1. Background
Orbit is a pyramid of soft tissue that encompasses the eye. The orbital septum is a fascia layer that attaches to the orbital wall and tarsal plate in the upper and lower eyelids. The septal layer is a barrier between the soft tissue of its orbital surface structures, so the inflammation confined to the anterior septum is called preseptal cellulitis, and confined to the posterior septum is called orbital cellulitis.
Paranasal sinuses are the most common source of orbital cellulitis. The ethmoid sinus lies in the nasal and is separated from the inner wall of the orbit by only a thin wall called lamina papiryracea. There are four pairs of sinuses around the orbit: ethmoidal, frontal, maxillary, and sphenoid. The orbital floor forms the ceiling of the maxillary sinuses and the orbital ceil forms from the floor of the frontal sinuses. The maxillary sinuses and the ethmoid sinuses are formed in the embryo, the ethmoid sinuses progress well at birth, but the maxillary sinuses grow during the first 2 years of life but do not stop growing until 6 years of age. The sphenoid and frontal sinuses are formed in childhood and will be complete in adolescence. Therefore, orbital cellulitis secondary to sinusitis during the first five years of life is exclusively caused by ethmoid sinusitis, and orbital cellulitis caused by ethmoid, maxillary, and frontal sinuses occurs after the age of seven. The apertures of the sinuses are larger in size than in the early stages of pre-growth. When the size of the sinuses increases, the apertures remain the same as the previous one, thereby draining the weakness of the sinuses during sinus inflammation. Natural fissures may be present in the walls and ceiling of the orbit, which may spread the infection to the sinuses (1, 2).
The orbit is covered by bone, and this limits the spread of inflammation to the orbit. Blood vessels and sinus nerve pierce the walls and make a way to spread infections to the orbit. The middle veins of the face and the orbits surrounding are discharged through the orbit into the cavernous sinus, which allows the transmission of facial and dental infections to the orbit and the brain (1, 2).
Preseptal cellulitis and orbital cellulitis are serious infections of the tissues around the eye. Although they can be seen at any age, children are most likely to be affected (3), and if not properly treated, they can have ophthalmic complications such as vision loss, endophthalmitis, and life-threatening complications such as cavernous sinus thrombosis, meningitis, cerebritis, and brain abscesses (4).
Inflammation of the anterior orbital septum is called preseptal cellulitis, which erythema and eyelid edema are the main characteristics. Eyelid edema in children is so severe that it prevents eye examination, making it difficult to differentiate preseptal cellulitis from orbital cellulitis. Preseptal infections are not relatively common and potentially dangerous. preseptal cellulitis is at least 6 to 10 times more common than orbital cellulitis (1). Preseptal infection can occur up to 60% under 5 years and up to 85% under 20 years old.
Orbital cellulitis is an inflammatory disease related to the superficial and deep structures of the orbit. Its main features are edema and erythema of the eyelids, conjunctivitis, restriction of eye movement, and proptosis. Orbital cellulitis is much rarer than preseptal cellulitis, but has the potential for worse and more deadly complications. Orbital cellulitis is seen in all age groups but affects most children, with a prevalence of 1.6 per 100,000 in children versus 0.1 per 100,000 in adults (5). Orbital cellulitis in children is twice as common in boys than in girls, whereas in adults there is no difference in sex except in cases of methicillin-resistant Staphylococcus aureus causing it, which is 4 times more in females. The average age range of children hospitalized with orbital cellulitis is 7 - 12 years old (6).
Pre-orbital cellulitis is called inflammation around the orbital, which encompasses both preseptal cellulitis and orbital cellulitis. However, the term is also used instead of preseptal cellulitis. For this reason, it is recommended not to use this term because it is of two meanings (2).
