1. Background
According to Utstein’s definition, cardiac arrest (CA) is the halt of heart’s mechanical function due to the lack of a palpable pulse and no response or apnea (agonal respiration). This definition distinguishes cardiac arrest from respiratory arrest, which is featured with apnea and Palpable pulse. According to Utstein’s style, cardiac arrest is categorized as in-hospital, when it occurs in a hospitalized patient who had a pulse at admittance point (1).
There is a growing trend of in-hospital cardiac arrest (IHCA) among adults, so that 292000 cases happen in the USA every year. This figure for children is 15200 and there is no growing trend for children. Given the recurrence cases, annual cardiac arrest cases in adults and children are 357900 and 19900 cases respectively in the United States of America (USA) annually (2). Similar studies using Utstein’s standards have shown notable changes in occurrence rate of IHCA, so that it is 3.25 out each 1000 cases in the east of Asia (3), There are no exact statistics available in Iran, this index has been reported above some international levels in some Asian countries such as the United Arab Emirates (UAE) and Saudi Arabia (4, 5).
Failure to provide timely cares for a CA case leads to death; however, circulation can be established using CPR. The CPR includes measures to revive vital signs of the heart and lungs and the circulation and respiration are sustained mechanically until the return of spontaneous circulation (ROSC). The latest CPR guidelines for adults were revised at basic and advanced levels in 2020 (6).
Studying the outcomes of resuscitation such as primary survival, STD, long-term survival, and cerebral performance of patients after cardiac arrest and return to life through a successful resuscitation are key topics for many researches in Iran and other countries. Studies have reported the ROSC of IHCA with different background diseases and in different wards between 15.3 and 51.03% (7-10). According to the updated report by American Heart Association STD ranges from 3.4 to 22% in 132 countries in the USA (11). A study between 1995 and 2015 on IHCA showed an improvement of shockable rhythm survival from 15.4% to 30.2%. Still, the increase in the non-shockable rhythm to shockable rhythm ratio from 4.4 to 6.4%, and that this increase is significant, can be an indicative of no improvement in total rate of STD (12). On the other hand, there are contradictory statistics compared to children age group, so that survival rate of IHCA cases with asystole cause and pulseless electrical activity (PEA) demonstrates a notable increase, while there has been no improvement in survival rate of IHCA with ventricular fibrillation or pulseless ventricular tachycardia (13). Comparison of IHCA and out of hospital cardiac arrest (OHCA) also yields contradictory results so that some studies report that STD is higher for OHCA and some report that it is higher for IHCA (10, 14). FNO is another index that is used by studies and different results have been reported (10, 15). The updated report by American Heart Association indicates that discharge with favorable neurological outcome from 0.8 to 20.1% (11), In Shockable rhythms 12.7% and in the study of Matsuyama et al. in Osaka, Japan, it was 12.5% (10, 15).
There are several factors effective in the outcomes of resuscitation such as gender, age, type of arrest, witness, non-witness, primary rhythm, defibrillation less than two minutes, good neurological condition without disability before cardiac arrest, hospital ward that cardiac arrest occurs, availability of monitoring, timely response by resuscitation team, resuscitation duration, resuscitation shift, no need to mechanical ventilation after resuscitation, white race, recent surgeries, trauma, cardiac cause, internal pacemaker, low blood pressure before arrest, angiotensin converting enzyme (ACE) inhibitor or ACE treatment, anti-arrhythmic drugs at time of cardiac arrest, clinical diagnosis of sepsis, kidney failure, cancer, and experience of resuscitator with these factors (16-21).
2. Objectives
It is reasonable to say that IHCA with poor prognosis is a challenging problem in hospitals (22), and different studies have reported different results for uncategorized populations. Therefore, there is a need for more studies using similar pattern. Given the importance of this subject, following prior studies by the author in this field, and that there has been no study on the CPR outcomes over the five past years in Kermanshah University of Medical Science or other medical centers in Iran, the present study aimed at assessing the five-year epidemiology and outcomes of in-hospital CPR in educational centers in Kermanshah.
3. Methods
3.1. Design
The study was carried out as cross-sectional study on patients hospitalized due to IHCA and received CPR afterwards from 2014 to 2018.
3.2. Setting and Participants
After obtaining a permission letter from the Department of Research and Technology, the author visited the medical-educational centers in Kermanshah City for sampling. Out of 5240 CPR forms (a standard form of health ministry of Iran) had filled out for adults in theses settings, 4625 forms met the inclusion criteria (Age over eighteen years, in-hospital CA based on the Utstein Style criteria). Patients with CA and no indication of CPR (i.e., those with rigor mortis or livor mortis) and patients with out-of-hospital CA and ROSC before hospital arrival who experienced another CA in emergency department were not included. Thus 1000 of them were selected through systematic sampling (200 forms for each year), it is notable based on Morgan`s table for sample size, power 95% and first type of error 0.05, 357 people were required. Documents of 33 cases were incomplete and replaced by new cases based on systematic sample model. To make sure of the consistency of IHCA report, Utstein’s instruction for IHCA studies was followed.
