1. Background
The presence of foreign bodies in the ear is a significant and critical emergency in the emergency department, with an estimated 11% of cases seen in ENT services involving foreign objects. Severe complications occur in approximately 22% of these cases, highlighting the potential risks associated with foreign bodies (1, 2). Unauthorized attempts to remove such objects can lead to irreparable damage. Research conducted in the United States indicates that children are most commonly affected, often inserting objects into their ears out of curiosity. In contrast, adults typically encounter foreign objects like pieces of cotton or matchsticks. Children may insert foreign bodies into the ear canal due to curiosity or improper ear-cleaning habits using tools like ear cleaners. Foreign bodies can be classified into metallic and non-metallic, simple and non-simple, or soft and hard. The removal methods vary based on the type of foreign body, its location, and the patient's cooperation (3, 4).
Materials that people have access to, whether edible or non-edible, can enter the ear, be swallowed, or become lodged in the airways. The size, shape, and consistency of these materials are crucial in determining the risk of mortality or complications due to airway obstruction. A foreign object in the nose may remain there for an extended period, leading to symptoms such as unilateral nasal obstruction, chronic and worsening purulent rhinitis or sinusitis, foul-smelling and unilateral secretions, and frequent nose manipulation by the affected person (5, 6). When a foreign object enters the body, it triggers a reaction that causes swelling, inflammation, and redness. This inflammation can make it more challenging to remove the foreign body, emphasizing the need for prompt removal before a significant inflammatory reaction occurs (7).
A foreign body in the ear can cause damage to the eardrum or middle ear. Symptoms of a foreign body in the ear may include ear pain, eardrum perforation, secretions due to otitis externa, or a feeling of fullness in the ear. Complications of not removing foreign bodies include bleeding and blood clots in the external ear canal (26%), eardrum damage or rupture (7%), severe infections of the external ear, and ultimately, hearing loss (8).
Although removing a foreign body from the ear is a relatively simple procedure, its potential complications necessitate the assistance of an otolaryngologist. The successful removal depends on several factors, including the location of the foreign body, the material involved, the doctor's skill, the available equipment, and the patient's cooperation (9).
Removing foreign bodies from the ear requires sufficient skill and knowledge, as attempts by non-specialists can cause damage to the external ear canal, perforation of the eardrum, or compression of the foreign object at the end of the ear canal. Such complications can exacerbate the patient's problems and make removal more challenging for medical staff.
Different methods are available for the correct removal of foreign bodies, and the choice of method should be at the discretion of the specialist. The most common approach involves using forceps and local anesthesia, which is effective when the foreign body has not penetrated deeply into the ear canal. Other methods include the use of syringes and warm water to remove deep-seated objects, provided there is no damage to the canal or eardrum and no bleeding from the ear (10). Surgery may be necessary when the foreign body is lodged at the end of the ear canal and cannot be removed by non-invasive methods. In cases where the patient does not cooperate despite all efforts, general anesthesia may be required, particularly in children (11).
2. Objectives
The main purpose of this research is to determine the types of foreign bodies, age distribution, and potential risks associated with improper removal or non-removal. Given the serious dangers posed by these foreign objects and the lack of similar research in Qom city, a detailed investigation is warranted.
3. Methods
This descriptive and cross-sectional study was conducted in 2019 using a census method on patients referred to Kamkar-Arabnia Hospital of Qom University of Medical Sciences. Initially, a set of inclusion and exclusion criteria were established. The inclusion criteria were: (1) the patient's file is complete; and (2) the patient presented to the hospital with a complaint of a foreign body in the ear. The exclusion criteria were: The patient's file is incomplete or illegible.
Data were collected using a checklist that included information on age, sex, type of foreign body, method of removal, and complications caused by the foreign body. This data was extracted from the patient's file, entered into SPSS 18, and analyzed using descriptive statistics, including prevalence, percentage, standard deviation, and mean.
4. Results
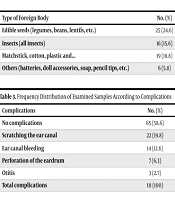
In this study, the results indicated that a total of 102 people participated, with an average age of 7.11 ± 12.41 years. Most participants were male (58.9%, n = 60), and the age group of 0 - 6 years comprised 49% (n = 50) of the participants (Table 1). The majority of foreign bodies were seeds (35.2%, n = 36), edible seeds (24.6%, n = 25), and matchsticks, cotton, and plastic (18.8%, n = 19) respectively (Table 2). In terms of complications, most individuals experienced no complications (58.6%, n = 65), followed by ear canal scratching (19.8%, n = 22) and ear canal bleeding (12.6%, n = 14) respectively (Table 3).
