1. Background
Childhood voiding and defecation dysfunction are common problems in children of all ages worldwide (1-5). The prevalence of bowel and bladder dysfunction in children is reported to be approximately 47% (1, 6). Until recently, the association of urinary and fecal dysfunction was considered accidental findings, but now it is accepted that due to the similarity of embryonic origin and joint denervation of the genitourinary and gastrointestinal tract, the possibility of urinary incontinence defecation dysfunction is possible. In most cases, the defense dysfunction of one device may be more pronounced and more noticeable than the other (3, 7). Urinary incontinence is the inability to control urinary at an age when children should naturally be able to control their urination. This dysfunction is a common problem in children due to delays in bladder maturation and urinary tract pathways (8, 9). Bladder dysfunction, according to the International Association for the Continuity of Children (ICCS), in children above 5 years of old, includes urinary incontinence (any involuntary loss of urine), enuresis (while sleeping), and increases or decreases of the neutralization frequency (the daily neutralization frequency at least 8 times and < 3, respectively). These definitions are related to children over 5 years (10, 11). Constipation is the most common bowel dysfunction in children. Parents have different definitions of constipation, and defecation may be interpreted as constipation, high stool volume, decreased frequency, and fear of defecation. Constipation is defined as a hard, bullet-like stool for at least 2 weeks. Another common pattern of constipation is functional bowel retention, which is the voluntary holding of stools with a large diameter and often painful stools at long intervals. Stool incontinence occurs when the sphincter pressure exceeds the normal pressure, and the baby’s underwear becomes dirty (12).
2. Objectives
Due to the different ethnic and socio-cultural characteristics, this study was conducted to investigate the frequency of voiding and defecation dysfunction in primary school children.
3. Methods
This cross-sectional descriptive-analytical study was performed on 400 children aged 7 to 13 years in Zahedan in 2016. Students aged 7 to 13 were selected to enter the study for a 1-year period. The subjects were selected by census among male and female students. The inclusion criteria were all students between the ages of 7 and 13 willing to participate in the study. Exclusion criteria were children with congenital neurological or urological problems and kidney disease. Data were collected through a questionnaire. Questionnaire questions were asked of each student, and explanations were given for each question if necessary. If the student was unable to answer or the answers were not reliable, their parents would be contacted, and questions were asked in a face-to-face session. The questionnaire questions were taken from Nelson’s 2016 book, which was used in an article entitled “Quantitative Standardization of Urinary dysfunction Symptoms” conducted by Farhat in 2000 (7).
The questionnaire related to urinary incontinence includes 10 questions. If the score was more than or equal to 6 in girls and more than or equal to 9 in boys, the person was considered as having urinary incontinence. Out of 400 students who filled out the urinary questionnaire, 13 were excluded due to incomplete answers. Therefore, 387 students enrolled in the study. Questions about defecation patterns were asked using the “Bristol stool chart” and were determined whether or not the person had a bowel dysfunction (13). Out of 400 students tested for defecation dysfunction, 17 answered the questionnaire incompletely and were excluded from the study. Therefore, the data obtained from 383 students were described in the study.
Finally, the data were collected and analyzed using SPSS 16 version (SPSS Inc, Chicago, Ill, USA). Statistical analysis was performed using descriptive and analytical statistics of the chi-square test. P-values less than 0.05 were considered statistically significant.
The research was approved by the Ethics Committee of Zahedan University of Medical Sciences (code: IR.ZAUMS.REC.1394.042) and is the result of a student thesis with code 1608.
4. Results
Of the 400 studied students, 188 were girls (47.1%) with a mean age of 10.2 ± 2.12 years, and 212 were boys (52.9%) with a mean age of 9.84 ± 2.02 years.
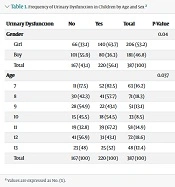
Table 1 shows the frequency of urinary dysfunction in children by age and sex.
| Urinary Dysfunction | No | Yes | Total | P-Value |
|---|---|---|---|---|
| Gender | 0.04 | |||
| Girl | 66 (33.1) | 140 (63.7) | 206 (53.2) | |
| Boy | 101 (55.9) | 80 (36.3) | 181 (46.8) | |
| Total | 167 (43.1) | 220 (56.1) | 387 (100) | |
| Age | 0.037 | |||
| 7 | 11 (17.5) | 52 (82.5) | 63 (16.2) | |
| 8 | 30 (42.3) | 41 (57.7) | 71 (18.3) | |
| 9 | 28 (54.9) | 22 (43.1) | 51 (13.1) | |
| 10 | 15 (45.5) | 18 (54.5) | 33 (8.5) | |
| 11 | 19 (32.8) | 39 (67.2) | 58 (14.9) | |
| 12 | 41 (56.9) | 31 (43.1) | 72 (18.6) | |
| 13 | 23 (48) | 25 (52) | 48 (12.4) | |
| Total | 167 (100) | 220 (100) | 387 (100) |
a Values are expressed as No. (%).