3.3. Data Collection
Based on the Utstein Style, the core CPR success outcomes are ROSC, STD or for thirty days, and optimum neurological function up to hospital discharge or for thirty days (1). In this study, ROSC was considered as the primary outcome of CPR, also STD and CPC were considered as the final outcome of CPR.
Data gathering tool included a standard form of registering IHCA based on Utstein’s style and cerebral performance categories (CPC) scale. Utstein’s instruction is supported by American Heart Association and other creditable associations in the world for IHCA. The instruction was revised in 2019 and it has been used by several studies in Iran (1, 7, 23). The form contains information like age, gender, work shift, ward of cardiac arrest, cause of cardiac arrest, patient’s primary rhythm, type of cardiac arrest (witness/ no witness), time gap between cardiac arrest and first shock, and long/short-term outcomes. The CPC represents five scales 1 to 5 and the patient is categorized in terms of cerebral performance at five levels of favorable cerebral performance (conscious, aware, doing tasks without help), relative cerebral disability (conscious, adequacy of cerebral performance in doing daily activities, ability to work under protection), sever cerebral disability (conscious, dependence to others to do tasks due to cerebral performance defect), coma or plant life (any level of coma without symptoms of brain death, unconscious, awake but unable to communicate with the environment, asleep-awake periods, spontaneously open eyes), and brain death (apnea, no cerebral reflex, and straight electroencephalograph, and so on). Scores 1 or 2 represents good performance or moderate disability respectively (24, 25).
The information form was based on combining the two measures and making trivial modifications based on research objectives. The form consisted of three parts; (1) demographics, disorders, and background disease; (2) 15 questions about background information as to CPR and ROSC; and (3) Information at discharge if survived, and neurological status of the patient based on CPC measure.
To examine content and face validity of the information form, the experts were consulted about content consistency of the tool with the objectives of study. Content validity index (CVI) and content validity ratio (CVR) were also measured (26). To this end, 20 experts including three anesthesiologist, four emergency medicine specialist, nine holders of MSc’s degree in nursing, four holders of BSc’ degree in nursing working in health centers in Kermanshah City were selected to examine the CVR of the tool. They were asked to examine each item based on a three-point spectrum (necessary, useful but not necessary, and not necessary). The minimum validity, given the number of experts and Lawshe’s coefficient was 0.42. Statements with validity less than this were removed from the tool. In addition, the CVI of the whole toll was obtained equal to 0.85 based on relevance of each item. Reliability of the tool was examined through a primary survey (26). That is, the information form was filled by two colleague researchers for 30 CPR patients based on their medical files and resuscitation form (Code 99). In addition, Kappa consistency coefficient was obtained as total reliability of the tool (Kappa = 0.81).
The resuscitation forms had been filled out during the resuscitation process by participating nurses and physicians under supervision of a supervisor and archived in the hospital. In the cases that cerebral performance status was not clearly recorded at discharge, supplementary information would be sought after using the phone number recorded in the files. To avoid fake results in the cases of several CPRs, only one successful CPR would be recorded.
3.4. Data Analysis
Data were analyzed using the SPSS software (v. 19.0). Descriptive statistics, Chi-square and Fisher’s exact tests were used to assess the relationship of CPR outcomes with demographic characteristics and qualitative variables. Moreover, the logistic regression analysis was performed to predict CPR outcomes. Variables with significant relationship with CPR outcomes in univariable analysis were entered into the logistic regression model.
3.5. Ethical Considerations
The Institutional Review Board and the Ethics Committee of Kermanshah Universities of Medical Sciences, Kermanshah, Iran, approved this study (codes: 95614 and KUMS.REC.1395.651). Necessary permissions for entering the study setting and performing data collection were obtained from the Research Administration of Kermanshah Universities of Medical Sciences, Kermanshah, Iran, and provided to the authorities of the study setting. Patients’ data were managed confidentially. It is noteworthy that in the study setting, consents for using patient data for research purposes were routinely obtained from patients and their family members at the time of hospital admission and were available in-patient medical records.
