1. Background
Alcohol and drug use are considered among the major health problems. Based on the 2019 report of the United Nations Office on Drugs and Crime (UNODC), 35 million people worldwide had drug use disorders. This report also indicated that opioids were responsible for two-thirds of 585,000 deaths due to drug abuse in 2017. Globally, 11 million people injected drugs in 2017, of whom 1.4 million live with human immunodeficiency virus and 5.6 million with hepatitis C (UNODC, 2019).
In recent years, therapists and researchers have used mindfulness training, either alone as an independent treatment or in combination with other therapies, to treat patients with drug use disorders (1) because these patients have lower levels of mindfulness than normal ones (2). Mindfulness is defined as the non-judgmental awareness and observation of one’s feelings, thoughts, and behaviors as they are happening (3). When individuals pay attention to their emotions, feelings, and thoughts, they observe themselves without judgment and focus on the present. Mindfulness-based treatments help individuals pay attention to their thoughts and feelings without caring about the content (4). One of the challenges of addicts is coping with their unpleasant experiences, thoughts, and feelings because they assume these thoughts and feelings as a part of their existence (3). Theoretically, mindfulness and accepting the existing experience allow the individuals not to respond to cravings immediately but experience them until gradually decreasing and disappearing. This gives individuals the ability to experience pain and negative emotions without overreacting, which often leads to impulsive behaviors, such as drug abuse (4).
Shame is one of the most critical negative emotions that can evoke impulsive behaviors, such as drug abuse (5). It is a self-conscious emotion defined as a negative and pervasive feeling about oneself in response to mistakes and defects (5). Shame is characterized by a generally negative evaluation of oneself (6). Research evidence suggests that shame is associated with drug use disorders.). Dearing et al. (5) indicated a positive relationship between shame proneness and addiction to drugs and alcohol. This relationship can predict relapse in individuals with different levels of drug use disorders. The findings of Bilevicius et al. (7) showed that people with severe depression experienced higher levels of shame associated with increased alcohol abuse and gambling-related problems. Bilevicius et al. (8) reported that shame played a crucial role in the tendency to exhibit addictive behaviors.
Self-criticism is defined as ones’ negative evaluation of their mistakes, defects, and those characteristics that may cause disapproval or exclusion from society (9). Self-criticism is considered as a strategy to deal with defects (9). Research suggests that self-criticism is associated with a wide range of psychological problems, including anxiety, post-traumatic stress disorder, eating disorder, emotional dysregulation, and drug use disorders (10). Blatt et al. (11) showed that those addicted to opioids experienced significantly higher levels of self-criticism than normal individuals did. Moreover, people with high levels of self-criticism that use the drug are more likely to be addicted to opioids eventually.
2. Objectives
Mindfulness-based treatments focus on experiencing what is happening without any judgment and evaluation. Therefore, the question here is whether or not mindfulness, with an emphasis on no judgment and evaluation, can reduce the levels of shame and self-criticism, both of which involve self-evaluation. The present research tries to answer this question.
3. Patients and Methods
This quasi-experimental study had a pretest-posttest and follow-up design with the statistical population of men with opioid use disorder (OUD) visiting the Iranian National Center for Addiction Studies (INCAS) in 2018 - 2019. Based on the effect size obtained from the interventions in previous studies (e.g., 0.66 reported by Louma in 2012) (12), the sample size in each group was estimated to be 15 using a power analysis (α = 0.05) and the analysis of covariance. Assuming an attrition rate of 20%, the final sample size was 36 (18 in each group). The participants were selected using convenience sampling.
The inclusion criteria were (1) being 20 - 45 years old, (2) having at least a high school diploma, (3) getting a negative urine test for opioid use, (4) meeting the diagnostic and statistical manual of mental disorders (DSM)-5 criteria for OUD, and (5) signing the informed consent form. The non-inclusion criteria entailed (1) the exhibition of psychotic symptoms based on the report of the psychiatrist at the INCAS; (2) affliction with organic brain syndrome based on the report of the psychiatrist or the physician at the INCAS; (3) serious suicidal thoughts based on the psychiatric interview; and (4) meeting the full criteria for personality disorder (borderline and antisocial personality) based on a diagnostic interview or at the discretion of the clinical psychologist based on the DSM-5 criteria. Moreover, the only exclusion criterion was absence from more than three treatment sessions. Finally, 9 participants were excluded from the study.
The remaining 27 participants were randomly divided into two groups as 12 in the mindfulness-based relapse prevention (MBRP) + treatment as usual (TAU) group and 15 in the TAU group. The participants in the TAU group were treated with routine care, including the administration of methadone and buprenorphine, individual or group therapies, and family training provided by addiction rehabilitation centers. Those in the MBRP group, in addition to routine care, attended eight sessions of MBRP, which is a combination of mindfulness meditation and cognitive-behavioral skills to prevent relapse. This intervention helps addicts raise their awareness of stimuli causing relapse and improve their automatic and habitual reactions to such stimuli (13). This research was approved by the Ethics Committee of the Department of Research and Technology of Shahid Beheshti University (IR.SBU.REC.1399.008) and was registered in the Iranian Registry of Clinical Trials (IRCT) (IRCT20170702034844N5).
