We identified 383 patients with a mean age of 5.5 years for over a period of 10 years.
Table 1 shows the demographic characteristics in children with urethral strictures. As shown in
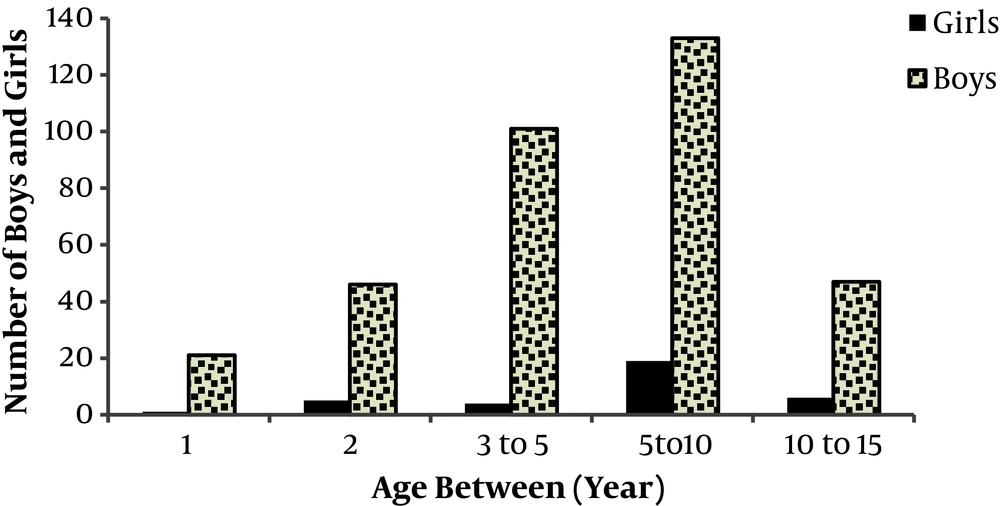
Figure 1, the study population was comprised of 348 boys and 35 girls. In the total population, the mean ± SD age with a minimum of 1 and a maximum of 15 years was 5.5 ± 3.4 years old. The distribution of age in boys with urethral strictures were as follows: 1 year (n = 21), 2 years (n = 46), 3 to 5 years (n = 101), 5 to 10 years (n = 133), and 10 to 15 years (n = 47). In girls, the distribution of age was categorized as follows: 1 year (n = 1), 2 years (n = 5), 3 to 5 years (n = 4), 5 to 10 years (n = 19), and 10 to 13 years (n = 6). As shown in
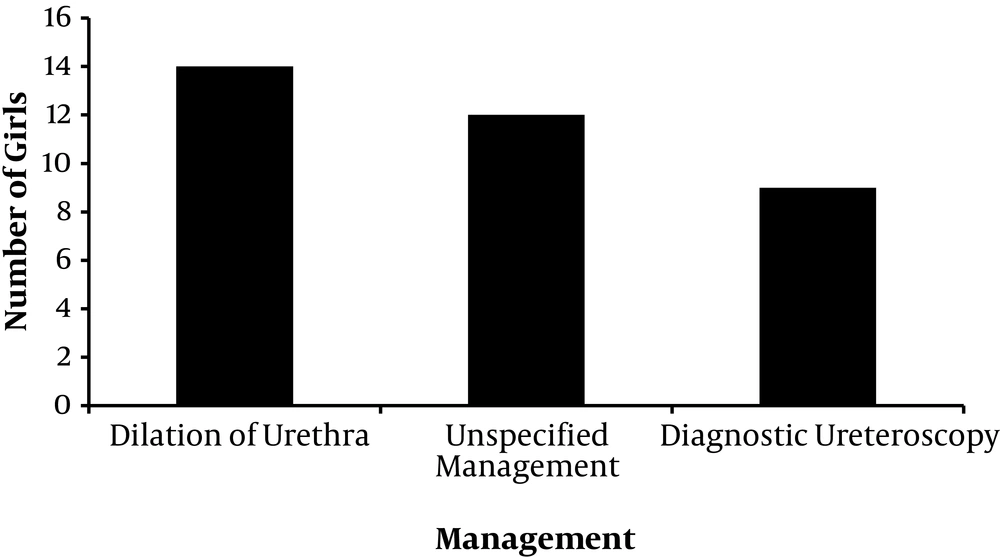
Figure 2, available data associated with management in girls confirmed: dilation of urethra (n = 14), diagnostic ureteroscopy (n = 7), and unspecified management (n = 12).
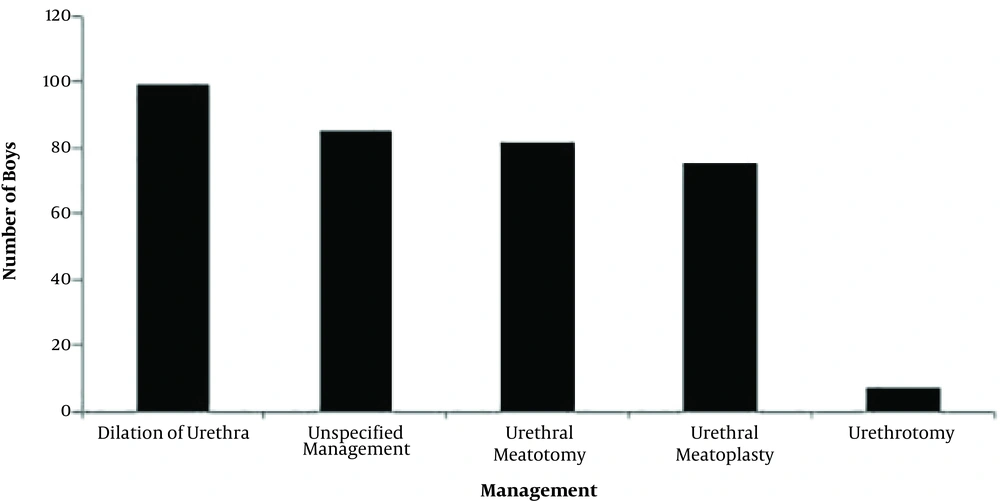
Figure 3 shows management strategy for boys with the disease of urethra ranked as: dilation of urethra (n = 99), urethral meatotomy (n = 82), urethral meatoplasty (n = 75), urethrotomy (n = 7), and unspecified management (n = 85). Management of disorders associated with the age was shown in
Table 2 as there was a significant difference associated with the age at the time of surgery consideration. Statistical analysis based on the Kruskal-Wallis test showed a significant difference between variables (P < 0.0001). The minimum age for urethrotomy in the population studied was at 4 years old. The mean age (year) of 9.1 and 6.4 was associated with urethrotomy and dilation of urethra, respectively that was significantly different from the mean age at the management as meatotomy (4.9) and matoplasty (4.4).