1. Background
Gastroschisis is considered as a congenital anterior abdominal wall defect with the incidence of about 2% - 5% per 10000 live births (1). Prevalence of gastroschisis is rising may be due to increased premature live births and improvement of peri-partum care. Prenatal diagnosis of gastroschesis is possible with surveillance sonography during pregnancy or raised Alpha-fetoprotein (AFP) (2).
Although almost all cases have malrotation and sometimes intestinal atresia, other coexisting anomalies are not common in gastroschisis and overall survival rate is supposed to be over 90% (3).
The Principal of gastroschisis treatment is based on reduction of herniated viscera into the abdominal cavity and primary abdominal wall reconstruction (1). This procedure may not be applicable in special circumstances such as complicated cases (necrosis or perforation), severe edema that interferes with simple reduction and significant loss of abdominal domain (1). Bianchi and Dickson suggested bedside primary reduction with favorable outcome (4).
Rapid transfer from delivery unit to neonatal operating room and early surgical intervention is a major factor in successful primary reduction and abdominal wall closure while the main challenge in gastroschisis primary repair outcome is the balance of abdominal cavity development and visceral volume. While the visceral volume is larger than abdominal cavity, abdominal compartment syndrome may be anticipated.
2. Objectives
In this article we introduce a new method of visceral decompression that is described as total bowel washing (TBW) to improve intra and post-operative outcome of gastroschisis primary repair and reduction of silo placement or compartment syndrome in treatment of abdominal wall defects.
3. Methods
All neonates with gastroschisis in Pediatric Emergency Department of Dr. Sheikh and Akbar Children’s Hospital (Mashhad) and Taleghani Hospital (Gorgan) from 2006 - 2019 were enrolled in this study. Those cases with Apgar less than 8, birth weight less than 2000 g (VLBW), preterm labor (less than 34 weeks post gestational age), asphyxia, addicted or diabetic mothers and complicated gastroschisis (coexisting bowel atresia or necrosis or perforation) were excluded.
Patients were divided into two groups regarding the method of gastroschisis management. Neonates in the first group were managed by conventional method of gastroschisis management that started by opening and widening of abdominal wall defect, reduction of viscera into abdominal cavity, evaluation of abdominal pressure and abdominal wall repair or silo placement mostly with further staged repair of abdominal wall.
Among other group of cases (TBW), neonates where transferred to operation theater rapidly as soon as admitted to NICU. In operation room and after placement of NG tube general anesthesia was induced using modified rapid sequence induction technique with further oro-tracheal intubation and ventilation support. 12 French Nelaton was inserted into the stomach via the mouth and gastric contents were evacuated.
Procedure began with whole body prep and draping, protruded and matted bowels were gently washed and soaked in warm normal saline for some minutes. This maneuver allows a minimal enterolysis to gently detach mated bowel loops outside of the abdominal cavity. Then the rest of small bowel was pulled out from abdominal cavity meticulously trough the abdominal wall defect. 10 cc/kg warm saline was inserted to the stomach through the gastric tube and the surgeon guides the water to the proximal jejunum and follow it through the bowel loops by milking.
Pushing the water back and forth through the small bowel helps to liquefy the thick meconium all along the gastrointestinal tract. Diluted meconium is pushed back to the stomach to be evacuated via the gastric tube. This procedure repeats several times to wash all along the small bowel and finally and after extraction of meconium plugs, the water starts to come out of anus slightly.