One of the most common predisposing factors for preseptal cellulitis is the spread of bacterial and, in some cases, viral (7) infections from paranasal sinuses (68.8%). Other causes included conjunctivitis (9.7%), upper respiratory tract infections (6.5%), insect bites (5.4%), trauma (3.2%), inflammation of the lacrimal glands (2.2%), dental abscess (2.2%), foreign body, eyelids lesions (shalazion, cilia), skin infections (impetigo), and iatrogenic actions such as oral and eyelid manipulations are other susceptible causes of preseptal cellulitis (8, 9). The most common cause of orbital cellulitis is spreading infection from the paranasal sinuses (82.4%), especially ethmoid sinus. Other predisposing factors for orbital cellulitis include direct trauma-induced inoculation (5.9%), upper respiratory tract infections (5.9%), insect bites (5.9%), bacteremia-induced blood infection, and spread of soft tissue infection around the eye and adnexal (8, 9).
2. Objectives
In this study, common symptoms, that the patients were diagnosed with orbital and pre-orbital cellulitis and referred to the emergency room, and its therapeutic aspect, were evaluated and reported. The findings of this study may help early diagnosis of orbital and pre-orbital cellulitis before it can cause complications and reduce mortality and help the health system deal with paraclinical methods for diagnosis to select the best and cheapest method for early diagnosis of the disease.
3. Methods
This study was a retrospective descriptive study that evaluated the frequency of clinical and para-clinical symptoms and therapeutic aspects of children hospitalized with preseptal and orbital cellulitis diagnosed at Ali-Ibn-Abitaleb Hospital as a central hospital of Sistan and Baluchistan Province, Iran, from 2016 to 2018.
The target population in this study was all patients under 18 years admitted to Ali-Ibn-Abitaleb Hospital in Zahedan who were diagnosed with preseptal and orbital cellulitis using ICD-9 diagnostic codes. Following the principles of Helsinki and Trustees and after approval by the Ethics Committee of Zahedan University of Medical Sciences by ethic code of 8621, the medical records of individuals diagnosed with preseptal and orbital cellulitis during this period were extracted from Medical Records Section, and met the inclusion and exclusion (including Incomplete patient records and patients’ inaccessibility to collect information) criteria afterward. Information about each patient included demographic variables (age, sex, and place of residence), cause of preseptal cellulitis or orbital cellulitis (such as trauma, insect bites, ulcers, sinusitis, etc.), symptoms, treatment, and results recorded in checklists.
After collecting data, patients were divided into two groups: preseptal cellulitis and orbital cellulitis. They were clinically diagnosed with edema and/or erythema of the periorbital. Orbital cellulitis was considered if signs of orbital involvement (photophobia, proptosis, painful extraocular motion, ophthalmoplegia, visual impairment, or chemosis) appeared, and post septal involvement was confirmed by computed tomography (CT). To distinguishing between post-septal and preseptal cellulitis, the absence of signs of orbital involvement was considered the diagnosis of preseptal cellulitis. Finally, the data were analyzed with SPSS software using descriptive and inferential statistical tests, and a P-value of less than 0.05 was considered significant. Limitations of the present study consisted of patients’ record deficiencies, difficult access to patients’ radiographs, and the inability of the researchers to accurately examine patients and record important points in the checklists.
4. Results
In this study, we studied 40 patients admitted to the pediatric ward of Ali-Ibn-Abitaleb Hospital in Zahedan with a diagnosis of preseptal and orbital cellulitis by mean age of 2.85 ± 0.46 years. A total of 29 (72.5%) preseptal cellulitis and 11 (27.5%) orbital cellulitis were admitted. Moreover, 55% of the patients were male, and 45% were female. The prevalence of orbital and preseptal cellulitis was almost the same in males and females (Table 1) (P-value < 0.05).