4. Results
Out of 1000 cases of resuscitation, 220 cases (22%) led to primary survival and ROSC ≥ 30 min and 780 cases (78%) failed. In addition, the number of patients with final success (STD) was 52 (5.2%). Table 1 lists the information about success over different years and based on chi square test. There is a significant difference between ROSCs in 2014 to 2018 (P = 0.043) so that success rate in 2018 is the highest (29.5%) and is the lowest (15.5%) in 2015. However, the difference in terms of STD is not significant (P = 0.631).
| Variables | Results of CPR | ||
|---|---|---|---|
| Not Return of Spontaneous Circulation | Return of Spontaneous Circulation | Statistical Test (P) | |
| Primary return of spontaneous circulation of CPR (spontaneous circulation at least for 30 minutes) | 0.043* | ||
| 2014 | 163 (81.5) | 37 (18.5) | |
| 2015 | 169 (84.5) | 31 (15.5) | |
| 2016 | 156 (78.0) | 44 (22.0) | |
| 2017 | 151 (75.5) | 49 (24.5) | |
| 2018 | 141 (70.5) | 59 (29.5) | |
| Overall | 780 (78.0) | 220 (22.0) | |
| Final survival to discharge of CPR (live discharge of hospital by cerebral function level 1 - 5) | 0.631 | ||
| 2014 | 191 (95.5) | 9 (4.5) | |
| 2015 | 190 (95.0) | 10 (5.0) | |
| 2016 | 191 (95.5) | 9 (4.5) | |
| 2017 | 189 (94.5) | 11 (5.5) | |
| 2018 | 187 (93.5) | 13 (6.5) | |
| Overall | 948 (94.8) | 52 (5.2) | |
Primary Return of Spontaneous Circulation and Survival to Discharge Rates of CPR a
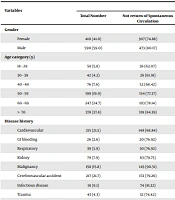
Gender was not an effective factor in the primary success of CPR (P = 0.054), while there was a significant relationship among cases’ age groups and primary survival based on chi square test (P < 0.001). That is, the highest ROSC of CPR was in age range 30 - 39 years (38.09%) and the lowest rate was in age group above 70 years old (15.06%). The highest success rate of CPR based on background diseases were with poisoning (32%), cardiac diseases (31.16%), and trauma (25.58%) and the lowest rate was with malignance (9.49%). In addition, the history of cardiac ischemic disorders did not have a significant relationship with primary success (P = 0.0586). The success rate in patients without ischemic background disorder (23.41%) was higher than that of the patient with a history of ischemia (18.34%). The first rhythms observed following cardiopulmonary arrest after connecting monitoring were asystole (44.5%), fibrillation/pulseless ventricular tachycardia (15.5%), bradycardia (32.5%), and pulseless electrical activity (7.5%). Among the noted rhythms, the highest chance of ROSC was with VF/VT rhythms (47.74%). Chi square test showed a significant relationship between the type of cardiac rhythm, shockable rhythms (VF/VT) in particular and ROSC (P < 0.001). The highest rate of ROSC was observed between 8 am and 12 am (32.11%) and the lowest rate was observed between 4 am and 8 am (8.24%). Chi square test showed a significant relationship between work shift and ROSC (P < 0.001). Totally, 867 patients had cardiac arrest with witness whether monitoring device or presence of health personnel and 133 had cardiac arrest without witness and received CPR in out-going wards. The rate of success of CPR in the patients with witness (23.41%) was notably higher that those without witness (12.78%) (P < 0.001). In terms of the place of cardiac arrest, emergency wards were at the top (25.8%), followed by ICUs (25.7%), and internal wards (10.7%) (Table 2).