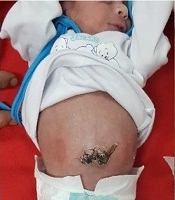
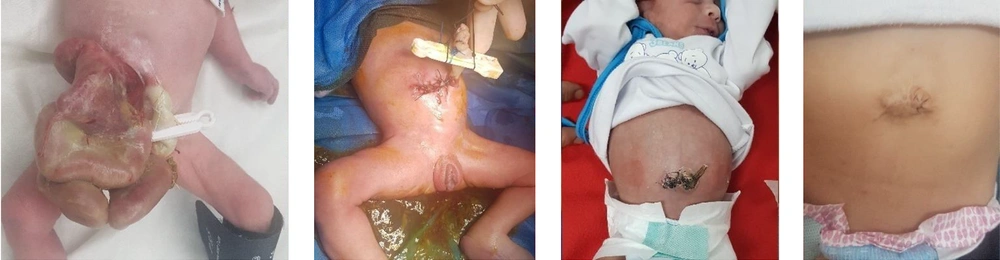
Passage of thin watery meconium through the anus by gentle milking is the key point to start the bowel reduction. This maneuver will also exclude probable bowel atresia that may coexist with gastroschisis. By the time of defecation through anus, the whole gastrointestinal tract is evacuated to reduce the volume of protruded viscera (Figure 1).
In the next step bowel reduction is accomplished without abdominal wall defect extension although abdominal wall stretching was performed just by finger traction and insertion of a wet gauze into the abdominal cavity to retain in place for a while.
Bowel loops reduction proceeds following wet gauze extraction while holding the abdominal wall up by the umbilical cord. Loop by loop bowel reduction proceeded and completed gently and abdominal wall closure was performed using full layer long absorbable stiches for fascia while skin was repaired by non-absorbable separated 3 - 0 nylon sutures. Abdominal cavity pressure was monitored intraoperatively by conventional methods such as intravenous line drip control and end inspiratory ventilator pressure monitoring. Those cases who showed elevated intra-abdominal cavity pressure over 20 cm H2O were reassessed again and while the high intra-abdominal pressure was confirmed the abdominal wall was reopened and total bowel washing by warm saline was repeated, the fascia kept open and skin closure was performed. Reassessment of intra-abdominal pressure was done at the end and in case of persistent high intra-abdominal pressure, skin stitches were removed and silo placement was tried. Patients were kept paralyzed sedated, intubated and transferred to NICU for close monitoring and ventilation support.
Intra-abdominal pressure rise over 20 cm H2O, anuria or limb mottling caused considering our criteria for reoperation with the same protocol which was mentioned in details before.
All neonates stayed under close and precise monitoring in NICU during post-operative days. Feeding started as soon as oro-gasteric tube drainage turned clear and non-bilious with the daily drained volume of less than 25 mL/kg (5). Parenteral nutrition was maintained during the waiting time for resuming bowel function.
Second group of patients were managed with conventional primary or staged abdominal wall closure using silo.
Some related variables such as type of delivery, gestational age, sex, maternal history and coexisting anomalies were recorded and intra and post-operative findings were also observed. Intra-abdominal pressure and need for ventilation support, time to start oral feeding and NICU stay and hospital admission time were also recorded and compared between the two groups.
4. Results
Fifteen neonates were allocated in each group. Patients’ demographic and anthropometric data are shown and compared between the two groups in Table 1.
| Demographic Variable | Conventional (N = 15) | TBW (N = 15) | P Value |
|---|---|---|---|
| Sex (male/female) | 9/6 | 10/5 | 0.342 |
| Gestational age (wk) | 37.4 ± 2.35 | 36.7 ± 3.12 | 0.271 |
| Type of delivery (NVD/CS) | 11/4 | 9/6 | 0.197 |
| Birth weight (gr) | 2616 ± 65 | 2365 ± 47 | 0.275 |
| Birth place (hospital/home) | 13/2 | 14/1 | 0.543 |
| Duration of surgery (h) | 36.7 ± 8.21 | 31.3 ± 7.19 | 0.094 |
All neonates were admitted to NICU after surgery. Intra-operative and post-operative findings are summarized in Table 2.
| Intra and Post-Operative Variable | Conventional (N = 15) | TBW (N = 15) | P Value |
|---|---|---|---|
| Operation duration (min) | 31.8 ± 7.34 | 38.3 ± 7.88 | 0.346 |
| Post-operative ventilation time (days) | 3.4 ± 1.28 | 2.7 ± 1.41 | 0.119 |
| Post-operative NGT time (days) | 4.7 ± 3.09 | 3.5 ± 2.08 | 0.213 |
| Time to oral feeding (days) | 8.4 ± 2.97 | 5.8 ± 1.56 | 0.007 |
| NICU care time (days) | 8.7 ± 3.11 | 6.1 ± 2.09 | 0.034 |
| Reoperation rate | 4 (26.7) | 2 (13.3) | 0.256 |
| Silo rate | 4 (26.7) | 1 (6.7) | 0.013 |
| Mortality rate | 5 (33.3) | 2 (13.3) | 0.195 |
aValues are expressed as mean ± SD or No. (%).
