1. Background
Knowledge about the age-matched penile size values enables the examiner to find out the abnormal penile size and keep careful track of treatment (1). There are several ways to measure penis length, including flaccid, stretched, erected, and ultrasonography (2, 3). Sometimes, evaluation of such children is delayed due to the lack of proper diagnosis (4). Delays in diagnosing and treating this problem can lead to serious complications after puberty, including anxiety, unsuccessful sexual relationships, and premature ejaculation (5). The best way to prevent this delay is to use international standards for penis measurement. Nevertheless, there is still a misdiagnosis or overdiagnosis. Aslan et al. (6) found that out of 65 children with a primary diagnosis of micropenis referred by primary care physicians and pediatrics, only 45 cases had true micropenis (69%). The main drawbacks of stretched penile length (SPL) method are obesity and buried penis, incorrect penis measurement in the stretched position due to excessive or inadequate stretching, insufficient physicians’ information about the current standards for aged-matched children's penis length, different techniques utilization, and possible mistakes by different examiners (intra- and inter-observer errors) (7).
Most research on penis size has been performed in infancy or adulthood, and there are few studies in childhood (6 - 15 years old). The most standard penis size tables are set for infants up to 10 years old, and normative data is unavailable for 10 - 15 years. Furthermore, in most studies, penis size has been calculated by the stretched method, and less attention has been paid to the flaccid technique, which may be a more straightforward method with less error (8). Today, SPL is used for measuring penis size. Therefore, due to the mentioned drawbacks of the SPL method, standardization and the creation of a new cut-off point for non-SPL (flaccid method) can help in more accurate and precise penis size measurement. It should be noted that this new method does not replace the standard SPL technique. However, using the two methods together may help to detect the size of the penis more accurately, especially in children.
2. Objectives
The purpose of this study was to establish novel reference values and flaccid penis length cut-off points for prepubertal children (6 - 15 years) and to compare the flaccid with stretched penile length. The main aim of this research was to familiarize primary care physicians, specialists, nurses, and researchers with the flaccid method and reduce the observers’ diagnostic errors using two methods of penile length measurement.
3. Methods
3.1. Study Setting and Design
This cross-sectional observational analytic study was conducted in two tertiary primary care hospitals, Tehran, Iran, during February 2011-August 2021. The samples were selected through the convenience sampling method.
3.2. Subjects and Age Slots
In this study, 300 children with a definitive diagnosis of micropenis and 300 healthy boys with normal penis length were studied. The inclusion criteria were healthy boys aged 6-15 without penile surgery. The exclusion criteria were webbed, trapped, buried penis, chordee, penile torsion, hypospadias, and abnormalities in external genitalia. A total of 260 participants were considered for the study using the statistical formula
3.3. Penile Length Measurement
All measurements were performed in the outpatient clinic room at 20 - 23°C supine by a flexible plastic ruler (SUPA Medical Devices, Iran). By compressing pubic fat, the distance between the tip of the glans to the pubic bone was calculated. When the penis was fully stretched, it was called SPL, and when it was not stretched (flaccid), it was named non-stretched penile length (NSPL). Two observers (a pediatrician and an urologist) performed measurements twice, and the mean of four values was calculated and recorded.
In order to obtain the NSPL (flaccid) cut-off point, the mean values of SPL and NSPL were separately calculated for each age slot, and then we subtracted these two values to get the mean difference (mean difference = mean SPL - mean NSPL). Finally, the resulting number (mean difference) was subtracted from the standard SPL cut-off point to obtain the NSPL cut-off for each age slot. For example, in the 6 - 7 age slot, the mean SPL was 2.49 cm, and the mean NSPL was 1.98 cm, resulting in a mean difference of 0.51 cm. According to the standard table of penile length (9), the standard SPL cut-off point for this slot was 3.3 cm, and the NSPL cut-off was determined as 2.8 cm (3.3 - 0.51 cm ≈ 2.8 cm).
3.4. Main Outcome Measures
The SPL, NSPL, mean differences, SPL cut-off point, and new NSPL cut-off point were measured for children aged 6 - 15 years. The primary study outcomes were sensitivity, specificity, negative predictive value (NPV), positive predictive value (PPV), and accuracy of NSPL cut-off point.
3.5. Statistical Analysis
All the data were analyzed by SPSS version 25.0 (IBM SPSS Inc., Chicago, IL, USA), and P-value < 0.05 were statistically significant. The quantitative data were shown as mean and standard deviation (SD). t-test was used for the statistical analysis of variables, and Spearman’s correlation coefficient was utilized to find the correlations between variables. The receiver operating characteristic (ROC) curve drawn by GraphPad Prism version 8.3.0 (538) was utilized to define sensitivity, specificity, PPV, NPV, and diagnostic accuracy for the new cut-off point. Furthermore, the area under the ROC curve (AUC) was calculated to determine the diagnostic power of the test.