| Female, No. (%) | Male, No. (%) | All, No. (%) | |
|---|---|---|---|
| Preseptal cellulitis | 13 (44.82) | 16 (55.17) | 22 (72.5) |
| Orbital cellulitis | 5 (45.45) | 6 (54.54) | 11 (27.5) |
| All | 18 (45) | 22 (55) | 40 (100) |
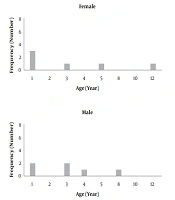
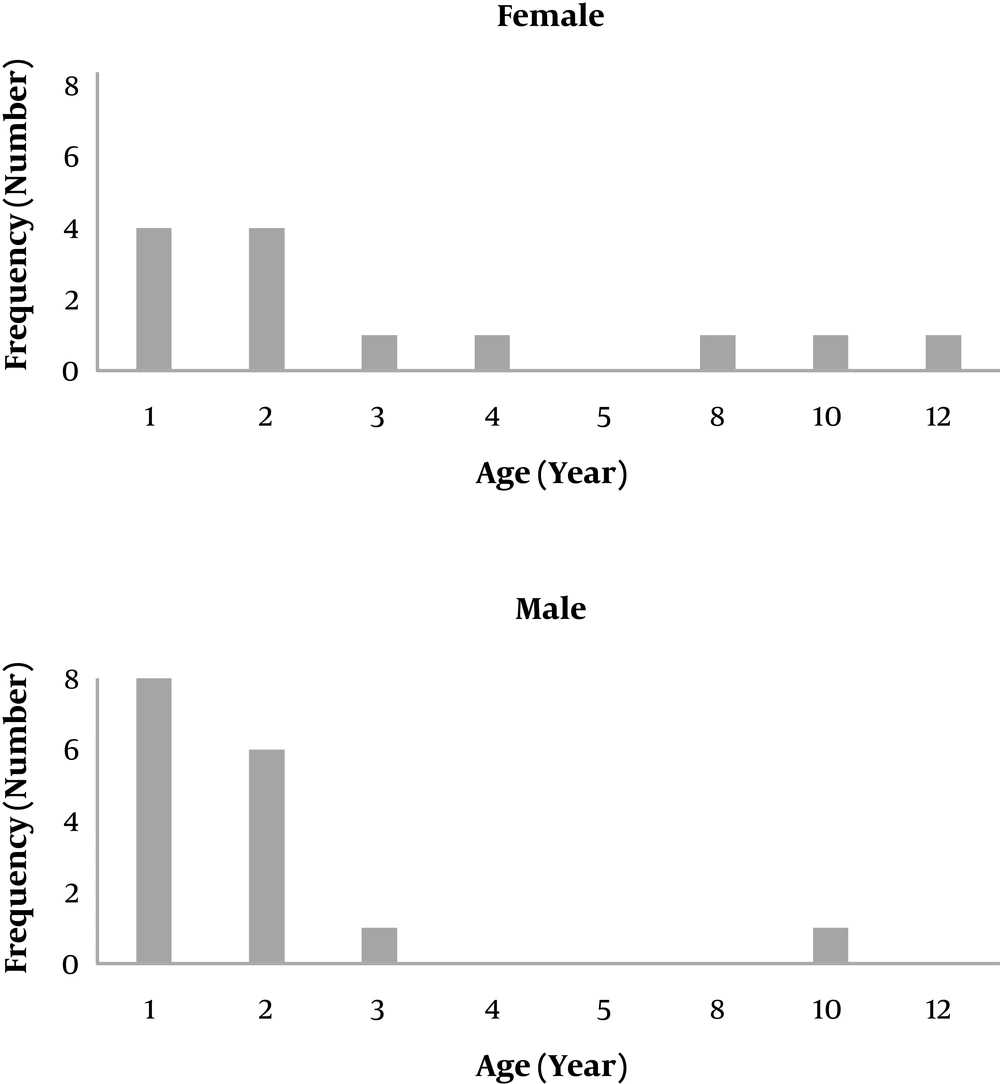
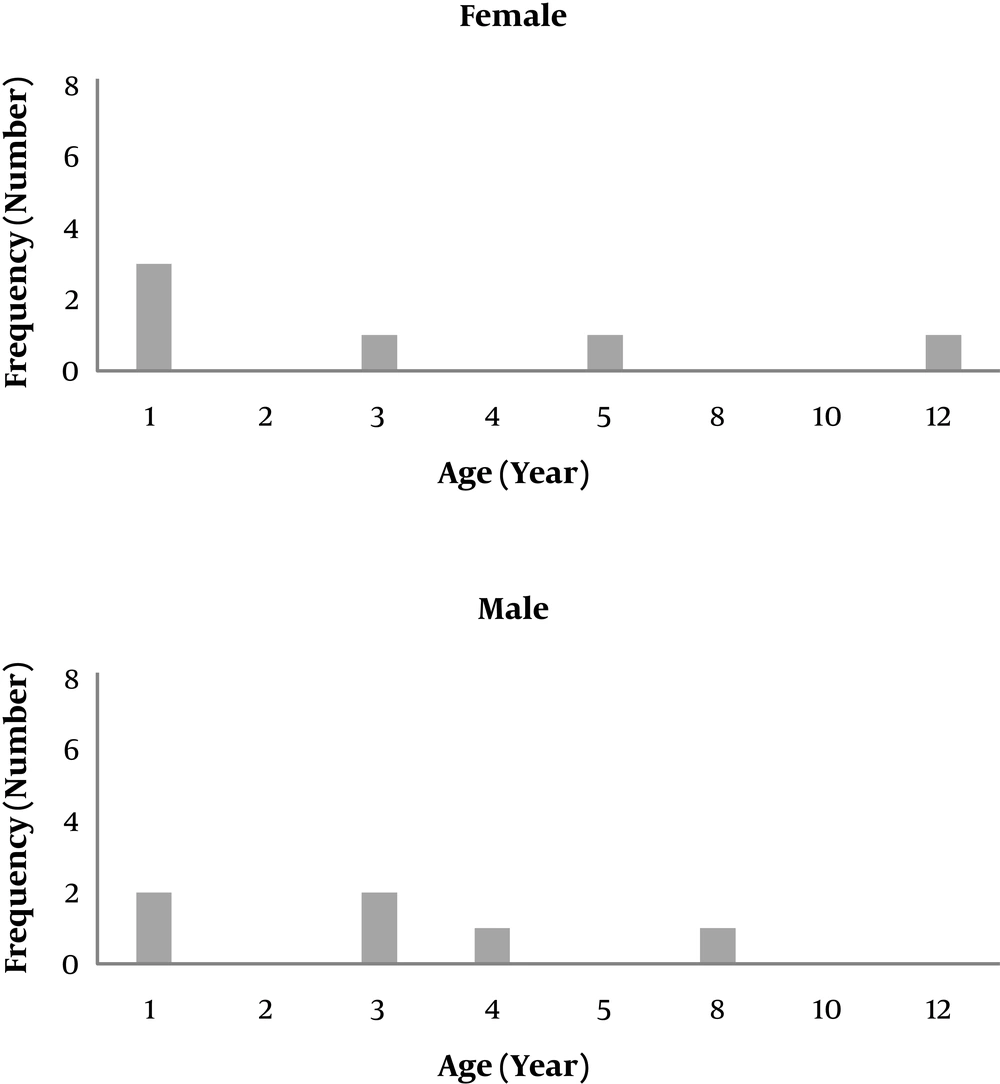
The mean age of the patients with preseptal cellulitis was 2.86 ± 0.59 years (mean ± SEM) with an age range of 12 days to 13 years, and in patients with orbital cellulitis was 2.82 ± 0.67 years (mean ± SEM) with an age range of two months up to eight years. The age distribution diagram of the patients overall had a skew to the left, which was more severe in patients with preseptal cellulitis (Figures 1 and 2).
