1. Introduction
Oral squamous cell carcinoma (OSCC) remains a significant global public health concern, with tobacco use as a primary risk factor. Among various forms of tobacco consumption, naswar—a smokeless tobacco mixture prevalent in Southeast Asia, Sri Lanka, Bangladesh, India, and nearby regions, including southeastern Iran—has garnered attention due to its strong association with oral cancer (1, 2).
Naswar consists of ground tobacco leaves, slaked lime, and occasionally flavoring agents. When placed intra-orally, it releases a potent mix of chemicals upon contact with saliva. This blend includes carcinogenic nitrosamines, nicotine, and other toxic compounds, which are readily absorbed through the oral mucosa (3).
Despite the well-documented risks of oral cancer associated with naswar use, including its high concentrations of carcinogenic nitrosamines and nicotine, many individuals continue its consumption. The adverse effects of naswar extend beyond oral health, contributing to systemic conditions such as cardiovascular diseases, gastrointestinal disorders, and reproductive health issues. Chronic use has been directly linked to oral mucosal lesions, periodontal disease, and a significantly heightened risk of oral cancer, highlighting its profound impact on public health (4, 5).
This study not only highlights a critical clinical scenario but also underscores the urgent need for tailored strategies to address the challenges posed by naswar-related oral cancers in affected populations.
2. Case Presentation
A 62-year-old woman presented to the Maxillofacial Surgery Department of Zahedan University of Medical Sciences in January 2024 with a longstanding history of naswar consumption spanning 40 years. She was referred from the oncology department due to a suspected squamous cell carcinoma (SCC) located on the right side of her face.
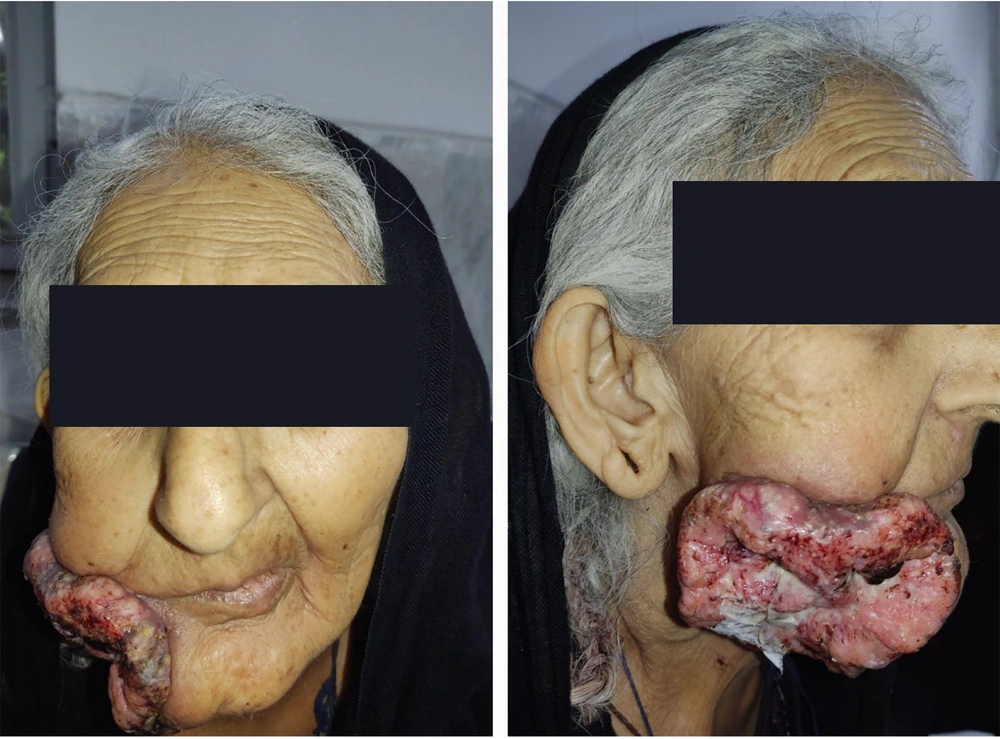
The patient reported progressive lesions dating back 3 - 4 years. She denied any systemic or allergic diseases but experienced consistent, severe facial pain. Clinical examination revealed a lesion measuring 10 by 15 centimeters, affecting both the oral mucosa and skin on the right mandible (Figure 1). The patient stated that the lesion initially grew slowly but later progressed rapidly. The lesion appeared naturally colored in the oral mucosa and had a soft texture. Over the past six months, the patient had developed paresthesia on the right side of her face, attributed to involvement of the inferior alveolar nerve.