Of the 387 students surveyed, 220 (56.9%) had urinary dysfunction, and 167 (43.1%) were healthy.
Also, of the 387 students, 206 (53.2%) were girls, of whom 66 (33.1%) were healthy, and 140 (67.9%) had urinary dysfunction. The result of the chi-square test between the 2 variables of urinary dysfunction and sex showed that the P-value is less than 0.05; there is a statistically significant relationship between the prevalence of urinary dysfunction and sex. Also, the prevalence of urinary dysfunction based on age was calculated. The highest prevalence of defecation and urinary dysfunction was at the age of 7 years, and out of all 7-year-old children (63 people), 52 (82.5%) had defecation and urinary disorders. The result of the chi-square test between the 2 variables of urinary incontinence and age showed that the P-value was less than 0.05, showing a statistically significant relationship between urinary dysfunction and age.
Table 2 shows the frequency of defecation dysfunction in children by age and sex.
| Defecation Dysfunction | No | Yes | Total | P-Value |
|---|---|---|---|---|
| Gender | 0.834 | |||
| Girl | 75 (38.3) | 121 (61.7) | 196 (51.1) | |
| Boy | 69 (36.9) | 118 (63.1) | 187 (48.9) | |
| Total | 144 (37.6) | 239 (62.4) | 383 (100) | |
| Age | 0.715 | |||
| 7 | 17 (26.9) | 46 (73) | 63 (16.4) | |
| 8 | 28 (42.4) | 38 (57.6) | 66 (17.2) | |
| 9 | 21 (43.7) | 27 (56.3) | 48 (12.5) | |
| 10 | 20 (60.6) | 13 (39.4) | 33 (8.6) | |
| 11 | 15 (31.2) | 33 (68.8) | 48 (12.5) | |
| 12 | 28 (38.9) | 44 (60.1) | 72 (18.8) | |
| 13 | 15 (28.3) | 38 (71.7) | 53 (15) | |
| Total | 144 (100) | 239 (100) | 383 (100) |
a Values are expressed as No. (%).
Of the 383 students surveyed, 239 (62.4%) had defecation dysfunction, and 144 (37.6%) were healthy.
Of the 383 students surveyed, 196 (51.1%) were girls, of whom 75 (38.3%) were healthy, and 121 (61.7%) had defecation dysfunction, and 187 (48.9%) were boys, of whom 69 (36.9%) were healthy, and 118 (63.1%) had defecation dysfunction. The result of the chi-square test between the 2 variables of defecation dysfunction and sex showed that the P-value was greater than 0.05, showing no significant relationship between defecation dysfunction and sex.
The highest prevalence of defecation dysfunction was at the age of 7 years. Of all children aged 7 to 13 years (63 people), 46 (73%) had defecation dysfunction.
The result of the chi-square test between the 2 variables of defecation dysfunction and age showed that the P-value was greater than 0.05, showing no significant relationship between defecation dysfunction and age.
5. Discussion
Childhood voiding and defecation dysfunction are common problems in children of all ages worldwide (1-5). Our study was conducted to evaluate the frequency of voiding and defecation dysfunction in primary school children in Zahedan in 2016. The results of our study showed that the highest prevalence of fecal incontinence belonged to the age group of 13 (77.1%) and 7 (73%), respectively, and the lowest prevalence belonged to the age group of 10 (39.4%) and 9 (56.3%), respectively. The prevalence of fecal incontinence was not significant among different age groups. The difference in the prevalence of urinary incontinence between girls and boys was statistically significant. The difference in the prevalence of defecation dysfunction between girls and boys was not significant. In the study by Vaz et al., in Brazil, the urinary incontinence label was estimated to be 28% in primary school children, with the highest prevalence among children aged 6 to 8, which is consistent with the present study. The highest prevalence of urinary incontinence in the present study was at the same age range (ie, in children aged 7 years) (8). In other epidemiological studies, Yuksel et al. reported the lowest rate of urinary incontinence in children of age 14 (4.9%) and the highest in children of 6 (23.1%). Risk factors obtained in this study included a lower level of education in parents, history of urinary incontinence in parents in childhood, having more than 2 roommates, having more than 4 siblings, and history of previous urinary tract infection. As can be seen in the study of Yuksel et al., the highest prevalence of urinary incontinence was in the lowest age group (6 years), which is consistent with the results of the present study (14).
