1. Background
Stress fractures are divided into insufficiency fractures, which occur due to normal stress onto an abnormally weakened bone and fatigue fractures, which are a result of repetitive stress on a normal healthy bone. Insufficiency fractures are beyond the scope of this article and hence won’t be discussed further, here onwards fatigue fractures will be referred to as stress fractures in this article (1). Stress fractures usually present with insidious pain, which occurs at the end of physical activity and aggravated during activity and daily routine activities. A change in pattern of exercise is usual history and on examination local tenderness and/or swelling are usually present
Stress fractures are common in military recruits due to repetitive stress on the same bone without adequate recovery time, however they are difficult to diagnose because of the most commonly used screening modality, i.e. the plain radiograph cannot detect stress fractures for approximately up to 06 weeks, a period which may extend up to 10 weeks (2, 3). On the other hand MRI is the most comprehensive method to assess potential stress fracture because of high level of both sensitivity (86% - 100%) and specificity (100%). However, it is not easily available in remote areas. Thus, there is need for an imaging modality, which is sensitive and specific as well as easily accessible for detecting stress fractures in recruits. It is a non-invasive method and simple to perform (4). In a pilot case-control study of 37 patients with metatarsalgia and normal radiographs, USG had a sensitivity of 83% and specificity of 76% compared to MRI in picking up metatarsal stress fractures (5). We hypothesize that USG may also act as an effective method for screening of stress fractures in other bones such as tibia.
Stress fractures are sub classified into low risk and high risk varieties (6), the low risk fractures usually respond to rest and heal themselves over a period of time, however, the high risk fractures may proceed to complete fractures or even to non-union /mal-union, hence the need for an early diagnosis to prevent these complications.
2. Objectives
We propose the use of diagnostic ultrasound as a tool for early detection of stress fractures.
3. Methods
3.1. Study Design
3.2. Hospital Based Prospective Study
We performed a diagnostic ultrasound in young recruits presented to us with new onset lower limb pain in the period of 26 months from April 2014 to Jun 2016 after sustained physical activity irrespective of the fact whether the plain radiographs done on them were normal or suspicious of stress fractures. All patients were then subjected to a MRI examination to confirm or negate our findings.
Written informed consent was obtained from all patients included in study.
In each case, a sonography was performed using a GE Logiq P5 ultrasound machine. A 3-10 MHz linear array transducer was used with a frequency between the range of 6 MHz and 9 MHz. All subjects gave permission to perform the test on them.
A radiologist with 12 years of experience in the US performed the examination with a linear transducer of 3.5 to 10.5 MHz frequency using appropriate gain settings. The axial and longitudinal grey-scale were obtained on tibiae, concentrating on the point of maximum tenderness with the patient in supine position and the knees slightly flexed.
USG findings: We concentrated on 3 ultrasound findings and the presence of any 2 of these findings was taken as a positive indication of presence of a stress fracture.
1) Periosteal elevation/Subperiosteal hematoma
2) Cortical thickening at the point of maximum tenderness
3) Break in continuity/step defect of the echogenic cortex
All MRI studies were done using 1.5-T system (Magnetom Avanto; Siemens, AG, Germany).
The MR imaging protocol followed was as follows:
(A) Axial T1-weighted SE sequence (TR-400-800; TE-minimal: slice thickness-4/1 mm; FOV-26; image matrix-256 × 190),
(B) Axial T2-weighted fast SE sequence (TR-> 1500; TE ~ 70 - 80; slice thickness-4/1 mm; image matrix, 256 × 256; Echo train length-8)
(C) Coronal T1-weighted SE sequence (TR-400-800; TE-minimal: slice thickness-4/1 mm; FOV-40; image matrix-256 × 190),
(D) Coronal T2-weighted FSE sequence (TR-> 1500; TE ~ 70 - 80; slice thickness-4/1 mm; image matrix, 256 × 256; Echo train length-8) and
(E) Sagittal STIR sequence (TR-> 2000; TE-20-40; TI-150; slice thickness-4/1 mm; FOV-26; image matrix-256 × 190; Echo train length-8).
MRI findings: the MRI findings were classified according to the Fredericson classification for medial tibial stress syndrome on MRI. This is an accurate method of correlating bony involvement with presenting symptoms of patients.