3.6. Inter-observer and Intra-observer assays
A t-test was utilized to evaluate the difference between the obtained values by the two observers. The interclass correlation (ICC) was also assessed to check the repetition values of each observer.
4. Results
4.1. Demographic Characteristics of Subjects
Mean ± SD of height was 145.3 ± 13.1 cm (119-176 cm), weight was 55.16 ± 16.53 kg (20 - 110 kg), and body max index 25.76 ± 5.93 kg/m2 (13.2 - 42.17 kg/m2). The mean ± SD of SPL and NSPL in children with micropenis was 2.98 ± 1.17 cm (1.3 - 7.1 cm) and 2.3 ± 1 cm (1 - 5.5 cm), respectively. In addition, the mean ± SD of SPL and NSPL in healthy children was 6.04 ± 1.61 cm (3.9 - 10.1 cm) and 5.1 ± 1.53 cm (2.5 - 9 cm), respectively. The correlation coefficient (r) between SPL and NSPL was 0.962 (P = 0.001). This finding pointed out that for each 1 cm increase in SPL, the NSPL rises by 0.962 cm.
4.2. Estimation of NSPL Cut-off Point
All age slot parameters (mean, SD, and mean difference) are demonstrated in Table 1. The mean differences of SPL and NSPL for the age slots 6 - 7, 7 - 8, 8 - 9, 9 - 10, 10 - 11, 11 - 12, 12 - 13, 13 - 14, 14 - 15, and 15 - 16 years were 0.51, 0.61, 0.58, 0.51, 0.61, 0.64, 0.62, 0.7, 0.64, and 1 cm, respectively. The NSPL cut-off points for the age slots 6 - 7, 7 - 8, 8 - 9, 9 - 10, 10 - 11, 11 - 12, 12 - 13, 13 - 14, 14 - 15, and 15 - 16 years were 2.8 (3.3 - 0.51 ≈ 2.8), 2.9 (3.5 - 0.61 ≈ 2.9), 2.9 (3.5 - 0.58 ≈ 2.9), 3.8 (4.3 - 0.51 ≈ 3.8), 3.9 (4.5 - 0.61 ≈ 3.9), 4.4 (5 - 0.64 ≈ 4.4), 4.2 (4.8 - 0.62 ≈ 4.2), 4.8 (5.5 - 0.7 ≈ 4.8), 6.6 (7.2 - 0.64 ≈ 6.6), and 8.1 cm (9.1 – 1 ≈ 8.1 cm), respectively. The SPL and NSPL cut-off points of all age slots are defined in Table 2.
| Age Slots, Year /Groups | SPL | NSPL | |||||
|---|---|---|---|---|---|---|---|
| Min | Max | Mean ± SD | Min | Max | Mean ± SD | Mean Difference b | |
| 6 - 7 | 0.51 | ||||||
| MP | 2.3 | 2.8 | 2.49 ± 0.13 | 1.5 | 2.2 | 1.984 ± 0.21 | |
| H | 3.9 | 7.1 | 5.27 ± 0.8 | 3 | 6 | 4.39 ± 0.72 | |
| 7 - 8 | 0.61 | ||||||
| MP | 2.5 | 3.6 | 3.21 ± 0.29 | 2 | 3 | 2.6 ± 0.24 | |
| H | 5.9 | 7.1 | 5.6 ± 0.84 | 3.2 | 5.8 | 4.7 ± 0.75 | |
| 8 - 9 | 0.58 | ||||||
| MP | 2 | 2.6 | 2.26 ± 0.22 | 1.4 | 2.1 | 1.68 ± 0.23 | |
| H | 3.9 | 7.7 | 5.97 ± 0.99 | 3 | 6.4 | 5.01 ± 0.93 | |
| 9 - 10 | 0.51 | ||||||
| MP | 1.5 | 3.7 | 2.55 ± 0.74 | 1 | 3.1 | 2.04 ± 0.71 | |
| H | 3.9 | 7.3 | 5.2 ± 0.38 | 3.1 | 6.5 | 4.39 ± 0.29 | |
| 10 - 11 | 0.61 | ||||||
| MP | 1.5 | 3.6 | 2.45 ± 0.79 | 1 | 3.1 | 1.84 ± 0.77 | |
| H | 3.9 | 7.8 | 5.26 ± 0.32 | 3 | 6.7 | 4.35 ± 0.24 | |
| 11 - 12 | 0.64 | ||||||
| MP | 1.3 | 3.7 | 2.68 ± 0.82 | 1 | 3.5 | 2.04 ± 0.73 | |
