1. Background
Assisted reproduction technology (ART) refers to all treatments or procedures encompassing the in vitro handling of both human oocytes and sperm or of embryos to establish pregnancy (1). From the birth of the first neonate conceived by ART in 1987, significant developments have been yielded in ART, and above four million children have been conceived by these techniques (2, 3).
Along with the development of ART, there are more concerns about the safety of these techniques and the prognosis of neonates conceived by ART than naturally conceived (NC) neonates (2). During ART, various drugs are used to stimulate ovulation and gametogenesis. Moreover, high-dose progesterone is used to support the luteal phase. All techniques can damage gametes or fetuses. Intracytoplasmic sperm injection (ICSI) is more aggressive than in vitro fertilization (IVF) because the sperm is directly injected into the oocyte in ICSI (4). Moreover, ICSI disables the natural selection of sperm by an oocyte resulting in the entering of genetically or morphologically abnormal sperm into the oocyte. Moreover, the transmission of multiple fetuses to the uterus increases the risk of multiple gestations, which is associated with low birth weight and other maternal or neonatal problems (5, 6).
Despite the recent advances in ART, it may be unsuccessful. Between 1980 and 1985, the rate of successful pregnancy by ART was 24% in women below 40 years and 14% in women above 40 years. Now, 22.4%, 23.3%, and 17.1% of IVF, ICSI, and the field effect transistor (FET) are successful in Iran, respectively (7). The success rate of ART is dependent on the patients’ age. This success rate is variable from 45% in patients below 35 years to 7% in patients above 42 years, which is due to the poor response of the ovary to stimulation or hyperstimulation syndrome (7).
Different studies have investigated the maternal or neonatal outcomes of ART and reported various problems, including multiple gestations, preterm labor, low birth weight, and intra-uterine growth retardation (IUGR), in neonates conceived by ART or their mothers (8-12). However, none of these studies have reported growth problems in neonates conceived by ART.
Serafin et al. reported that birth defects are not directly related to the use of ART (13). Cardiometabolic risk in children conceived using ART had no significant difference compared to those conceived without treatment (14). Kaye et al. concluded no concerning trends in adverse birth outcomes for singleton infants born ART (15).
2. Objectives
Although most neonates conceived by ART have optimal conditions after labor, investigating the risk factors of poor outcomes can help plan interventional protocols (16). Accordingly, the present study aimed to determine the one-year prognosis of neonates conceived by ART.
3. Methods
3.1. Subjects and Design
A prospective study was conducted on neonates conceived by ART from April 2020 to October 2021 at the Mahdieh Hospital affiliated with Shahid Beheshti University of Medical Sciences in Tehran, Iran. The Mahdieh Hospital is a referral and an educational, medical hospital with a level 3 neonatal intensive care unit (NICU) and 71 beds of NICU admission, which admits high-risk delivery for pregnant women. Moreover, there are facilities for assisting reproduction technologies in this hospital.
3.2. Data Collection
Data collection was performed by a trained research assistant using a pre-designed checklist from the maternal and neonatal medical records. The checklist included gestational age (GA) at delivery, complications during delivery, demographic characteristics of neonates, hospitalization at the ward or NICU, the first- and fifth-minute Apgar scores, preterm labor, IUGR, and the presence of any disease or anomaly in the neonates. A total of 165 neonates conceived by ART participated in this study. To compare the data of neonates conceived by ART with naturally conceived (NC) neonates, 165 NC neonates took part in the study. All neonates were followed up one year later to evaluate their weight, length of hospital stay, or mortality. GA ≤ 37 weeks was considered premature, and when compared to GA, birth weight < 10th or > 90th percentile was considered small gestational age (SGA) and large gestational age (LGA), respectively. Eventually, the obtained data from 330 neonates were imported into SPSS software.
3.3. Statistical Analysis
The statistical analysis was performed with IBM SPSS software version 25. We used descriptive and analytical-inferential statistics. To determine data distribution, One-Sample Kolmogorov-Smirnov Test was used. The χ2 test, Fisher’s exact test, t-test, Mann-Whitney test, and Pearson test were used to analyze the data.