Primary signs of increased intra-abdominal pressure were detected in six neonates during post-operative period. As these cases were considered prone to abdominal compartment syndrome so they underwent reoperation (4 in conventional group and 2 in TBW). All reoperations in conventional approach consisted of silo placement and staged abdominal wall closure, while one of the two reoperations in TBW group was managed by facial opening, redoing bowel washing and skin closure.
In-hospital mortality rate was 33.3% in conventional approach compared to 13.3% in TBW group.
Long term fallow up of our cases also showed better cosmetic results in TBW group considering the length of scar formation and the shape of umbilicus.
5. Discussion
Bowel reduction into the abdominal cavity and abdominal wall repair is the main stay of gastroschisis management. The most challenging part of this procedure is the dilemma of loss of abdominal domain that leads whether to a successful abdominal closure or subsequent abdominal compartment syndrome that maybe life threatening. This serious fatal complication warrants staged repair and silo placement.
Although stage repair with silo maybe inevitable sometimes but it will be associated with increased rate of complications, infection and sepsis, prolonged ICU care and hospital stay and increased time to initiate enteral feeding (1).
Any maneuver that provides an extra space in abdominal cavity or safely reduces the volume of protruded viscera is considered as a valuable step toward primary gastroschisis repair.
In this light, NGT and folly insertion and gastric and bladder evacuation are included as principals of gastroschisis management.
Bianchi (1998) was the first one who proposed bedside bowel reduction and further primary abdominal closure without anesthesia with better outcome and fewer complications (4) but this procedure’s failure rate in management of Gastroschisis is reported as 20% - 50% in the literature (6).
Another concern about bedside Gastroschisis management is the significant stress response of neonate due to poor pain control and unstandardized suboptimal procedure environment (7, 8). Regarding these concerns, several articles proposed primary closure under analgesia or caudal anesthesia (6, 9).
In this study, we proposed modifications on gastroschisis primary closure supposed to increase the success rate of primary reduction.
Total bowel washing and intraluminal prep which is summarized as TBW method, will evacuate the whole intestine from retained thick meconium while warm saline will promote bowel circulation and a gentle entrolysis may subside bowel edema and subsequent easier and safer primary Gastroschisis repair. Benefits of bowel evacuation at the time of primary bowel reduction was also mentioned in an article by Rattan et al. as a good prognostic sign to preclude bowel atresia (1). We observed a significantly better outcome in terms of faster GI rehabilitation, less need to silo placement and shorter NICU and hospital stay in TBW method. Operation time was slightly longer in TBW group while the difference was not significant statistically. TBW improved bowel motility and function during post-operative period after gastroschisis repair and also helped to rule out any coexisting bowel atresia. Oral feeding intolerance is a common post-operative dilemma in gastroschisis management that may prolong NICU and hospital stay and increase TPN time and related complications (3). We observed beneficial effects of TBW in faster recovery of neonate with gastroschisis which may also decrease medication and hospitalization fees (6).
Mortality rate was also lower in TBW group although the difference was not significant statistically as other similar articles also indicated (10). Considering the clinical and preclinical finding among those patients who died during our follow up, main causes of mortality were sepsis and abdominal compartment syndrome. In this light, improving abdominal cavity decompression, decreasing NICU stay and faster bowel rehabilitation may justify lower mortality rate in TBW group.
Long term follow up of our cases also showed better cosmetic results in TBW group considering the length of scar formation and the shape of umbilicus which is also mentioned in other literatures (11).
5.1. Conclusions
Total bowel washing and complete evacuation of gastrointestinal tract from thick meconium will increase the success rate of primary repair and improve the outcome of gastroschisis management.