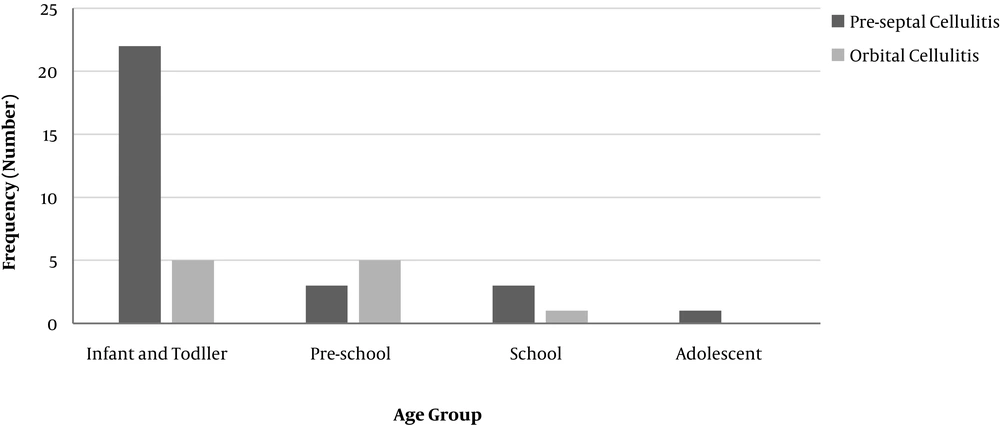
According to the age group, including infant, toddler (from birth to 2 years), pre-school (2 to 7 years), school (7 to 12 years), adolescence (12 to 18 years), the highest incidence of disease was in infancy and toddler, and the lowest incidence was in adolescence ages, and the prevalence of preseptal cellulitis was also higher at all stages except for pre-school (Figure 3) (P-value < 0.05).
According to the findings of the study, eyelid edema was the most common clinical finding in both groups of orbital and preseptal cellulitis. Extracellular paralysis and chemosis were not observed in any of the patients. Eye proptosis and movement restriction were reported in only two cases of orbital cellulitis. Reduced vision, eye pain, and fever were more common in orbital cellulitis patients, whereas erythema was more prevalent in patients with preseptal cellulitis (Table 2).
| Clinical Findings | Female, No. (%) | Male, No. (%) | All, No. (%) |
|---|---|---|---|
| Decreased vision | 20 (68.96) | 9 (81.81) | 29 (72.5) |
| Eye pain | 7 (24.13) | 5 (45.45) | 12 (30) |
| Eye redness | 27 (93.1) | 9 (81.81) | 36 (90) |
| Eye proptosis | 0 | 2 (18.18) | 2 (5) |
| Outer muscle paralysis | 0 | 0 | 0 |
| Chemosis | 0 | 0 | 0 |
| Eyelid edema | 28 (96.55) | 11 (100) | 39 (97.5) |
| Eye movements Restrictions | 0 | 2 (18.18) | 2 (5) |
| Fever | 24 (82.75) | 10 (90.90) | 34 (85) |
After evaluation of paraclinical findings in patients, leukocytosis and increased CRP in patients with preseptal cellulitis, and increased ESR in patients with orbital cellulitis were seen. Blood culture results were positive only in two patients, one was Staphylococcus aureus (orbital cellulitis), and the other was coagulase-negative staphs (preseptal cellulitis). Despite incomplete patients’ records, secret cultures were positive in four cases, all of which were preseptal cellulitis (Staph epidermidis, Streptococcus pneumonia, and two coagulase-negative staphs) (Table 3).
