1. Background
Negative early relationships with parents and their impact on the development of psychopathology have been of interest to various theoretical approaches. Early life experiences have an extensive long-term effect on children’s behavioral and psychological development (1). Pervasive life experiences during growth may be associated with significant biological changes and alterations in the response of the allosteric system, thus exerting long-term effects on the endocrine, nervous, and immune systems (2).
Although the causes of mental health problems are multifactorial, negative early life experiences are one of the risk factors that have been empirically studied in recent years. It is estimated that the onset of more than one-third of all mental disorders can be referred to as exposure to childhood trauma (3). In fact, negative early life experiences contribute to the development of psychiatric pathology of several disorders in early adulthood, including mood disorders (4), anxiety disorders (5), destructive behaviors (6), antisocial behaviors (7), substance abuse (8, 9), psychosis (10, 11), and suicidal behaviors (12). The literature shows a positive relationship between negative early life stress and the development of borderline personality disorder and symptoms (13, 14).
There are several scales to measure early life experiences, such as The Inventory of Stressful Events in Childhood and Adolescence (15), The Adverse Childhood Experience Questionnaire (ACE) (1), The Early Trauma (16), and The Child Abuse and Trauma Scale (CATS) (17). These scales mainly focus on parental behavioral recall. In addition, they do not examine subtler forms of trauma, such as submissive behaviors, threats, or lack of love, which can significantly impact the formation of psychological problems.
According to social ranking theory, parent-child interactions can be conceptualized as hierarchical relationships within an attachment context. This theory emphasizes down-rank threats and submissive behavior (18, 19). Based on this theory, when children are raised in an environment where their abilities are ignored, their emotions are not validated, rejected, or rejected by parents., they may experience feelings of unlovely and fear of parents, they may have to adopt unwanted or involuntary submissive and defensive behaviors to deal with this potentially traumatic environment. These submissive defense strategies aim to reduce or disable criticism and aggression of the dominant other or its hostile intention (19, 20).
As a result, the Early Life Experiences Scale (ELES) was developed by Gilbert et al. (19). This scale examines the importance and value of evaluating the recall of personal behaviors and personal emotional experiences from childhood (19). This scale has three separate subscales: Feeling threatened (I tried to stay away from my parents to avoid harm), submissiveness (I felt rejected if I did not do what others wanted me to do), and feeling valued/unvalued (I felt comfortable with my parents) (21). Many tools designed to improve parenting have focused on recalling parenting behaviors, but the early life experience scale focuses on personal behaviors and feelings. Psychometric properties of this scale have been investigated in different countries and have shown appropriate validity and reliability (22, 23).
This scale is important to measure adults’ recollections of the levels of fear, panic, or threat they felt as children rather than focusing on parental behaviors, which can be accompanied by a reduction in defense strategies in measuring early life events. However, the self-report scale is not found to measure reminders of submissiveness, feeling valued/unvalued, or feeling threatened by parents. It is vital to have reliable tools for measuring them to expand research and evaluate early life experiences. Due to the need to study the psychometric characteristics in different cultures (24), this research can help increase knowledge about cultural influences on this structure. Therefore, Iranian clinicians will have a valuable screening tool to learn about early life experiences.
2. Objectives
Due to the psychological consequences of early life experiences and the lack of a reliable and valid scale in Persian, the present study was conducted to investigate the validity and reliability of the Persian version of the ELES.
3. Methods
3.1. Participants and Sampling
This is a cross-sectional descriptive factor analysis study. The study population consisted of all Iran University of Medical Sciences students in the academic year 2019 - 2020. The minimum sample size for Confirmatory Factor Analysis (CFA) is 200 people (25). Accordingly, the study sample consisted of 231 (109 males and 122 females) students of the Iran University of Medical Sciences selected by convenience sampling. Inclusion criteria were being a student at the Iran University of Medical Sciences, awareness of research objectives, and informed consent to participate in research. Exclusion criteria were leaving more than 30% of questions unanswered and specific response patterns, such as answering different questions with the same answers or marking a single option in consecutive questions.