| Variables | Results of CPR | |||
|---|---|---|---|---|
| Total Number | Not return of Spontaneous Circulation | Return of Spontaneous Circulation | Statistical Test (P) | |
| Gender | 0.054 | |||
| Female | 410 (41.0) | 307 (74.88) | 103 (25.12) | |
| Male | 590 (59.0) | 473 (80.17) | 117 (19.83) | |
| Age category (y) | < 0.001* | |||
| 18 - 29 | 58 (5.8) | 36 (62.07) | 22 (37.93) | |
| 30 - 39 | 42 (4.2) | 26 (61.91) | 16 (38.09) | |
| 40 - 49 | 76 (7.6) | 52 (68.42) | 24 (31.58) | |
| 50 - 59 | 199 (19.9) | 154 (77.37) | 45 (22.61) | |
| 60 - 69 | 247 (24.7) | 193 (78.14) | 54 (21.86) | |
| > 70 | 378 (37.8) | 319 (84.39) | 159 (15.6) | |
| Disease history | N/A | |||
| Cardiovascular | 215 (21.5) | 148 (68.84) | 67 (31.16) | |
| GI bleeding | 26 (2.6) | 20 (76.92) | 6 (23.08) | |
| Respiratory | 39 (3.9) | 30 (76.92) | 9 (23.08) | |
| Kidney | 79 (7.9) | 63 (79.75) | 16 (20.25) | |
| Malignancy | 158 (15.8) | 143 (90.51) | 15 (9.49) | |
| Cerebrovascular accident | 217 (21.7) | 172 (79.26) | 45 (20.74) | |
| Infectious disease | 91 (9.1) | 74 (81.32) | 17 (18.68) | |
| Trauma | 43 (4.3) | 32 (74.42) | 11 (25.58) | |
| Surgery | 76 (7.6) | 57 (75.0) | 19 (25.0) | |
| Poisoning | 25 (2.5) | 17 (68.0) | 8 (32.0) | |
| Diabetes complications | 31 (3.1) | 24 (77.42) | 7 (22.58) | |
| Diabetes history | 0.632 | |||
| Yes | 231 (23.1) | 184 (79.65) | 47 (20.35) | |
| No | 769 (76.9) | 596 (77.5) | 173 (22.5) | |
| Hypertension history | 0.65 | |||
| Yes | 483 (48.3) | 375 (77.66) | 108 (22.36) | |
| No | 517 (51.7) | 405 (77.36) | 112 (21.66) | |
| Ischemic heart disease history | 0.058 | |||
| Yes | 278 (27.8) | 227 (81.66) | 51 (18.36) | |
| No | 722 (72.2) | 553 (76.59) | 169 (23.4) | |
| Primary rhythm | < 0.001* | |||
| VT/VF | 155 (15.5) | 81 (52.26) | 74 (47.74) | |
| Asystole | 445 (44.5) | 369 (82.92) | 76 (17.08) | |
| Bradycardia | 325 (32.5) | 261 (80.31) | 64 (19.89) | |
| PEA | 75 (7.5) | 69 (92.0) | 6 (8.0) | |
| CPR time in 24 hours | < 0.001* | |||
| 8 - 12 | 218 (21.8) | 148 (67.89) | 70 (32.11) | |
| 12 - 16 | 125 (12.5) | 95 (76.0) | 30 (24.0) | |
| 16 - 20 | 155 (15.5) | 112 (72.26) | 43 (27.74) | |
| 20 - 24 | 163 (16.3) | 125 (76.69) | 38 (23.3) | |
| 24 - 4 | 157 (15.7) | 133 (84.71) | 24 (15.29) | |
| 4 - 8 | 182 (18.2) | 167 (91.76) | 15 (8.24) | |
| Cardiac arrest type | < 0.001* | |||
| Witness | 867 (86.7) | 664 (76.59) | 203 (23.41) | |
| Non-witness | 133 (13.3) | 116 (87.22) | 17 (12.78) | |
| CPR ward | N/A | |||
| Emergency | 258 (25.8) | 193 (74.80) | 65 (25.20) | |
| Surgery | 75 (7.5) | 57 (76.0) | 18 (24.0) | |
| Internal | 107 (10.7) | 89 (83.18) | 18 (16.82) | |
| ICU | 257 (25.7) | 198 (77.04) | 59 (22.96) | |
| CCU | 74 (7.4) | 55 (74.32) | 19 (25.68) | |
| Infection | 83 (8.3) | 67 (80.72) | 16 (19.28) | |
| Oncology | 11 (1.1) | 10 (90.91) | 1 (9.1) | |
| Orthopedic | 15 (1.5) | 11 (73.33) | 4 (26.67) | |
| Neurology | 103 (10.3) | 87 (84.47) | 16 (15.53) | |
| Dialysis | 9 (0.9) | 7 (77.78) | 2 (22.22) | |
| Para clinics | 8 (0.8) | 6 (75.0) | 2 (25.0) | |
Relationship Between ROSC with Some Contextual Variables a
Table 3 lists the results of logistic regression with regard to identifying the factors in the ROSC. There was a significant relationship between the ROSC and Primary rhythm, female gender, CPR between 8 am and 12 am, CPR between 4pm and 8pm, and cardiopulmonary arrest (CPA) with witness.