| Paraclinical Findings | Preseptal Cellulitis, No. (%) | Orbital Cellulitis, No. (%) | All, No. (%) |
|---|---|---|---|
| Leukocytosis | 25 (86.20) | 7 (63.63) | 32 (80) |
| ESR increasing | 25 (86.20) | 10 (90.90) | 35 (87.5) |
| CRP increasing | 12 (41.37) | 3 (27.27) | 15 (37.5) |
| Positive Blood culture | 1 (3.44) | 1 (9.09) | 2 (5) |
| Positive secrete culture | 4 (13.79) | 0 | 4 (10) |
In both groups, the most common cause of cellulitis was sinusitis (42.5%), and the lowest cause was dacryocystitis (5%) and dental infection (5%) in both groups. The frequency of sinusitis was significantly higher in orbital cellulitis (63.63%) than in preseptal cellulitis (34.48%). After sinusitis, skin ulcers (24.13%) and trauma (17.24%) were the most common causes of preseptal cellulitis, respectively, whereas, in orbital cellulitis, there was no case of skin ulcer or trauma infection (Table 4) (P-value < 0.05).
| Cause | Female, No. (%) | Male, No. (%) | All, No. (%) |
|---|---|---|---|
| Sinusitis | 10 (34.48) | 7 (63.63) | 17 (42.5) |
| Skin lesions | 7 (24.13) | 0 | 7 (17.5) |
| Trauma | 5 (17.24) | 0 | 5 (12.5) |
| Surgery around the eyes | 2 (6.89) | 2 (18.18) | 4 (10) |
| Foreign body | 2 (6.89) | 1 (9.09) | 3 (7.5) |
| Dacryocystitis | 2 (6.89) | 0 | 2 (5) |
| Dental infection | 1 (3.44) | 1 (9.09) | 2 (5) |
Antibiotics consisted of ceftriaxone, cloxacillin, vancomycin, clindamycin, ceftazidime, and penicillin. These antibiotics were used alone or in combination with two or more medications depending on the patient’s medical need. The most commonly used antibiotics in both types of cellulitis were ceftriaxone-cloxacillin (eight cases of preseptal cellulitis and five cases of orbital cellulitis). The most common antibiotics used in the treatment of preseptal cellulitis were ceftriaxone-vancomycin combination, and the most antibiotic in orbital cellulitis patients was ceftriaxone-cloxacillin combination. Ceftriaxone-clindamycin and ceftriaxone-vancomycin-clindamycin were used only in the treatment of preseptal cellulitis, and ceftriaxone-vancomycin-penicillin and ceftazidime-vancomycin were used only in the treatment of orbital cellulitis (Table 5).
| Drug(S) Used | Preseptal Cellulitis (N = 29) | Orbital Cellulitis (N = 11) | All (N = 40) |
|---|---|---|---|
| Ceftriaxone-cloxacillin | 8 | 5 | 13 |
| Ceftriaxone-vancomycin | 9 | 3 | 12 |
| Ceftriaxone | 6 | 1 | 7 |
| Ceftriaxone-clindamycin | 5 | 0 | 5 |
| Ceftriaxone-vancomycin-penicillin | 0 | 1 | 1 |
| Ceftazidime-vancomycin | 0 | 1 | 1 |
| Ceftriaxone-vancomycin-clindamycin | 1 | 0 | 1 |
5. Discussion
Inflammation of the eyelids and tissues surrounding orbit without symptoms of orbital involvement (such as proptosis of the eye or restriction of eye movements) is commonly known as preseptal cellulitis, which is a type of facial cellulitis. It is more common in young children and may occur following bacteremia, trauma, infectious wounds, or abscesses in orbital areas such as bioderm, glomerulus, conjunctivitis, dacryocystitis, and insect bites. Patients usually present with eyelid swelling that may be severe enough to impair the evaluation of the globe. In contrast, orbital cellulitis is an inflammation of the orbital tissues behind the septum, which presents with symptoms of proptosis, restriction of eye movements, chemosis, swelling of the eyelids, and, in severe cases, decreased vision, and pressure on the optic nerve. Patients usually feel ill and have fever and leukocytosis.