Continuous variables are presented as mean ± standard deviation, and categorical parameters are expressed as No. (%) and compared using the chi-square test. All tests were 2-tailed, and the significance level was set at α = 0.05.
4. Results
IVF was performed in 70.3% of neonates conceived by ART, and in the remaining neonates, IUI was performed. The mean duration of infertility was 6.8 ± 4.2 years. Table 1 shows the general characteristics of the ART and NC groups. The mean age of the mothers in the ART and NC groups was not significantly different (31.8 ± 5.9 vs. 30.8 ± 5.5 years, respectively, P = 0.15). The mean gravidity was significantly different between the ART and NC groups (1.8 ± 1.2 vs. 2.3 ± 1.3, respectively, P < 0.001). The mean parity was significantly different between the two groups (0.4 ± 0.7 vs. 1.0 ± 0.9, respectively, P < 0.001). Mean GA was significantly lower in the ART group than in the NC group (34.8 ± 3.6 vs. 36.2 ± 3.0, respectively, P < 0.001). The mean birth weight was significantly lower in the ART group than in the NC group (2359 ± 782 vs. 2612 ± 673, repectively, P = 0.002). Moreover, the mean GA was lower, but multiple pregnancies was higher in the ART group than in the NC group (P < 0.05). Table 1 presents other maternal and neonatal characteristics.
| Characteristic of Neonates | ART Group (N = 165), No. (%) | NC Group (N = 165), No. (%) | P-Value | Odds Ratio (CI) |
|---|---|---|---|---|
| Mothers’ age, y | 31.8 ± 5.9 | 30.8 ± 5.5 | 0.15 | - |
| Mean gravidity | 0.4 ± 0.7 | 2.3 ± 1.3 | < 0.001 | - |
| Mean parity | 0.4 ± 0.7 | 1.0 ± 0.9 | < 0.001 | - |
| Mean gestational age, w | 34.8 ± 3.6 | 36.2 ± 3.0 | < 0.001 | - |
| Mean birth weight, g | 2359 ± 782 | 2612 ± 673 | 0.002 | - |
| Gender | 0.03 | 0.61 (0.39 - 0.94) | ||
| Male | 81 (49.4) | 101 (61.6) | ||
| Female | 83 (50.6) | 63 (38.4) | ||
| Previous history of abortion | 39 (23.6) | 29 (17.6) | 0.22 | 1.45 (0.85 - 2.48) |
| Nulliparity | 120 (72.2) | 64 (38.8) | < 0.001 | 4.21 (2.65 - 6.70) |
| Multiple pregnancies | 74 (44.8) | 16 (9.7) | < 0.001 | 0.33 (0.24 - 0.72) |
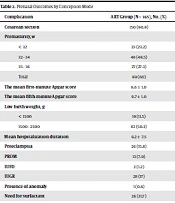
Table 2 shows perinatal complications by the conception mode. Compared to the NC group, the prevalence of cesarean delivery (C/S) delivery, preterm labor, deficient birth weight and low birth weight, maternal preeclampsia, need for surfactant, and need for mechanical ventilation were significantly higher in the ART group (P < 0.0.5). The mean first- and fifth-minute Apgar score was significantly higher in the ART group than in the NC group (P < 0.05). While the rate of neonatal hospitalization was similar in the two groups, the length of hospital stay was significantly higher in the ART group than the NC group (9.2 ± 7.5 vs. 6.2 ± 6.3 days, respectively, P < 0.001).
