1. Introduction
Congenital giant right atrial aneurysm (CGRAA) is a very rare disease with diverse clinical manifestations. Surgical excision of the aneurysm is the treatment of choice (1, 2). To the best of our knowledge, to date, no CGRAA with retro-left ventricular extension involving coronary artery has been reported. We report a case with an unusually huge congenital right atrial aneurysm with extension to the posterior aspect of the left ventricle with subtle adherence of the posterior descending coronary artery to its wall.
2. Case Presentation
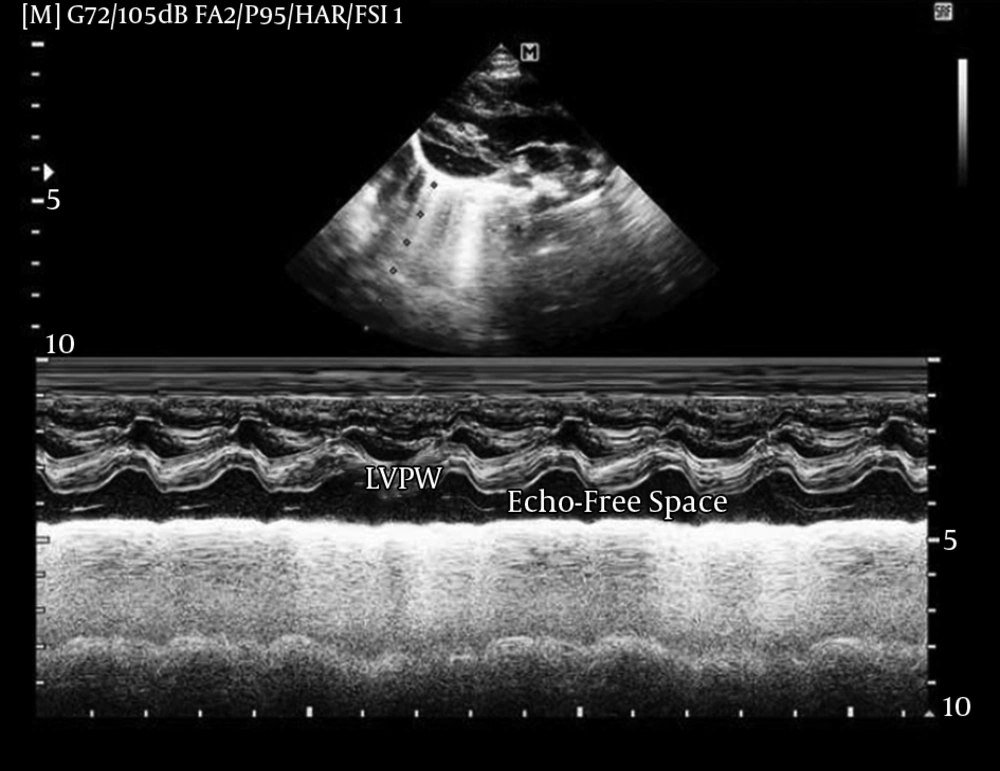
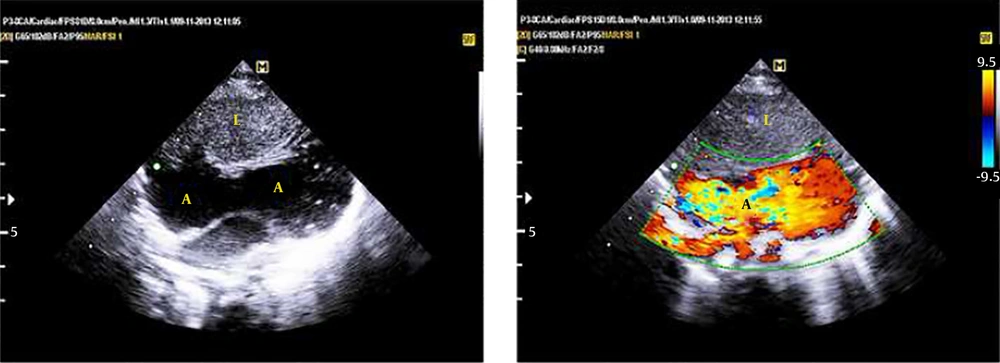
A 3.5-month-old infant with the diagnosis of imperforated anus and hypospadias was referred to our clinic with a history of colostomy in the neonatal period. On physical examination, he was acyanotic with normal cardiac auscultation. Electrocardiogram and chest X-Ray were normal. On echocardiography, an echo-free space was seen behind the left ventricular posterior wall, both in the parasternal long-axis and modified four-chamber views (Figure 1 echo videos 1 and 2 in the supplementary file). There were tissue strands within this space, mimicking the presence of purulent pericardial effusion. Lowering the Nyquist frequency revealed blood flow in this huge effusion-like, echo-free space (Figure 2). Thorough examination showed an unusually shaped congenital giant right atrial aneurysm (CGRAA), with an oblique lie, extending from the right side and anterior of the heart to the left and posterior of the left ventricle (Videos 3 - 5 in the supplementary file). The infant experienced episodes of witnessed transient supraventricular tachycardia during echocardiographic examination and afterwards during admission. He underwent surgical operation for resection of aneurysm (Video 6 in the supplementary file). Immediately, after weaning from cardiopulmonary bypass (CPB), he developed hypotension. The CPB was re-established. Posterior descending coronary artery (PDA) was damaged and the patient died in the operation room.