The present study was performed on the records of patients admitted to pediatric ward of Ali-Ibn-Abitaleb Hospital in Zahedan as a central hospital for a period of two years from 2016 to 2018 with the diagnosis of preseptal or orbital cellulitis. The number of patients during the study period was 40 patients with 72.5% hospitalization due to pre-orbital cellulitis and 27.5% due to orbital cellulitis diagnosis. The frequency of preseptal vs orbital cellulitis in the study by Goncalves et al. (8) was 84.54% and 15.45%, and in Uy and Tuano (10) were 62% and 38%, respectively, that were consistent with the present study.
In the present study, the ratio of male to female in both groups of preseptal and orbital cellulitis was about 1.2, and there was no significant difference between the two sexes. This study was consistent with the study of Rodriguez et al. (11), who did not show a significant difference between the sexes. Uy and Tuano’s study showed that the ratio was 1.2 in preseptal cellulitis, while 2.2 in orbital cellulitis (10), and a 15-year epidemiological study in Saudi Arabia showed the ratio was 1.65 (12).
In the present study, the most common clinical findings were eyelid edema (97.5%), pre-septic cellulite (96.55%), and orbital cellulitis (100%), which were consistent with the findings of Bagheri et al. (13) Findings by Uy and Tuano’s study were also aligned (10).
No extraocular muscle paralysis and chemosis were reported in this study, while in other studies, including the study of Uy and Tuano (10), 89% and 77% of patients with orbital cellulitis were reported, respectively, and in Bagheri et al.’s study (13), only one case had extraocular muscle paralysis and 33.7% had chemosis. The reason for the difference between previous studies and the present study can be attributed to the different patients and different treatment methods of this study compared to recent studies.
In our study, only two patients (5%) with orbital cellulitis showed proptosis and limited eye movement, while in the study of Bagheri et al. (13), 20.7% and 38%, respectively, were reported, in the Robinson et al.’s study (14) reported 6 cases of proptosis, in the study of Welkoborsky et al. (15), 7 children with ocular movement disorders and the study of Goncalves et al. (8) reported 9 cases of proptosis. The results of these studies were somewhat consistent with our study because proptosis and restricted eye movement are mainly seen in patients with orbital cellulite.
The most common paraclinical findings were ESR increase in 87.5% of patients (86.20% in preseptal cellulitis and 90.90% in orbital cellulitis), and leukocytosis in 80% of patients (86.20% in preseptal cellulitis and 63.63% in orbital cellulitis). As seen, there is no significant difference between the two cellulitis types in the paraclinical findings of our study. In the study of Santos et al. (16), leukocytosis and increased CRP were more frequently reported in patients with orbital cellulitis than in patients with preseptal cellulitis. Welkoborsky et al. (15) reported an increase in white blood cell count and CRP in children who had orbital cellulitis due to sinusitis compared to children who had non-inflammatory orbital problems. According to previous studies, the prevalence and distribution of paraclinical findings in other studies were not consistent with the present study, which was due to differences in the number of orbital cellulitis patients (only 1 in our study), severity of disease, and individual examiner accuracy.
In the present study, the most common underlying cause in both types of cellulitis, sinusitis, was 42.5% (63.63% in orbital cellulitis and 34.48% in preseptal cellulitis), and as seen, the frequency of sinusitis was higher in orbital cellulitis than in preseptal cellulitis. The second underlying cause in preseptal cellulitis patients was cutaneous ulcers, and in patients with orbital cellulitis was orbital surgery. Rare cases were related to dacryocystitis and tooth infection, which is similar to the findings of most other studies. In the study of Bagheri et al. (13), the most common cause of both types of cellulitis was sinusitis with 36.6% (orbital cellulitis with 53.8% and preseptal cellulitis with 24.1%), the second leading cause of preseptal cellulitis was skin lesions, and in orbital cellulitis was surgery around the eye. In the study of Santos et al. (16), infection of the sinuses was 28.5% in preseptal cellulitis, and 85.5% in orbital cellulitis, and other causes of preseptal and orbital cellulitis were infection of the tooth, trauma, oculolacrimal infection, skin infection, and insect bites. In Robinson’s study, sinus infection was the most common cause of orbital cellulitis, the other underlying causes were mild facial trauma and orbit, insect bites, and tooth pain (14). In the study of Uy and Tuano (10), the three most common causes of preseptal cellulitis were eyelid infection, eyelid trauma, and nasal-lacrimal duct obstruction; therefore, the three most common causes of orbital cellulitis were eyelid infection, sinusitis, and dental abscess. In the study of Chaudhry et al. (12), the most common cause of orbital sinusitis was sinusitis (39.4%) followed by trauma. In a 10-year epidemiological study of orbital and preseptal cellulitis in China, the most common orbital cellulitis risk was paranasal sinus disease, and the most common risk factors for preseptal cellulitis were pediatric skin lesions and adult dacryocystitis (17).
