1. Background
Breast cancer is one of the most common cancers among women worldwide. Despite many advances in its treatment, low life expectancy is a major problem that indicates the importance of cancer cells phenotyping, cell molecular composition, receptor expression, and the hormonal status of patients. These are great guides for choosing the right treatment for any individual with breast cancer (1).
Breast cancer is one of the diseases in which various hormone receptors are effective in its occurrence and metastasis, including the hormone receptors such as estrogen, progesterone, and epidermal growth factor HER2. Due to the importance of these receptors and their interaction with other receptors in the body, their expression is important in patients with breast cancer (2). However, many factors are effective in treating breast cancer, and choosing the appropriate treatment regimen should be determined for each person based on that personal factor. One of the most important factors in these patients is the status of hormone receptors and HER2 receptors. Nowadays, different treatment regimens for treating breast cancer focus on the hormone receptor or HER2 receptor, depending on the patient's condition (3). The status of the HER2 receptor is important because in HER2 positive breast cancer response to treatment is reduced, and the recurrence of the disease is increased, and limited drugs such as Trastuzumab are effective and used in combination with the individual's chemotherapy regimen. It has led to a remarkable improvement in treatment (4).
Another effective drug in prevention and treatment is Tamoxifen, which acts through estrogen receptors and, depending on its target tissue, can show estrogenic or anti-estrogenic effects in breast tissue due to the high density of estrogen receptors. The anti-estrogenic effects of Tamoxifen can play an important role in treating breast cancer (5). Chemotherapy alone is insufficient for younger patients with steroid hormone receptor-positive tumors because the ovarian tissue is not well-inhibited and sex hormones are still secreted, using Tamoxifen or GnRH analogs will help to suppress the hormonal secretion. Therefore, one of the important factors in choosing the treatment is the status of the sex hormones secretion and menopause in the patient (6, 7).
Another factor that changes the risk of breast cancer and responds to treatment is obesity and diabetes, which are on the rise worldwide. In these diseases, hyperinsulinemia, elevated IGFs, hyperglycemia, and elevated inflammatory cytokines happen, which interferes with the development and progression of breast cancer (8). One of the receptors involved in this pathway is the insulin-like growth factor-1 (IGF-1) receptor, which acts through the kinase pathway. Its relationship with the estrogen, progesterone, and HER2 receptors is not well-understood. It should be noted that the treatment of breast cancer without the metabolic disorders consideration may cause resistance to the treatment, so the metabolic status of the body and its relationship with the sex hormones should also be considered (9, 10).
The selection of the best drug for breast cancer treatment might be due to the patient’s hormonal and biochemical status that would determine the environment covering the tumor cells in different patients. There is a hormonal cycle in women and changes in the secretion of sex hormones during various years before and after menopause. In this study, the cellular response alterations of understudy drugs due to interaction by some commonly used anti-cancer drugs and sex hormones in the culture media is investigated.
2. Methods
2.1. Cell Culture
The human breast cancer SKBR-3, MDA-MB-231, ZR-75-1, BT-474, and MCF7 cells used were obtained from the cell culture laboratory of Pharmaceutical Research Center of Shahid Beheshti University of Medical Sciences (Tehran, Iran), were grown in RPMI 1640 (Gibco BRL, USA) media supplemented with 10% Fetal Bovine Serum (Gibco BRL, USA) and 1% PenStrep (Gibco BRL, USA) for testing Trastuzumab (Aryogen, Iran) and MTT assay. RPMI 1640 media without phenol red supplemented with 10% Newborn Calf Serum (Gibco BRL, USA) and 1% PenStrep was used for testing Tamoxifen (Iran Hormone, Iran), Ethinyl Estradiol (Iran Hormone, Iran), and progesterone (Iran Hormone, Iran). All the cells were grown in the humidified incubator with 5% CO2 at 37°C.
2.2. Clonogenic Assay
Clonogenic assay or colony formation is an in-vitro cell cytotoxicity assay based on the ability of the single cell to form a colony. The clonogenic assay enables an assessment of the differences in reproductive viability between the controlled untreated cells and cells that have undergone various treatments.
