1. Background
Body dysmorphic disorder (BDD) and social appearance anxiety (SAA) are psychological disorders centered on dissatisfaction with the body. BDD is defined by the preoccupation with one or more minor appearance defects that are often accompanied by repetitive thoughts and behaviors (1, 2). SAA is one of the structures that has been introduced for this purpose and is a combination of features of BDD and SAA (3). Hart defines SAA as worry about others’ negative evaluations of body characteristics (3, 4). For this reason, these people are more likely to avoid situations where others are judging their bodies. In addition, SAA is associated with social anxiety, eating disorders, fear of negative evaluation, avoidance of social relationships, feelings of loneliness, and media addiction (due to fewer appearances) (3, 5-9).
In recent years, problems related to body dissatisfaction have increased in Asian countries, including Iran (10). The prevalence of BDD and its comorbidity with other psychological issues led researchers to better understand anxiety symptoms about the body in different forms and degrees and the factors affecting it. One of the factors discussed in recent years is the impact of social messages from social groups, especially the media. Research shows that constant exposure to ideal images from the media makes young people feel more pressured to evaluate their appearance (11, 12). Thompson has introduced a concept called sociocultural attitudes toward appearance (SATA) to examine the impact of social messages on body value from three sources: peers, parents, and the media. It is assumed that these three primary sources affect the body image through two mechanisms of comparison and internalization of ideal appearance (13).
Studies have shown that various factors affect people’s vulnerability to internalization, comparison, and body dissatisfaction. Parental care and insecure attachments are protective factors for the relationship between the internalization of ideal media images and body image (14). It can be argued that the relationship between receiving social messages and changes in body image is influential in a person’s psychological history, such as the degree of internalization and comparison. A lack of emotional care and support may be associated with deficits in the regulation of anxiety and self-doubt, leading to greater use of internalization and comparison. The sum of these can be predictors of more psychological disorders, such as BDD and SAA (15, 16).
Etiological studies suggest that the consequences of early and persistent exposure to childhood trauma are not limited to a post-traumatic stress disorder (PTSD) but can affect the psychological capacity of self-regulation, relationships with people, and one’s perception of oneself and others; they can also predict BDD (16). On the other hand, experiencing abuse or neglect means that children do not receive enough love, a sense of belonging, and support from their primary caregivers (17). In this situation, children are likely to internalize and attribute parental attitudes toward themselves (18).
Overall, a person’s initial experiences can influence the body image and related feelings, such as comparison and internalization of social messages. However, studies that have dealt with BDD predictors have seldom reflected a comprehensive view of pathology and society in parallel. In a previous study, attachment and parental care quality were mediators between media message internalization and physical dysmorphia (14). In addition, due to the high association of symptoms of BDD and SAA with psychiatric disorders, it is necessary to further assess the relationship between individuals and their bodies.
2. Objectives
There are few studies investigating the pathological path of the mediating role of SATA in the relationship between childhood trauma and SAA and the symptoms of BDD. Therefore, the present study aimed to investigate the relationship between childhood traumas with BDD symptoms and SAA with the mediating role of SATA.
3. Methods
This cross-sectional study was conducted on 415 students from five medical universities in Tehran, Iran using convenience sampling in 2019 - 2020. After checking the inclusion criteria, the research plan was first introduced to the study population, and upon their consent to participate in the study, they were provided with pre-prepared questionnaires. Participants filled out the anonymous questionnaires on the campus of their universities. A clinical psychologist distributed the questionnaires and collected the data. The researcher’s e-mail was also provided for contact if they had any questions or wanted to be informed of the results. The inclusion criteria were being a student at a medical university, willingness to participate in the study, and being in the age range of 18 - 35 years. Also, all incomplete questionnaires were excluded from the study. The ethical committee of Shahid Beheshti University of Medical Sciences approved this study (code: IR.SBMU.MSP.REC.1398.760).
The Child Trauma Questionnaire (CTQ) has 28 items that measure five areas of traumatic experiences: emotional abuse, physical abuse, sexual abuse, emotional neglect, and physical neglect. It is scored on a 5-point Likert scale. The reliability of the test with the test-retest method is in the range of 0.79 to 0.94, and the concurrent validity of childhood trauma has been reported in the range of 0.59 to 0.78. In the original subscales, Cronbach’s alpha for physical neglect, emotional neglect, physical abuse, emotional abuse, and sexual abuse is 0.60, 0.91, 0.88, 0.87, and 0.94, respectively (17). In Iran, the reliability was between 0.94 and 0.79 (19).