3.1. Data Collection Tools
Other as Shamer Scale (OAS): This self-report questionnaire was developed by Goss et al. to measure one’s overall judgments about how others evaluate them. Goss et al. (14) developed this scale based on three major components: the feeling of inferiority, feeling of emptiness, and being ashamed for making mistakes. Cronbach's alpha of this scale was 0.92 in the present study. Foroughi et al. (15) studied the factor structure and psychometric parameters of the Iranian version of this scale and assessed its divergent and convergent validity about perfectionism, negative emotion, and self-compassion.
Forms of Self-Criticizing/Attacking and Self-Reassuring Scale (FSCRS): This scale was developed by Gilbert et al. (16) to determine the level of self-criticism and the ability to self-reassure when one faces problems. It consists of 22 items in the three subscales of inadequate-self (IS), hated-self (HS), and reassured-self (RS) that are scored based on a 5-point Likert scale. Cronbach's alpha coefficient of 0.9 has been reported for this scale. Its construct validity was assessed by comparing it with the Levels of Self-criticism (LOSC) Scale (17). Correlation analysis showed a significant relationship between these two scales. In addition, internalized self-criticism in the LOSC scale revealed correlations with IS (0.77), HS (0.57), and RS (-0.45) in the FSCRS (16).
4. Results
Demographic information of the participants is presented in Table 1. There was no significant difference between groups in terms of the demographic variables.
a Differences between groups in the demographic variables based on the results of the chi-square analysis
b Values are expressed as mean ± SD.
Descriptive statistics (mean and standard deviation) of research variables are shown in Table 2.
| Variables | TAU | TAU + MBRP |
|---|---|---|
| Shame | ||
| Pretest | 43.8 ± 18.52 | 29.08 ± 12.33 |
| Posttest | 45.27 ± 15.66 | 29.17 ± 15.07 |
| Follow-up | 39.23 ± 15.57 | 24.5 ± 12.04 |
| Inadequate self | ||
| Pretest | 23.27 ± 5.81 | 22.17 ± 7.86 |
| Posttest | 23.66 ± 5.64 | 21.67 ± 8.09 |
| Follow-up | 22.97 ± 5.46 | 19.25 ± 7.47 |
| Reassured self | ||
| Pretest | 19.13 ± 4.78 | 23.67 ± 8.74 |
| Posttest | 17.47 ± 5.34 | 20 ± 8.16 |
| Follow-up | 18.02 ± 4.42 | 18.02 ± 4.42 |
| Hated self | ||
| Pretest | 6.93 ± 1.79 | 7.91 ± 1.73 |
| Posttest | 6.07 ± 1.94 | 3.92 ± 1.16 |
| Follow-up | 5.28 ± 1.67 | 3.75 ± 0.96 |
aValues are expressed as mean ± SD.
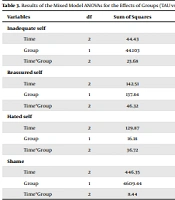
A mixed-design analysis of variance (ANOVA) was used to test the following research hypotheses: “MBRP group therapy is more effective than TAU alone in reducing the feeling of shame in individuals with OUD” and “MBRP group therapy is more effective than TAU alone in reducing self-criticism in individuals with OUD” (Table 3).
| Variables | df | Sum of Squares | Mean Square | F | P Value | Effect Size | Power of Test |
|---|---|---|---|---|---|---|---|
| Inadequate self | |||||||
| Time | 2 | 44.43 | 22.21 | 1.12 | 0.331 | 0.04 | 0.24 |
| Group | 1 | 44.103 | 44.103 | 1.1 | 0.314 | 0.04 | 0.17 |
| Time*Group | 2 | 23.68 | 11.84 | 0.6 | 0.498 | 0.02 | 0.14 |
| Reassured self | |||||||
| Time | 2 | 142.51 | 71.25 | 2.54 | 0.091 | 0.09 | 0.48 |
| Group | 1 | 137.84 | 137.84 | 2.49 | 0.134 | 0.09 | 0.33 |
| Time*Group | 2 | 46.32 | 23.16 | 0.82 | 0.445 | 0.03 | 0.18 |
| Hated self | |||||||
| Time | 2 | 129.87 | 64.93 | 38.62 | 0.001 | 0.61 | 1 |
| Group | 1 | 16.18 | 16.18 | 3.65 | 0.057 | 0.13 | 0.45 |
| Time*Group | 2 | 36.72 | 18.36 | 10.92 | 0.001 | 0.3 | 0.99 |
| Shame | |||||||
| Time | 2 | 446.35 | 223.17 | 5.92 | 0.005 | 0.19 | 0.59 |
| Group | 1 | 4609.44 | 4609.44 | 7.43 | 0.011 | 0.23 | 0.74 |
| Time*Group | 2 | 8.44 | 4.22 | 0.11 | 0.898 | 0.004 | 0.07 |
Our results showed that none of the intergroup, intragroup, and interactive sources of variation in IS and RS were statistically significant (P > 0.05), whereas the study stages (F = 32.62 and P = 0.001) and group-stage interaction (F = 10.92 and P = 0.001) were statistically significant sources of variation in HS. Bonferroni's method was utilized to examine the points of difference in the test stages for HS. The findings of the current study indicated that the mean HS significantly decreased in the posttest and follow-up stages compared to the pretest (P = 0.05).