Single-cell suspensions were prepared by trypsinization. Then the cells were counted by trypan blue dye and hemocytometer slide, appropriate cell numbers were seeded in the 6-wells based on the doubling time of the cell lines, different concentrations between 0 - 200 µg/mL of drugs (Trastuzumab, Tamoxifen, Ethinyl Estradiol, and Progesterone) were considered for testing with the exposure time of 7 days. For each concentration, three replicates were considered. In order to normalize the resulting data, three controls were set by exposing the cells to compounds-free solvent in each set of experiments. The incubation time for colony formation varies from 1 - 3 weeks for different cell lines until enough acceptable colonies were formed in the control wells; it is accepted that the time must be equivalent to at least six cell divisions. After the colonies had formed, the supernatant was aspirated, and the wells were washed with normal saline. Then the colonies were fixed with 70% ethanol for 15 min and stained with trypan blue, and the number of colonies was counted (11).
2.3. Cell Growth Curve and Co-treatment
In order to study the effect of estrogen in the culture media and changes in the cell response to Tamoxifen, according to the status of the receptors of the tested cells, MCF7 and ZR-75-1 were selected. Cells were trypsinized, and after counting, 1.5 × 104 cells were seeded in 12 wells. Two hours after implantation of cells, the half-maximal effective concentration (EC50) of drugs calculated from the clonogenic assay was added to each well, and cells were counted for 12 days in different wells. The growth curve and growth slope of cells in different groups were compared with each other to measure the Tamoxifen effects on alive cells growth and duplication rates.
2.4. Cell Viability Measurement Using an MTT (3- (4,5-Dimethylthiazol-2-Yl)-2,5-Diphenyltetrazolium Bromide, A Tetrazole) Assay
Due to the expression of estrogen receptors in both MCF7 and BT-474 cell lines and the lack of expression of HER2 receptors in MCF7, these two cell lines were selected for this study using MTT assay. The MTT assay has been widely used to evaluate cell viability. The cells were trypsinized, and 1,000 - 3,000 cells were seeded in 96-well plates and allowed to attach for 24 h. Insulin was added to a group of cells at a concentration of 10 µg/mL to investigate its interference to the cellular pathway of estradiol and Tamoxifen. Different concentrations of drugs (0 - 200 µg/mL) were added to the cells and exposed for 24 h, then MTT (5 mg/mL) was added and cells were incubated for 4 h, the supernatant was removed, and DMSO was added to the medium to dissolve the formazan crystals, and the absorption was read at 570 nm (12, 13).
2.5. Statistics
The median inhibitory concentration (IC50) and the half-maximal effective concentration (EC50) were calculated by plotting the percent of cell survival vs. logarithm of compound concentration. All statistical analyzes were performed by GraphPad PRISM® 6 software (GraphPad Software, Inc.) using non-linear regression. Comparisons between the groups were made by a one-way analysis of variance (ANOVA) followed by an appropriate post-HOC test to analyze the difference. Data are expressed as mean ± SEM.
3. Results
3.1. Cells Survival Curves
Table 1 shows the results of the clonogenic assay after counting colonies and statistical analysis. The IC50 value of Trastuzumab is calculated at 2.88 ± 0.55 µg/mL for SKBR3, while the other under-study cell lines did not respond to this drug as was expected due to the lack of Her2 receptors in those cell lines.
| Cell Line | Subtype | Receptor Status | EC50 in µg/mL (mean ± SEM) Tamoxifen | IC50 in µg/mL (mean ± SEM) Trastuzumab | EC50 in µg/mL Estradiol | ||
|---|---|---|---|---|---|---|---|
| ER | PR | HER2 | |||||
| SKBR-3 | H | - | - | + | 3.01 ± 0.058 | 2.88 ± 0.55 | - |
| MDA-MB-231 | TNB | - | - | - | 6.3 ± 0.19 | - | - |
| MCF7 | LA | + | + | - | 2.36 ± 0.32 | - | 220 |
| ZR-75-1 | LA | + | +/- | - | 4.98 ± 0.48 | - | 180 |
a The ER, PR, and HER2 receptors of the cell lines are also indicated in a column for each cell line plus their subtypes as Luminal A (LA), HER2 positive (H), and Triple-negative B (TNB).