Fredericson classification for tibial stress fractures (7)
- Grade 1: Periosteal edema only
- Grade 2: Edema in bone marrow visible on T2WI
- Grade 3: Edema in bone marrow visible on both T1WI and T2WI
- Grade 4: Signal abnormality in cortex
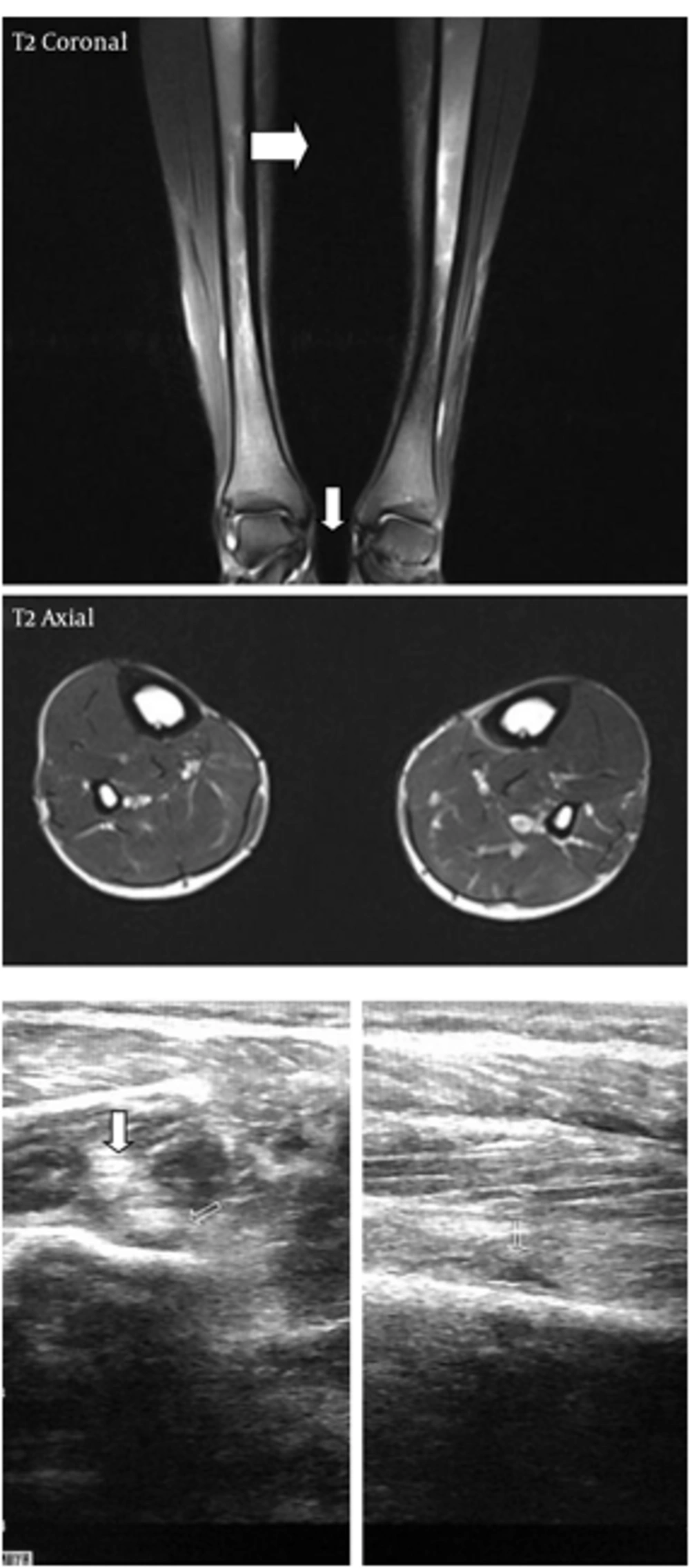
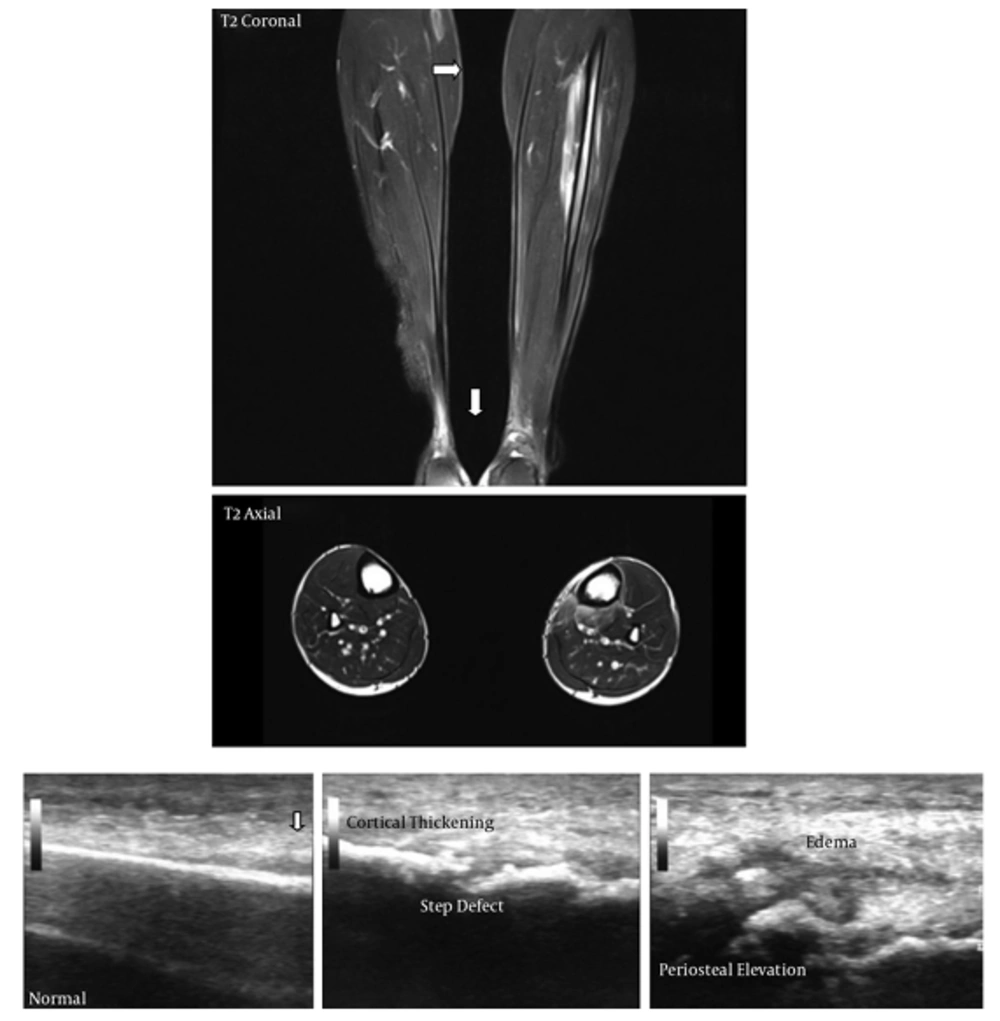
All findings and measurements by both USG and MRI are reliable. All imaging studies were performed and evaluated by experienced radiologists (Figures 1 and 2).
3.3. Inclusion Criteria
All patients with new onset lower limb pain with local point tenderness in the tibia
3.4. Exclusion Criteria
Patients with frank fractures on plain radiographs
Patients with more than 4 weeks of symptom onset
3.5. Patients with Metallic Implants
Patients with claustrophobia who could not be subjected to an MRI examination
4. Results
Out of the 64 patients studied, 49 patients had no evidence of stress fracture on plain radiographs, 20 patients had positive indication of stress fracture on USG, and 32 patients had some evidence of stress fracture on diagnostic ultrasound but not fulfilling criteria.
43 patients had stress injury on MRI. Out of these 43 patients, 15 patients had a positive indication of a stress fracture on USG with more than 2 features fulfilling the criteria and on the MRI they mostly had a grade III/IV injury, except 2 patients who showed grade II injury; only 6 out of 43 had normal USG findings and 22 had at least grade I/II stress injury with USG findings that did not fulfill the criteria.
Out of the 22 patients with positive USG findings, 5 patients had a normal MRI.