Yale-Brown obsessive-compulsive scale body dysmorphic disorder (BDD-YBOCS) is a 12-item self-report tool on a 5-point Likert scale that measures the severity of BDD symptoms (16) and includes two factors of obsession and compulsion. The questionnaire’s correlation with similar questionnaires ranges between 0.25 and 0.58. Cronbach’s alpha coefficient was 0.93 (13). Veisy et al. confirmed the validity and reliability of the questionnaire in Iran (19). The results showed that the questionnaire has a medium correlation (0.25 to 0.58) with similar questionnaires. Cronbach’s alpha coefficient was 0.93 for the total scale.
Sociocultural Attitudes Towards Appearance Questionnaire (SATAQ) includes 22 questions on a 5-point Likert scale, consisting of two subscales of internalization and three subscales related to social pressures (20). Cronbach’s alpha was between 0.79 and 0.93. Confirmatory factor analysis (CFA) showed that this 2-factor model had a good fitness (20). In Iran, the reliability was between 0.63 and 0.64 (21). This questionnaire was translated into Persian by Sadeghi et al. Its internal validity was 0.77, which shows an acceptable internal consistency. Also, in calculating the reliability using the split-half method, Cronbach’s alpha for the first half was 0.63 and for the second half was 0.64 (21).
Social Appearance Anxiety Scale (SAAS) consists of 16 items designed by Hart (3). The participants can rate their answers on a 5-point Likert scale. Internal consistency was 0.94 (3). CFA showed that SAAS is a one-factor questionnaire. The internal consistency of the present study was calculated (Cronbach’s alpha = 0.94). Cronbach’s alpha for the total score was α = 0.95. Also, the relationship between SAAS and BDD (r = 0.73; P < 0.01), body shape (r = 0.46; P < 0.01), and social physique anxiety (r = 0.79; P < 0.01) showed a good convergent validity.
3.1. Data Analysis
In the descriptive section, statistical indexes, tables, and graphs were used to describe the research variables. In the inferential section after the test, presuppositions such as the multilinearity of the predictive variables were considered. All statistical analyses (descriptive statistics, Pearson’s correlation coefficient, and structural equation modeling [SEM]) were performed using SPSS version 24 and AMOS version 21 software.
4. Results
The age range of participants was 21 - 28 years (mean = 24.5, SD = 5.49). Also, 287 (69.2%) subjects were female, and 126 (30.8%) were male. Regarding marital status, 69 (16.6%) participants were married, and 346 (83.4%) were single. In terms of educational level, 219 (52.8%) students had a bachelor’s degree, 132 (31.8%) had a master’s degree, and 64 (15.4%) had a doctoral degree.
Table 1 presents the central (mean) and dispersion (standard deviation) indicators of research variables, including BDD, SAA, childhood traumas, SATA, and the subscales.
| Variables | Mean ± SD |
|---|---|
| Body dysmorphic | 26.73 ± 7.59 |
| Obsession | 12.05± 3.69 |
| Compulsion | 10.66 ± 3.41 |
| Avoidance | 1.90 ± 1.15 |
| Insight | 2.18 ± 1.18 |
| Social appearance anxiety | 33.85 ± 13.43 |
| SATA | 54.82 ±15.49 |
| Internalization | 16.01 ± 4.13 |
| Comparison | 12.89 ± 4.55 |
| Family | 8.71 ± 4.01 |
| Peers | 7.91 ± 3.47 |
| Media | 9.30 ± 5.17 |
| Childhood traumas | 48.75 ± 12.34 |
| Emotional negligence | 6.26 ± 2.40 |
| Physical negligence | 8.67 ± 3.90 |
| Sexual abuse | 6.26 ± 2.45 |
| Emotional abuse | 8.83 ± 1.53 |
| Physical abuse | 10.98 ± 4.14 |
The normality and multicollinearity assumptions were examined. The variance inflation factor (VIF) and statistical tolerance indexes were used to test the non-multicollinearity hypothesis, considering that none of the values related to the tolerance index was less than 0.01. None of the values related to the VIF was more than 10. Accordingly, non-multicollinearity assumption could also be confirmed.