The four cell lines used in this article did not respond to the increasing progesterone concentrations. Up to 200 µg/mL progesterone was used in this study, but no toxicity was observed. The two cell lines of SKBR3 and MDA-MB-231 did not respond to the estradiol, and it was also expected due to the lack of estrogenic receptors in these cell lines. However, in the cases of MCF7 and ZR-75-1 cell lines with estrogen receptors, estradiol stimulated the growth at low concentrations and inhibited the growth at high concentrations. Such a phenomenon has been seen and reported with other investigators (14). As is shown in Table 1, Tamoxifen has affected all these cell lines irrespective of the presence or lack of different receptors. Tamoxifen was shown to be a toxic agent for all these cell lines with the maximum toxicity for the MCF7 cell line, and the least toxicity for the MDA-MB-231.
3.2. Growth Curve Alterations
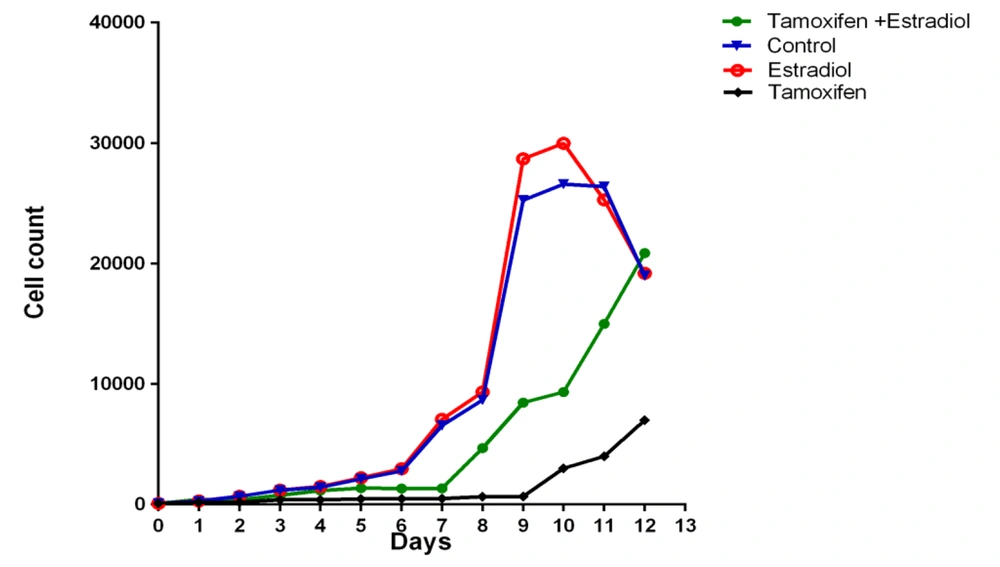
Figure 1 shows the results of the use of Tamoxifen and estradiol at their EC50s each for 12 days alone and then together on the MCF7 cell line, with the slope of each diagram at the logarithmic phase of the growth being presented at Table 2.
