1. Background
Otitis media with effusion (OME) is a collection of fluid in the middle ear space without any acute inflammation symptoms. This disease is common in children at peak ages of two and five years. Furthermore, 80% of children have had at least one episode of OME before the age of ten. By the age of 7 - 8, about eight percent of children have serious fluid accumulation in the middle ear, with an increase in winter. The serous fluid remains in the middle ear for 6 to 10 weeks. However, in some cases, it may remain more than 3 months, which is called middle ear infection with chronic effusion (COME) (1).
Untreated COME leads to hearing loss, eardrum rupture, adhesive otitis media, tympanosclerosis, temporal bone necrosis, and cholesteatoma. As a result of hearing loss, which is a prominent manifestation of ear infection, the patient may have language, speech, and cognitive development disorders and experience academic failure (2).
Eustachian tube dysfunction is generally considered to be an important factor in the pathogenesis of otitis media, and hypoventilation of the middle ear and serous fluid or mucoid accumulation is the main clinical-pathologic factor in this disease. Eustachian tube dysfunction causes air pressure and fluid build-up in the middle ear and prevents middle ear cleaning and protection; therefore, microorganisms enter the middle ear. In 91% of patients, the causative bacteria are those colonized in the nasopharynx and adenoid is a reservoir of pathogenic bacteria. Enlarged adenoids can also cause Eustachian dysfunction and otitis media (3, 4).
Ventilation tube is one of the best middle ear effusion (chronic serous otitis) treatments (5). In addition to chronic inflammation of the middle ear along with fluid accumulation, myringotomy surgery and ventilation tube insertion are needed in cases of recurrent acute middle ear infection and severe retraction and atelectasis of the tympanic membrane (6).
Ear ventilation tubes (or vent tube) are very small tubes that are placed in the eardrum and allow air to enter the middle ear. They are also called tympanostomy tubes, ventilation tubes or pressure equalization tubes. There are two basic types of ear tubes: short-term and long-term. Short-term tubes are smaller and typically stay in place for six months to a year before falling out on their own (7).
Some benefits of ventilation tube insertion include reduction of future ear infections risks, treatment of hearing loss due to middle ear fluid, improvement of speech and balance problems, and improvement of chronic ear infections, which may cause sleeping problems (8).
While the VT insertion surgery can be considered a simple procedure with significant benefits, it can also have adverse effects. Reports show several adverse effects of VT insertion on the tympanic membrane. Some VT insertion surgical complications include otorrhea, tympanosclerosis, eardrum rupture, eardrum stretching, and cholesteatoma. In many cases, it is difficult to distinguish the complications of the disease from the complications that resulted from the treatment (9).
Otorrhea is the most common complication of ventilation tube, which can occur in 3% to 50% of cases (10). Two out of every three children with VT develop otorrhea every year (11). There is no significant evidence that precautions, when exposed to water, can prevent this disease. Otorrhea is related to nasal discharge during an upper respiratory infection. Nasal discharge results from the incompatibility of Eustachian tubes or reaches the middle ear through the external ear canal (12).
Tympanosclerosis is a condition caused by hyalinization and subsequent calcification in the collagen layer of the tympanic membrane, which mostly occurs in patients who underwent VT insertion surgery. Ear injury (trauma), as one of the important factors of tympanosclerosis, is commonly associated with myringotomy and VT insertion. Bleeding inside the eardrum is another pathogenesis of tympanosclerosis. In a meta-analysis performed by Kai et al., the incidence of this complication has been reported to be 32% VT insertion may cause tympanic membrane atrophy. Permanent eardrum rapture is another adverse complication of VT insertion (12, 13).
Bingham et al. suggested that eardrum rupture should be diagnosed as a permanent complication if it persisted for one year (14). Wilson also suggested that the rupture of the secondary tympanic membrane caused by VT insertion may be due to the growth of squamous epithelium on the lower surface of the tympanic membrane (15). Barati et al. (14) and Kamrani et al. (4) observed complications of VT insertion in their study.
Patients with exacerbated ear infection symptoms, including earache and symptoms of upper respiratory tract infections, hearing loss, or symptoms of upper airway obstruction, referred to a specialist physician and were diagnosed to have VT surgery. While this is one of the most common children’s surgeries requiring general anesthesia, few studies have been done on its long-term complications (16).
2. Objectives
The purpose of this study was to evaluate the complications of VT insertion surgery in children under the age of 10 in the Kamkar Hospital of Qom from 2017 to 2019.
