1. Background
Human immunodeficiency virus (HIV) is a virus that in its progressive stage of infection causes acquired immunodeficiency syndrome (AIDS). At the first stage of the infection, a person may feel no symptoms or may suffer from a flu-like disease (1-3). As the infection progresses, the immune system becomes feeble and the risk of infections such as tuberculosis, hepatitis C, and other probable infections increases.
HIV can transmit in many ways e.g. unprotected sex, infected blood transfusions, and infected needles, from mother to baby in the period of pregnancy (vertical transmission), childbirth or lactation (4). The ways of transmission are different among countries. In 2017, most HIV cases in the United States occurred for homosexual men (66% of total lately diagnosed) (5). In some countries, HIV is more prevalent in cities because of the stress, urban lifestyle, and any other factors that provide opportunities for sexual activities (6).
The prevalence of AIDS has increased in the last decades. Approximately, 76.1 million people have suffered from HIV throughout the world and 35 million have lost their lives because of this virus (7). According to some reports, 36.9 million people have been living with HIV at the end of 2017 that included 35.1 million adults and 1.8 million children aged < 15 years (8). The prevalence of HIV is also increasing in Iran and the most common way of transmission is through the infected syringe among drug users (9).
Many factors such as age, gender, marital status, and other individuals’ characteristics may affect the progress of HIV and the death of HIV-infected persons. HIV attacks the immune system and destroys the CD4+ T cells; thus the number of CD4+ T cells in a sample of blood can be an important indicator of the strength of the immune system. The trends of CD4 changes are associated with the progress of HIV and the death of HIV-infected persons. Therefore, a decrease in the number of CD4+ T cells over time suggests the deterioration of the immune system and infection vulnerability (10, 11).
Usually, in studies where information is gathered on both time to record data and repeated measures of biomarkers (longitudinal data), a separate analysis is conducted on each recorded outcome; however, in many occasions, interest may also lie in studying their association structure. For instance, in this human immunodeficiency virus (HIV) research, the interest lies in the association between CD4+ T cell counts and the time of survival for HIV-infected persons. Therefore, the use of a separate model for each outcome may be inappropriate and lead to incorrect conclusions because of the relationship between the two data components (12). When the survival and longitudinal process are associated, using the joint analysis of survival and longitudinal data can account for the measurement error in longitudinal data and provide fewer estimate bias and more efficient conclusions.
Previous studies showed that description of HIV-positive population is important in HIV management and effective antiretroviral treatment is different between countries (13). Therefore, it is essential to study the factors affecting survival time in HIV-infected patients in each country separately.
In 2018, Akbari et al. (13) assessed survival and associated factors among patients living with HIV/AIDS in Iran by the Cox proportional hazards model and showed gender, age, CD4 count, and antiretroviral therapy as the significant mortality risk factors. Other researchers, Baghfalaki et al. (14) in 2013, developed and implemented a robust joint model in a simulation study on HIV-infected patients and concluded that observation time and the previous infection had significant effects on CD4+ T cell counts and HIV patients’ survival time.
2. Objectives
To our knowledge, there are only a few studies to identify the factors, influencing the survival time of HIV patients by using Bayesian joint models in Iran. The novelty of our study is the use of a more precise and powerful model to identify effective factors in the survival of HIV patients in Iran. As a result, this research aimed to use a Bayesian joint model to identify effective factors in the survival time of HIV-infected persons and determine the relationship between the trends of CD4+ T cell counts and survival time in HIV-infected persons.
3. Methods
In this population-based study, we used the HIV/AIDS surveillance data from Mashhad’s Counseling Center of Behavioral Diseases, Khorasan Razavi province, northeast of Iran during 1994 - 2014. Data were collected by referring to the patients’ files at the health center. The variables included in the analysis are marital status (single, divorced, married), gender, immunological classification (advanced HIV if CD4+ T cell counts at the beginning of the study was < 350 per mm3, not advanced HIV if CD4+ T cell counts at the beginning of the study was ≥ 350 per mm3), Antiretroviral treatment (yes, no) age, CD4+ T cell counts, survival time (from HIV diagnosis until death or censured) were considered. The study included 260 HIV-infected individuals. This research has been registered with the code of ethics, IR.MUMS.REC.1396.282, at the Ethics Committee of Mashhad University of Medical Sciences.
