1. Introduction
Acute respiratory disease caused by COVID-19 was introduced by Coronavirus beta and first reported in China in 2019. It has spread rapidly worldwide and has become a pandemic. This disease mainly affects adults (1). The exact prevalence of COVID-19 in neonates is unknown, but the severe form of the disease has been reported more frequently in children younger than 1 year of age; however, in general, the severity of the disease is lower in children than in adults (2). It affects multiple body systems, including the cardiovascular, respiratory, gastrointestinal, nervous, dermal, hematologic, immunologic, renal, and hepatic systems.
Fever, agitation, cough, respiratory distress, diarrhea, and vomiting are the most common complaints among adults with COVID-19. Clinical signs of this infection in nonspecific neonates include temperature instability, acute respiratory syndrome, cardiovascular dysfunction, and gastrointestinal symptoms (3).
Pulmonary hemorrhage in children and neonates is associated with high mortality and has several causes. Pulmonary hemorrhage after COVID-19 pulmonary infection has been reported rarely (4).
However, it is associated with high mortality, and no effective treatment is known.
Because of the new manifestations of COVID-19 in neonates, in this study, four symptomatic neonates with COVID-19 and positive PCR results who were admitted to the neonatal intensive care unit of Firoozabadi Hospital with pulmonary hemorrhage were evaluated for clinical signs, radiological and laboratory findings, and their outcomes.
Our study defined pulmonary hemorrhage as fresh, continuous bloody fluid from the ETT in mechanically ventilated infants or gross hemorrhage from the lower airway during laryngoscopy when a newborn was intubated due to sudden clinical deterioration.
2. Case Presentation
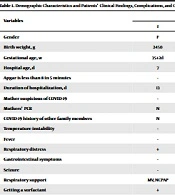
In the present study, we examined four neonates admitted to the neonatal intensive care unit of Firoozabadi Hospital, Iran University of Medical Sciences, Tehran, Iran. Their demographic characteristics and clinical findings are shown in Table 1, while their paraclinical findings, complications, and outcomes are summarized in Table 2.
| Variables | Case No. | |||
|---|---|---|---|---|
| 1 | 2 | 3 | 4 | |
| Gender | F | M | M | M |
| Birth weight, g | 2450 | 2350 | 1100 | 1135 |
| Gestational age, w | 35+2d | 36+2d | 28+3d | 28+3d |
| Hospital age, d | 7 | 1 | 1 | 1 |
| Apgar is less than 8 in 5 minutes | - | - | + | + |
| Duration of hospitalization, d | 13 | 11 | 6 | 3 |
| Mother suspicious of COVID-19 | - | - | + | + |
| Mothers’ PCR | N | - | + | + |
| COVID-19 history of other family members | N | N | N | N |
| Temperature instability | - | - | - | - |
| Fever | - | - | - | - |
| Respiratory distress | + | + | + | + |
| Gastrointestinal symptoms | - | - | - | - |
| Seizure | - | - | - | - |
| Respiratory support | MV, NCPAP | MV, NCPAP | MV | MV |
| Getting a surfactant | + | + | + | + |
| Pneumothorax | - | + | - | - |
| Duration of receiving antibiotics, d | 13 | 12 | 6 | 3 |
| Consequences | D | D | D | D |
Demographic Characteristics and Patients’ Clinical Findings, Complications, and Outcome
| Variables | Case No. | |||
|---|---|---|---|---|
| 1 | 2 | 3 | 4 | |
| Findings of echocardiography | MR | ASD, VSD, PDA | PDA, PFO | PDA, TR, ASD |
| CXR findings | Patchy and fluffy opacities | Patchy, linear opacities | Complete whiteout with just an air bronchogram visible | Ground-glass opacities; nodular densities |
| WBC | 4300 | 12800 | 6400 | 10500 |
| PMN, % | 35 | 80 | 32 | 20 |
| LYM, % | 53 | 13.7 | 59 | 74 |
| PLT/mm3 | 380000 | 292000 | 223000 | 205000 |
| CRP of the first day | 2 | 32 | .3 | 1 |
| COVID PCR | + | + | + | + |
Paraclinical Findings of Patients
Of these four neonates, two were near-term, and two were preterm. In premature neonates, the Apgar score was less than five minutes, requiring resuscitation at birth, and all but one neonate was admitted within the first 24 hours after birth. In these neonates, respiratory distress was the predominant sign of hospitalization.
All patients had elevated CRP levels during hospitalization. There was no evidence of involvement of other systems, such as the renal or neurological systems. None of the patients showed any signs of coagulopathy at admission.
All neonates received two doses of surfactant administered in the first 24 hours for preterm infants and the first 48 hours for the other two neonates. The average length of hospital stay was eight days, and in the end, all patients died of severe pulmonary hemorrhage.
This study was approved by the Research Ethics Committee of the Iran University of Medical Sciences (approval ID: IR.IUMS. REC.1401.310)
3. Discussion
In this study, we examined four newborns of mothers with COVID-19 (definite or suspected) who were treated in the neonatal intensive care unit of the Firoozabadi Hospital between March 2019 and August 2021. These newborns had pulmonary hemorrhage.
The incidence of pulmonary hemorrhage was the same in preterm and full-term neonates.
The most common symptom on admission to the hospital was respiratory distress (100%), and all patients required intensive ventilation, a finding consistent with that of other studies (2).
The concomitant involvement of the kidneys (AKI) and pulmonary involvement (pulmonary hemorrhage) after COVID-19 infection have been reported in case studies of adults with vasculitis, particularly necrotizing polyangiitis (5, 6); however, none of the neonates had neurologic symptoms and did not show involvement of the kidneys or other organs.
COVID-19 was not detected in family members, and maternal PCR was positive in two cases. These results confirm the transmission of the disease from asymptomatic individuals or postpartum transmission of the disease to newborns, which is also consistent with the results of De Bernardo et al. (7).
Lung CT examinations were not performed in any of our newborns, and the most common abnormal radiographic finding of the lungs was in patients with RDS (100%); pneumothorax was observed in one newborn. The most common finding on CT scans and lung radiographs in patients with COVID-19 is grand glasses with or without pulmonary consolidation (8).
In children with COVID-19, lymphopenia was also found in 75% of patients (9); however, this finding, indicative of disease severity, was found in only 25% of our newborns. Myocarditis, pericarditis, and arrhythmias are among the myocardial infarctions reported in children with COVID-19 (10, 11). In the present study, this type of heart disease was not detected in any of the newborns, but at least one congenital heart disease, such as PFO, ASD, VSD, and PDA, was detected in 100% of the newborns. In contrast, pulmonary hypertension was not detected in any of the newborns. In addition, all neonates received two doses of surfactant, which had no beneficial effects.
Although it was not possible to assess the overall outcome of pulmonary hemorrhage in neonates with COVID-19 because of the small sample size of our study, we can claim that the overall outcome of the neonates was not reasonable based on the results of the present study. In addition, the lack of a CT scan and PCR for all mothers or other family members was a limitation of this study.
3.1. Conclusions
COVID-19 is a new phenomenon in the medical world that involves various organs with different pathologies. Pulmonary hemorrhage, especially in neonates, is a dangerous but unknown manifestation of this disease. The clinical report showed that clinical signs, laboratory findings, and imaging were severe in neonates with COVID-19 who had pulmonary hemorrhage, which may also be related to surfactant damage and degradation.