1. Background
Kawasaki disease (KD) is an acute, febrile, and systemic vasculitis with unknown etiology while special infections and super-antigens are considered to have roles in disease development (1, 2). Its prevalence in Asian countries was estimated as 239 cases per 100000 children less than five years old (3, 4).
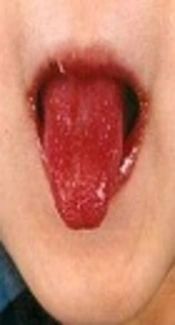
High grade fever, rash, redness of the lips and a typical strawberry tongue, cervical lymph node enlargement, and swelling over the hands/feet are common presentations of the disease (5, 6). One of the most common complications of KD is cardiac complications, which is present with coronary artery disease, myocarditis, and pericarditis (2). Coronary artery disease remains as the most prevalent cardiac complication presenting in one fourth of untreated children (7, 8).
Administration of intravenous immunoglobulin (IVIG) during the first 10 days after symptoms detection will result in lower coronary artery aneurysm between 10% - 21% of cases could show drug resistance (9, 10).
2. Objectives
Recently, researchers focus on the predictors of IVIG resistance in children with KD to add additional therapies. We designed this study to evaluate the role of Kobayashi risk scoring for determining refractory KD.
3. Methods
This retrospective study conducted in the children wards of all affiliated hospitals of TUMS (Tehran University of Medical Sciences) between October 2014 and October 2016.
Medical records of all cases with KD were reviewed and demographic data, previous history, coronary artery involvement, valvular diseases, laboratory findings, and days with a fever were extracted for all cases. Then, Kobayashi score was calculated. Patients divided into low and high-risk groups due to Kobayashi score: low risk, Kobayashi score less than four, and high-risk group (Kobayashi score more than four).
Data analysis was conducted by means of SPSS software version 22 (IBM, Chicago, IL, USA).
Data were presented as mean ± SD for continuous variables and frequencies for categorical ones. ANOVA was used for comparing continuous variables. P value less than 0.05 was considered to be significant.
4. Results
A total of 168 cases were enrolled. Fifty-six (33%) were female and 112 (67%) were male. Four cases (2.4%) had pulmonary diseases, four (2.4%) had hypertension, and five (3.1%) had a family history of Kawasaki disease. The most common echocardiographic finding was mitral regurgitation (Table 1).
| Variable | Valvular Involvement |
|---|---|
| MR | 36 (21.4) |
| TR | 12 (7.1) |
| MR + TR | 20 (11.9) |
| MR + TR + PI | 4 (2.4) |
| Kobayashi score | |
| Low risk | 156 (92.9) |
| High risk | 12 (7.1) |
Abbreviations: MR, mitral regurgitation; PI, pulmonary insufficiency; TR, tricuspid regurgitation.
a Values are expressed as No. (%).
There was no significant difference regarding the Kobayashi score in different groups regarding coronary involvement (Table 2).
| Coronary Involvement | Kobayashi Score | P Value |
|---|---|---|
| No involvement | 1.9 ± 1.1 | 0.6 |
| One vessel involvement | 2.3 ± 0.9 | |
| Two vessels involvement | 1.7 ± 0.8 | |
| Three vessels involvement | 2 ± 1.9 |
In cases without coronary involvement, 93.5% were classified as low risk, in one and two vessels involvement groups, all were categorized as low risk and among three vessels involvement cases, 75% were known as low risk.
5. Discussion
The results of the current study showed that Kobayashi score is not proper for predicting coronary involvement in children with Kawasaki disease.
In Japan, Kobayashi score is well established and valuable. Sleeper et al., in 2011, found that the Kobayashi scoring system is not useful for children with KD who live in North America (10).
Previous studies conducted in the USA and UK to determine predictive values of Kobayashi score for IVIG resistance found that the sensitivities were 42% and 58% while the specificities were 87% and 35% (10, 11). In another study in China, Fu et al., reported sensitivity and specificity of Kobayashi score for IVIG resistance as 49% and 72% (12).
KD is a vasculitis with incidence of 7.3 per 100000 in Iranian children (13), which occurs mostly in cases under 5 years (the peak incidence is three to five months for girls and three to five months and at nine to 11 months for boys) (2, 14).
One of the most complications of KD is coronary artery aneurysm while longer duration of fever is strongly associated with coronary artery aneurysm (15).
In one fourth of untreated children, coronary aneurysm occurs while IVIG treatment reduces this rate to 5% (8, 16).
Although timely administration of IVIG will reduce complications, between 10% to 20% of children do not respond to treatment who are at a higher risk of coronary complications (17).
Determining cases who are at a higher risk of developing coronary complications is valuable to protect against ongoing problems. Kobayashi scoring system is helpful in predicting IVIG resistance cases to initiate suitable treatment (18).
In this study, coronary involvement was detected in 26% and Kobayashi score was not predictive of severity of coronary involvement. In a previous study conducted by Zhao et al. (19), the prevalence of coronary artery complications in KD patients was reported as 36%, while this rate was 31.7% in the study of Deng et al. (20).
More studies are needed to evaluate the role of Kobayashi scoring system for predicting severity of coronary artery lesions in Iranian children with KD.
5.1. Conclusions
Kobayashi score is not useful for predicting severity of coronary involvement in children with Kawasaki disease.