| H | 3.9 | 7.8 | 5.59 ± 0.23 | 3.1 | 7 | 4.59 ± 0.15 | |
| 12 - 13 | 0.62 | ||||||
| MP | 1.5 | 3.5 | 2.26 ± 0.6 | 1 | 2.9 | 1.64 ± 0.55 | |
| H | 3.9 | 8.2 | 6.02 ± 0.49 | 3 | 7.1 | 5.14 ± 0.37 | |
| 13 - 14 | 0.7 | ||||||
| MP | 1.5 | 3.5 | 2.5 ± 0.57 | 1.1 | 2.5 | 1.81 ± 0.51 | |
| H | 3.9 | 9.8 | 7.2 ± 0.69 | 3.3 | 9 | 6.19 ± 0.67 | |
| 14 - 15 | 0.64 | ||||||
| MP | 2 | 3.5 | 2.68 ± 0.5 | 1.3 | 3 | 2.04 ± 0.47 | |
| H | 4 | 10.1 | 8 ± 0.32 | 2.5 | 9 | 6.95 ± 0.32 | |
| 15 - 16 | 1 | ||||||
| MP | 3.9 | 7.1 | 4.9 ± 0.92 | 2.5 | 5.5 | 3.91 ± 0.66 | |
| H | 9.5 | 14.2 | 13.1 ± 1.6 | 7.5 | 12.2 | 11.1 ± 1.5 | |
Abbreviations: SPL, stretched penile length; NSPL, non-stretched penile length (flaccid); Min, minimum; Max, maximum; SD, standard deviation; MP, micropenis; H, healthy boys.
a Values are expressed in cm.
b Mean difference = mean SPL-mean NSPL.
| Age Slots (y) | Mean Difference | Standard SPL Cut-off Point | NSPL Cut-off Point |
|---|---|---|---|
| 6 - 7 | 0.51 | 3.3 | 2.8 |
| 7 - 8 | 0.61 | 3.5 | 2.9 |
| 8 - 9 | 0.58 | 3.5 | 2.9 |
| 9 - 10 | 0.51 | 4.3 | 3.8 |
| 10 - 11 | 0.61 | 4.5 | 3.9 |
| 11 - 12 | 0.64 | 5 | 4.4 |
| 12 - 13 | 0.62 | 4.8 | 4.2 |
| 13 - 14 | 0.7 | 5.5 | 4.8 |
| 14 - 15 | 0.64 | 7.2 | 6.6 |
| 15 - 16 | 1 | 9.1 | 8.1 |
Abbreviations: SPL, stretched penile length; NSPL, non-stretched penile length (flaccid).
a Values are expressed in cm.
b SPL and flaccid (NSPL) cut-off points were defined in 6 - 15 old aged boys. As observed, the ages 11 - 15 years old have been completed in this table. Standard SPL cut-off point = mean SPL - 2.5 SD; NSPL cut-off point = standard SPL cut-off point-mean difference.
4.3. Statics of NSPL Cut-off Point
A total of 600 boys (300 with micropenis and 300 without micropenis) were re-evaluated by a novel NSPL cut-off point and standard SPL cut-off point to assess the sensitivity and specificity of the NSPL cut-off point. Based on the SPL cut-off point, 300 children were non-micropenis, and 300 were micropenis, while the new NSPL cut-off point revealed 284 non-micropenis and 316 micropenis children (16 subjects in the micropenis group were false positive). Status and forecast (reality and observed) of 600 subjects by NSPL cut-off point are shown in Table 3.
| Status and Forecast | Micropenis (N) | Healthy (N) |
|---|---|---|
| NSPL cut-off point shows micropenis | True positive (300) | False positive (16) |
| NSPL cut-off point shows healthy | False negative (0) | True positive (284) |
Abbreviations: NSPL, non-stretched penile length (flaccid); N, number.
a False negative was not observed, and 16 subjects in the micropenis group were false positive.