3. Discussion
We performed a literature review on congenital right atrial aneurysm from 2001 to 2014 (Table 1). Fifteen cases, with age ranging from 20 weeks of gestation to 75 years, are reported from eight countries. However, none of them had the unusual shape and geometry of CGRAA seen in our case. Furthermore, in none of these cases, the coronary artery was attached to the aneurysm.
Congenital giant right atrial aneurysm is a very rare cardiac anomaly and right atrial aneurysms are rarer than the left (3, 4). Yildirim et al. reported 18 cases up to 2006, whereas Chatrath et al. reported 60 cases up to 1998 (4, 5). Klisiewicz et al. reported only seven cases up to 2004 (6). About half-of the reported cases were asymptomatic (7-9). Clinical presentation included arrhythmia, thrombosis, heart failure and incidental cardiomegaly on chest X-ray (10-13). In a recent review by Harder et al., all cases underwent resection of aneurysm (13).
| Authors | Year | Country | Number of Cases | Type of Article | Age at Diagnosis | Gender | Age at Operation | Treatment | Outcome | Presentation | Duration of Follow-Up | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Harder et al. (13) | 2014 | USA | 5 | Case series and review | 26 months | Female | 26 months | Resection | good | Supraventricular tachycardia | 4 m |
| 20 weeks (prenatal) | Not defined | 4 months | Resection | good | - | 3 years of age | ||||||
| Prenatal | Not defined | 15 months | Resection | good | - | 4 years | ||||||
| 18 weeks (prenatal) | Not defined | 6 weeks | Resection | good | - | 2 years | ||||||
| 5 | Male | 5 years | Resection | good | Incidental finding of cardiomegaly | 10 years | ||||||
| 2 | Uppu et al. (12) | 2013 | USA | 1 | Case report | 2 | Male | 2 years | Resection (surgical reduction) | good | Incidental finding of massive cardiomegaly | Not defined |
| 3 | Narain et al. (11) | 2012 | India | 1 | Case report | 18 | Male | 18 years | Medical treatment | good | Right heart failure | Not defined |
| 4 | Zaqout et al. (14) | 2011 | Belgium | 1 | Case report | 7 days | Male | Not defined | Resection | good | Cardiac murmur | Not defined |
| 5 | Lee et al. (15) | 2011 | Korea | 1 | Case report | 2 weeks | Not defined | 2 weeks | Resection | good | Referral case | Not defined |
| 6 | Zhao-xia et al. (16) | 2010 | China | 1 | Case report | 38 | Male | 38 years | Resection | good | Paroxysmal chest pain | Not defined |
| 7 | Agematsu et al. (17) | 2009 | Japan | 1 | Case report | 31 | Male | 31 years | Resection | good | Cardiomegaly on chest X-Ray(CXR) | Not defined |
| 8 | Yoon et al. (8) | 2009 | 1 | Case report | 69 | Female | - | - | good | Incidental finding of cardiomegaly on CXR | Not defined | |
| 9 | Yildirim et al. (4) | 2006 | Turkey | 1 (authors state 18 cases were reported to 2006) | Case report | 42 | Female | Medical treatment (anticoagulation therapy) | good | Palpitation, dyspnea and precordial pain | Not defined | |
| 10 | Klisiewicz et al. (6) | 2004 | Poland | 1 (authors state 7 cases were reported to 2004) | Case report | 30 | Female | 30 years | Resection | good | Abnormal cardiac silhouette | Not defined |
| 11 | Chatrath et al. (5) | 2001 | USA | 1 (authors state 60 cases were reported to 1998) | Case report | 5 | Male | 5 years | Resection | good | Incidental finding of cardiomegaly | 1 year |
Normal P wave on Electrocardiography (ECG), despite huge enlargement of right atrium (RA) (1), can be explained by the absence of myocardium in the aneurysmal wall.
We report on an infant with an unusual–shaped CGRAA and imperforated anus, leading to death because of injury to the posterior descending coronary artery (PDA) that was attached to the aneurysmal wall. This case indicates the importance of careful preoperative delineation of coronary arteries in patients with CGRAA with a retro-left ventricular extension. Resection of aneurysm is not the optimal treatment for all cases of CGRAA. Closure of the neck of the aneurysm from the inside of the right atrium is recommended in cases with this special anatomy, as in our case.
3.1. Conclusion
This case was the first reported case of CGRAA associated with imperforated anus and retro-left ventricular extension of the CGRAA with posterior descending coronary artery embedded in the wall of the aneurysm. Our patient died due to damage to PDA. Careful delineation of coronary artery anatomy by either coronary computerized tomography (CT) angiography or conventional coronary angiography, is mandatory in these cases. Simple closure of the neck from inside RA seems to be a safer surgical approach.