| Variables | B | SE | EXP (B) | P Value |
|---|---|---|---|---|
| Gender (female) | 1.029 | 0.389 | 1.73 | 0.041 |
| Age (< 50 years) | 1.632 | 0.73 | 2.84 | 0.03 |
| Primary rhythm (VF/VT) | 3.13 | 0.421 | 12.73 | 0.001 |
| CPR time (8 - 12) | 4.30 | 0.721 | 6.55 | 0.003 |
| CPR time (16 - 20) | 3.55 | 1.03 | 2.78 | 0.02 |
| Cardiac arrest type (witness) | 1.53 | 0.56 | 2.56 | 0.001 |
The Variables Affect ROSC
There was no significant relationship between gender and STD (P = 0.073); however, there was a relationship between age groups and STD (P < 0.001). That is, with an increase in age, a tangible decrease happens in STD rate. The highest STD was observed with patients diagnosed with poisoning (20%) and the lowest rate of STD was with patients with malignancy (1.90%). History of diabetes, hypertension, and cardiac ischemic disorders did not have a relationship with STD. However, the primary rhythm was an effective factor in STD (P = 0.026) so that the highest STD was observed with VT/VF rhythm (9.03%). There was no significant relationship between time of CPR and STD; while type of CPA (witnessed/not witnessed) had a significant relationship with STD (P = 0.031). Additionally, prolongation of CPR was an effective factor in STD so that STD decreased with an increase in CPR duration (P < 0.001). Post-CPR dysrhythmia had a significant relationship with STD (P = 0.012); so that patients without dysrhythmia had the highest STD rate. Moreover, patients with higher consciousness level after CPR had a higher STD rate so that 70.59% of patients with consciousness level 12 - 15 (Glasgow Coma Scale) leaved the hospital alive (P < 0.001) (Table 4).
| Variables | Results of CPR | |||
|---|---|---|---|---|
| Total Number | Not survival to Discharge | Survival to Discharge | Statistical Test (P) | |
| Gender | 0.073 | |||
| Female | 410 (41.0) | 387(94.39) | 23 (5.61) | |
| Male | 590 (59.0) | 561 (95.08) | 29 (4.92) | |
| Age category (y) | < 0.001* | |||
| 18 - 29 | 58 (5.8) | 51 (87.93) | 7 (12.07) | |
| 30 - 39 | 42 (4.2) | 37 (88.10) | 5 (11.90) | |
| 40 - 49 | 76 (7.6) | 69 (90.79) | 7 (9.21) | |
| 50 - 59 | 199 (19.9) | 185 (92.96) | 14 (7.04) | |
| 60 - 69 | 247 (24.7) | 239 (96.76) | 8 (3.24) | |
| > 70 | 378 (37.8) | 367 (97.09) | 11 (2.91) | |
| Disease history | N/A | |||
| Cardiovascular | 215 (21.5) | 201 (93.49) | 14 (6.51) | |
| GI bleeding | 26 (2.6) | 24 (92.31) | 2 (7.69) | |
| Respiratory | 39 (3.9) | 37 (94.87) | 2 (5.13) | |
| Kidney | 79 (7.9) | 76 (96.20) | 3 (3.80) | |
| Malignancy | 158 (15.8) | 55 (98.10) | 3 (1.90) | |
| Cerebrovascular accident | 217 (21.7) | 208 (95.85) | 9 (4.15) | |
| Infectious disease | 91 (9.1) | 87 (95.60) | 4 (4.40) | |
| Trauma | 43 (4.3) | 40 (93.02) | 3 (6.98) | |
| Surgery | 76 (7.6) | 71 (93.42) | 5 (6.58) | |
| Poisoning | 25 (2.5) | 20 (80.0) | 5 (20.0) | |
| Diabetes complications | 31 (3.1) | 29 (93.55) | 2 (6.45) | |
| Diabetes history | 0.076 | |||
| Yes | 231 (23.1) | 218 (94.37) | 13 (5.63) | |
| No | 769 (76.9) | 730 (94.93) | 39 (5.07) | |
| Hypertension history | 0.066 | |||
| Yes | 483 (48.3) | 460 (95.24) | 23 (4.76) | |
| No | 517 (51.7) | 488 (94.39) | 29 (5.61) | |
| Ischemic heart disease history | 0.052 | |||
| Yes | 278 (27.8) | 267 (96.04) | 11 (96.7) | |
| no | 722 (72.2) | 681 (94.32) | 41 (5.68) | |
| Primary rhythm | 0.026* | |||
| VT/VF | 155 (15.5) | 141 (90.97) | 14 (9.03) | |
| Asystole | 445 (44.5) | 424 (95.28) | 21 (4.72) | |
| Bradycardia | 325 (32.5) | 310 (95.38) | 15 (4.62) | |
| PEA | 75 (7.5) | 73 (97.33) | 2 (2.66) | |
| CPR time in 24 hours | 0.596 | |||
| 8 - 12 | 218 (21.8) | 205 (94.04) | 13 (5.96) | |
| 12 - 16 | 125 (12.5) | 119 (95.2) | 6 (4.8) | |
| 16 - 20 | 155 (15.5) | 146 (94.19) | 9 (5.81) | |
| 20 - 24 | 163 (16.3) | 153 (93.87) | 10 (6.13) | |
| 24 - 4 | 157 (15.7) | 150 (95.54) | 7 (4.46) | |
| 4 - 8 | 182 (18.2) | 175 (96.15) | 7 (3.85) | |