| MCF7 Cell Line | Control | Tamoxifen | Estradiol | Tamoxifen + Estradiol |
|---|---|---|---|---|
| Best Fit Values Slope | 2410 ± 419.3 | 401.8 ± 103.9 | 2527 ± 475.8 | 1447 ± 264.8 |
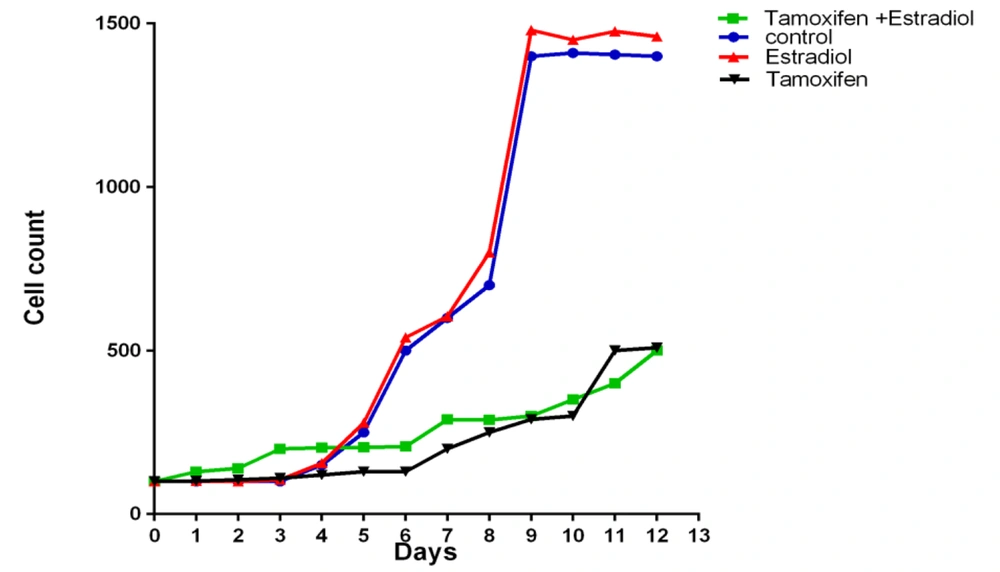
The ZR-75-1 cell line has also been studied in this experiment, and its growth curve changes are shown in Figure 2 and Table 3.
| ZR-75-1 cell line | Control | Tamoxifen | Estradiol | Tamoxifen + Estradiol |
|---|---|---|---|---|
| Best Fit Values Slope | 136.9 ± 15.88 | 29.46 ± 5.240 | 143.8 ± 16.14 | 28.27 ± 2.489 |
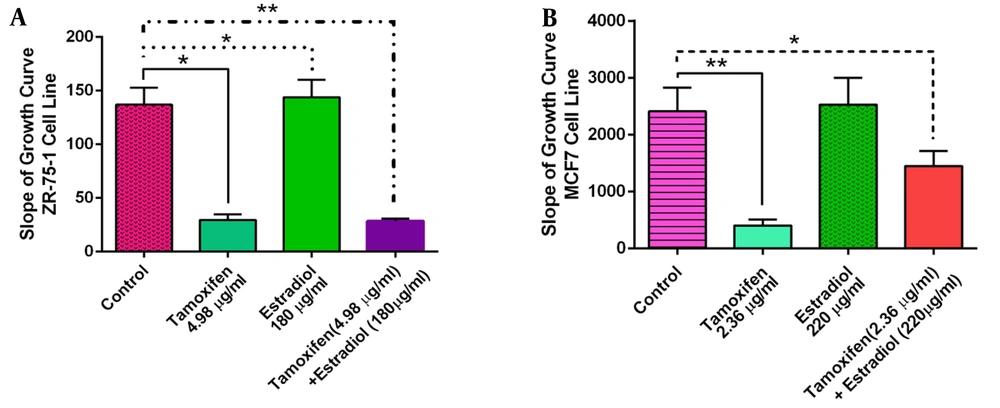
The statistical analysis of the data for the effects of estradiol or Tamoxifen exposure to these cell lines alone or combined is shown in Figure 3 for a better analysis of these agents effects on the cells growth.
3.3. Effects of Insulin
Table 4 shows the IC50 obtained from the MTT assay and the cell specifications used in this study. Please note that this table only presents the point of IC50s of estradiol and Tamoxifen in these cell lines with or without insulin, and does not necessarily show the principal effects of insulin on the toxicity of these agents. Insulin does not significantly change the IC50s of Tamoxifen on MCF7 (P-value = 0.0957) or BT-474 (P-value = 0.645) cell lines. However, the IC50 of estradiol was altered in both MCF7 (P-value = 0.006) and BT-474 (P-value = 0.0165) cell lines after the addition of insulin, significantly.
| Cell Line | Subtype | Receptor Status | IC50 in µg/mL (Mean ± SEM) Tamoxifen | IC50 in µg/mL (Mean ± SEM) Estradiol | ||
|---|---|---|---|---|---|---|
| ER | PR | HER2 | ||||
| BT-474 | LB | + | + | + | 4.62 ± 0.44 (without insulin) 4.9 ± 0.87 (with insulin) | 36.03 ± 2.55 (without insulin) 41.98 ± 0.62 (with insulin) |
| MCF7 | LA | + | + | - | 6.47 ± 0.17 (without insulin) 7.5 ± 0.8 (with insulin) | 18.43 ± 0.69 (without insulin) 23.11 ± 0.44 (with insulin) |
Abbreviations: LA, Luminal A; LB, Luminal B.