3. Methods
This historical cohort study was carried out on 205 children under the age of 10 who underwent VT insertion surgery in Kamkar Hospital from 2017 to 2019. Demographic questionnaire (including age, sex, family medical history, reasons for surgery, date of surgery) and patient medical records (complications and symptoms) were used for data collection. The inclusion criteria were age (under 10 years old), having serous otitis media, having VT insertion surgery and complete medical records. The exclusion criteria were concurrent diseases that affect the eardrum and having incomplete medical records. To obtain informed consent, the study population was informed about the subject and procedure of study and participants were invited for re-examination and interview. Subsequently, postoperative status and surgery side effects, including otitis media, tympanic membrane atrophy, tympanosclerosis, tympanic membrane perforation, and otorrhea data were recorded using an interview and examination. Descriptive statistics were used to describe the basic features of the data and independent t-test, Mann-Whitney U-test, Fisher’s exact, and chi-square test were used for analysis. Data were then entered into SPSS 18 software with a significance level of less than 0.05.
4. Results
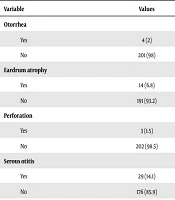
The results showed that a total of 205 children aged three to 10 years underwent VT insertion surgery in Kamkar Hospital from 2017 to 2019. Moreover, 117 children were boys (57%), and none had a family medical history (Table 1). In many cases, ventilation tube insertion was due to serous otitis with hypotrophy, resulting in 200 (97.6%) operations involving VT with adenoidectomy. The study of surgery complications showed that in 201 (98%) cases, VT insertion resulted in otorrhea. Tympanosclerosis, eardrum atrophy, and perforation cases due to VT insertion were 25 (14.1%), 14 (6.8%), and 3 (1.5%), respectively. Also, serous otitis recurrence was observed in 29 cases (14.1%). Embedded VT was observed and reported in 27 (13.2%) of the examinations. There were also 8 (3.9%) cases of infections and recurrences with T-tube insertion (Table 2).
| Variable | Values |
|---|---|
| Sex | |
| Male | 117 (57.1) |
| Female | 88 (42.9) |
| Date of surgery | |
| 2017 | 127 (62) |
| 2018 | 54 (26.3) |
| 2019 | 24 (11.7) |
| Family medical history | |
| Yes | 0 (0) |
| No | 205 (100) |
aValues are expressed as No. (%).
| Variable | Values |
|---|---|
| Otorrhea | |
| Yes | 4 (2) |
| No | 201 (98) |
| Eardrum atrophy | |
| Yes | 14 (6.8) |
| No | 191 (93.2) |
| Perforation | |
| Yes | 3 (1.5) |
| No | 202 (98.5) |
| Serous otitis | |
| Yes | 29 (14.1) |
| No | 176 (85.9) |
| Adenoidectomy | |
| Yes | 200 (97.6) |
| No | 5 (2.4) |
| Tympanosclerosis | |
| Yes | 25 (12.2) |
| No | 180 (87.8) |
| Observing VT during the examination | |
| Yes | 27 (13.2) |
| No | 178 (86.8) |
| T-tube insertion | |
| Yes | 8 (3.9) |
| No | 198 (96.1) |
| Surgery | |
| Serous otitis with tonsillar hypertrophy | 200 (97.6) |
| Serous otitis without tonsillar hypertrophy | 5 (2.4) |
aValues are expressed as No. (%).
Initially, two groups of boys and girls were compared in terms of how long ago surgery was performed. Since time distribution was not normal in these two groups, Mann-Whitney U-test was used for comparison, which showed no significant difference between the two groups in terms of elapsed time after surgery (P value = 0.84) (Table 3). The comparison of the age of the patients who underwent surgery showed a difference between the two groups where the mean age of the girls was significantly higher than that of the boys. The girls in the sample seemed to need surgery at an average age of 6.7 years, which was one year later than the boys (Table 4).
| Sex | Number | Mean, mo | Mean Rank | Sum of Rank | Mann-Whitney U | P Value |
|---|---|---|---|---|---|---|
| Boy | 117 | 26.78 | 103.7 | 12133 | 5066 | 0.84 |
| Girl | 88 | 26.82 | 102.07 | 8982 | ||
| Total | 205 | - | - | - | - | - |
| Sex | Number | Mean, mo | Mean Rank | Sum of Rank | Mann-Whitney U | P Value |
|---|---|---|---|---|---|---|
| Boy | 117 | 5.6 | 89.53 | 10475 | 3572 | 0.001 |
| Girl | 88 | 6.7 | 120.91 | 10640 | ||
| Total | 205 |
The results also showed that boys were more at risk of getting serious otitis, but no significant difference was observed between boys and girls (P value > 0.05). In the case of tympanosclerosis, girls were more at risk. In cases of eardrum atrophy, VT observation, and T-tube there was no significant difference between boys and girls (P value > 0.05). In the case of T-tube, one of the cells in the table had a frequency of less than 5, so Fisher’s exact test was used. Based on Fisher’s exact test there was no significant difference in the frequency of two sexes and values were mostly close to each other (P value > 0.05) (Table 5).
