1. Background
The coronavirus disease 2019 (COVID-19) pandemic is a serious public health concern worldwide. The virus was first documented in some cases of unexplained pneumonia in December 2019. The mechanism of infection and the subsequent manifestations are still not proven and not very clear (1).
Coronavirus is an RNA virus isolated and named for the first time in the 1960s. Currently, there are seven known coronavirus subtypes that can infect humans, and four subtypes are responsible for the pathogenesis of human common colds, which usually do not cause a serious illness (2).
It is well-documented that the virus can cause mainly respiratory symptoms, but the newly emerging data suggest that the virus can cause many system involvements such as gastrointestinal, musculoskeletal, neurological, vascular, hematological, and other manifestations (3).
Molecular diagnosis of COVID‐19 infection is usually done adopting the reverse transcription polymerase chain reaction (RT-PCR) by nasopharyngeal swab. Other methods that are suggestive of the diagnosis include the typical chest CT scan findings, which include widespread lung fibrosis distributed mainly at the peripheral zones (4).
Many classifications have been proposed for infected individuals based on clinical manifestations. Some affected individuals are asymptomatic carriers with no clinical and even radiological manifestations of the disease. Other patients may manifest respiratory manifestations of the disease with variable degree of lung infection and lung fibrosis, and other patients have severe disease or critical disease manifestations in which patients have multisystem infection. Depending on different clinical manifestations, some patients require no hospitalization, while others may need hospitalization or admission to the intensive care unit (ICU). It is estimated that around 20% of patients develop critical illness and the mortality range varies from 1% to 30% (1, 5).
The mortality rate of COVID‐19 is lower than severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS), but COVID‐19 is more lethal than seasonal flu with high complication rates, particularly in those with comorbidities (3).
Many complications have been reported, such as lung damage, post-viral asthenia, fulminant myocarditis, and disseminated intravascular coagulopathy (3).
Assessment of the blood parameters showed that infected patients with COVID-19 have various alterations in the blood parameters, particularly those with severe clinical course. The most common documented changes in the blood parameters include changes in the white blood cells (WBC), particularly neutrophils, lymphocytes, and platelets (1, 4).
2. Objectives
This study aimed to detect the most common changes in the blood parameters in COVID-19 patients and compare them with healthy individuals.
3. Methods
In this study, 350 individuals were grouped into two equal groups of COVID‐19 patients and healthy controls with negative history of medical problems and COVID-19 test. Patients with COVID-19 were diagnosed by RT-PCR on a smear taken from the nasopharynx and/or throat.
Under full aseptic technique, about 2.5 mL of whole blood was placed in an EDTA tube then placed on a mixer for about 5 minutes. Blood parameters were then estimated by performing CBC using automated hematology analyzer Sysmex XP300® Japan.
3.1. Reference Values
The reference values were estimated according to the World Health Organization (WHO) reference values (Table 1) (6, 7).
| Parameter | Normal Value | Elevated | Reduced |
|---|---|---|---|
| Hemoglobin (D/L) | |||
| Males | 13.5 to 17.5 | > 17.5 | < 13 |
| Females | 12.0 to 15.5 | > 15.5 | < 12 |
| WBC | 3 - 11 × 109 /L | > 11 × 109 /L | < 3 × 109 /L |
| Neutrophils | 1.5-7.5 × 19 /L | > 7.5 × 19 /L | < 1.5 × 109 /L |
| Lymphocytes | 1-3.5 × 19 /L | > 3.5 × 19 /L | < 1.0 × 109 /L |
| Monocytes | 02 - 1 × 19 /L | > 1.0 × 19 /L | < 0.2 × 19 /L |
| Eosinophils | 0.02 - 0.5 × 119 /L | > 0.5 × 19 /L | < 0.02 × 119 /L |
| Platelets | 150 - 450 × 19 /L | > 450 × 109 /L | < 150 × 109 /L |
4. Results
The mean age of patients involved in this study was 53.73 years (males: 52.57%). Middle-aged patients constituted about 55.43% of participants, elderly patients 26.29%, and young patients 18.29%.
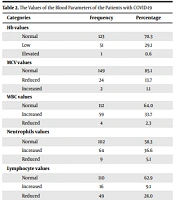
Blood analyses were done for the patients, and the results of the investigations are shown in Table 2.
| Categories | Frequency | Percentage |
|---|---|---|
| Hb values | ||
| Normal | 123 | 70.3 |
| Low | 51 | 29.1 |
| Elevated | 1 | 0.6 |
| MCV values | ||
| Normal | 149 | 85.1 |
| Reduced | 24 | 13.7 |
| Increased | 2 | 1.1 |
| WBC values | ||
| Normal | 112 | 64.0 |
| Increased | 59 | 33.7 |
| Reduced | 4 | 2.3 |
| Neutrophils values | ||
| Normal | 102 | 58.3 |
| Increased | 64 | 36.6 |
| Reduced | 9 | 5.1 |
| Lymphocyte values | ||
| Normal | 110 | 62.9 |
| Increased | 16 | 9.1 |
| Reduced | 49 | 28.0 |
| Monocytes values | ||
| Normal | 131 | 74.9 |
| Increased | 20 | 11.4 |
| Reduced | 24 | 13.7 |
| Eosinophil values | ||
| Normal | 34 | 19.4 |
| Increased | 4 | 2.3 |
| Reduced | 137 | 78.3 |
| Platelets values | ||
| Normal | 130 | 74.3 |
| Increased | 6 | 3.4 |
| Reduced | 39 | 22.3 |
Comparison of different blood parameters was done between the cases and controls, and the correlation was estimated in terms of P-values. There was a significant correlation between all the blood parameters and infection with COVID-19 (Table 3).