The correlation between different variables of the study is shown in Table 2.
| Variables | 1 | 2 | 3 | 4 |
|---|---|---|---|---|
| Body dysmorphic | 1 | |||
| Social appearance anxiety | 0.773 ** | 1 | ||
| SATA | 0.497 ** | 0.435 ** | 1 | |
| Childhood traumas | 0.276 ** | 0.293 ** | 0.105 * | 1 |
a * P < 0.01; ** P < 0.05
According to Table 3, all fit indices indicate the suitable fitness of the model.
| Chi-Square | Chi-Square/df | RMSEA | SRMR | CFI | IFI | TLI | |
|---|---|---|---|---|---|---|---|
| Statistics | 151.168 | 1.844 | 0.045 | 0.045 | 0.973 | 0.973 | 0.965 |
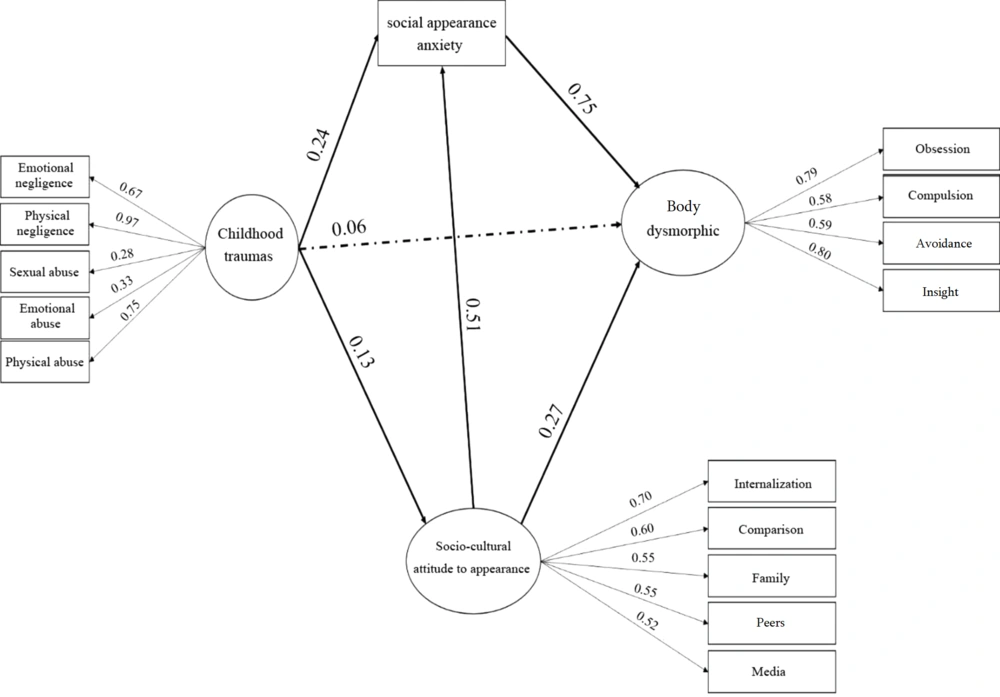
Figure 1 shows the significant paths as continuous and the non-meaningful paths as discontinuous lines. According to the results presented in Figure 1, all routes are significant.
The bootstrap method used a 2000 sampling process with a 95% confidence interval to determine the indirect effect. According to Table 4, the indirect effect of childhood trauma on the BDD variable through the mediating role of SAA was significant (P < 0.05, b = 0.171). According to Table 4, the indirect effect of SATA on the BDD variable through the mediating role of SAA was significant (P < 0.05, b = 0.308).
| Independent Variables | Mediator Variables | Dependent Variables | b | P |
|---|---|---|---|---|
| Childhood traumas | SATA | body dysmorphic | 0.034 | 074/0 |
| Childhood traumas | SAA | body dysmorphic | 0.171 | 0.005 |
| SATA | SAA | body dysmorphic | 0.308 | 0.003 |
5. Discussion
The present study investigated the relationship between childhood traumas with BDD and SAA through the mediating role of SATA. The goal was to develop and consolidate separate studies that suggested childhood trauma could be associated with physical BDD problems in adulthood (13); however, they paid less attention to the pathological trauma path and the assessment of the trauma effect and social attitudes.