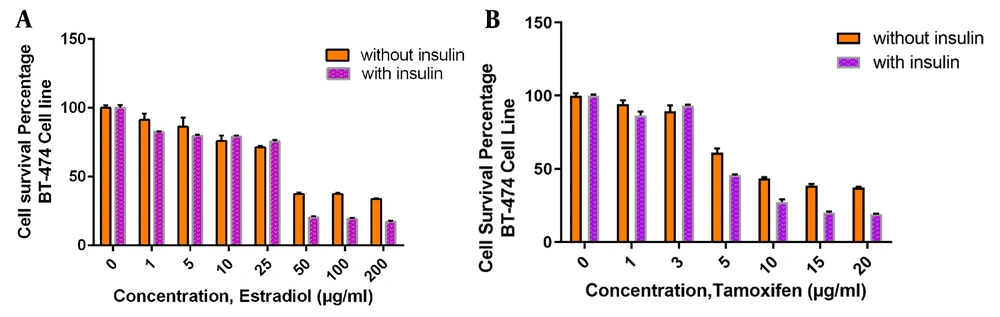
Figures 4 and 5 show the effects of insulin on the dose-response curves of the different concentrations of estradiol or Tamoxifen on BT-474 and MCF7 cell lines. As is shown in this figure, BT474 cells show a breakdown survival at the doses of 50 µg/mL of estradiol and 5 µg/mL of Tamoxifen (almost around the IC50 of these agents, as is shown in the Table 4). The 10 µg/mL addition of insulin to the media increases the cytotoxicity of both estradiol and Tamoxifen in any doses, with a higher magnitude of effect on these break downing doses for any of estradiol or Tamoxifen.
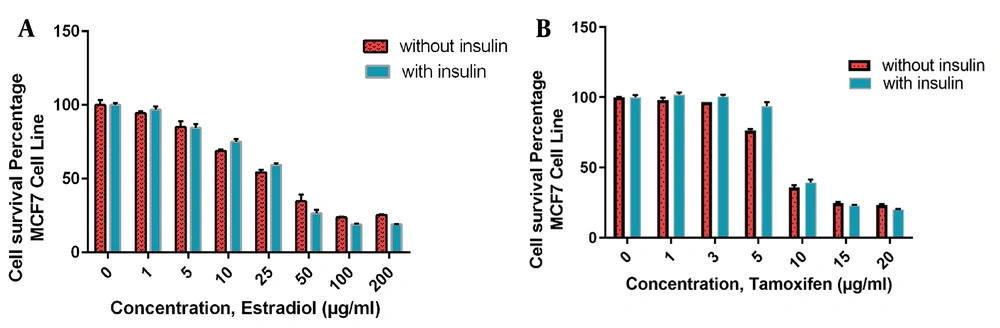
Figure 5, on the MCF7 cell line, presents a different role for insulin addition to the culture media. As is shown in Figure 5Aand B, insulin increases the cells resistance to the cytotoxicity of estradiol and Tamoxifen with a higher magnitude of resisting effect at the 50 µg/mL of estradiol and 10 µg/mL of Tamoxifen (around the IC50s of these agents).