| Categories | Study Population | Significance | |
|---|---|---|---|
| Patients (n = 175) | Controls (n = 175) | ||
| Age groups | 0.000 b | ||
| Young age | 32 (18.3) | 78 (44.6) | |
| Middle age | 97 (55.4) | 84 (48.0) | |
| Elderly | 46 (26.3) | 13 (7.4) | |
| Hb values | 0.000 c | ||
| Normal | 123 (70.3) | 174 (99.4) | |
| Low | 51 (29.1) | 0 (0.0) | |
| Elevated | 1 (0.6) | 1 (0.6) | |
| MCV values | 0.000 c | ||
| Normal | 149 (85.1) | 175 (100.0) | |
| Reduced | 24 (13.7) | 0 (0.0) | |
| Increased | 2 (1.1) | 0 (0.0) | |
| WBC values | 0.000 c | ||
| Normal | 112 (64.0) | 171 (97.7) | |
| Increased | 59 (33.7) | 4 (2.3) | |
| Reduced | 4 (2.3) | 0 (0.0) | |
| Neutrophils values | 0.000 c | ||
| Normal | 102 (58.3) | 174 (99.4) | |
| Increased | 64 (36.6) | 1 (0.6) | |
| Reduced | 9 (5.1) | 0 (0.0) | |
| Lymphocyte values | 0.000 b | ||
| Normal | 110 (62.9) | 144 (82.3) | |
| Increased | 16 (9.1) | 29 (16.6) | |
| Reduced | 49 (28.0) | 2 (1.1) | |
| Monocytes values | 0.000 b | ||
| Normal | 131 (74.9) | 173 (98.9) | |
| Increased | 20 (11.4) | 0 (0.0) | |
| Reduced | 24 (13.7) | 2 (1.1) | |
| Eosinophil values | 0.000 c | ||
| Normal | 34 (19.4) | 148 (84.6) | |
| Increased | 4 (2.3) | 1 (0.6) | |
| Reduced | 137 (78.3) | 26 (14.9) | |
| Platelets values | 0.000 c | ||
| Normal | 130 (74.3) | 175 (100.0) | |
| Increased | 6 (3.4) | 0 (0.0) | |
| Reduced | 39 (22.3) | 0 (0.0) | |
a Values are expressed as No. (%) unless otherwise indicated.
b Pearson chi-Square test.
c Fisher's Exact test.
5. Discussion
The majority of cases infected with COVID-19 suffer from mild to moderate symptoms and recover with an appropriate medical care. Moreover, about 15 - 30% of the patients suffer from severe course of the disease, and the fatality rate may reach up to 15%. Acute respiratory distress syndrome (ARDS) is the leading cause of death in the majority of COVID-19 patients. One of the main causes of ARDS is the cytokine storm (cytokine release syndrome), a deadly and uncontrolled systemic inflammatory response caused by the release of excessive amounts of proinflammatory cytokines. The hematological parameters are usually prominent and more severe in patients with more severe clinical course (3, 8, 9).
There was a significant correlation between the age of patients and infection with COVID-19 (P = 0.000). Studies proved a similar relationship with the age (10).
The hemoglobin level of our patients was within the normal ranges in 70.3%, and reduced in 29.1% of cases. Most of the published studies suggested that the hemoglobin level has no correlation with the infection with COVID-19; however, the relation was positive in our patients when compared to the normal individuals (P = 0.000). Some authors suggested a positive relation with the infection, but its mechanism is still unclear. Patients with low hemoglobin may be at higher risk for infections, including viral infection; this point requires further evaluation and investigation.
The white blood cells (WBC) count is elevated in most patients infected with either bacteria or viruses, as a normal body response to systemic infection. In our patients, the WBC were elevated in 33.7% of the patients, while 64% of patients had WBC count within the normal range. The correlation was significant between the infection and WBC count (P = 0.000); the majority of the published studies found a similar correlation with the WBC count (11, 12).
Lymphopenia was reported in 28% of our patients, while lymphocytosis was seen in around 9.1% of them. There was a very significant correlation between the infection with COVID-19 and reduction in the lymphocytes count. The percentage of reduction in the lymphocyte count varies in different studies so that some authors reported that up to 80% of their patients had lymphopenia (3, 13).
Monocytopenia is one other manifestation of viral infections. In our patients, the majority of patients had normal monocytes count, monocytes were reduced in around 13% of cases, and increased in around 11% of them. There was a very significant association between the monocyte count and infection with COVID-19 (P = 0.000).
A meta-analysis study found that the severity of thrombocytopenia is also associated with the severity of the disease. The study also suggested that there is a sharp decline in the number of the platelets among the non-survivors. Among our patients, thrombocytopenia was diagnosed in 22.3% of COVID-19 patients, and 74.3% had normal reference values for platelets. The platelets count also showed a very significant correlation with the disease compared to non-infected individuals (P = 0.000) (3, 14).
5.1. Conclusions
COVID-19 infection is associated with multisystem symptoms and signs, and there are numerous laboratory abnormalities. An increased focus should be on changes in the blood parameters as valuable markers in suggesting the infection when the RT-PCR is negative. These parameters can give clues about the severity of the infection and predict the admission to the intensive care unit (ICU).