The ELES was prepared based on cross-cultural adaptation guides. First, three Ph.D. candidates in clinical psychology translated the original version of the ELES from English into Persian, and any translation differences were settled by discussion. Second, two fluent mental health specialists in both Persian and English translated the prepared Persian version into English. Third, the authors reviewed the Persian translation.
In the next stage, the scale was implemented in a pilot study on a sample of 25 students of Iran University of Medical Sciences, and the existing problems were corrected. To evaluate the reliability of the retest, 36 students in the study re-completed the ELES two weeks later. In this study, all students had complete freedom to participate in the research, and before completing the questionnaire to observe ethical considerations, a brief explanation about the study’s objectives was given to them. They were assured that the collected data would be considered in groups.
3.2. Measures
3.2.1. Early Life Experiences Scale
It was developed in 2003 by Gilbert et al. (19). This scale includes 15 items and three subscales (threat, submissiveness, and unvalued). Each item of the scale is rated on a five-point Likert scale ranging from 1 = completely untrue to 5 = very true to evaluate how much each statement was true for the participant. The authors found good reliability with Cronbach’s alphas of 0.89 for threat, 0.85 for submissiveness, 0.71 for (un)valued, and 0.92 for the total scale (19).
3.2.2. Schizotypal Trait Questionnaire-B Form
This questionnaire was developed by Claridge and Broks (26) and revised by Rawlings et al. (27). It has two scales: Scale A: Schizotypal personality (STA) and scale B: Borderline personality (STB). The Schizotypal Trait Questionnaire-B (STB) was used in this study to evaluate borderline personality patterns. It consists of 24 items and three subscales (hopelessness, impulsivity, and stress-related paranoid/dissociative symptoms) that are answered as yes/no. Rawlings et al. reported a retest validity of 0.80 (27). In Iran, Mohammadzadeh et al. reported the reliability coefficient of retest during four weeks as 0.84 for the total scale, while those of hopelessness, impulsivity, and stress-related paranoid/dissociative symptoms were 0.53, 0.72, and 0.50, respectively (28). The alpha coefficient was 0.77 for the total scale and 0.64, 0.58, and 0.57 for the hopelessness, impulsivity, and stress-related paranoid/dissociative symptoms, respectively (28). In this research, Cronbach’s alpha was 0.77.
3.2.3. Self-compassion Scale-Short Form
It was developed in 2011 by Raes et al. (29). It contains 12 items and six subscales (self-kindness, self-judgment, common humanity, mindfulness, and over-identification). Each item is rated on a 5-point Likert scale ranging from 1 (almost never) to 5 (almost always). Total Self-compassion Scale-Short Form (SCS-SF) scores have demonstrated high correlations with long-form SCS total scores. Moreover, each subscale correlates significantly with the equivalent long-form scale (r = 0.89 to r = 0.91) (29). The SCS-SF total score shows good internal consistency. However, subscales demonstrate varying internal consistencies (30). In Iran, research results supported the three-factor structure of self-compassion in a national sample (root mean square error of approximation (RMSEA) = 0.08, normed fit index (NFI) = 0.94, and comparative fit index (CFI) = 0.97), with Cronbach’s alpha of 0.78 (30). In this research, Cronbach’s alpha was 0.76.