| Variables | No. (%) |
|---|---|
| Gender | |
| Female | 42 (41.1) |
| Man | 60 (58.9) |
| Age category | |
| 0 - 6 | 50 (49) |
| 6 - 12 | 32 (31.4) |
| 12 - 18 | 8 (7.8) |
| Over 18 years | 12 (11.8) |
| Type of Foreign Body | No. (%) |
|---|---|
| Seeds (beads, beads, rosary seeds, pearls, etc.) | 36 (35.2) |
| Edible seeds (legumes, beans, lentils, etc.) | 25 (24.6) |
| Insects (all insects) | 16 (15.6) |
| Matchstick, cotton, plastic and... | 19 (18.8) |
| Others (batteries, doll accessories, soap, pencil tips, etc.) | 6 (5.8) |
| Complications | No. (%) |
|---|---|
| No complications | 65 (58.6) |
| Scratching the ear canal | 22 (19.8) |
| Ear canal bleeding | 14 (12.6) |
| Perforation of the eardrum | 7 (6.3) |
| Otitis | 3 (2.7) |
| Total complications | 111 (100) |
In this section, the results indicated that in the age group of 0 - 6 years, most foreign bodies were seeds. In the 6-12-year age group, seeds were also common, with 9 cases, while in the 12-18-year age group, 5 cases involved seeds. For individuals over 18 years old, most foreign bodies were matchsticks, cotton, and plastic (Table 4). Additionally, only 22 patients required anesthesia for the removal of the foreign body (Table 5). In the age groups of 0 - 6, 6 - 12, and 12 - 18 years, the majority of foreign bodies were removed without complications. However, 5 individuals over 18 years old experienced ear canal bleeding.
| The Age Range (y) | Grains | Edible Seeds | Insects | Matchstick, Cotton, Plastic and... | Other |
|---|---|---|---|---|---|
| 0 - 6 | 21 | 16 | 5 | 11 | 5 |
| 6 - 12 | 9 | 7 | 7 | 1 | 1 |
| 12 - 18 | 5 | 1 | 2 | 1 | 0 |
| Over 18 | 1 | 1 | 2 | 6 | 0 |
| Gender | Perform Anesthesia | Without Anesthesia |
|---|---|---|
| Man | 13 | 47 |
| Female | 9 | 33 |
| Total | 22 | 80 |
5. Discussion
This study aimed to conduct an epidemiological investigation of foreign bodies in the ear, as well as their treatment and complications, at Kamkar-Arabnia Hospital in Qom in 2019. A total of 102 participants were included in the study. According to existing studies, the incidence of foreign bodies in the emergency room ranges between 1 - 3%, highlighting its importance as a critical issue that sometimes requires prompt intervention (12, 13).
The results of this study showed that the average age of the participants was 12.41 ± 7.11 years. Most participants were male and in the age group of 0 - 6 years. The most common foreign bodies were seeds, edible seeds, matchsticks, cotton, and plastic, respectively. In terms of complications, most participants experienced no complications, while others had ear canal scratches or bleeding. A study found that more than 50.1% of patients were 8 years old or younger, with a predominance of males. In adults, foreign bodies in the ear were often self-inflicted due to personal needs (13). Similarly, a study by Hashemi et al. reported that most patients were male and under 15 years old (14). These findings align with our study, emphasizing the importance of considering the gender and age of individuals, as young children often insert foreign objects out of curiosity or play, and males might be more frequently affected due to external work environments.
In a study conducted by Mangussi-Gomes et al., it was found that 9.5% of patients required additional tests to detect the foreign body, while 69.4% were identified using a simple CT scan. However, CT scans are not always effective in detecting certain foreign objects, such as fish and chicken bones. Thus, for suspicious cases, further diagnostic measures are necessary, as the types of foreign bodies can vary based on geographical and social characteristics (13). For instance, in developing countries, foreign bodies are often seeds or cotton pieces, while in developed countries, plastic pieces are more common (15, 16).
In this section, the results showed that the primary foreign body in the age groups of 0 - 6, 6 - 12, and 12 - 18 years was seeds, while individuals over 18 years of age more commonly had matchsticks, cotton, and plastic. Only 22 patients required anesthesia for foreign body removal. Additionally, in the age groups of 0 - 6, 6 - 12, and 12 - 18 years, most individuals had the foreign body removed without complications. However, 5 individuals over the age of 18 experienced canal bleeding. In other studies, only a small percentage of patients required anesthesia for foreign body removal, which is consistent with our findings (13). Furthermore, the rate of complications in our study was very low, aligning with similar research (17, 18).
The differences observed across studies in the need for general anesthesia and complication rates may be attributed to the fact that our cases were managed exclusively by otolaryngologists. As specialists in this field, they are adept at handling foreign body cases, thereby reducing the likelihood of complications. It is crucial to follow up with patients, particularly when insects or other foreign objects that do not cause infection are present.
The rapid removal of foreign bodies from the ear using traditional methods poses a significant challenge for otolaryngologists. Treatment success depends on various factors, and there is no conclusive evidence favoring one method over others. However, it is known that the persistence of foreign bodies in the ear, nose, and throat for more than 72 hours, along with repeated removal attempts, increases the risk of complications. Such situations are both unpleasant and unusual, and they significantly diminish the chances of successful removal.
A strength of this study is its focus on an important issue that has not been extensively studied at the university level, particularly concerning certain age groups. A limitation of the study was the presence of incomplete and illegible files. Future research is recommended to involve longer-term studies and interventions, examining how different medical approaches affect the removal of foreign bodies based on the type of foreign material and specific age groups.
5.1. Conclusions
Based on the study results and the complications associated with foreign bodies in the ear, it is essential to develop and implement strategies to prevent the entry of foreign bodies and to plan for their effective removal if necessary.