4. Discussion
Breast cancer treatment and its challenges are one of the most important issues in medicine. The estrogenic receptor and its signaling pathway have a significant role in this issue. It is while that the traditional belief of estrogen being a pure proliferating and Tamoxifen, as an antiestrogen agent, acting as a solid anti-proliferating agent is shaken. Estradiol has presented a dual and tricky role on the cancer cells proliferation; to execute cell proliferation in physiologic but cytotoxicity in high concentrations. Tamoxifen has also been shown to present proliferating effects in some cell lines that have co-expression of ER and HER2 (14). Various receptors and their cellular signaling pathways are the most reasonable candidates to explain these paradoxes. Although the traditional estrogen gene expression stimulation might work through the formation of a dimer and DNA binding adventure, its non-genomic pathway of EGFR and HER2 phosphorylation leading to PI3K/Akt and MAPK activation might be responsible for its diverse effects in different breast cancer cell lines (15). Again, the traditional anti-estrogenic effects of Tamoxifen might weaken with its long application through the EGFR signaling pathway in some cell lines. Some other interfering agents on this pathway are coming along one by one to present their roles in estrogen chiastic adventure, including insulin that has shown a cross-talk between its IGF1R with the EGFR and HER2 pathways. In our experiments using different cell lines with the various expressions of the above receptors, we have explored these complexities further.
To show that the cellular characteristics of our five selected cell lines are in agreement with the previous publications for such an adventure, a general cytotoxicity assay was performed, and Trastuzumab blocked the HER2 positive cell line of SKBR-3 growth (IC50 = 2.88 ± 0.55 µg/mL), high doses of estradiol blocked the proliferation of MCF7, BT-474, and ZR-75-1 cell lines. In contrast, Tamoxifen blocks all of these cell lines. For the Trastuzumab, in a study, by Costantini et al., that investigated the possibility of breaking the resistance to this drug in the Trastuzumab-resistant cell lines, the MDA-MB-231 cell line showed similar results to our study and didn’t respond to the drug. In another study, Trastuzumab has been applied on two cell lines with a positive HER2 receptor of BT-474 and SKBR-3, and the MCF7 cell line with the final result confirming our study. As per our results, they have also confirmed that the MCF7 cell line did not respond to this drug, indicating that HER2 receptor expression is required to respond to the treatment with Trastuzumab, and if this receptor is not expressed in patients, there will be no benefit from treatment with this drug. In the study of Zazo et al., the sensitivity of different cell lines to the presence of Trastuzumab with a concentration of 15µg/mL in their cell culture for 7 days was investigated, and the cell proliferation changes were compared with the control group. These investigators have also observed that the SKBR-3 cell line is one of the sensitive categories to this drug and its growth rate has decreased by 50.67% (16-18). Looking at our cytotoxicity results on the selected cell lines and the above mentioned references confirms the features of these cell lines for the understudy receptors and signaling pathways.
Our results of Tamoxifen cytotoxicity on these cell lines presented the following rank order: MCF7 > SKBR-3 > ZR-75-1 > MDA-MB-231. The highest level of cytotoxicity is observed for the MCF7 cell line. Tamoxifen is a non-steroidal drug that treats breast cancer with positive hormone receptors and works through the ER-mediated transcription cascade. However, it was also useful in estrogen receptor-negative cancers and causes toxicity through apoptosis and activation of the caspase-3 pathway. In Salami and Karami-Tehrani experiment, two cell lines, MCF7 and MDA-MB-468, with different expressions of estrogen receptors were studied. During this study, caspase cascade and proteins involved in apoptosis were studied. The MCF7 cell line has shown more sensitivity to Tamoxifen, presumably through the estrogenic receptors. However, the toxicity of the MDA-MB-468 cell line has been observed through the activation of the caspase pathway, with no alterations in the Bcl-2 and Bax apoptotic proteins (19, 20).
In another study, 5 cell lines (SKBR-3, MDA-MB-231, MDA-MB-468, MDA-MB-453, and HCC-1937) that are ER-negative were examined, and Tamoxifen acts on these cells through the CIP2A-dependent p-Akt downregulation and causes apoptosis. It was found that ERβ receptor is expressed in these cell lines as one of the factors in the cell response to Tamoxifen in both ER-positive and ER-negative breast cancer patients (21, 22). This study generally agrees with other studies that have shown differences in the response to Tamoxifen of ER+ and ER- breast cancer cells in-vitro.