| Complication | ART Group (N = 165), No. (%) | NC Group (N = 165), No. (%) | P-Value | Odds Ratio (CI) |
|---|---|---|---|---|
| Cesarean section | 150 (90.9) | 111 (67.3) | < 0.001 | 0.21 (0.11 - 0.38) |
| Prematurity, w | < 0.05 | 0.43 (1.56 - 3.78) | ||
| < 32 | 23 (23.2) | 17 (27) | ||
| 32 - 34 | 49 (49.5) | 15 (23.8) | ||
| 35 - 36 | 27 (27.3) | 31 (49.2) | ||
| Total | 99 (60) | 63 (38.2) | ||
| The mean first-minute Apgar score | 8.6 ± 1.0 | 8.4 ± 1.1 | < 0.05 | - |
| The mean fifth-minute Apgar score | 9.7 ± 1.0 | 9.6 ± 0.8 | 0.01 | - |
| Low birth weight, g | < 0.001 | - | ||
| < 1500 | 19 (11.5) | 16 (9.1) | ||
| 1500 - 2500 | 83 (50.3) | 41 (24.8) | ||
| Mean hospitalization duration | 9.2 ± 7.5 | 6.2 ± 6.3 | < 0.001 | - |
| Preeclampsia | 26 (15.8) | 9 (10.6) | < 0.05 | 3.24 (1.47 - 7.16) |
| PROM | 13 (7.9) | 15 (9.1) | 0.84 | - |
| IUFD | 2 (1.2) | 0 (0) | - | - |
| IUGR | 28 (17) | 11 (6.7) | < 0.05 | 2.86 (1.37 - 5.96) |
| Presence of anomaly | 1 (0.6) | 0 (0) | - | - |
| Need for surfactant | 26 (31.7) | 16 (19.5) | 0.11 | 1.92 (0.94 - 3.92) |
| Need for mechanical ventilation | 41(50.0) | 34 (41.5) | 0.35 | 1.41 (0.76 - 2.62) |
| Prenatal diseases | < 0.001 | - | ||
| RDS | 69 (84.1) | 36 (43.9) | ||
| NEC | 2 (2.4) | 0 (0) | ||
| Icter | 8 (9.8) | 33 (40.2) | ||
| Others | 3 (3.7) | 13 (15.9) | ||
| Prenatal mortality | 9 (5.5) | 13(7.9) | 0.38 | - |
Abbreviations: PROM, premature rupture of membrane; IUFD, intrauterine fetal death; IUGR, intrauterine growth retardation; RDS, respiratory distress syndrome; NEC, necrotising enterocolitis.
The present results indicate that prematurity is more prevalent in the ART group, with a peak at GA between 32 and 34 weeks. While labor at GA < 32 weeks or 35 - 36 weeks is more common in the NC group, about one-third of the neonates in the ART group was born at GA 32 - 34 weeks (Table 2). Regarding the prenatal diseases resulting in neonatal hospitalization, respiratory distress syndrome (RDS) and necrotizing enterocolitis (NEC) were more prevalent in the ART group; in contrast, icter and other diseases were more prevalent in the NC group (P < 0.05). Although the prevalence of prenatal mortality was not different between the two groups (P = 0.38), IUFD and congenital anomaly were only observed in the ART group (n = 2 and n = 1, respectively).
Many complications of preterm birth are more common in the ART group than in the NC group. Accordingly, we assume that the complications are a direct reflection of prematurity and are not attributed to artificial conception. Then we analyzed the data once more. Table 3 shows statistically significant differences between the two pregnancy methods in many variables.
