Socio-economic inequalities in medicines prescription can impose substantial burdens on the health systems. Current research investigates such inequalities in the pharmaceutical sector of Iran. In general, while non-prescribed medicines were concentrated among disadvantaged groups, a significant pro-rich was observed in the use of prescribed medicines in Iran. We explained these socio-economic inequalities through decomposition analysis.
The concentration index indicated a pro-rich distribution of prescribed medicine use in Iran. We also adjusted this pro-rich inequality relative to the need factors that lead to a pro-rich horizontal inequity in the prescribed medicine use. Our finding is inconsistent with previous studies (
25,
26) that reported favorable access to medicines in the Iranian pharmaceutical market. It seems that these studies neglect the accessibility dimension of access that is predominantly related to the household's ability to pay. But the results of some studies indicate the existence of inequality in medicine use in Iran (
27,
28), which is consistent with our results. Inequality in the Iranian pharmaceutical sector can be consistent with other studies showing inequality in health services (
29,
30). Therefore, since healthcare services are concentrated among the better-off, a rich distribution of prescribed medicine use in Iran can be justified. Our results are consistent with previous studies that observed pro-rich inequality in pharmaceutical spending (
31) in Brazil and also prescribed medicine use in Canada, Denmark, and Uruguay (
8,
32,
33). Previous studies in China have shown pro-rich inequality in anti-diabetic (
11) and anti-hypertensive (
12) drug treatment. One international study also reported different socio-economic inequalities in terms of concentration index for secondary prevention of cardiovascular disease in some of LMICs and Sweden. While countries such as Saudi Arabia, China, Colombia, India, Pakistan, and Zimbabwe had pro-rich socio-economic inequality, pro-poor distributions were found for Sweden, Brazil, Chile, Poland, and the occupied Palestinian territory (
34). This showed a significant variation in the access to medicines in the world.
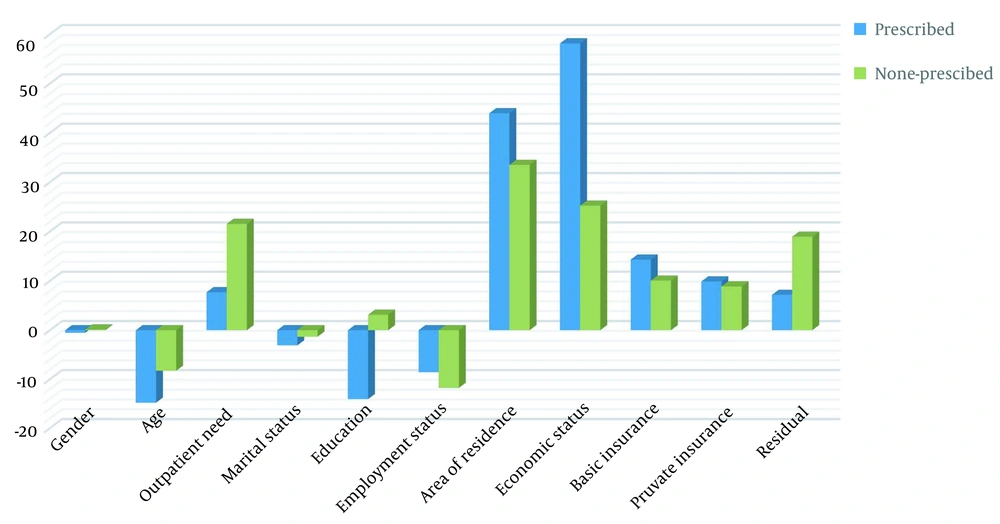
The results showed that the economic status of the households explains about 60% of the observed pro-rich inequality in prescribed medicine use. Although there are no studies with the same methodology that surveyed adult participants, our results are in line with a former study that tried to explain socio-economic inequities in medicine use among Brazilian children (
35). Another study in China found income to be the most important factor explaining socio-economic inequality in diabetes medication (
11). Our result is consistent with a previous Iranian study that reported inequality in healthcare use (
29). There are substantial debates about decreasing subsidies in the pharmaceutical market of Iran that may exuberate socio-economic inequality in medication and healthcare utilization. Location of residence was another main contributor to the observed inequality in the prescribed medicine use. Similar to our findings, other studies (
35,
36) showed that people living in remote areas have poor access to essential medicines. Although Iran has a well-organized rural health system (
37), a former study (
29) showed that residence in rural areas could increase pro-rich inequality in healthcare utilization. Basic and private health insurance were other factors that played a positive role in inequality in the prescribed medicine use. According to Anderson's model of behavioral use of health care, health insurance can be considered as an enabling factor that facilitates access to health care services (
38). Expanding the health insurance benefits package could increase access to needed drugs in Iran. However, blind health financing reforms may increase healthcare costs by increasing pharmaceutical expenses. Due to the positive impact of the national essential list on universal health coverage (
1), Iran should promote this strategy and require various health insurance plans to include these drugs in their benefits packages.