Among the cell lines studied in our experiments, the MCF7 and ZR-75-1 cell lines have estrogen receptors and respond to the addition of estradiol in the media. According to the results of the clonogenic assays, it was observed that low concentrations of estradiol have a stimulating effect on growth, which gradually changed to the growth inhibitory effect with the increasing concentrations. When the concentration of 10 nM of 17β-estradiol was exposed to the MCF7 cell line for 48 hours, the Bcl-2 protein was increased and protected cells from apoptosis (23). In another article, the effects of androgenic and estrogenic compounds on the ZR-75-1 cell line have been studied, and it has been observed that these two substances can neutralize the effects of each other, while estradiol exerts its effects faster than androgens (24).
We have also investigated the effects of the estradiol and Tamoxifen presence in the culture medium in this paper. According to Tables 2 and 3 and Figure 3, the ZR-75-1 cell line was also more sensitive to the effects of estradiol in a dose-dependent manner with a significant growth difference from the control cells. The magnitude of growth difference in the presence of estradiol was not significant for the MCF7 cell line. Tamoxifen, meanwhile, significantly inhibited the growth of both cell lines. In agreement with our results, Katzenellenbogen et al., have also shown that the estrogenic stimulating effects of estradiol are not as potent as the Tamoxifen inhibitory effects on the MCF7 cell line (25). In another study comparing the growth stimulation and inhibition effects of estradiol and Tamoxifen on the ZR-75-1 cell line, cells were grown in the serum-free media to eliminate the potential effects of estrogens in the serum. These cells were exposed to the increasing concentrations of estradiol with or without Tamoxifen. The final result has confirmed that estradiol can only neutralize some of the inhibitory effects of Tamoxifen, being less potent on the estrogenic receptors than this drug (26).
Our results as shown in Figure 3 on the growth performance of the two cell lines in the presence of estradiol, Tamoxifen, and co-administration of these agents, have also confirmed that the inhibitory effects of Tamoxifen on cell growth are superior when co-administered with estradiol. The ZR-75-1 cell line is more sensitive to these effects and has a higher response to the estrogenic and anti-estrogenic compounds than the other cell lines studied in our experiments.
Insulin has been shown to have a meditative role during previous estrogenic or HER-2 studies. Different researchers have added different concentrations of insulin to the cells' growth media while investigating the effects of estrogen, Tamoxifen, or Trastuzumab (27, 28). We have also looked at the potential effects of insulin on the two cell lines with variable kinds of receptors. Table 4 shows the effects of insulin in the cell media of MCF7 and BT-474 and the changes in their response to the estrogenic and anti-estrogenic compounds of the estradiol and Tamoxifen. As the results show, insulin has no effect on the toxicity of Tamoxifen in either cell line while moderated the effects of estradiol toxicity at high concentrations.
Just as estrogen can stimulate estrogen receptors and cell proliferation, and its role in breast cancer is well-known, other factors, like the insulin-like growth factors (IGFs), also stimulate estrogen receptors in ER-positive breast cancer cell lines. This evidence has suggested that these two cell proliferation regulatory pathways are linked to each other and that the stimulation or inhibition of each pathway might affect the performance of the other. Insulin-like growth factor IGF-I protects many cells against apoptosis. One study has found that blood insulin levels were elevated in patients with uterine cancer and were directly related to tumorigenesis in these patients. Insulin is a mutagenic and anti-apoptotic agent for many types of cells, and these effects are dependent on the PI3K/Akt pathway (29, 30). These findings confirm the results of our study on the toxicity of estradiol on the MCF7 and BT-474 cell lines showing that the presence of insulin in the cell media protects them against high doses of estradiol toxicity. One possibility to express these controversies might be looking at the cells' proliferation or cytotoxicity. Table 4 and Figures 4 and 5 represent two different assumptions in presenting cytotoxicity of estradiol and Tamoxifen, with Table 4 focusing on the IC50 and Figures 4 and 5 on all ranges of different concentrations. Looking at Table 4, insulin increases the IC50 of estradiol but does not affect the cytotoxicity of the Tamoxifen. However, there is a different story with Figures 4 and 5. The cytotoxicity pattern of estradiol and Tamoxifen is presenting a well-sigmoidal shape with the breakdown values of 5 µg/mL for Tamoxifen and 50 µg/mL for estradiol. The IC50s of these agents are within this falling range where the cell signaling may undergo dramatic alterations.