| Complications | Preterm (N = 164) | Term (N = 166) | ||||
|---|---|---|---|---|---|---|
| ART Group (N = 99) | NC Group (N = 65) | P-Value | ART Group (N = 66) | NC Group (N = 100) | P-Value | |
| Cesarean section | 90 (90.9) | 51 (78.5) | 0.025 | 60 (90.9) | 59 (59.0) | < 0.001 |
| The mean first-minute Apgar score | 8.2 ± 1.7 | 7.2 ± 1.7 | 0.001 | 9.0 ± 0.00 | 8.9 ± 0.5 | 0.041 |
| The mean fifth-minute Apgar score | 9.2 ± 1.8 | 8.6 ± 1.3 | 0.017 | 10.0 ± 0.00 | 9.9 ± 0.4 | 0.158 |
| Low birth weight (gr) | 0.017 | |||||
| < 1500 | 19 (19.2) | 16 (24.6) | - | - | - | |
| 1500 - 2500 | 71 (71.7) | 34 (52.3) | 12 (18.2) | 7 (7.0) | 0.027 | |
| > 2500 | 9 (9.1) | 15 (23.1) | 54 (81.8) | 93 (93.0) | ||
| Hospitalization | 8.5 ± 7.8 | 5.9 ± 5.3 | 0.026 | 3.0 ± 0.8 | 4.6 ± 3.5 | 0.392 |
| PROM | 6 (6.1) | 9 (13.8) | 0.091 | 7 (10.6) | 6 (6.0) | 0.280 |
| IUGR | 9 (9.1) | 0 (0) | 0.009 b | 4 (6.1) | 0 (0) | 0.024 b |
| RDS or NEC or Icter or others | 78 (84.1) | 65 (100) | < 0.001 | 4 (6.1) | 17 (17.0) | 0.038 |
| Prenatal mortality | 9 (9.1) | 12 (18.5) | 0.079 | 0 (5.5) | 1 (1.0) | 0.415 b |
a Values are expressed as No. (%).
b Fisher-exact test
In the ART group, the mothers used either IVF (n:116 and 70.30%) or IUI (n:49 and 29.70%) technique. There was no statistical difference among the means of hospital days (P = 0.38), preterm birth (P = 0.48), other complications (P = 0.52), and mortality (P = 0.46) in IUI and IVF.
All neonates were followed up one year later. Table 4 shows the outcomes of neonates during one-year follow-up. Compared to the NC group, the hospital stay rate and the prevalence of bodyweight < 5% were higher in the ART group during the follow-up (P < 0.05); however, the mortality rate was not different between the two groups (P = 0.37).
| Outcome | ART Group (N = 156), No. (%) | NC Group (N = 161), No. (%) | P-Value |
|---|---|---|---|
| Re-admission | 38 (24.4) | 22 (13.7) | 0.02 |
| Weight < 5% | 33 (21.2) | 18 (11.2) | 0.02 |
| Mortality during follow-up | 3 (1.9) | 1 (0.6) | 0.37 |
5. Discussion
Despite the development of ART techniques, the findings of previous studies on the obstetric, perinatal, and neonatal outcomes following ART are inconclusive, partly because of different study designs, populations, and countries. The present hospital-based cohort study on 330 subjects was carried out from April 2016 to October 2017 to investigate pregnancy complications and ART-related prenatal and neonatal outcomes. There was a 33-percent increase in the incidence of multiple gestations in the ART pregnancies compared with the NC group. Compared to the NC group, neonates in the ART group were more delivered by a C/S, were more premature with a peak at GA 32 - 34 weeks, had a higher risk of IUGR, had a lower birth weight, had a higher hospitalization duration, and had a higher risk of NEC and RDS. Besides higher prenatal complications, the maternal complications of pregnancy were higher in the ART group than in the NC group. A three-fold increase was found in the incidence of pre-eclampsia in ART pregnancies compared to NC pregnancies. Following up on the patients for one year showed that the ART group was more prone to need to admit to the ward and had a bodyweight < 5%, implying a retarded growth and higher vulnerability to the diseases than their NC counterparts.
Wu et al. reported that the risk of adverse obstetric outcomes and vascular complications was higher in pregnancies conceived by ART compared to natural conception (17). Previous studies have suggested an increased risk of preterm delivery and IUGR in children conceived by ART (18-21). A recent meta-analysis analyzed data from 27,819 IVF/ICSI pregnancies and found a higher risk of preterm delivery in IVF/ICSI-conceived children compared to NC children (21). Egan et al. mentioned that vulnerable child syndrome might more likely occur when mothers use ART (22). Esposito et al. and Zhang et al. reported that preterm birth was related to ART (23, 24). Also, Sunderam et al. reported that low birthweight in ART infants was 18.3% compared to all infants (8.3%) (25). A prospective cohort study found that the OR for preterm delivery in IVF was 2.19 (95% CI:1.59 - 3.02) (20). Similarly, the results of the present study showed a higher risk of preterm delivery, especially at GA 32 - 34 weeks and IUGR. However, some obstetrical or gynecological variables, such as multiple gestations, may confound the relationship between ART and preterm delivery and IUGR, suggesting the need for their adjustment in future studies (19).
