1. Background
Bier's block is the technique of administrating intravenous local anesthetic substances in a region where its venous return is mechanically impeded by a tourniquet. This technique was first described by August Gustav Bier in 1908 (1) and has evolved to a popular technique with analgesia reaching success rate of above 95% (2, 3). This approach has undergone technical modifications since it was first introduced and when compared with general anesthesia, this technique provides clinical benefits of rapid recovery, lower incidence of post-operative nausea and vomiting, and timely same-day discharge (4-7). Although this technique has been traditionally used in operating rooms, the mentioned advantages make it suitable for use as an analgesic method in the emergency department (ED).
There are limited studies evaluating the safety and effectiveness of Bier’s block at the emergency department. There are studies, which have shown the effectiveness of this technique at the emergency department when used for management of upper extremity fractures in children (8, 9). Another study by Mohr also proved the safety and effectiveness of this technique in outpatient clinical settings for the adult population (10).
2. Objectives
In this study, we aimed to compare the effectiveness, complications, duration, hemodynamic stability and patient and physician satisfaction between systemic analgesia and Bier’s block method performed at the emergency department.
3. Patients and Methods
3.1. Study Design
This was a non-blinded randomized clinical trial performed at two tertiary health care centers, with census of 65,000 and 35,000 visits per year, during years 2012 and 2013. The study design was approved by ethics committee of the corresponding university and submitted to the National Clinical Trials website with ID, name of the hospitals, university and country removed for blinding purposes. Informed consents were obtained from patients and patients who refused to participate in the study were excluded from the study and received analgesia based on the physician responsible for analgesia preference.
3.2. Population
All adult Patients (aged 18 or more) with upper extremity trauma who needed procedural analgesia in the ED were included in this study. Patients with a history of seizure, known allergy to analgesic substances, sickle cell anemia, peripheral vascular disease and arteriovenous fistula or infection in upper extremities were excluded from the study. Patients who needed emergent intervention/s that last more than one hour were also excluded from the study. Randomization was done using sealed envelopes containing computer-generated block random allocation numbers.
3.3. Intervention
After introduction of the protocol of Bier’s block (using 2 mg/kg of 0.5% lidocaine) or systemic analgesia (using midazolam 0.1 mg/kg and fentanyl 3 µg/kg initially, additional doses of midazolam 0.05 mg/kg and fentanyl 1 µg/kg given every 10 minutes as needed), patients underwent the necessary procedure. Physicians who were responsible for the analgesia, had authority to change the method of analgesia in each group, if necessary.
3.4. Measurements
Patient’s age, sex, site and type of injury, vital signs and pain score using the Numerical Rating Scale (NRS) were recorded before the introduction of analgesia. Patient’s vital signs were documented at the end of the procedure. Satisfaction of the patient, surgeon and physician responsible for analgesia for the applied analgesic method was obtained before discharge from the ED operating room. Patients also scored their level of pain before discharge and their vital signs were recorded at another instance. Time of initiation of analgesia, initiation of procedure, end of procedure, and gaining consciousness in systemic analgesia group and time of discharge from ED operating room were documented and patients were discharged from the ED operating room when eligible.
