1. Introduction
In the research carried out by Harmon on patients swallowing foreign objects, she concluded this is a self-harming behavior of which 79 percent of these patients suffered from at least one psychiatric disorder (1).
Even though there have been several reported cases of intentional swallowing (personal correspondences, 2004 - 2005) seen by liaison psychiatrists, remarkably, most of these reports are published in surgical and gastroenterological journals focusing on the physical damages of the swallowed object rather than the psychiatric characteristics of the patients. The patients reported from the psychiatric point of view divulges that patients with this behavior could be placed in four categories: Pica, personality disorder, malingering, and psychosis (2).
Malingering as a way to contact health services and receive clinical attention repeatedly seems to happen in prisons and mental health wards (3). Furthermore, foreign object ingestion is behavior among people with personality disorder as a parasuicidal behavior which, unfortunately, identical to self-injurious behavior, is recurring and resistant to treatments (4) and finally, psychotic patients, as the result of their delusions or hallucinating commands, may swallow nonfood objects which according to Velitchkov's et al. study in 1996 could be around 23 percent of object swallowing patients (5).
The death result of zinc intoxication after swallowing 461 coins in one patient (6) and the requirement of aggressive treatment for lead poising due to swallowing 206 bullets by another (7), both with a schizophrenia diagnosis, shows that out of the four categories mentioned above, the latter group is remarkable for the high count of items swallowed.
Often the swallowed foreign bodies (80 - 90%) are spontaneously disposed of, 10 - 20% of cases require endoscopy to remove the foreign body, and less than 1% require surgery to remove the foreign body or treatment of its complications (8).
The presented patient is a case with psychiatric disorders who have swallowed sharp and dangerous foreign bodies and undergone laparotomy twice to remove the foreign bodies and their complications.
2. Case Presentation
The patient is a 17-year-old girl hospitalized in the poisoning intensive care unit of Afzalipour Hospital due to deliberate poisoning with pills in July 2019. She was then transferred to the psychosomatic medicine ward. Her history contains repeated self-harming behaviors that intensified the month before her admission. She was hospitalized twice due to deliberate pill poisoning and admitted twice to the Surgery ward as the result of swallowing a knife blade and a razor blade. She also had a history of self-cutting on her upper limbs and swallowing a gold chain in the month before her admission such that in the physical examination, their scars are observed as some irregular lines from her right forearm to the right arm. The hospital is the main general hospital of the city, with more than 462 beds, and the only hospital with a psychosomatic medicine ward in Kerman, southeast of Iran.
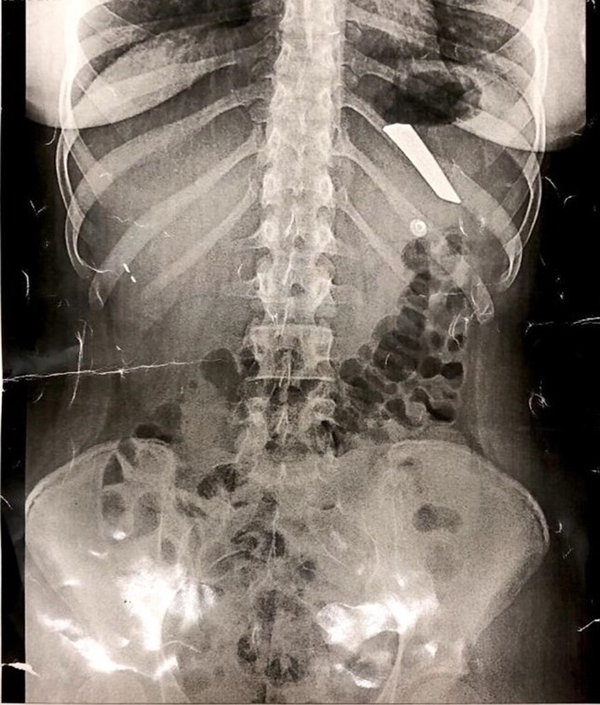
The patient swallowed knife blades three times during the year before her admission. The patient had detached the knife blade, which measured around 9 cm in length and 1.5 cm in width, from its haft, and swallowed it at first; it had been disposed of while under close observation and serial radiography X-ray (Figure 1).