All these findings have been elaborated in Table 1.
| S.No | Age | Sex | Xray | USG Findings | MRI Findings | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Periosteal Changes | Cortical Thickening | Cortical Breach | Increased Flow | Gr I | Gr II | Gr III | Gr IV | ||||
| 1 | 19 | M | + | + | + | + | |||||
| 2 | 20 | M | Normal | + | + | ||||||
| 3 | 18 | M | Normal | + | + | + | + | ||||
| 4 | 17 | M | Normal | + | + | ||||||
| 5 | 21 | M | Normal | + | |||||||
| 6 | 20 | M | Normal | + | + | ||||||
| 7 | 18 | M | Normal | + | + | ||||||
| 8 | 22 | M | + | + | + | + | |||||
| 9 | 19 | M | Normal | + | + | ||||||
| 10 | 18 | M | Normal | + | + | ||||||
| 11 | 17 | M | + | ||||||||
| 12 | 20 | M | + | + | |||||||
| 13 | 21 | M | + | + | + | + | + | ||||
| 14 | 22 | M | Normal | + | + | + | |||||
| 15 | 18 | M | Normal | + | + | ||||||
| 16 | 19 | M | Normal | + | + | ||||||
| 17 | 21 | M | Normal | + | |||||||
| 18 | 21 | M | Normal | + | + | ||||||
| 19 | 20 | M | Normal | + | + | ||||||
| 20 | 19 | M | Normal | + | + | ||||||
| 21 | 17 | M | Normal | + | + | ||||||
| 22 | 18 | M | Normal | + | + | + | |||||
| 23 | 19 | M | Normal | + | + | ||||||
| 24 | 20 | M | Normal | + | + | + | + | ||||
| 25 | 18 | M | Normal | ||||||||
| 26 | 17 | M | + | + | + | + | |||||
| 27 | 21 | M | Normal | + | |||||||
| 28 | 20 | M | Normal | + | |||||||
| 29 | 18 | M | Normal | + | + | ||||||
| 30 | 22 | M | Normal | ||||||||
| 31 | 19 | M | Normal | + | |||||||
| 32 | 18 | M | Normal | + | |||||||
| 33 | 17 | M | Normal | + | + | ||||||
| 34 | 20 | M | Normal | ||||||||
| 35 | 21 | M | Normal | + | + | ||||||
| 36 | 22 | M | + | + | |||||||
| 37 | 18 | M | Normal | + | + | + | + | ||||
| 38 | 19 | M | Normal | + | |||||||
| 39 | 22 | M | Normal | + | + | ||||||
| 40 | 21 | M | + | + | + | + | |||||
| 41 | 20 | M | Normal | + | |||||||
| 42 | 19 | M | Normal | + | + | ||||||
| 43 | 17 | M | Normal | ||||||||
| 44 | 18 | M | Normal | + | + | ||||||
| 45 | 20 | M | Normal | ||||||||
| 46 | 21 | M | Normal | + | + | + | + | ||||
| 47 | 22 | M | Normal | + | + | ||||||
| 48 | 18 | M | Normal | + | |||||||
| 49 | 19 | M | Normal | + | |||||||
| 50 | 21 | M | + | + | + | + | |||||
| 51 | 21 | M | Normal | + | |||||||
| 52 | 20 | M | Normal | + | + | ||||||
| 53 | 19 | M | + | ||||||||
| 54 | 17 | M | |||||||||
| 55 | 18 | M | + | + | + | + | |||||
| 56 | 20 | M | + | ||||||||
| 57 | 21 | M | Normal | + | + | ||||||
| 58 | 20 | M | + | ||||||||
| 59 | 18 | M | Normal | ||||||||
| 60 | 22 | M | Normal | + | + | ||||||
| 61 | 19 | M | + | + | + | + | |||||
| 62 | 18 | M | + | + | |||||||
| 63 | 17 | M | Normal | + | + | ||||||
| 64 | 20 | M | + | + | + | + | |||||
| 65 | 21 | M | Normal | + | + |
All observations were subjected to a biostatistical analysis using the conventional 2 × 2 table analysis method for assessing the sensitivity and specificity of USG against MRI, which is the best modality for detecting stress fractures. In comparison with MRI, in our study, the overall sensitivity of USG in detecting the stress fracture was found to be 86.05% with a specificity of about 77.27%. With a positive predictive value of 88.10% and a negative predictive value of 73.91%, USG is a highly accurate and sensitive modality for detection of stress fractures in patients (Table 2).