3.1. Statistical Analysis
Variables were summarized and demonstrated as frequency (%) for categorical variables or mean (standard deviation (SD)) for continuous variables. We used a Bayesian joint model to analyze the longitudinal and survival data simultaneously. The joint model was created from two sub-models; one sub-model relates to a longitudinal process and the other sub-model relates to the survival process. To fit the joint model, we used a mixed-effect model for the longitudinal sub-model and Cox regression model for the survival sub-model and linked them by using unobserved random effect through corresponding shared parameter. In fitting the joint model, the survival time was assumed as a dependent variable and marital status, gender, age, immunological classification, antiretroviral treatment as independent variables in survival sub-model and the CD4+ T cells was assumed as dependent variable, and time, marital status, gender, age, and antiretroviral treatment as independent variables in the longitudinal sub-model.
Because of the skewness in the CD4+ T cell counts variable, we first sought a proper transformation for this variable. The second root transformation seemed to appropriate because it showed to have a normal distribution. Parameters in the joint model were estimated under the Bayesian framework and implemented using Markov chain Monte Carlo (MCMC) methods. To compare many models with different random effect structures and different trajectory of time in the longitudinal sub-model, we considered the deviance information criterion (DIC) to choose the best model. According to the DIC criteria, the model with random intercept and quadratic time effect had the lowest DIC = 11417.66 and was considered to be the final model. All statistical analyses were performed using R software, version 3.4.1 with JM Bayes package at a significance level of 0.05.
4. Results
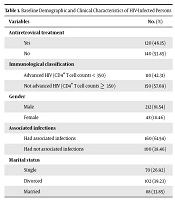
The study included 260 people, of whom 212 (81.54%) were male. The baseline characteristics of HIV-infected individuals are presented in Table 1. There were 68 cases (26%) of death events. At the beginning the study, 110 patients (42.3%) had advanced HIV (CD4+ T cells < 350), 70 (26.9%) were single, 102 (39.2%) were divorced and 88 (33.9%) were married. The mean age (SD) at the diagnosis was 40.3 (9.1) years and the mean (SD) for the number of CD4+ T cells of HIV-infected persons in the first measurement was 390.8 (410.8) per mm3. Of all cases, 60 (61.54%) individuals had other associated infections, including hepatitis C, hepatitis B, tuberculosis, and human T-lymphotropic virus.
| Variables | No. (%) |
|---|---|
| Antiretroviral treatment | |
| Yes | 120 (46.15) |
| No | 140 (53.85) |
| Immunological classification | |
| Advanced HIV (CD4+ T cell counts < 350) | 110 (42.31) |
| Not advanced HIV (CD4+ T cell counts ≥ 350) | 150 (57.69) |
| Gender | |
| Male | 212 (81.54) |
| Female | 48 (18.46) |
| Associated infections | |
| Had associated infections | 160 (61.54) |
| Had not associated infections | 100 (38.46) |
| Marital status | |
| Single | 70 (26.92) |
| Divorced | 102 (39.23) |
| Married | 88 (33.85) |
The results of the fitting Bayesian joint model are shown in Table 2. The survival sub-model parameters, including gender, antiretroviral treatment, and associated parameter were significant at 0.05 level. The risk of death for men was 5.1 times more than women, and among those who did not receive antiretroviral treatment was 3.5 times more than those who received treatment.
The longitudinal sub-model included intercept, linear and quadratic time, age and antiretroviral treatment. The subject who took the antiretroviral treatment had lower CD4+ T cells than those who did not take the antiretroviral treatment significantly. By increasing the age, the number of CD4+ T cells is decreased. By reducing the survival time, the number of CD4+ T cells is significantly reduced.
The estimated association parameter in Bayesian joint model, an indicator of the shape and relationship of the two survival and longitudinal sub-models, was -0.217 (95% CI: -0.323, -0.136), which was statistically significant (P < 0.001). According to the estimated hazard ratio for association parameter (0.805) (Table 1), we can say the increase in the number of CD4+ T cells reduces the risk of death.