3.5. Statistical Analysis
All data were entered and analyzed by the SPSS software version 18.0 for windows (SPSS Inc., Chicago, IL). Numerical variables were presented as means (SD), while categorical variables were summarized by absolute frequencies and percentages. Chi-square test, independent samples T-test and general linear model were used for comparing the two groups. To detect a statistically significant difference in NRS scores with two-sided type 1 error of 10% and power of 80%, sample size of 30 per group was sufficient.4. Results
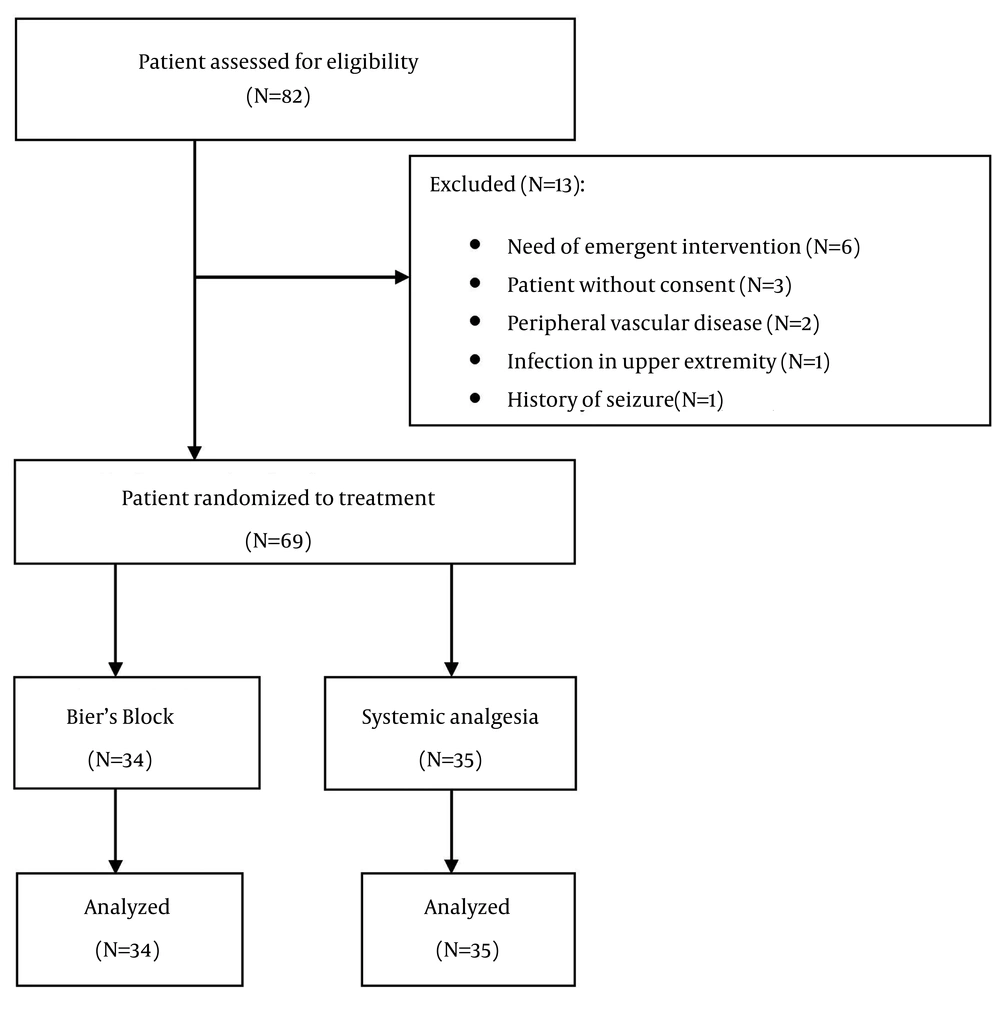
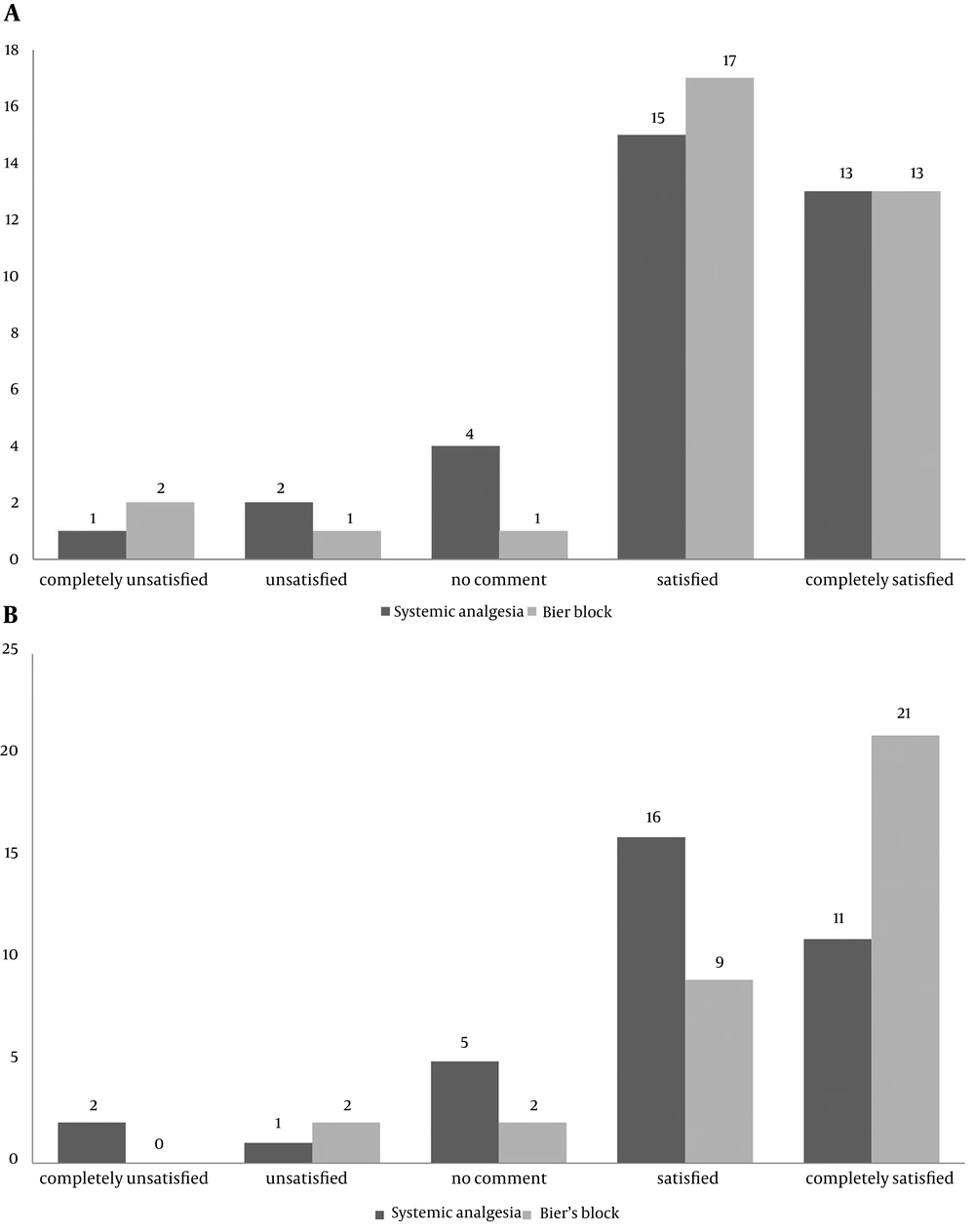
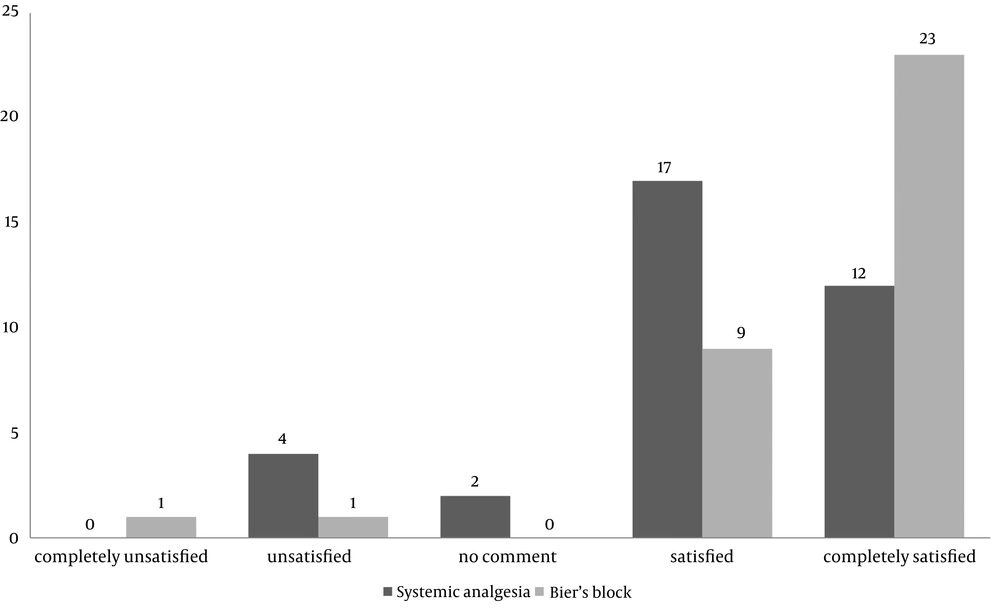
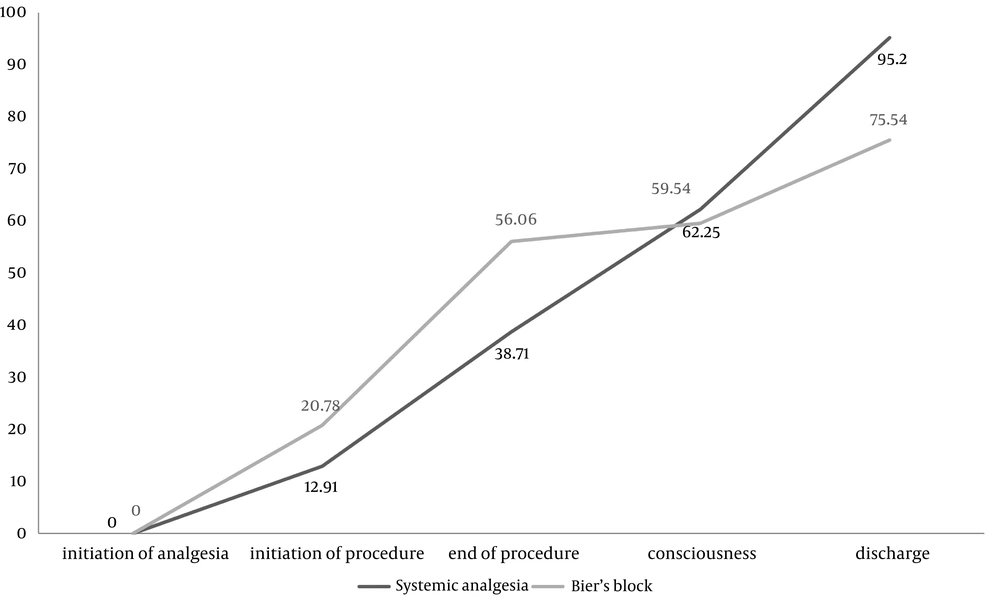