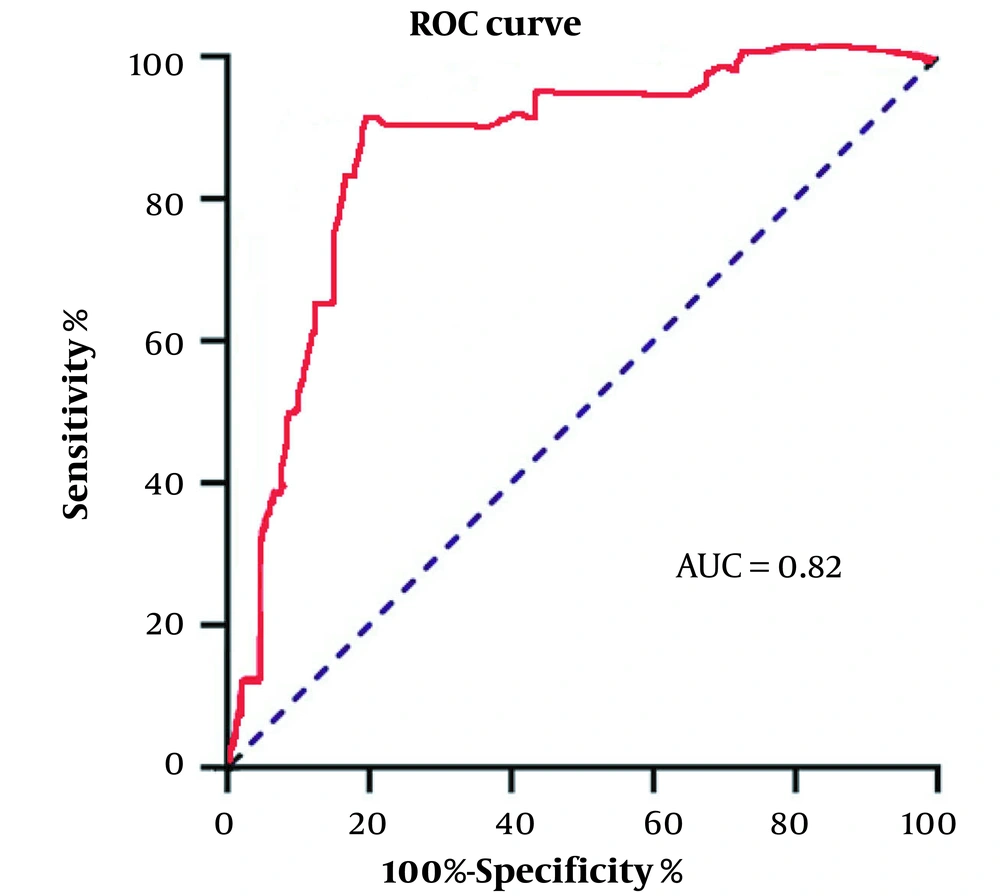
Specificity was calculated as 94.66% = true negative/true negative + false positive (284/284 + 16 = 94.66%), sensitivity as 100% = true positive/true positive + false negative (300/300 + 0 = 100%), and accuracy as 97.33% = true negative + true positive/true positive + false positive + true negative + false negative (284 + 300/300 + 16 + 284 + 0 = 97.33%). PPV, NPV, and other values of the NSPL (flaccid) cut-off point are presented in Table 4. The ROC curve demonstrated the statics of the NSPL cut-off point, and the AUC value in the ROC curve was 0.82. It showed that the diagnostic power of the test was good (Figure 1).
| Statistics | Values | 95 % CI |
|---|---|---|
| Sensitivity cut-off | 100.00 | 98.53 - 100.00 |
| Specificity cut-off | 94.66 | 89.77 - 96.28 |
| Positive likelihood ratio | 15.56 | 9.69 - 25.00 |
| Negative likelihood ratio | 0.00 | |
| PPV | 8.25 | 4.64 - 11.16 |
| NPV | 100.00 | |
| Accuracy | 97.33 | 91.09 - 99.59 |
Abbreviations: PPV, positive predictive value; NPV, negative predictive value.
a Receiver operating characteristic (ROC) curve drawn by GraphPad Prism version 8.3.0.538 was utilized to define the sensitivity, specificity, PPV, NPV, and diagnostic accuracy of the new cut-off point. All values are expressed in percent (%).
4.4. Inter-assay and Intra-assay Observers Analysis
Inter-assay observer analysis showed that SPL and NSPL mean differences between the two observers were not significant (0.03 cm, P = 0.875, and 0.03 cm, P = 0.871, respectively). Furthermore, an ICC rate of more than 80% is desirable and acceptable. The ICC of SPL and NSPL by each observer was 0.997 (P = 0.001). The findings showed that measurement repeatability by each observer was precise and acceptable.
