities and swallowing-related QOL. Patients having primary tumors in the oral cavity or oropharynx may have an undesirable QOL and an appreciably greater swallowing dysfunction compared to patients with primary tumors in the larynx and hypopharynx.
The mean MDADI scores for the 62 patients at the time of treatment completion were emotional (77.4 ± 11.0), functional (77.7 ± 14.5), physical (59.4 ± 13.7), global (56.1 ± 23.9), and total (67.1 ± 13.2). The questionnaire was administered again at 3 months and 6 months after therapy. The mean global scores were lower and more variable (SD = 23.9) than the other subscale scores. Among the other 3 subscale scores, the mean physical domain scores were the lowest at all times of assessment. Overall, there was a drastic improvement in the swallowing-related QOL as indicated by the rising MDADI scores at subsequent follow-up.
As would have been expected, a strong association was found between the patient-reported MDADI scores and the severity of dysphagia. Again, it is worth noting that the global domain and the composite MDADI scores are not reliable measures to assess dysphagia-related QOL. It is the functional, emotional, and physical components that are more consistent and reflect the specific domains of a patient’s perception of his swallowing ability. Hence, we have taken these domains as primary endpoints of interest when using the MDADI as a QOL measure tool.
When constrictor mean dose exceeded 50 Gy, the mean global score would be 54.3 at the time of treatment completion, which improved at subsequent follow-up visits, but this was not statistically significant. It can be explained by the fact that the global score consists only of a single question, which indicates the impact of dysphagia on the day-to-day routine of individuals. So, we do not consider it an appropriate measure of QOL. The emotional component of the inventory was found to have a mean score of 73 at treatment completion when the dose constraints to constrictor muscles and larynx were not respected. This correlation was statistically significant 3 months after the treatment but failed to maintain this association between MDADI in the sixth month after the treatment.
The total MDADI scores of the patients, whose mean constrictor dose and mean larynx dose exceeded 50 Gy and 45 Gy, respectively, were markedly low. Dmeans of the cervical esophagus failed to show a correlation with any of the MDADI parameters.
There was a remarkable improvement in the QOL of patients as shown by the rising MDADI scores. Out of 62 patients, 10 did not show a significant change in their swallowing function status. Two patients developed worsening of symptoms and when they were evaluated further, they were found to have a new primary in the oropharynx and hypopharynx.
Jensen et al. (8) conducted a retrospective study aiming at establishing a correlation between QOL questionnaire scores and the findings of an instrumental method of assessing dysphagia called functional endoscopic evaluation of swallowing (FEES). There were 35 patients in the study, most of whom had an oropharyngeal primary. The EORTC, QLQC30, and H&N35 questionnaires were administered and FEES was done to assess late dysphagia. QOL score values and abnormal FEES findings significantly correlated with the dose to the supraglottic larynx and upper oesophageal sphincter.
According to a study by Langendijk et al. (9), there was a significant correlation between observer-assessed grades of dysphagia and all the MDADI parameters for 37 patients.
The relationship between the radiation dose received by the muscular structures of the swallowing apparatus and the dysphagia-related QOL in patients with carcinoma oropharynx was studied by Levendag et al. (10). A steep dose-effect relationship was established with a 19% increase in the probability of dysphagia with every additional 10 Gy of mean dose. A dose-effect relationship between dose to the critical structures and swallowing complaints was observed. One way to improve the QOL is to restrict the doses received by the swallowing apparatus below its tolerance level.
5.1. Limitations
This study is limited by the fact that the size of the study population is small, the QOL-related questionnaire was not administered before treatment, and dysphagia was not objectively assessed by instrumental methods for appropriate comparison with subjective assessment. There was heterogeneity in population as the number of patients with oral cavity tumors was far higher compared to other subsites.
Furthermore, only the mean doses to critical structures were taken into account; parameters like V30 or V40 would have been even more valuable.
5.2. Conclusions
In conclusion, MDADI is a popular validated measure of swallowing outcomes in H&N cancer research. Despite its limitations, the present study has demonstrated that using modern techniques like VMAT can potentially result in a better QOL for the patients. Though a significant number of patients with head and neck squamous cell carcinoma were treated with VMAT developed acute dysphagia at the time of treatment completion, it was transient. A larger cohort of patients coupled with a volume-based analysis of the dose received by critical structures would provide a clearer picture of the impact of dysphagia on QOL.