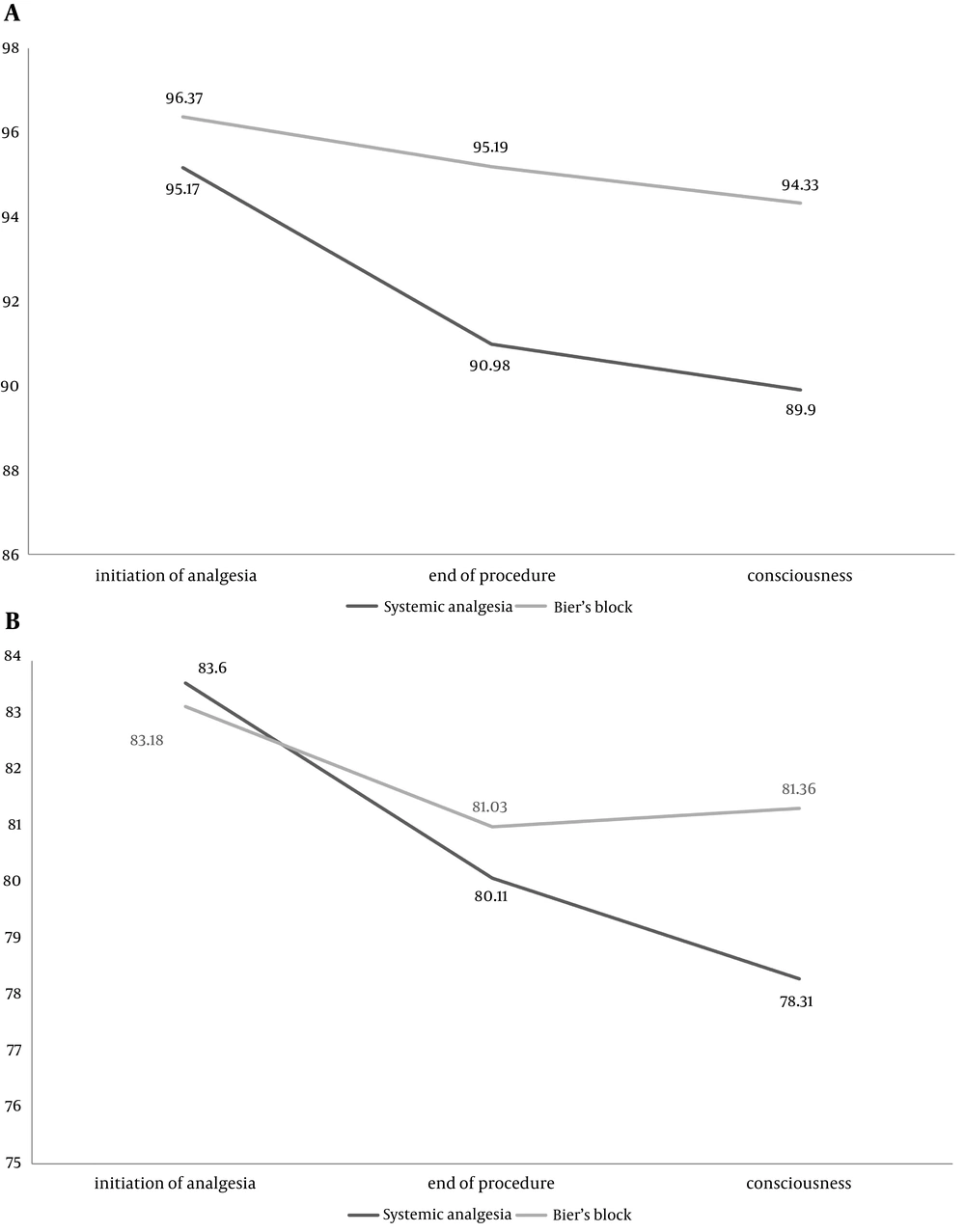
Of the 82 patients assessed for eligibility, 13 patients were excluded and 69 patients took part in the study (Figure 1). Data regarding age, sex, type and site of injury in each group is summarized in Table 1. There were no statistically significant differences between the two groups in baseline characteristics. Pain intensity according to the NRS for each group before and after introduction of analgesia and level of decrease in each group are described in Table 2. There were no differences between the two groups in baseline pain intensity, but pain intensity after induction of analgesia was significantly lower and level of decrease in pain was significantly higher in Bier’s block group. Satisfaction of surgeon, patient and physician responsible for analgesia was assessed using the five-point Likert scale (from completely satisfied to completely unsatisfied) (Figure 2 and 3). There were no statistically differences between the two groups regarding surgeons’ satisfaction (P = 0.35), but patients’ satisfaction (P = 0.1) and physicians responsible for analgesia satisfaction (P = 0.05) was significantly higher in Bier’s block group. The total number of patients with complications was not significantly different between the two groups. Table 3 describes the frequency of various complications in each group. There was no significant difference between total numbers of patients with complications in the two groups (P = 0.35). Analysis of time taken at different stages of the whole operation in each group showed that applying Bier’s block took a longer duration than applying systemic analgesia; however, the whole operation duration was significantly less in Bier’s block group (general linear model P-value < 0.01). Figure 4 shows time spent at different stages in each group. Mean arterial pressure and pulse rate declined during the operation in both groups. Decline in both these variables was significantly more in the systemic analgesia group (general linear model P-value for both variables < 0.01). Figure 5 shows changes in mean arterial pressure and pulse rate in both groups during the operation.