| Cardiac arrest type | 0.031* | |||
| Witness | 867 (86.7) | 819 (94.46) | 48 (5.54) | |
| Non-witness | 133 (13.3) | 129 (96.99) | 4 (3.01) | |
| CPR ward | N/A | |||
| Emergency | 258 (25.8) | 243 (94.19) | 15 (5.81) | |
| Surgery | 75 (7.5) | 70 (93.33) | 5 (6.67) | |
| Internal | 107 (10.7) | 101 (94.39) | 6 (5.6) | |
| ICU | 257 (25.7) | 247 (96.11) | 10 (3.89) | |
| CCU | 74 (7.4) | 70 (94.59) | 4 (5.4) | |
| Infection | 83 (8.3) | 79 (95.18) | 4 (4.82) | |
| Oncology | 11 (1.1) | 11 (100) | 0 (0) | |
| Orthopedic | 15 (1.5) | 14 (93.33) | 1 (6.67) | |
| Neurology | 103 (10.3) | 98 (95.15) | 5 (4.85) | |
| Dialysis | 9 (0.9) | 8 (88.89) | 1 (11.11) | |
| Para clinics | 8 (0.8) | 7 (87.5) | 1 (12.5) | |
| CPR time (min) | < 0.001* | |||
| < 10 | 53 (5.3) | 28 (52.83) | 25 (47.17) | |
| 10 - 20 | 33 (3.3) | 24 (72.73) | 9 (27.27 | |
| 20 - 30 | 87 (8.7) | 79 (90.80) | 8 (9.20) | |
| > 30 | 827 (82.7) | 817 (98.79) | 10 (1.21) | |
| Dysrhythmia after CPR | 0.012* | |||
| Supraventricular | 79 (35.91) | 61 (77.22) | 18 (22.78) | |
| Ventricular | 45 (20.45) | 38 (84.44) | 7 (15.56) | |
| Non-dysrhythmia | 96 (43.64) | 69 (71.87) | 27 (28.13) | |
| GCS after CPR | < 0.001* | |||
| 3 - 7 | 117 (53.18) | 99 (84.62) | 18 (15.38) | |
| 8 - 11 | 86 (39.09) | 64 (74.42) | 22 (25.58) | |
| 12 - 15 | 17 (7.73) | 5 (29.41) | 12 (70.59) | |
The Factors Related with Survival to Discharge a
Table 5 lists the factors effective in STD; age, CPR duration, post-CPR consciousness level, primary rhythm, and type of cardiac arrest (witness /no witness) are the predictors of STD after ROSC.
| Variables | B | SE | EXP (B) | P Value |
|---|---|---|---|---|
| Age | 1.095 | 0.376 | 2.99 | 0.022 |
| CPR time duration | 1.736 | 0.891 | 12.6 | 0.001 |
| GCS after CPR | 2.095 | 0.473 | 10.73 | 0.001 |
| Primary rhythm | 2.736 | 1.021 | 3.466 | 0.012 |
| Cardiac arrest type (witness) | 2.639 | 0.389 | 17.25 | 0.031 |
The Variables Affect Survival to Discharge
Table 6 lists different CPC levels of patients at discharge. According to Fisher’s exact test, only post-CPR GSC and CPR duration had a significant relationship with CPC (P < 0.001) so that 70.59% of patient with post-CPR GCS level of 12 - 15 and 37.21% of the patients with CPR duration below 20 min left the hospital at a favorable level of CPC (CPC1-2). Also, 82.69% of discharged patients had favorable neurological status.
| Variables | No. (%) |
|---|---|
| CPC 1 | 27 (51.92) |
| CPC 2 | 16 (30.77) |
| CPC 3-5 | 9 (17.3) |
The Cerebral Performance Categories (CPC) Throughout Discharge
5. Discussion
Totally, 22% of CPR cases led to ROSC of 30min or higher. Shao et al. reported a post-CPR ROSC of 35.5% and the difference in the results can be explained based on background diseases and lower age average of the samples (27). A prospective multi-center study in 13 hospitals in seven provinces in China by Hu et al. reported post-CPR ROSC equal to 37.3% (28). This difference in the results might be explained by different study environments so that Hu et al.’s study was limited to emergency department and our study covered all hospital wards. Primary success of CPRs in Nolan et al. in the UK was 45%. They reported that primary return was defined as 20min ROSC at least and they had a different study population, which can explain the difference in the findings (29). Goodarzi et al. conducted a prospective cohort study between 2012 and 2013 on 320 CPR cases in Kermanshah and reported the ROSC of CPRs equal to 15.3% (7), which is lower than the five-year average reported here. The significant increase in success rate of CPR between 2014 and 2018 indicates an improvement of ROSC after IHCA in Kermanshah. This change can be explained by better educations about using CPR guideline (2015), higher experience of physicians and personnel with CPR and 24/7 presence of emergency medicine specialists in the educational-medical centers under study.