The concentration index also revealed an inequality in favor of the poor in non-prescribed medicine use in Iran. This finding contrasts with a former Iranian study (
20) that reported pro-rich socio-economic inequality in self-medication in Iran. In previous research, authors used household budget data provided by the Statistics Center of Iran. These data are monetary data and do not accurately show health-seeking behaviors. Since poor households may not have enough affordability to pay for non-prescribed medicines, the definition of self-medication in this study may be restrictive. Hence, it seems self-medication in Iran is distributed among lower socio-economic groups. This means that poor people in Iran generally use medicines they already have at home or probably seek to use over-the-counter medicines to meet their health needs. It should be noted that in this study, self-medication was used both for people who did not seek healthcare services and for those who used pharmacy drugs without a prescription. Of course, the frequency of the first case was higher in our study. Our finding is consistent with a previous local study (
27) which showed that self-medication in a province of Iran is concentrated among the poor. There were no international studies on socio-economic inequality in non-prescribed medicine use. However, there are contradictory results observed regarding the socio-economic determinants of this kind of medicine use. Some studies (
39) have shown that higher socio-economic groups are more likely to use non-prescribed medicines. In contrast, other studies (
40,
41) have shown that this practice is more common among lower socio-economic groups. Decomposition analysis showed that residence was the main driver of pro-poor inequality in non-prescribed medicine use. As previously discussed, rural residents have poor access to health care, especially for complex healthcare needs. Economic status was another major contributor to the pro-poor inequality in non-prescribed medicine use, explaining about 25 percent of it. This is could be related to the higher use of non-prescribed medicine among disadvantaged groups, which has been confirmed in other studies (
40,
41). The number of healthcare needs was another key determinant in the inequality in this type of medicine use. This indicates that people with poor health take medication to meet their health needs without consulting a doctor. Hence, healthcare authorities should facilitate the access of people in need of health services to the required medicines. In any case, it seems that self-medication in Iran is related to the accessibility of healthcare services. Therefore, the implementation of policies that increase access to health services by increasing insurance coverage can also greatly reduce the pro-poor inequality in non-prescribed medicine use. However, the impact of cultural and behavioral factors on self-medication should not be overlooked (
42), which unfortunately were not considered in this study.
Although this research provided valuable evidence on socio-economic inequality in Iran's pharmaceutical sector, some limitations in the interpretation of the results should be considered. First, this study only explored overall medication and could not be used for socio-economic inequality for specific drugs. Socio-economic disparities for some drugs may be much greater. It is suggested that future studies perform inequality analysis for different drugs. Second, the self-reported nature of the data may lead to recall bias. Third, this is a cross-sectional analysis, and our findings necessarily fail to demonstrate a causal relationship between the independent variables and medicine use.
5.1. Conclusions
We observed significant pro-rich inequality in prescribed medicine use as well as pro-poor inequality in non-prescribed medicine use in Iran. Economic status and location of residence were key factors that contributed to the pro-rich inequality in the use of prescribed medicines. The order of these factors for socio-economic inequality in non-prescribed medicine use was reversed. Anyway, it seems that paying subsidies to disadvantaged households and facilitating the access of residents in rural areas can reduce socio-economic inequalities in the pharmaceutical market of Iran. In addition, it seems that the inclusion of the National Essential Medicines Strategy in healthcare financing can moderate the socio-economic inequalities in medicine use in Iran.