| Total Cases | Systemic Analgesia Group | Bier’s Block Group | P-value | |
|---|---|---|---|---|
| Number | 69 | 35 | 34 | |
| Age, y | 42.57 ± 17.68 | 42.77 ± 17.37 | 42.38 ± 18.25 | 0.92 a |
| Gender | 0.93b | |||
| Male | 47 | 24 | 23 | |
| Female | 22 | 11 | 11 | |
| Type of injury | 0.70b | |||
| Laceration | 14 | 5 | 9 | |
| Fracture | 35 | 20 | 15 | |
| Dislocation | 6 | 2 | 4 | |
| Tendon injury | 9 | 5 | 4 | |
| Foreign body | 3 | 2 | 1 | |
| Fracture-dislocation | 2 | 1 | 1 | |
| Site of injury | 0.96b | |||
| Fingers | 3 | 1 | 2 | |
| Hand | 11 | 6 | 5 | |
| Wrist | 9 | 4 | 5 | |
| Forearm | 34 | 17 | 17 | |
| Elbow | 9 | 5 | 4 | |
| Arm | 3 | 2 | 1 |
a T-test.
b Chi-square test.
a Numerical Rating Scale.
b T-test.
c P Value was less than 0.1 which is considered statistically significant.
| Bier’s Block Group, No. (%) | Systemic Analgesia Group, No. (%) | |
|---|---|---|
| Nausea | 2 (5.88) | 11 (31.43) |
| Vomiting | 1 (2.94) | 9 (25.71) |
| Change in analgesia method with surgeon's request | 1 (2.94) | 0 (0) |
| Change in method of analgesia with patient's request | 1 (2.94) | 0 (0) |
| Seizure | 3 (8.82) | 0 (0) |
| Pain in tourniquet site | 6 (17.65) | 0 (0) |
| Hypoxia | 0 (0) | 4 (11.43) |
| Total number of patients with complications | 13 (38.24) | 16 (45.71) |
| Total number of patients | 34 (100) | 35 (100) |
5. Discussion
In this non-blinded randomized clinical trial we aimed to compare pain reducing ability, satisfaction of surgeon, patient and physician responsible for analgesia for two methods of analgesia, including Bier’s block and systemic analgesia. We also compared complications, duration and hemodynamic changes between these two methods. Since age, gender ratio, site and type of injury were not significantly different between the two groups, we can claim that bias resulting from dissimilarity between these characteristics was minimal in our study. Patients who underwent Bier’s block showed a greater decrease in their score of pain than systemic analgesia. Physicians responsible for analgesia were more satisfied with Bier’s block than systemic analgesia; however this difference did not exist in surgeons and patients. Total number of appeared complications did not differ significantly between the two groups. Except for one case of seizure in Bier’s block group and four cases of hypoxia in the systemic analgesia group, other complications were not life threatening. These five complications were managed successfully in our study and did not result in termination of operation or change in method of analgesia. Decreased incidence of post-operative nausea and vomiting was one of the mentioned advantages of regional anesthesia over general analgesia in previous studies (5, 11). This fact was emphasized in our study as well as previous studies. Our results show that time spent for applying Bier’s block itself is more than the time taken for introduction of systemic analgesia, however whole duration of operation was shorter in the Bier’s block group. This fact can be explained by the time taken for other steps of operation in systemic analgesia such as time for regaining consciousness. Shorter hospital stay is one of advantages of Bier’s block over systemic analgesia that has been proved by previous studies (6). Both pulse rate and mean arterial pressure showed a significant drop during the operation in both groups, but this drop was more significant in the systemic analgesia group. This data can indicate that patients who undergo systemic analgesia are more prone to significant instability in their hemodynamic status.
5.1. Limitations
This study has various limitations. Due to the limited resources we applied type I error of 10% for this study, which decreased the number of patients enrolled and increased probability of false positive results. As the nature of Bier’s block and systemic analgesia were different, we were unable to blind patient, surgeon or physician responsible for analgesia, which could result in biases. In conclusion, since Bier’s block showed more analgesic effects, it resulted greater satisfaction for the physician responsible for analgesia, took less time and caused less hemodynamic instability in our study. Furthermore, regarding lack of significant differences in satisfaction of surgeons and profile of complications between the two groups, it seems that choosing Bier’s block can be more favorable to systemic analgesia in procedural sedation for upper extremity procedures in the ED.