Considering the significance of the group-stage interaction, the two groups were significantly different, at least in one of the study stages. Therefore, an independent t-test was used to investigate the points of difference. The results demonstrated no significant difference between the two groups in pretest (t = -1.4, P = 0.16), whereas posttest (t = 3.37, P = 0.002) and follow-up (t = -2.83, P = 0.009) mean scores of those who received a combination of MBRP group therapy and TAU were significantly lower than those treated with only TAU. In terms of shame, the results in Table 2 show that the differences between study stages (F = 5.92, P = 0.005) and the groups (F = 7.43, P = 0.01) were statistically significant. In addition, the results of Bonferroni's method indicated that the mean score of shame significantly decreased in follow-up compared to the pretest and posttest stages (P = 0.05). The findings generally suggested that the combination of MBRP group therapy and TAU was significantly more effective than TAU alone (P = 0.05).
5. Discussion
The results of the present study showed that MBRP group therapy was more effective than TAU in reducing the feeling of shame. This finding is consistent with previous studies (12, 18-23). However, the obtained results are not consistent with those reported by Proeve, Anton, and Kenny (24), who investigated the effectiveness of mindfulness-based cognitive therapy (MBCT) on shame, self-compassion, and psychological distress in anxious and depressed individuals. They reported that MBCT reduced internal shame, measured by self-conscious emotions, but could not affect external shame. One reason for these contradictory results may be the difference in the statistical population. Proeve et al. (24) investigated anxious and depressed individuals, whereas the study population of the current research consisted of individuals with OUD. Moreover, there were differences between these two studies in terms of treatment protocols. Proeve et al. (24) applied MBCT, while we used MBRP group therapy, designed specifically for people with drug use disorders and emphasizes the factors associated with negative emotions associated with the feelings of shame, which are prevalently observed in individuals with drug use disorders.
These findings can be attributed to the fact that individuals with drug use disorders experience higher levels of shame because of the labels given by society as addicts, along with their failure in controlling drug abuse and playing their familial and social roles correctly. They try to avoid this annoying feeling in order to reduce the pain and suffering it causes. Unfortunately, when one tries to avoid shame, this attempt will increase and accumulate shame in the long run, even though it may make the person feel calm and free in the short run. Although negative self-perceptions are annoying, direct efforts to change them can backfire and augment their frequency and strength (12). The present study and other similar research demonstrate that mindfulness-based interventions can help individuals get rid of the repetitive cycle of avoidance and shame and replace avoidance with acceptance. Shame is a feeling associated with maladaptive self-focus attention, whereas mindfulness-based interventions emphasize what is happening at the moment without any judgment. Mindfulness helps individuals consider negative emotions, including shame, less threatening and upsetting. These are experienced realistically without taking into account any presuppositions or giving them any special meaning (13).
Our results are consistent with the findings of Gilbert (4) and Shahbazi et al. (25), who reported that mindfulness could be effective in reducing self-criticism. However, no study in the literature separately investigated the effects of mindfulness-based therapies on HS, RS, and IS. To explain these results, it is better first to clarify the meaning of these subscales. The IS refers to an inner feeling of being inadequate and underestimating oneself because of failures and obstacles. In other words, the individuals who feel inadequate, think they deserve to criticize themselves and are disappointed. As the opposite of IS, the RS demonstrates one's feeling of self-love and positive views on themselves. The HS refers to a destructive response caused by failures and obstacles based on self-hatred. This component involves hatred and an aggressive and sadistic view of oneself to the extent that one may even choose to harm oneself (16).
Mindfulness helps such individuals learn to love themselves. For instance, in one of the exercises of this intervention, titled "compassionate meditation", individuals learn to have a kinder and more permissive view of themselves because it is a prerequisite for loving their loved ones. Mindfulness teaches people that thoughts are merely thoughts and not facts, and they learn to disregard negative thoughts about themselves and not get involved in these thoughts entering their minds (13, 26).
5.1. Conclusions
The results showed that MBRP could be considered as an effective therapeutic approach to reducing shame and self-criticism in individuals with OUD. Shame and self-criticism are considered risk factors for substance use and relapse. Therefore, mindfulness-based therapies are considered one of the influential therapies for people with addiction and substance use disorders who have high levels of shame and self-criticism.
5.2. Limitations
The generalizability of the results of the current study is limited due to the study population being limited to the INCAS and the small sample size.