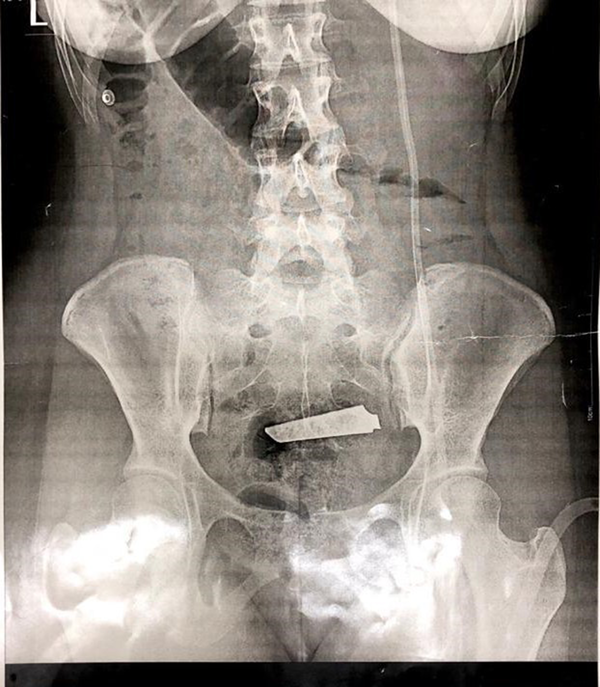
The second time, the patient was observed for two days, but due to sigmoid rupture and damage to the left ovary, the patient underwent a laparotomy not only to remove the knife but also to repair the left ovary and sigmoid (Figure 2).
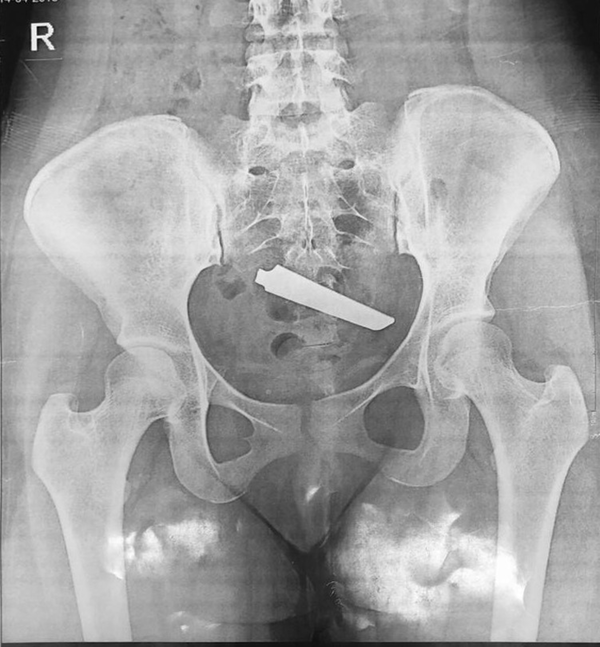
The third time, a month before her admission in June 2019, the patient underwent a laparotomy, and the knife blade was removed (Figure 3) and a week after her discharge, she again swallowed a razor blade, which was not perceived in the patient's x-ray while she was under supervision; she reported that the razor blade was spontaneously disposed of the next day. Generally, the patient began to swallow foreign objects when she was 14 years old, and on average, every year, she swallowed 9 foreign bodies, including coins, a Gold chain, Razor, and knives.
The patient is the youngest child of a family with two other siblings. At birth, she was delivered by cesarean section, her mother had a difficult labor, and she was distressed at delivery. She had normal growth and development, and her physical appearance was short and thin. In childhood, she had limited relationships with her peers and never had a close friend. Her parents divorced when she was 6 years old, and the patient lives with her mother and 2 sisters. The patient's father and aunt have been hospitalized several times for psychiatric disorders. Her father started working as a teacher when he was young, but he was not functional, and as a result, he was given an admin job in school and made redundant shortly after while her mother was a school driver. During her childhood, while her mother was at work, she was physically abused by her father several times and witnessed her father's suicide, asking her to plug in the wires connected to his body to the electricity main. According to her mother's testimony, her father had mood swings, breakouts, suicide attempts, and decreased functionality and was diagnosed with major depression and personality disorder. Due to her learning difficulties, the patient continued her education with supportive education, and the onset of the disease exacerbated her learning difficulties.
At the age of 13, the patient suddenly developed depression, anxiety, severe restlessness, and loneliness, and ran away from home, she underwent treatment with the diagnosis of type 1 bipolar disorder, and it was noted and confirmed by the patient that before beginning the symptoms, she had a history of sexual abuse -touching her breasts- by an unknown man. Despite therapy with multiple mood stabilizers (sodium valproate and lithium), antipsychotics (haloperidol, risperidone, and tranqopine), hospitalization, and electroconvulsive therapy (13 and 8 sessions) since the onset of the disease, however, she did not respond well to therapy. One year after the onset of the disease, she demonstrated rapid mood swings, frequent home runs, and self-harming behaviors such as taking detergents, and pills, self-immolation, and swallowing foreign objects. Before these activities, the patient became restless and was momentarily relieved.
The patient reported having a lover with unilateral love from the onset of the illness, whereas their relationship is limited to telephone calls from her which, according to her, have always been rejected by the other party, and she was treated as an intruder. She repeated the lover's notion in every visit and said, "I called him many times, but he told me not to call again and hung up the phone even at once he told me that he had got married and not to call him again". She had not seen the aforementioned lover of her relatives, and the patient often attributes her restlessness to being rejected by her loved one. She mentions that she doesn't swallow foreign bodies to commit suicide, and after these activities, she always calls the emergency department for help. Although she does not appear to be trying to deliberately kill herself, there is always the possibility of death by mishap.