Besides the preterm labor, the ART group was more prone to have a low birth weight (< 2500 gr) than the NC group in this study. These findings are consistent with previous studies suggesting an increased risk of low birth weight (LBW) among children conceived by ART compared to those conceived without medical assistance (21). The supraphysiological hormonal environment of the IVF cycle may be a significant cause of LBW in ART conception (19). However, a Dutch population-based study showed that the birth weight of siblings conceived with IVF was not significantly different from their NC-conceived siblings (26). This finding suggests the importance of consideration of maternal infertility as a factor that may contribute to the risk of LBW.
Consistent with our findings, previous studies have demonstrated that ART pregnancies are associated with a greater risk of cesarean sections (18, 27, 28). This is not due to the higher risk of multiple pregnancies in ART; however, ART pregnancies were associated with a greater risk of cesarean sections in singleton births (27). Moreover, elective and emergency cesarean sections are more common in ART pregnancies (27). However, a population-based Swedish study during a 25-year period showed a gradual decline in this increased risk of cesarean section rate (which nonetheless remains elevated compared to non-IVF pregnancies), implying that the development of the ART techniques has resulted in a lower risk of C/S (28).
AER is associated with known prematurity risks (9). Our findings showed that both RDS and NEC are more prevalent in ART neonates than in NC neonates. However, Turker et al. (9) reported that IVF was associated with RDS but not with NEC; similarly, Ahmad et al. suggested similar prematurity-related complications for IVF-conceived preterm infants compared to matched controls except for bronchopulmonary dysplasia and respiratory medication exposure (29). The discrepancy between our findings and those reported by Turker et al. and Ahmad et al. may be related to the inclusion of IVF, and intrauterine insemination (IUI) conceived neonates in our study, implying the need for further investigation of prematurity-related complications in IUI conceived neonates. Moreover, the ART and NC groups were not homogenous in terms of prematurity in this study.
Besides prenatal outcomes, ART has adverse obstetric outcomes. In the present study, a 3-fold increase in the incidence of preeclampsia was associated with pregnancies conceived by ART. Previous studies have reported a higher risk of preeclampsia in ART-conceived women (11). Preeclampsia is the leading cause of maternal and perinatal mortality and morbidity. The mechanisms by which ART leads to preeclampsia are not clear yet. Defective placental vascular remodeling is the suggested mechanism of preeclampsia (30); hence, further studies are needed to understand the underlying mechanisms to delineate placental development in ART births.
The main driver for adverse prenatal and obstetric outcomes in ART pregnancies is the higher risk of multiple gestations in ART. Moreover, singleton ART pregnancies still have a higher incidence of adverse outcomes than naturally conceived pregnancies (19). Infertility and epigenetic changes in genes involved in growth and development during hormonal stimulation and embryo culture may be independent risk factors (19). The present findings support previous reports on the relationship between increased obstetrical and perinatal morbidity with mortality and ART. Moreover, our findings showed that the infants in the ART group are more prone to need to admit to the ward and also have a bodyweight < 5%, implying a retarded growth and higher vulnerability to diseases during the one-year follow-up. It should be noted that based on the previous reports, twins or early preterm neonates conceived by ART compared to non-ART counterparts had similar neonatal outcomes (31, 32), and no additional management may be needed for them.
5.1. Conclusions
This report demonstrates that ART-conceived pregnancies may accompany several side effects. Accordingly, we recommend that mothers with ART-conceived pregnancies take benefit from more vigilant antenatal surveillance and delivery in advanced hospitals with tertiary-level neonatal intensive care centers.