| Variable | Estimate | 95% Credible Interval (CI) | P Value | Hazard Ratio (HR) |
|---|---|---|---|---|
| Survival Sub-Model | ||||
| Age, y | 0.015 | (-0.017, 0.046) | 0.330 | 1.015 |
| Antiretroviral treatment | ||||
| Yes | -1.246 | (-1.935, -0.641) | < 0.001a | 0.288 |
| No | 0 | - | - | 1 |
| Gender | ||||
| Male | 1.638 | (0.486, 3.197) | 0.006a | 5.145 |
| Female | 0 | - | - | 1 |
| Immunological classification | ||||
| Had advanced HIV (CD4+ T cell counts < 350) | -0.460 | (-1.158, 0.180) | 0.167 | 0.631 |
| Did not have advanced HIV ( CD4+ T cell counts ≥ 350) | 0 | - | - | 1 |
| Marital status | ||||
| Single | 0.551 | (-0.142, 1.265) | 0.119 | 1.735 |
| Divorced | 0.492 | (-0.154, 1.240) | 0.159 | 1.635 |
| Married | 0 | - | - | 1 |
| Association parameter | -0.217 | (-0.323, -0.136) | < 0.001a | 0.805 |
| Longitudinal Sub-Model | ||||
| Intercept | 27.384 | (24.022, 30.604) | < 0.001a | - |
| Age, y | -0.082 | (-0.152, -0.011) | 0.031a | - |
| Time, y | -0.741 | (-0.934, -0.554) | < 0.001a | - |
| Time2, y | 0.029 | (0.012, 0.045) | 0.001a | - |
| Antiretroviral treatment | ||||
| Yes | -4.827 | (-6.193, -3.505) | < 0.001a | - |
| No | 0 | - | - | - |
| Gender | ||||
| Male | -1.384 | (-3.039, 0.272) | 0.099 | - |
| Female | 0 | - | - | - |
| Marital status | ||||
| Single | -0.696 | (-2.270, 0.857) | 0.401 | - |
| Divorced | 0.021 | (-1.111, 1.094) | 0.952 | - |
| Married | 0 | - | - | - |
| σb0 | - | - | - | - |
aSignificant factors at the level of 0.05.
5. Discussion
Although there has been a great deal of progress in identifying pathogenesis and epidemiology of HIV, the number of HIV-infected people around the world are increasing substantially. In this study, we used the Bayesian joint model to investigate the association between the risk of death event and the change in CD4 biomarker that is repeatedly measured over time and to determine the factors associated with the survival of HIV-infected persons. Our results demonstrated that in the survival sub-model, gender and antiretroviral treatment and in the longitudinal sub-model, age, linear and quadratic time effect, and antiretroviral treatment were significant predictors.
According to the result of the joint model, the risk of death was higher in male than female inasmuch as HIV-infected males were 5.145 times at risk of death than HIV-infected females. Some studies reported that survival time for HIV-infected males is less than females (15, 16). There may be different reasons for this difference; for instance, females in earlier stages may be more aware of their infection and take the antiretroviral therapy (15, 16).
Our study demonstrated antiretroviral treatment was a significant factor in the remaining time to death of HIV-infected persons and those who did not receive antiretroviral treatment were at risk of 3.476 (1/0.288) times compared to those who received treatment. This result is in agreement with other studies’ results implemented in Iran. Akbari et al. (13), accessed the survival and associated factors among people living with HIV/AIDS and showed that gender, age, CD4 count, and antiretroviral therapy were the significant risk factors in HIV patients’ mortality.
In the longitudinal sub-model, the intercept for CD4+ T cell counts was significantly different in HIV-infected persons because the subjects had different CD4+ T cell counts at the beginning of the study. Also, our findings indicated that time had a negative effect on CD4+ T cell counts, so with the increase of time, the CD4+ T cell counts were decreased. This result is consistent with the results of a study conducted in 2017 in the Amhara region (17). Based on their retrospective study that was conducted to evaluate the effective factors on the number of CD4+ T cells, variables such as time, age, marital status, gender, and immunological classification were reported to be significant.
Seid et al. (18) compared separate and joint model on HIV data. Their results of the joint model showed variables of time and gender in the longitudinal sub-model and gender, age, clinical stage and functional status in survival sub-model, which are in agreement with some of our results.
The estimated association parameter (α) in the joint model is statistically significant (P < 0.05). This indicates that there is strong evidence of an association between the effects of the longitudinal outcome with the risk of an event, implying higher values of the CD4+ T cells associated with longer survival.
Many studies that support the joint modeling of the longitudinal data and survival time emphasize the significant correlation between the longitudinal trajectory of the CD4 and the survival time of HIV-infected persons (19, 20). According to a study carried out by Lim et al. (20) in 2013, it was revealed that death hazard depended on the longitudinal process and number of CD4+ T cells can affect the risk of mortality in HIV patients.
There are some limitations to this study; first, the use of data recorded by registration centers do not allow the accuracy of the data to be verified and may provide information bias (21). Second, in the present study, owing to the lack of availability of measurements for other markers, only the effect of a longitudinal marker has been investigated, but considering more markers such as CD8+ T cell counts or viral load could provide more useful and accurate results. The strengths of the current study are that we were able to identify a series of variables that affect the progression of HIV and the factors associated with the death of HIV-infected persons using a Bayesian joint model.
5.1. Conclusions
By using CD4+ T cell counts as a covariate in the Bayesian joint model, the survival time results for HIV-infected persons were estimated more precisely. It can be inferred that at the beginning of antiretroviral treatment, especially in men and controls, the CD4+ T cell counts can increase the survival time of HIV-infected persons.