The patient has no clear history of hallucinations and delusions, but during her admission to the psychosomatic ward, she was anxious and restless, and fearful of being threatened by red-eyed people disguised in lion covers to harm her. The patient also shows poor concentration and flight of ideas while talking, an inability to interact with others, and decreased executive functionality during admission. The patient was prescribed clozapine, starting initially at 12.5 mg daily. Due to its adverse effects, she couldn't tolerate more than 100 mg daily. The patient was discharged once she reached the intended dose of medicine, and after her discharge, she adhered to her regular visits and medications. She was offered psychotherapy sessions but unfortunately didn't attend.
She was followed up for about 2 years. She had better verbal communication with others and even went to university. Her suicidal behavior and attempts reduced noticeably after starting Clozapine treatment but were re-admitted after deliberate poisoning with clozapine due to her rejection from her loved one five months later. Nevertheless, there has been no report of foreign objects ingestion to date.
3. Discussion
Gitlin et al. reported 5 patients, where 3 swallowed sharp metal razors while the other 2 swallowed pens and pencils (2). Similar to the patients in this article, all 5 cases were females under 34 years old with psychiatric disorders, a hospitalization history, and self-injury. Contrary to our patients who underwent laparotomy twice, none required surgery to remove the foreign body.
In another study, a 43-year-old man diagnosed with depression was reported swallowing a knife blade to commit suicide, and similar to the patient, in this case, the blade of the knife was removed by laparoscopy, and he started antipsychotic therapy (9). Contrary to the reported case, this behavior was not repetitive and was intended to be suicidal, and there were no complications as a result of swallowing the knife blade. In Gitlin et al. article on the case report, it has been demonstrated that there is an emptiness feeling and tension before self-destructive behaviors such as swallowing a foreign object that shows the importance of psychiatric support in these patients (2).
Swallowing foreign bodies is a complex process that can lead to serious complications if not properly managed, and timely psychiatric consultation and supportive therapy for these patients are essential. The patient in this article, as a result of swallowing knife blades, suffered serious complications such as ovarian rapture and sigmoid that, according to our knowledge, is the first case of ovarian rapture that required the laparotomy procedure twice and left the patient's abdomen two scars as the result of horizontal and vertical incisions.
Self-harming patients who frequently harm themselves incur a high cost of medical care for the health system and could be expensive for caregivers economically and psychologically. Due to the nature of this behavior, it is common for these patients to exhibit severe anger and emotional instability, often stemming from a history of childhood physical or sexual abuse, as well as deprivation (2).
In the reported patient, there is deprivation regarding unstable family conditions and economic problems and reported sexual abuse. Swallowing foreign bodies is interpreted as both self-punishment and punishing others) those who thought they were hurt or may be blamed for their despair or rejection (while different forms of self-harm exist and are dangerous to the patient's health and uncomfortable for the therapist, the main difference between swallowing foreign objects and other self-harming methods is that swallowing foreign bodies has no external signs, and the patient is exposed to uncertain dangers in the future. It has serious risks of gastrointestinal rupture until it is disposed of, requiring further attention from the therapeutic system and caregivers.
Regarding the reported patient dynamics, it can be said that by describing unilateral love, she must be loved and more attention since she fails to achieve this goal, which damages her mother's and others' self-esteem.
The role of hospitalization for these types of patients is controversial. Brief psychiatric hospitalization may be reasonable to protect the patient against suicide and psychological symptoms, to save others from injury, or when the patient experiences acute stressful life events (10).
Specifically, for the patient in this report, a short admission to eliminate the effects of suicide and reach medical stability was necessary; besides, the patient was quickly discharged as soon as the Clozapine dose reached its peak, so she would not become dependent on the hospital. Her suicidal behavior and attempts decreased significantly after starting clozapine treatment. It seems that clozapine treatment can effectively reduce suicidal behavior and self-harm in this case. A study conducted by Wimberly et al. found that the rate of self-harming episodes was higher in non-clozapine antipsychotic treatment periods and significantly lower in clozapine treatment periods (11). In another study, the average dose of 125 mg/day of clozapine decreased self-injurious behavior among a prison population (12). Therefore, clozapine treatment is recommended for patients with repeated suicidal behavior and self-harm.
Although she did not attend psychotherapy sessions, she responded and cooperated in organized and formal telephone calls by psychiatry residents, which effectively prevented her from serious self-harming activities.
Reports suggest that the intentional swallowing of foreign objects behavior is more resistant than other self-harming activities and may have a worse prognosis. If the swallowing behaviors indicate a higher severity psychiatric disease, that will help explain the prognostic dissimilarity in these individuals.
The strength of this case study is that it allows researchers to witness and record information about this rare case of object swallowing. Furthermore, it helps clinicians to create suggestions for future studies. One limitation was the patient's lack of full cooperation in attending the outpatient setting punctually. Findings from this case report cannot be generalized, demanding further surveillance and research.