Also, Loening-Baucke showed that the prevalence rates of fecal incontinence, urinary incontinence during the day, and nocturnal urinary incontinence were 4.4%, 3.3%, and 1.8%., respectively (2). In another study, Loening-Baucke showed that the prevalence of urinary dysfunction was higher in children from low-income families than in those from middle-income and high-income families. Probably parents with high incomes mostly had a higher level of education; therefore, this can be an advantage in educating and supporting their children (3). The study by Mohammad Jaafari et al. reported prevalence rates of 38.4% for urinary incontinence and 29% for fecal incontinence in children. In their study, the prevalence of urinary incontinence was higher in boys than girls. There was no statistically significant relationship between different age groups. However, in contrast to the present study, the prevalence of urinary incontinence was not related to gender (15). In the study of Yuksel et al. (14), the mean age of children with urinary incontinence was lower than children without urinary incontinence, partially confirming the results of the present study. The prevalence of defecation dysfunction was significantly different based on age and sex. The results of this study are consistent with the study of Chen et al. (16). Using findings from the history and physical examination, as well as ultrasound and radiography of the bladder, they reported prevalence of 44.2% of defecation in normal individuals without urinary tract infection. Also, in this study, the prevalence of dysfunction was higher among girls than boys (16).
They also stated that bowel dysfunction had a proven relationship with more usage of computer games and entertainment; thus, we can reduce the prevalence of these dysfunctions by properly educating parents (14). In a 2017 study, Fazeli found that 19% of children held their urine at least half of the time with various maneuvers (17). In the study by Mohammad Jaafari et al., as well as in the present study, the prevalence of fecal dysfunction was higher in boys than in girls (15). In 2012, Cobussen-Boekhorst reported prevalence of 8% of defecation dysfunction in the United States (18), and Croffie reported prevalence of 28% of constipation in children in Asia in 2006 (19). Studies that investigated the prevalence of urinary dysfunction (such as nocturnal enuresis) have provided different results, such that,10% in Egypt, 16% in Turkey and 16% in China is, 6% India, 11% Nigeria, 33% Saudi Arabia 28 %. (14, 17) and 56.9% Zahedan (Iran). Many studies, including those of Miskulin et al. and Carman et al., have reported a higher incidence of enuresis in boys than in girls (20, 21).
In 2010, Miskulin et al. (20) examined the prevalence of enuresis in 6- and 7-year-old elementary school children and finally reported a prevalence of 1.2%. In a 2013 study, Zargar et al. (22) estimated the prevalence of urinary incontinence in children at 14.4%, which was higher in boys than in girls (22). In a 2013 study, Wolfe-Christensen et al. concluded that the more severe the urinary incontinence, the greater the severity of constipation and psychological problems (23). Based on the study of Carman et al. and Wolfe-Christensen et al., it seems that the diagnosis of the excretory dysfunction and elimination of the underlying factor are necessary; in this regard, education should be comprehensive and include psychological issues (21, 23).
In 2021, Sadeghi-Bojd et al. showed that of the 200 children with enuresis, 134 (67%) were girls, and 66 (33%) were boys, which is the same as ours. Fecal incontinence was observed in 99 cases (49%), and 101 (51%) did not have fecal incontinence. Urinary tract infection was observed in 142 children (71%). According to imaging studies, 34 children (17%) with enuresis had congenital kidney abnormalities, and 166 (83%) had no kidney problems (24).
One of the limitations of our study is that the data were obtained from a questionnaire. Some studies have shown that parents report some symptoms less than the actual amount.
Also, our study represents a small sample of the society, and to generalize it to the whole society, further studies in different parts of the country are highly recommended.
Therefore, we suggest that randomized clinical trials are needed to compare parental reports with objective clinical data.
5.1. Conclusions
The prevalence of defecation dysfunction in school-age children was much higher than in previous studies. This may be due to differences in cultural and geographical environments. Due to the high prevalence of defecation dysfunction in children, it is recommended to have more focus on public education on various types of urinary and fecal dysfunction in urban and rural communities.