A single value of IC50 within this range might well present an idea for the relative effects of different agents, but it is misleading in signaling interpretation. With a careful look at the other bars in Figures 4 and 5, Insulin increases the resistance of MCF7 cells to both estradiol and Tamoxifen, while a reverse feature is shown for these agents' application on the BT-474 cell line which expresses HER2. Insulin has presented synergistic effects with estradiol through the PI3K/Akt pathway that eventually induces cell proliferation (31). Tamoxifen has also been shown to present estrogen agonistic effects on cell proliferation in ER and HER2 positive cell lines like BT-474. This is also through the cross-talking between ER, EGFR, IGF1, and HER2. 4-hydroxy tamoxifen is about 4 times stronger than Tamoxifen on estrogen receptors. MCF7 cells growth inhibition is not high when these cells are exposed to this agent, unless when both IGF1-R and ER are suppressed. Our finding is in agreement with this observation since MCF7 cells exposed to insulin that stimulates IGF1-R became more resistant to Tamoxifen and estradiol high doses. On the other hand, 4-hydroxy tamoxifen has strongly inhibited the growth and proliferation of BT-474 cells that are overexpressing HER2 but are low in IGF1 receptor (32). Our result does not agree with this experiment, as we have seen an increase in cytotoxicity in BT-474 while exposed to both Tamoxifen and insulin that stimulates IGF1. Estradiol is also presenting the same cytotoxic effects on BT-474 when it is co-exposed to insulin in our results. This might indicate the presence of some other interfering mechanism in the cross-talk of IGF1 and HER2 in the presence of ER that needs more investigations, and adds to the complexity of this story. Although Insulin has protected these cells against the high doses of estradiol, but did not present any significant effects on the toxicity of Tamoxifen.
The phosphoinositide-3 kinase (PI3K) pathway has been identified as an important target in breast cancer's appearance or therapeutic outcome. This pathway is probably one of the most important pathways in cancer metabolism, growth regulation, proliferation, and cell survival. Various factors cause resistance to endocrine therapy, one of which is activating the PI3K pathway. PI3K pathway is one of the common pathways between the three receptors, estrogen, HER2, and IGF-I. Studies show that increasing the activity of the PI3K signaling pathway causes resistance of cells to anti-HER2 treatment. This signaling pathway also interferes with the expression of estrogen receptors in ER-positive breast cancer, reducing the expression of estrogen receptors in these cells, thereby creating resistance to hormonal therapy. Insulin resistance, type 2 diabetes, and hyperinsulinemia also increase the activity of the PI3K signaling pathway, thereby impairing the response to HER2 and ER targeted therapy in cancer patients with a background in these diseases (33, 34).
One of the non-genomic mechanisms by which Tamoxifen works is the G protein-coupled receptor of GPR30. This receptor is present in most of the ER-positive breast cancers, including MCF7 and ZR-75-1 cell lines that Tamoxifen inhibits their growth. GPR30 might well be a good reason for the sensitivity of these cell lines to the effects of Tamoxifen in the presence or absence of the estrogen receptor stimulating factor of estradiol. The same outcome has also been seen in our results of the co-treatment of cells with estradiol and insulin when the effects of Tamoxifen have always been predominant. However, there are reports that the chronic exposure of cells to Tamoxifen and the long-term treatment of patients with this agent might cause resistance to the drug. One of the reasons is the translocation of the GPR30 receptor, which activates the EGFR and PI3K pathway and thus creates resistance to the Tamoxifen, adding to the multifactorial nature of breast cancer therapy (35, 36).
4.1. Conclusion
The mechanism of cellular signaling cross-talk isn’t a one-way pattern, each of the pathways increasingly affects the other signaling cascades, and not all of them produce similar results, making any simple outcome prediction for the cancer treatment so difficult. The results of the exposure of cells to any of these factors alone or in combinations are not accurately predictable. With the present knowledge, a simple selection of drugs for breast cancer patients with various cell types and biological environments is almost impossible. A complete examination of the presence of various receptors on the neoplastic cells and the amount of different growth-stimulating agents in any individual with breast cancer is required before making any final decision on the treatment protocol for such a patient.