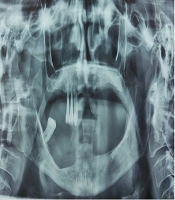
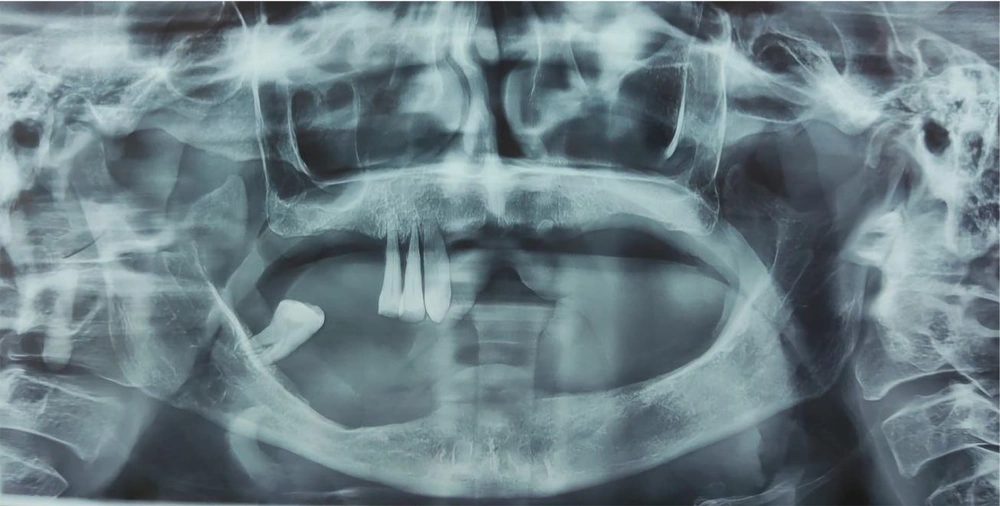
The patient’s oral hygiene was severely compromised, with generalized oral mucosal inflammation and severe periodontitis. Panoramic imaging (OPG) showed severe bone resorption in the mandibular body region on the right side, accompanied by osteolytic lesions indicative of the aggressive and destructive nature of the carcinoma (Figure 2). Apart from four teeth, the patient had lost all her teeth, which could not be retained due to significant bone resorption.
A biopsy sample measuring 0.5 by 0.5 centimeters was obtained from the buccal mucosa on the right side of her mouth after local anesthesia administration and sent for pathological analysis. The diagnosis confirmed high-grade SCC.
Further assessment revealed significant progression of the carcinoma, involving adjacent tissues and displaying high histological grade features consistent with a poor prognosis. Imaging studies confirmed infiltration into deeper tissues, including the maxilla and surrounding structures. Additional investigations identified metastatic spread to the chest, indicating advanced disease progression.
After extensive discussions with the attending oncologist and surgical team, the patient was presented with treatment options, including surgical resection and adjuvant therapy. Given the advanced stage of the disease, the potential complications of surgery, and the poor prognosis, the patient opted against surgical intervention. Her decision was influenced by concerns about postoperative recovery, quality of life considerations, and the perceived limited benefits of aggressive treatment at this stage.
3. Discussion
The widespread use of naswar continues in various regions, driven by cultural traditions, socio-economic factors, and perceived medicinal benefits. Addressing its public health impact requires a comprehensive approach encompassing prevention, early detection, and cessation efforts. Public health campaigns emphasizing education, awareness, and behavioral interventions are essential to alter cultural attitudes and discourage initiation, particularly among vulnerable groups such as youth and women. Ensuring access to healthcare services for the early detection and management of oral lesions associated with naswar use is critical. Targeted screening programs for high-risk populations can facilitate early diagnosis of oral cancer, potentially improving treatment outcomes and reducing the disease burden (2, 6, 7).
Despite growing awareness of its health risks, challenges in curbing naswar use persist due to deeply rooted cultural norms, limited healthcare resources, and economic disparities. Longitudinal studies are needed to comprehensively understand the cumulative health impacts of lifelong naswar consumption and to inform evidence-based interventions. Future research should also explore alternative strategies, such as harm reduction approaches and pharmacological treatments, to support cessation efforts. Collaboration among healthcare providers, policymakers, and community leaders is vital for implementing culturally sensitive interventions that respect diverse cultural practices while promoting public health. The continued consumption of naswar presents a multifaceted public health challenge, with significant risks to oral and systemic health. Addressing this issue necessitates coordinated prevention, early detection, and cessation strategies to mitigate its impact on affected populations (1, 5, 8).
This case report underscores the challenges in managing advanced squamous cell carcinoma resulting from prolonged naswar use. The established correlation between naswar consumption and oral malignancies highlights the urgent need for public health initiatives aimed at reducing its prevalence. Furthermore, the case emphasizes the importance of patient-centered care and shared decision-making in oncological practice, particularly when dealing with complex clinical scenarios and poor prognostic indicators. By analyzing this case, we underscore the significance of comprehensive patient education, culturally sensitive cessation interventions, and the critical role of interdisciplinary collaboration in managing complex cases of oral cancer associated with smokeless tobacco use.