3.2.4. Difficulties in Emotion Regulation Scale
It is a self-report scale for evaluating emotion regulation difficulties by Gratz and Roemer in 2004 (31). This scale includes 36 items and six subscales (no acceptance of negative emotions, difficulties engaging in goal-directed behaviors, difficulties controlling impulsive behaviors, limited access to effective emotion regulation strategies, lack of emotional awareness, and lack of emotional clarity). Each item is rated on a scale from 1 (almost never) to 5 (almost always). Earlier research has shown good internal consistencies (> 0.80) and stabilities (> 0.69) within both clinical and nonclinical populations and significant correlations with other emotion regulation measures. The construct and predictive validity of the scale scores within both clinical and nonclinical populations have also been supported (31). Psychometric properties of the Persian version of this scale have been investigated and confirmed in clinical and nonclinical samples. In these surveys, Cronbach’s alpha coefficients for questions of no acceptance of negative emotions from 0.73 to 0.88, for difficulties engaging in goal-directed behaviors from 0.72 to 0.89, for difficulties controlling impulsive behaviors from 0.75 to 0.90, for limited access to effective emotion regulation strategies from 0.76 to 0.85, for lack of emotional awareness from 0.72 to 0.86, for lack of emotional clarity from 0.77 to 0.90, and for the total score of the scale from 0.79 to 0.92 were obtained (32). In this research, Cronbach’s alpha was 0.83.
3.3. Data Analysis
We cleaned and screened the data. Below 5% of the data in the dataset were missing. Confirmatory factor analysis was used to assess the structural validity of the scale and Cronbach’s alpha to determine its internal consistency. Intraclass correlations coefficient (ICC) was employed to evaluate the test-retest reliability. The Pearson correlations between the ELES scores and STB, SCS-SF, and Difficulties in Emotion Regulation Scale (DERS) scores were investigated for divergent and convergent validity. Data analysis was done using SPSS-20 and LISREL version 8.80.
4. Results
4.1. Description of the Sample
The participants’ age ranged from 19 - 52 years, with a mean of 26.62 and a standard deviation of 6.02. There were 157 (68%) single and 74 (32%) married people. Five (2.2%) had Associate’s degrees, 111 (48.1%) had Bachelor’s degrees, 104 (45%) had Master of Science degrees, and 11 (4.8%) were Ph.D. students.