According to most studies, bacterial sinusitis causes secondary orbital cellulitis with secondary expansion to the globe. Patients often have a history of chronic sinusitis or a history of pre-illness upper respiratory infection. Improper sinus drainage and blockage of the mucociliary transfer system can lead to bacterial overgrowth and bacterial sinusitis. The anatomical proximity of the sinuses to the orbits and the thinness and sometimes congenital defects of the intercostal bones of the sinuses and the globe will transmit infection and orbital involvement. The lamina papyrus is a thin paper-like barrier that separates the orbit from the ethmoid air cells as well as creates a rich vein system between the ethmoid sinus and the orbit that these veins lack valves. These complexes are discharged into the upper and lower ophthalmic veins and eventually into the cavernous sinus (18). With age, the sinus cavity enlarges substantially, but its outflow remains almost as basic as it was in young children. The relative extent of Ostia in young children is somewhat justified by the higher incidence of acute sinusitis in this group, with frequent infections of the upper respiratory tract tending to involve the nose and sinuses as a single structure (19).
In the present study, antibiotics of ceftriaxone, cloxacillin, vancomycin, clindamycin, ceftazidime, and penicillin were used as a combination of two drugs and a multi-drug in 82.5% of patients with both types of cellulitis. Only ceftriaxone antibiotics were used in six patients with preseptal cellulitis and one patient with orbital cellulitis as an individual. In the study of Uy and Tuano (10), antibiotics were used for the treatment of all patients with preseptal cellulitis, but intravenous antibiotics were required for 82% of cases. Cloxacillin with oxacillin was the initial treatment of choice. In patients with orbital cellulitis, all patients were prescribed intravenous antibiotics, and monotherapy with cloxacillin or oxacillin was the most common treatment (15). In the Robinson et al. study (14), all patients were administered intravenous antibiotics who used Broad-spectrum antibiotics, but the three most commonly used antibiotics were benzylpenicillin, Ofloxacin, and metronidazole. In Crosbie et al. study (20), all patients were administered cefotaxime IV, and cloxacillin IV, and those with allergies were treated with topical nasal xylometazoline hydrochloride. In the study of Chen et al. (21), 65% of children were injected with both antibiotics and steroid IV, the rest 35% were treated only with Intravenous. Finally, children who received steroids in addition to antibiotics were hospitalized for a shorter time (21). Bagheri et al. (13) used a range of antibiotics, including cefalothin, gentamicin, amikacin, cefazolin, ceftazidime, ceftriaxone, vancomycin, metronidazole, ciprofloxacin, ampicillin, cloxacillin, and clindamycin. As shown, the results of recent studies were largely consistent with the results of the present study. These reasons can be attributed to the small differences in the opinions and experiences of the individual who examines the patient, the differences in the clinical and paraclinical symptoms of the patients, the severity of the disease, and the different responses of each individual to all types of medications.
5.1. Conclusions
Orbital and preseptal cellulitis was approximately similar in both sexes. The most common clinical and paraclinical findings were edema and redness of the eyelids, respectively, and increased ESR. The most common cause of orbital and preseptal cellulitis was sinusitis. The consequences of the underlying diseases can be prevented by timely treatment.