The STD over the five years under study was 5.2%. A prospective observational study (2015) in Sant Olav University Hospital in Norway between January 2009 and August 2013 showed that 25% of CPR patient survived to discharge (30). One reason for the difference in the findings in this regard can be the primary rhythm in the patient so that they reported that 53% of the cases had a shockable primary rhythm. In addition, a systematic meta-analysis study from January 1990 to December 2016 reported STD in the studies under study equal to 8% and the cases were limited to the patient with cerebral veins diseases under CPR (24). Salari et al. and Goodarzi et al. reported STD in Iran equal to 7.2% and 10.6% respectively (7, 23). The low STD level in the mentioned studies compared to other studies like (7), can be explained by different inclusion criteria. Lack of a significant difference (P = 0.631) in terms of STD between 2014 and 2018 supports the fact that STD rate has not changed over the past decade (31, 32). The increase of awareness about optimizing clinical care after CPR and new studies on the causes can lead to better results in the future (2).
By taking into account the intervening variables in Logistic Regression test, female gender, age < 50-year, VF/VT cardiac dysrhythmia, CPR between 8am and 12am, CPR between 16pm and 20pm, and type cardiac arrest (witness) had a significant relationship with the primary result of CPR – i.e., the effective factors in the primary result of CPR.
Several studies have reported a higher successful CPR rate in morning shifts compared to overnight shifts (7, 23, 29). The low success rate of resuscitation following IHCA during overnight shifts might be due to tiredness of personnel, less readiness, understaffed overnight shifts, and slower response speed overnight (7, 33).
In addition, consistent with the present study, other studies like Shao et al. and Movahedi et al. reported that gender had a direct relationship with ROSC so that this rate was higher in women than men (27, 34). Finding such a relationship might be due to the number of samples and different male/female ratio in the sample groups. For instance, Adamski et al. reported results different from our results (22). At any rate, male gender is a risk factor for cardiac patients and the less chance of successful CPR in male gender is reported in several studies (7, 34). The relationship between younger age and primary survival after CPR was also consistent with Shao et al. for patients under 60 years old and Nolan et al. (27, 29). Salari et al. reported that the primary success of CPR in patients below 60 years old was notably higher (23). Chen et al. conducted a study in Taiwan and concluded that younger patients received longer CPRs (3). Meaney et al. reported that asystole was the most common rhythm and the frequency of VF/VT shockable rhythms was 24% (35). Bergum et al. reported that only 28% of the cases of first observed rhythms were shockable VF/VT cardiac rhythm (30). Shao et al. and Nolan et al. reported results consistent with the present study so that the highest arrhythmia was asystole. In addition, ROSC was higher in the case of shockable rhythms and there was a significant relationship between Shockable rhythms and ROSC (27, 29). The wide consistency of the results by different studies indicates that shockable rhythms is a good prognosis of CPR.
The ROSC rates with witnessed and non - witness were 23.41% and 12.78% respectively. These findings are consistent with Salari et al. (23). Identification of this factor as an effective factor in ROSC shows a better chance of response and shockability of the heart in the early moments of cardiac arrest and the initiation of CPR.
The highest success rate was with cardiac arrest due to poisoning (32%) and cardiac failures (31.16%) and the lowest success rate was with malignancy (9.49%) and infectious diseases (18.68%). Bergum et al. reported the ROSC for cardiac problems equal to 30%, which is consistent with our results (30). The findings indicate that background diseases that involve several organs like malignancy and sepsis have a lower chance of successful CPR, which is consistent with other studies (7, 23, 36).
Logistic regression analysis showed that age < 50 years, primary rhythm, CPR duration, GCS, and arrest with witness or under monitoring had a significant relationship with STD. Therefore, these factors are predictors of STD.