Table 1 presents the mean and standard deviation of the ELES, its three subscales, and their correlations. As can be seen, there was a significant correlation between the total score of the scale and its three subscales in the range of 0.36 to 0.90.
Abbreviation: ELES, Early Life Experiences Scale.
a P < 0.01
4.2. Reliability
Cronbach’s alphas were determined with the total sample (n = 231). Cornbrash’s alpha coefficients for the total scale, submissiveness, feeling valued/unvalued, and feeling threatened were gained as 0.74, 0.85, 0.66, and 0.80, respectively. Test-retest reliability was determined for the ELES total scale and three subscales with a sample of 36 students who answered the ELES twice at a two-week interval. Intraclass correlations coefficients for the total scale, submissiveness, feeling valued/unvalued, and feeling threatened were gained as 0.88, 0.95, 0.90, and 0.85, respectively.
4.2.1. Confirmatory Factor Analysis
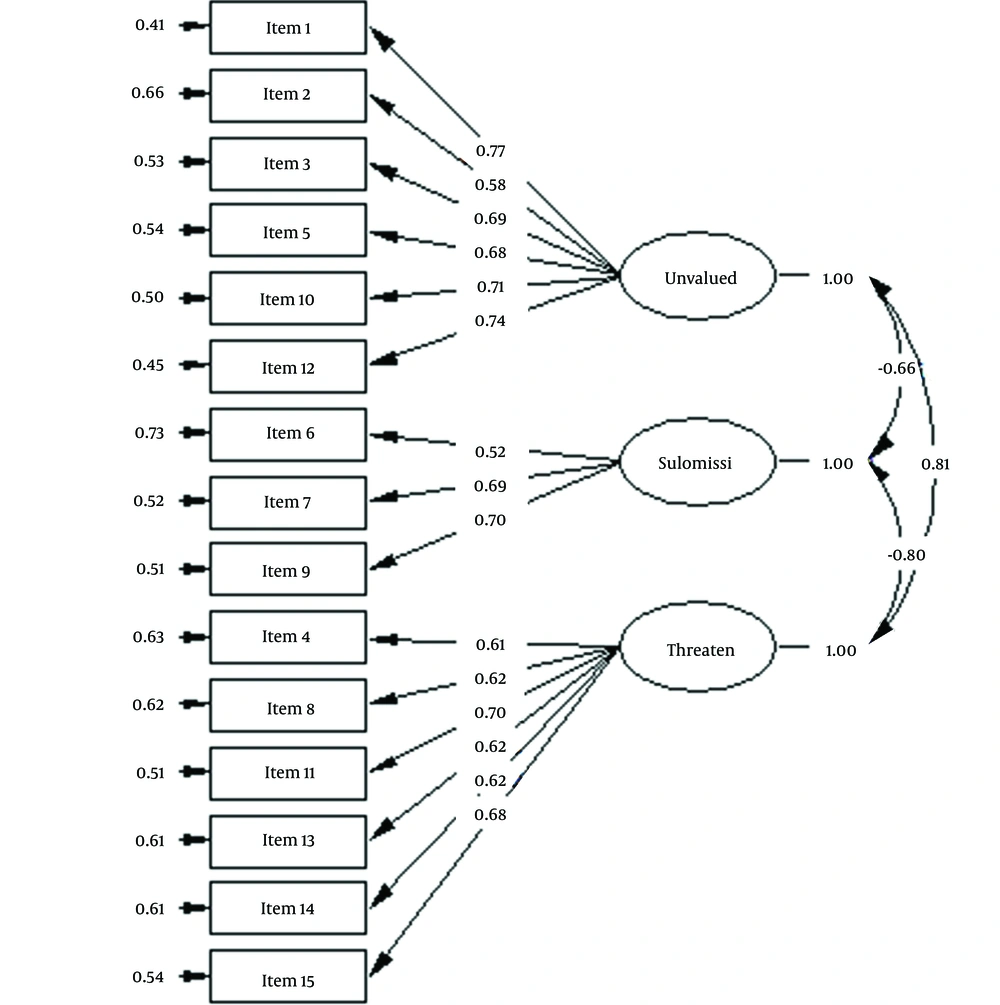
The validity of the ELES was assessed through two methods: CFA and divergent and convergent validity. LISREL software was used for performing CFA to examine the three-factor structure of the ELES. We used the fitting indices of chi-square (χ2), CFI, the incremental fit index (IFI), RMSEA, and NFI to fit the three-factor structure of this scale. For NFI, CFI, RFI, and IFI fit indices, a value above 0.90 indicated the acceptable fit of the model. SRMR ≤ 0.10 and RMSEA ≤ 0.08 indicated the acceptable fit of the model. The results of the fit indices are given in Table 2. Based on the results, the three-factor model of the ELES had a good fit (Figure 1).
| Fit Indices | χ2 | χ2/df | RMSEA | IFI | CFI | SRMR | NNFI | NFI | GfI | RFI | AGFI |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Quantity | 229.49 | 2.64 | 0.08 | 0.96 | 0.96 | 0.07 | 0.95 | 0.95 | 0.88 | 0.92 | 0.84 |
Abbreviations: RMSEA, Root mean square error of approximation, IFI, incremental fit index; CFI, comparative fit index; NFI, normed fit index.
4.3. Convergent and Divergent Validity
As seen in Table 3, the relationship between early life experiences and self-compassion was negative, indicating divergent validity of the scale (P < 0.01). Alternatively, the relationship between early life experiences and borderline personality traits and the difficulty in regulating positive emotion indicated the convergent validity of this scale (P < 0.01).