5. Discussion
The previous standard SPL table was set up for birth to 10 years old. The present study aimed to introduce the NSPL method to researchers. Furthermore, the normative data were completed for children aged 6 - 15 years. The sensitivity, specificity, and accuracy of NSPL were 100%, 94.66%, and 97.33%, respectively. It seems that this method was simple and repeatable and may be helpful for the accurate measurement of penile length in children.
It is important to evaluate penis size in routine examinations because external genitalia abnormality may indicate underlying endocrine dysfunction, genetic disease, or structural malformations (10-13). Misdiagnosis causes anxiety and stress for the child and parents and imposes additional and unnecessary diagnostic and treatment costs on the patient and his family. According to the previous studies, the main problem and error were overdiagnosing true micropenis in healthy boys.
A study on 765 children aged 8 - 13 years with an initial diagnosis of a small penis showed that only 20% of the children had true micropenis (14). Another study on 65 children defined that 31% of children referred with small penis were not true micropenis (6). In a recent study on 1798 boys aged 7 - 14 years with an initial diagnosis of a small penis diagnosed by primary care physicians, only 261 cases (15%) had true micropenis. They believed that the lack of familiarity with penis size at any age, incorrect measurement of the penis (erroneous and overstretched), utilizing different techniques, and possible mistakes induced by different observers (intra- and inter-observer errors) were the most important causes of this discrepancy (15). In these studies, SPL was used to measure the penile length, but we applied the flaccid method, and the overdiagnosis rate was about 5.4% (16 subjects false positive).
In the NSPL method, the stretch factor is removed. Therefore, the possibility of error and overstretch by the observers is eliminated and may help in correctly measuring the penis. Due to the mentioned drawbacks of the SPL method, establishing novel reference values and a new cut-off point for NSPL (flaccid method) can reduce the overdiagnosis of micropenis in boys referred to the hospital's outpatient clinic and help in more accurate and precise penis size measurement. It should be mentioned that this new technique does not replace the standard SPL method. However, utilizing two reference values together can help detect the size of the penis more accurately, especially in children.
Scarce data about penis size measurement were found in prepubertal children, and most studies have been performed on neonates, infants, and men, and less attention has been paid to prepubertal ages. Most studies evaluated children up to 10 years old and adult men, and there is a lack of nomograms for boys aged 10 - 15 (8, 16-18). Consequently, the present study was performed at the age of 6 - 15 years, and the penile length was measured for the first time in two flaccid without stretching and stretched methods. The findings of the current study completed this age gap, and the two methods were compared, and new cut-off points were obtained for prepubertal boys.
In the most recent studies, the SPL method has been considered, while the flaccid method has been less discussed. Today, there is no consensus on the preferred and appropriate method for measuring penis length (19). Systematic research reviewed diverse methods of measuring penis length (flaccid, stretched, and erected) in adult men. They found no definitive evidence of superiority among these methods (20). On the other hand, another study on 201 adult men reported that flaccid measurements were relatively accurate in predicting penis size. They believed SPL and NSPL methods underestimated the erect penile size and were significantly observer-dependent (7). From the practical and clinical point of view, it is important to mention that an erect measurement is difficult in the clinical setting to counsel men who came for penile length evaluation, and it is not possible at all for children (21). Our study was performed on prepubertal children and showed that if the flaccid method is correctly performed from the pubic bone (no pubic skin) to the tip of the penis, it can lead to the correct measurement of penile length with acceptable sensitivity, specificity, and accuracy, and along with SPL method can help to correct the diagnosis of true micropenis. Furthermore, it was more tolerable for the child because the penis was not stretched.
One of the limitations of this study was that children under 6 years old were not referred for examination. Parents may have paid less attention to penis size at this age, and as a result, they did not go to the clinic for examination. It is suggested that this issue be resolved by increasing the knowledge of parents and family physicians. Penile size measurement is observer-dependent. Therefore, teaching and retraining the correct method of penile size measurement to primary care physicians and pediatric nurses can help prevent the misdiagnosis or overdiagnosis of this issue. The age-matched value of the penis should be provided to define the abnormal penile length and keep careful track of treatment by physicians.
5.1. Conclusions
This study presented novel non-stretched flaccid reference values for penile length. According to the findings of the current research, sensitivity, specificity, and accuracy of flaccid cut-off points were acceptable with good diagnostic power. This study was a step to attain a precise reference value for penis measurement in prepubertal children. It seemed that the flaccid method is less dependent on the observers, more tolerable by children, more exact, with allied definition, and repeatable. All primary care practitioners and pediatric nurses can use these new cut-off points as a reference for prepubertal boys to prevent the misdiagnosis and/or overdiagnosis of micropenis.