| USG Results | Stress # | ||
|---|---|---|---|
| +ve | -ve | Total | |
| +ve | 37 | 05 | 42 |
| -ve | 06 | 17 | 23 |
| Total | 43 | 22 | 65 |
Sensitivity = 37/43 × 100 = 86.05%
Specificity = 17/22 × 100 = 77.27%
Positive predictive value = 37/42 × 100 = 88.10%
Negative predictive value = 17/23 × 100 = 73.91%
False-ve = 06/43 × 100 = 13.95%
False +ve = 05/22 × 100 = 22.72%
On the contrary, sensitivity of radiographs in detecting stress fractures is very low (approximately 37.02%). However, it has a high specificity of 95.45% with a positive predictive value of 95.11%. (Table 3) Therefore, if features of stress fracture are detected on radiograph, it is highly likely that the same will be confirmed by a MRI.
| X-Ray Results | Stress # | Total | |
|---|---|---|---|
| +ve | -ve | ||
| +ve | 16 | 01 | 17 |
| -ve | 27 | 21 | 48 |
| Total | 43 | 22 | 65 |
Sensitivity = 16/43 × 100 = 37.02%
Specificity = 21/22 × 100 = 95.45%
Positive predictive value = 16/17 × 100 = 95.11%
Positive predictive value = 21/48 × 100 = 43.75%
False –ve = 26/43 × 100 = 60.46%
False +ve = 01/22 × 100 = 04.54%
5. Discussion
Stress fractures are difficult to diagnose clinically because of a significant overlap of symptoms with many musculoskeletal injuries, which may be significantly less severe and also due to underreporting of symptoms by the affected patients themselves leads to delayed diagnosis of stress fractures (1).
Though the precise mechanism of stress fracture is not completely understood, in case of young recruits, it is proposed that recurrent stress without adequate periods of rest, stimulate the remodeling process, increasing osteoclastic resorption and causing bone weakness due to imbalance in process of healing. Muscle weakness causes loss of the buffering action of the muscle and the entire stress is borne by the bone itself. If the causative agent is not removed, micro damages accumulate with resultant stress fracture (1).
Stress fractures are common in our setting, which caters for young patients from various arms of the military, as plain radiographs are more often than not, not informative enough and the modality of choice MRI (8-12) cannot be used as a screening tool because of the cost and time involved and also because of absence of availability in the developing world. An MRI for every suspected stress fracture would not be possible or practical or cost effective.
In the past, bone scintigraphy was used as a gold standard for detection of stress fractures (12, 13), however, multiple studies have now shown that because of high rate of false negative examinations (14-17) and even as tumors and infections mimic stress fractures on bone scans, MRI is now the method of choice for imaging of stress fractures (18).
Therapeutic ultrasound has been propagated as a tool for detecting an early stress fracture but due to limitations such as very low latitude in pain production and problems in reproducibility as well as high operator dependence, it has not gained wide acceptance (19, 20).
There have been infrequent reports (21, 22) of use of diagnostic ultrasound for diagnosis of stress fractures in literature; however, it still hasn’t acquired a widespread acceptance and no large scale validation studies were encountered by the authors to the best of their knowledge. Few case studies in literature purport the use of ultrasonography to detect subperiosteal and periosteal changes and bony injuries. In a recent series of 5 metatarsal stress fractures, Bodner found other sonographic features, as in our case: small fluid collection, soft tissue oedema, and colour Doppler sonography rich vascularity surrounding the fracture area (23). In a pilot case-control study of 37 patients with metatarsal pain and normal radiographs, ultrasonography had a sensitivity of 83% and specificity of 76% compared with MRI in detecting metatarsal stress fractures (5).
Diagnostic ultrasound enjoys a higher sensitivity and specificity (6, 24), when compared to plain radiographs, is easily available, cheap, and reproducible. With adequate training it can be standardized, thus doing away with the problem of operator dependence.
Stress fracture presents pathologically as either a break in bony contour, periosteal reaction or subperiosteal hematoma (25). Bone is an obstacle for an ultrasound and because of the difference in impedance between the bone and adjacent soft tissue, the bony surface presents as a strong echogenic line and hence allows the sonologist to view even small imperfections in contour. Thereby allowing early detection of steps/breaks in bony contour as well as presence of subperiosteal hematoma and the entire gamut of findings required to diagnose an early stress fracture. In addition, use of color Doppler allows visualization of increased vascularity in the periosteal reaction signaling the acuteness of the fracture (25).
Early detection of stress fracture with this effective screening tool could lead to preservation of precious productive man-hours, by facilitating early return to work and also prevent complications from undiagnosed high risk fractures.