| Type of Complication | Status | Values | Chi-Square | df | P Value | |
|---|---|---|---|---|---|---|
| Boy | Girl | |||||
| Tympanosclerosis | Yes | 11 (9.4) | 15 (15.9) | 1.986 | 1 | 0.16 |
| No | 106 (90.6) | 74 (84.1) | ||||
| Eardrum atrophy | Yes | 8 (6.8) | 6 (6.8) | 0 | 1 | 0.99 |
| No | 109 (93.2) | 82 (93.2) | ||||
| Serous otitis | Yes | 19 (16.2) | 10 (11.4) | 0.983 | 1 | 0.32 |
| No | 98 (83.8) | 78 (88.6) | ||||
| Observing VT during the examination | Yes | 15 (12.8) | 12 (13.6) | 0.029 | 1 | 0.86 |
| No | 102 (87.2) | 88 (86.4) | ||||
| T-tube | Yes | 6 (5.1) | 2 (2.3) | - | - | 0.47b |
| No | 111 (94.9) | 86 (97.7) | ||||
aValues are expressed as No. (%).
bFisher’s exact test.
5. Discussion
This study was carried out on 205 children under the age of 10 who underwent VT insertion surgery in Kamkar Hospital from 2017 to 2019. As studies show, there were 127 (62%) surgeries in 2017, 54 (26.3%) surgeries in 2018, and 24 (11.7%) surgeries in 2019. Moreover, 117 surgeries (approximately 57%) were performed on boys and the rest were performed on girls, which is inconsistent with the study by Khalili et al. (17) and Karimi et al. (18). Some studies have shown that complications of VT insertion are higher in females; however, this issue was not proven in our study, which can be due to the non-normal distribution of gender variables in the patients under study. Also, no positive family history was recorded for any of the children in this study.
In this study, more surgical complications, including otorrhea, eardrum atrophy, perforation, serous otitis, and tympanosclerosis were observed, which was consistent with similar studies (10, 14, 18-20). In fact, these results indicate the need to look after children to prevent such complications. According to the analysis, there was no significant relationship between the two groups of boys and girls in terms of elapsed time after the surgery and insertion of VT in different years, which was inconsistent with similar studies (20). The reason for this disagreement could be different study locations and different disease distribution in these two studies. Studying the relationship between age and time of surgery showed a significant difference where the mean age of girls was significantly higher, and the girls needed surgery later than the boys. These results were consistent with similar studies (18).
This study showed girls experience tympanosclerosis complications more than boys, but there was no significant difference between the two groups. These results were in agreement with the study of Barati et al. (14) and Klopp-Dutote et al. (21). But not consistent with the study by Hassmann-Poznanska et al. (22). and Yaman et al. (23). This inconsistency may be due to the geographical location of the study. Also, 6.8% of children found to have eardrum atrophy after VT insertion surgery that was consistent with the studies of Banan et al. (20) and Zielnik-Jurkiewicz et al. (24). Moreover, the incidence rate was the same in both groups. There was no difference in the incidence to show a reduction of eardrum atrophy after VT insertion surgery.
Serous otitis was 14.1%, although the results show boys are more at risk, there was no significant difference, which was consistent with Jelinek et al. study (24). In fact, one could argue that the longer the time elapsed after surgery, the more likely it is to have serious otitis. So, timing plays an important role in the probability of this complication. Less than 5% of boys and girls needed T-tube insertion, but there was no significant relationship between the two groups of boys and girls.
The limitations of this study included incomplete records, patients’ and parent’s refusal to cooperate, and coexisting infections and middle ear diseases. It is also suggested to conduct studies to identify the risk factors and their effects, the effects of VT insertion on hearing and quality of life, and long-term complications.
5.1. Conclusions
The findings of the current study show no significant difference in surgical complications between the two groups of boys and girls. The mean age of girls was significantly higher only in studying the relationship between the age of the patients and the time of need for surgery.