1. Background
Q fever is a widespread zoonotic infection caused by C. burnetii, an obligate intracellular gram-negative organism (1). Domestic ruminants are considered the main source of human infections. C. burnetii does not usually cause clinical symptoms in animals, but can sometimes cause late stage abortions, death after birth and delivery of weak offspring. After animal infection, frequent shedding of highly resistant organisms occurs in birth products, vaginal discharges, feces and milk (2, 3). C. burnetii infections are not uncommon in humans, and outbreaks of Q fever that sometimes affect thousands of people are well-documented (4). Recently, Q fever proved to be a more common cause of severe febrile illness than malaria among hospitalized patients in northern Tanzania (5).
In Sudan, Q fever has been recognized since 1952 when C. burnetii was first isolated from ticks collected at the Cairo Municipal Abattoir on infested camels and bulls imported from Sudan (6). Taylor et al. (7) also indicated that 28 out of 401 (6.9%) human sera collected in different regions of Sudan were positive for C. burnetii antibodies.
2. Objectives
To generate updated and reliable data, it is important to allow proper risk assessment of C. burnetii infection. Owing to the meager and old data on Q fever disease available since 1988 in dairy cattle and camels in Sudan, this survey was conducted to determine the prevalence of anti- C. burnetii antibodies in cattle and camels in nine States in Sudan during May 2015 - March 2016.
3. Methods
3.1. Study Design
This cross-sectional survey included nine states of Sudan. Sample size estimation was calculated, using the formula n = 4PQ/L2, where n is the required number of animals to be examined; P is a known or estimated prevalence; and Q = (1 - P); L is the allowable error. The number of animals estimated, using this formula assuming 10% prevalence rate, was 144. Since location-to-location variation was expected, the sample size was increased and all collected sera (n = 244) were tested.
3.2. Sample Collection
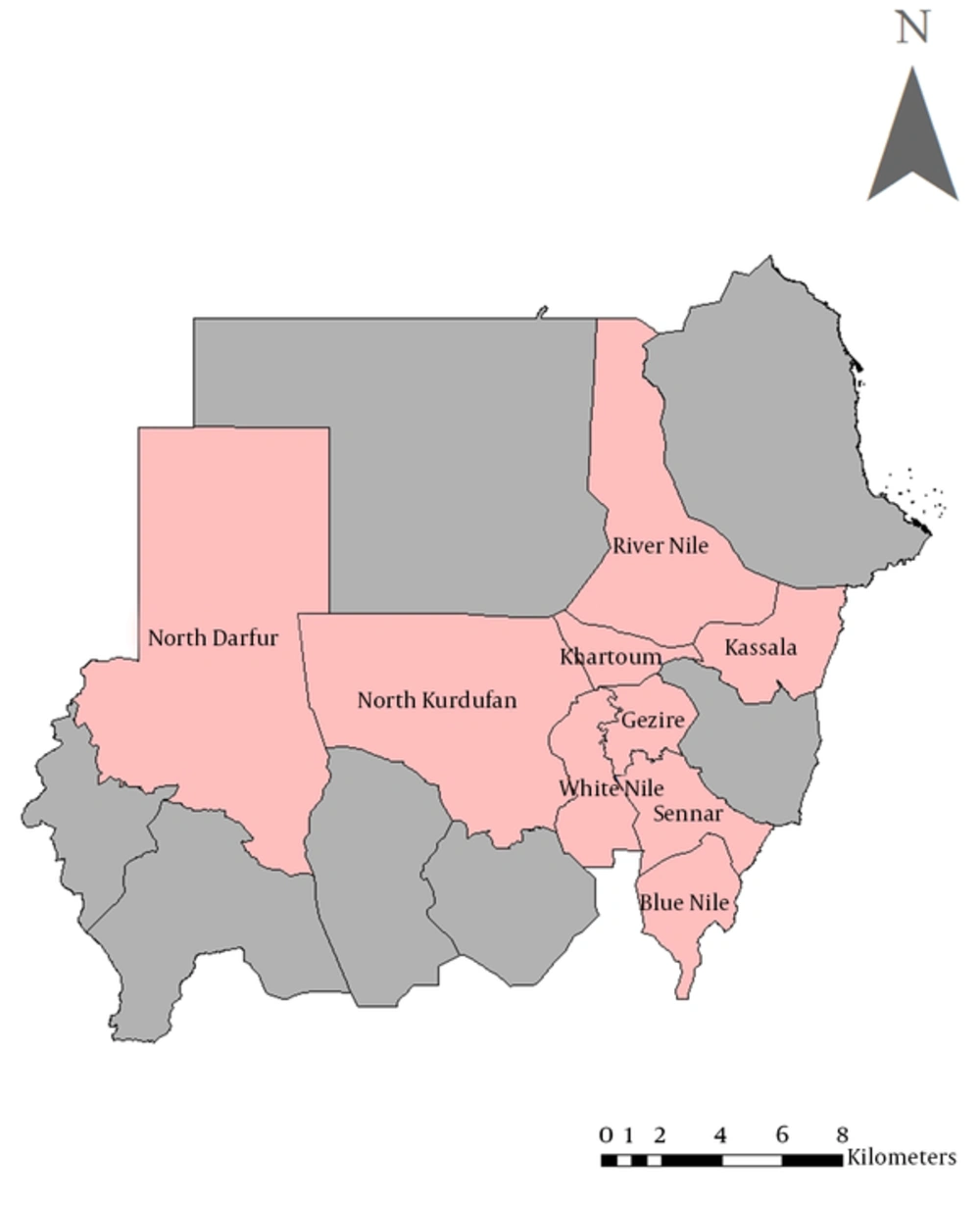
Collection of animal samples was reviewed and was in accordance with the animal welfare code of Sudan. Five mL of blood samples were collected from 244 adult, apparently healthy dairy cattle and from 76 healthy camels in nine States in Sudan (Blue Nile, El Gezira, Kassala, Khartoum, North Darfur, North Kordofan, River Nile, Sennar and White Nile States) during May 2015 - March 2016 (Figure 1). These locations were selected based on their importance for livestock raising. In each area, samples were collected from at least four groups of dairy cattle and camels that were kept apart. Selection of groups was made randomly and the formal mechanism used was lottery. Sera were obtained by centrifugation at 1500 rpm/min. for 10 minutes and kept at -20°C until tested.