Consistent with our findings, Salari et al. reported that none of the patients older 60 years old left hospital alive after CPR (23). In addition, based on multiple regression test, Shao et al. found a significant relationship between age < 60 years and survival rate of patients after CPR (27). Movahedi et al. did not found a significant relationship between age and STD; still, they showed that individuals with 24hrs survival after CPR were younger that the patient who did not survived 24hrs after CPR (34). Other studies have also mentioned patient’s age as an effective factor in survival of patients after CPR (7, 29, 37).
The STD was significantly higher with VF/VT shockable rhythms compared with non-Shockable rhythms. Meaney et al. reported consistent results with ours (35). Bergum et al. reported that 53% of cases with shockable rhythms resulted in STD, which indicates good prognosis of such rhythms for resuscitation (30). Hirlekar et al. also reported consistent results in this area (38). A study found that STD was notably higher with shockable rhythms compared with non-shockable rhythms and there was a significant relationship between the primary cardiac rhythm and shockability of rhythm and final result of CPR (23). There are reliable evidences for the higher survival chance after cardiac arrest with a shockable rhythm when a defibrillator is used immediately after cardiac arrest. Despite no changes of the STD of asystole patients with pulseless electrical activity over the past decades, there has been a notable increase in the STD of patients with shockable rhythms. This might be due to sensitivity of these rhythms to cardiac shock and return to normal rhythm when cardiac shock is implemented in a timely manner (30).
Logistic regression test indicated that CPR duration was an effective factor in STD. The CPR duration in 82.7% of the cases was more than 30 min; and Chi square test indicated that there was a significant relationship between CPR longer or shorter than 30min and STD (P < 0.001). Miranzadeh et al. reported that CPR duration was a key predictor factor of survival (33). Consistently, Bansal et al. concluded that CPR duration shorter or longer than 10 min was a key factor in predicting success and STD (8). What is clear from the present and other studies is that the shorter the CPR duration the higher the chance of STD (3).
The largest number of resuscitated patients in this study (53.18%) had a GCS of 3 - 7. The results showed a significant relationship between consciousness level after CPR and STD so that 70.59% of the patients with STD had a GCS of 12 - 15. Logistic regression test showed that post-CPR GCS was a predicting factor of STD in patients. There are a few studies in this area; that were reported similar results about Glasgow scale’s predicting value for STD after CPR (39, 40).
The STD rate in cardiac arrests with witness or under monitoring was 5.54% and this rate for cardiac arrest non - witness was 3.01%. The logistic regression test showed a significant relationship between cardiac arrest with witness and STD. Salari et al. showed that none of the patients with cardiac arrest without witness survived to discharge (23). Herlitz et al. showed that STD after CPR is doubled when CPR initiates within one minute after cardiac arrest compared with CPR initiated after one minute (41)
In addition, 82.69% of CPR patients with CPC1-2 survived to discharge. In general, CPC1-2 is considered as suitable and independent neurologic status (38). Wittayachamnankul et al. showed that after implementation of advance CPR course, 82.60% of the discharged patients had a favorable neurological status (9). Inconsistent with Yukawa et al., only 13.92% of STD patients had a favorable neurological status (42). The difference can be rooted in the type and background of the study (42) that OHCA patients were under study.
Moreover, 70.59% of the CPR patients with post-CPR GCS of 12 - 15 and 37.21% of the patients with CPR duration of less than 20min had CPC1-2 at discharge. According to Fisher’s exact test, GCS after CPR and CPR duration had a significant relationship with CPC (P < 0.001). Two studies reported similar findings about GCS level and neurological outcomes after CPR (39, 42).
Caltekin et al. studied IHAC and OHAC cases and found a significant relationship between good neurological status in patients with CPR duration < 20 min (P = 0.007). However, only 23.3% of patients with a CPR duration < 20 min had a good neurological status, which is less than what was found here (10). Some similar studies have also listed the factors effective in good neurological status after successful CPR for IHCA cases; which shows that CPR duration is effective in good neurological status at discharge after CPR (22, 43).
5.1. limitations
The study has some limitations, in some cases, the status of patients' CPC during discharge was not specified in the patients' medical records, so we tried to take the information by calling the patient or families via the phone number written in the electronic records. However, we believe this study is more generable due to random sampling and high sample size.
5.2. Conclusions
Despite the improvement in the CPR outcomes compared to previous studies in Kermanshah City, the short-term outcomes and STD after CPR were not in a desirable condition. However, the favorable neurological outcome was an indicative of good care services after successful CPRs. This finding can be a motivation for the medical personnel in doing a better CPR operation. Given the potential of health centers in Kermanshah City, codification and implementation of routine educational programs and improvement of the quality of these services, surveying the quality of CPR and cares afterwards, and supplying the equipment needed for giving feedbacks during a cardiopulmonary resuscitation procedure can lead to an improvement of CPR outcomes.