Therefore, this study shows that a person who has experienced childhood abuse and neglect, when placed in a social environment (family, peers, media) in which appearances are essential for acceptance and rejection, internalize this attitude and further compare themselves with ideal patterns, thus, experiencing BDD and SAA symptoms
This hypothesis shows that childhood traumas through the mediating role of sociocultural attitude toward appearance not directly. It can be concluded that traumatic experience cannot directly lead to BDD and pursue the path of the pathology of other disorders unless the person realizes the importance of appearance in relation to others, in which case individuals tend to internalize and compare more, leading to BDD. Boohar’s study showed that BDD is associated with parental attitudes and messages that involves confirmation or scorn directly related to the body (18).
On the other hand, childhood traumas predict SAA both directly and through SATA. Schaefer’s study found that women who experienced childhood trauma reported more negative body satisfaction than those who did not experience trauma (13). This result is consistent with studies showing that internalizing the ideal appearance and perceived rejection can predict SAA. The trauma that a person experiences during childhood is focused not only on the symptoms after the pathology but also on the person’s perception of themselves and others. When a child is abused or neglected at an age when they create images and patterns of themselves, others, and the world, they generalize such events to themselves, others, and the world (16).
The findings showed that physical abuse and emotional neglect were the best predictors among the trauma subscales. Physical abuse is a trauma related to the body that experiences punishment, ridicule, criticism, and emotional harassment through the body. These feelings may be related to the body. Moreover, in these circumstances, the abuser has become the owner of the child’s body, as if the body does not belong to the person and there is someone else who decides about it (21). This is where another’s control over one’s body becomes internalized. We can conclude that a person who feels tormented by their body in the presence of others or feels pressured to lose weight and transform their body is concerned about another person’s opinion and decision about their body. In that case, their body may again become the subject of punishment and rejection. In addition, emotional neglect, which is somehow associated with not receiving love and attention (people may internalize such an experience and attribute it to their self-value), is accompanied by feelings of worthlessness, seeking approval, and fear of rejection in adulthood (21-24). However, in this situation, how these pathologies manifest themselves through BDD and SAA emphasizes the mediating role of SATA. If an individual receives attitudes and reactions from the family, peers, and the media, such as admiration or ridicule, about the appearance of individuals or themselves, they are likely to form the belief that appearance determines value, approval, and acceptance (11-13, 21). In this atmosphere, the media may convey the implicit message that appearances should be perfect by displaying ideal, flawless images and advertising for bodily changes, and the defect may cause differences or rejection. Therefore, those who already have concerns about imperfection when exposed to this view of appearance are more likely to have concerns leading to appearance. So, the social pressure received from the media forcing them to change themselves is intensified, leading to concern about their desirability. Comparison and internalization may be a way of having an explicit criterion for their desirability in the eyes of others. Previous experiences in earlier communications have shown that they are judged, rejected, or humiliated when caregivers do not approve of them.
For this reason, SAA, which focuses more on the anxiety and doubts of the individual over appearance in social communication, was directly and indirectly predicted through trauma and SATA. Therefore, a person who has experienced trauma does not seem to own their body. In this case, the body belongs to another person who must approve and accept it; otherwise, it may be the source of punishment and rejection, similar to physical abuse.
5.1. Conclusions
Recognizing the variables affecting BDD plays an essential role in prevention, education, and treatment. Studies showed that various factors influence the pathways leading to anxiety about the body. They are gradually formed from childhood experiences and are reinforced by internalized social messages from the family, peers, and media. It is important to know its formation pathways and influential factors for assessment, education, and treatment, even from an early age.
Contrary to previous studies, the mediating role of SATA in the present study emphasized its importance concerning childhood trauma and BDD and SAA. This finding is in line with some previous studies, but somehow emphasizes the relationship between trauma, psychological trauma, personality traits, and BDD. It is important to pay to the role of social internalization, the effects of culture, and society on symptoms and problems. Thus, in training, evaluating, and treating body dysmorphic problems, we can also look at influential factors, such as changes in the media and advertising and values and culture, in addition to retrospective and psychological perspectives, such as early traumatic experiences.
This study had some limitations. The samples consisted of students from Tehran universities who have different personalities and cultural characteristics. For example, they are more perfectionists and probably use more media. These features may have influenced the answers to the questions. Therefore, it is suggested that these variables be measured in groups with other characteristics. Another limitation is the retrospective nature of the study, which may lead to possible bias.