3.3. Serological Assay
Commercial Q fever antibody indirect ELISA test kits (IDEXX Laboratories, USA) were used to detect anti- C. burnetii IgG antibodies based on the manufacturer’s instructions. The sample optical densities (OD) were measured by a microplate ELISA reader (Asys Expert Plus, Austria) at 450 nm. The sample to positive control ratio (S/P ratio) was then determined, using the following formula:

The cutoff value of antibody titer is ≥ 40%; i.e., all samples that have S/P ratio ≥ 40 are considered positive as indicated in the kit literature.
4. Results
C. burnetii antibodies were detected in dairy cattle and camels in all areas tested with varying prevalences. The seroprevalence rates in dairy cattle ranged from 3.3% in Nile River to 100% in White Nile State. The prevalence rates were highest in White Nile (100%) and Blue Nile (90.5%), moderate in El Gezira (53.3%) and North Kordofan (50%), and was lowest in Sennar (13.3%), Khartoum (9.4%), Kassala and North Darfur (6.7%) and River Nile (3.3%) States, with an overall prevalence of 29.92%.
The prevalence rates of antibodies in camels ranged from 20% in Kassala to 87.5% in North Kordofan State. The prevalence rates were highest in North Kordofan (87.5%) and River Nile (86.7%), moderate in El Gezira (40%) and lowest in Kassala (20%) States, with an overall prevalence of 64.5%.
5. Discussion
In this study, ELISA was used to detect antibodies to C. burnetii as the technique is very suitable for epidemiologic studies. Moreover, it is more sensitive, faster and convenient than both complement fixation test (CFT) and indirect immunofluorescent antibody (IFA) (8). Our results indicate that dairy cattle and camels are commonly exposed to C. burnetii in Sudan, with an overall seropositivity of 29.92% and 64.5% in cattle and camels, respectively.
Hamza (9) recorded a seroprevalence of 1.6% in Sudanese cattle, using capillary agglutination test (CAT). Harbi and Awad El Karim (10) reported that the prevalence rate of anti- C. burnetii antibodies in Sudanese camel’s sera was 11.9% and 12.2% in El Butana and Kassala regions, respectively, using capillary agglutination test. The difference in the prevalence between these studies and ours might be partially attributed to the different techniques used in determining these prevalences. Notwithstanding, there is more than four decades difference between timing of the works, and during this time C. burnetii infection might have intensively increased due to many factors such as an increase in animal population and intensification of animal breeding.
The differences in prevalence rates between the States herein reported may be attributed to local ecological factors, type of management and practices, flock size... etc. that might influence the transmission rates and infection with C. burnetii.
In this study, the overall seropositivity of Q fever detected in dairy cattle and camels (29.92% and 64.5%) was higher than that reported in goats (24.22%) in Sudan by Hussien et al. (11). This may, among other factors, be due to the fact that cattle and camels are more susceptible to tick infestation than goats. Ticks and aerosol infection are the main routes of C. burnetii transmission to domestic animals (12).
Q fever has been reported in many countries with different prevalence rates since the disease was described in 1935 (13). The seroprevalence of Q fever reported in this study in cattle (29.92%) was higher than that reported for cattle in Egypt (13%), Senegal (4%), Ghana (18%), Chad (7%) and South Africa (8%) (14-18), and it was lower than that reported in Nigeria (55%) and Cameroon (32%) (19-21). In this study, the prevalence of Q fever in camels (64.5%) was lower than that reported in Chad (80%) (22) and higher than that reported for camel in Saudi Arabia (15.9%) using PCR (23). These differences in seroprevalence rates among different areas may reflect the intensity of infections due to several reasons as mentioned earlier.
Transmission of C. burnetii through milk and semen is also possible (2, 24). All animal hosts for Q fever secrete C. burnetii in milk; thus, consumption of raw or unpasteurized milk or milk products could be a source of infection to humans (2). Consumption of raw camel milk is a widespread habit in the Sudanese society. However, generally, consumption of raw milk and milk products from all domestic species should be avoided to reduce the risk of infection with Q fever as well as with other milk and milk products borne pathogens.
Fever is one of the main symptoms of Q fever infections in humans. This can lead to incorrect diagnosis based on clinical symptoms alone since other febrile diseases, such as malaria, brucellosis, typhoid, visceral leishmaniasis, arboviral diseases, fevers of unknown origin (F.U.O) etc. are prevalent in Sudan. Hence, public health workers should consider Q fever diagnosis especially in those in close contact with animals.
In conclusion, Q fever is prevalent in dairy cattle and camels in Sudan. Therefore, more countrywide epidemiological studies on Q fever in both farm animals and humans should be undertaken.