Abbreviations: ELES, Early Life Experiences Scale; SCS, Self-compassion Scale; STB, Schizotypal Trait Questionnaire-B form; DERS, Difficulties in Emotion Regulation Scale.
a P < 0.05
b P < 0.01
5. Discussion
This study aimed to investigate the factor structure and psychometric properties of the Persian version of the ELES in a sample of students. Cronbach’s alpha internal consistency coefficient was used to assess the validity of the ELES. The internal consistency coefficients showed that this scale has good reliability (with Cornbrash’s alpha coefficient for the total scale, submissiveness, feeling valued/unvalued, and feeling threatened to be 0.74, 0.85, 0.66, and 0.80, respectively). These results are consistent with research by Gilbert et al. (19), Gouveia et al. (22), and León-Palacios et al. (23). In the study of Gilbert et al., which was conducted to develop and assess the psychometric properties of the ELES, Cronbach’s alpha coefficients for the three factors of the questionnaire were 0.71 to 0.89 (19).
In the study of León-Palacios et al., conducted on 960 subjects to assess the psychometric properties of the ELES in Spain, Cronbach’s alpha coefficients for three factors were 0.81 to 0.90 (23). Gouveia et al. also obtained Cronbach’s alpha coefficients for three factors as 0.66 to 0.77 in adolescents aged 13 - 18 and 0.86 for the total scale (22). The ELES has three factors (submissiveness, threat, and unvalued). Preliminary studies related to the questionnaire development and those conducted in other countries confirmed the three-factor structure of the questionnaire (19, 22, 23). The results of this study are consistent with the mentioned studies. According to social ranking theory, defensive and submissive behaviors such as avoidance, passive inhibition, and withdrawal in case of problems are protective factors because child rebellion will increase criticism and reduce the emotional bond of parents. A child who frequently experiences criticism, humiliation, and rejection over time in the family context may represent others as powerful, hostile, and despotic and himself as worthless, vulnerable, and humble, which can cause too much attention to threats, sensitivity to criticism, shame, or signs of external rejection (18), leading to increased vulnerability to emotional problems in the future (21). In the study of Gilbert et al., test-retest reliability on 21 students did not show sufficient stability during two months (19). However, our research showed good test-retest reliability, consistent with the studies of Gouveia et al. (22) and León-Palacios et al. (23).
The borderline personality symptoms questionnaire and difficulty regulating emotion were used to assess convergent validity. The results showed a significant positive correlation between borderline personality symptoms (33) and difficulty in emotion regulation (34, 35). In explaining this finding, it can be said that childhood traumatic experiences have remarkable effects on the ability to respond adaptively to emotional challenges. These early experiences probably contain elements that enable teenagers and young adults to recognize and understand their feelings adequately but are incapable of responding to and coping with them (36). In addition, people with borderline personality traits have usually experienced early traumatic experiences in childhood, leading to negative emotions such as loneliness, rejection, abandonment, and shame (37); they often use dysfunctional emotion regulation strategies to cope with emotions (38). Self-compassion questionnaire was used to assess the divergent validity. Early life events significantly negatively affect self-compassion (39-41). In explaining these results, it can be said that compassion provides people with more experience of happiness, hope, courage, and positive emotions (42), and they experience less anxiety when thinking about life problems (43), so it can moderate the effects of early life experiences. Also, people with higher self-compassion due to being open and associated with their sufferings experience a sense of care and kindness towards themselves, along with understanding their inadequacies and failures.
This study’s limitations include using self-report tools, such as response sets and memory distortion. Some emotional changes, such as depression or mood swings, could lead to bias or memory changes. It is recommended to consider controlling variables that can change memory. We only used the student sample; others can check it in other samples to see if this factor structure is validated. Other tools, such as depression and anxiety that are associated with early life experiences, can be used to measure convergent validity.
5.1. Conclusions
Based on the results of this study, it can be said that the Persian version of ELES has psychometric properties (factor structure, validity, and reliability). Considering the importance of measuring early life experiences in the formation of psychological pathology and its impact on different aspects of life in different periods, this tool can be used in research and clinical practice (with caution). It is also recommended to investigate its psychometric properties in clinical populations.