1. Background
The health expenditure of the gross domestic product (GDP) trend in the world and in Iran is increasing steadily (1, 2). In 2000, 4.7% of Iran's GDP was devoted to the health sector, while it reached 8.1% in 2016 (1). In addition, healthcare expenditures or direct medical costs in the world are on the rise, which is considered to be a major challenge for health policymakers (3, 4). In addition, non-medical costs have intensified the challenge through increasing out-of-pocket patient costs (5).
In general, patients incur the three categories of direct, indirect, and intangible costs in receiving healthcare services (6), and some of these costs are paid out-of-pocket. Notably, out-of-pocket payments are classified as direct costs, which refer to the costs of diagnostic and treatment processes (7, 8). Direct costs could be medical and non-medical; direct medical costs include the payments for disease diagnosis and treatment, patient admission, prescriptions, follow-ups, hospitalization, and rehabilitation (9, 10); in official statements, direct medical costs are expressed as healthcare expenditures. These costs are partly paid by insurance systems and partly by patients (5). Direct non-medical costs refer to the costs that patients must pay for access to medical services; such examples are medical commuting and transportation costs, accommodation costs, food costs or the phone charges required for setting appointments. These costs are also classified as out-of-pocket payments (11).
Out-of-pocket payment is the most inefficient and unfair approach to healthcare financing, which leads to the increased rate of poverty (12). In low- and middle-income countries, the main source of healthcare financing is the out-of-pocket payments of patients, which cause catastrophic health expenditures (CHEs) in households (13, 14). In these countries, the financing of the health system is poor and causes numerous households to sell their assets or borrow money to pay for healthcare expenditure (15, 16). Approximately 150 million experience financial stress each year due to the out-of-pocket expenditures for healthcare services, while 100 million face poverty (17, 18).
The share of out-of-pocket payments of the total costs in health care and CHEs are important factors to be considered in healthcare planning and policymaking (19, 20). Iran is a middle-income country (21), and the financing of the Iranian health system covers a combination of public income, social insurance, private insurance, and out-of-pocket payments (22). According to the most recent global report in this regard, the rate of out-of-pocket health expenditures in Iran was 38.79% in 2016 (23). Meanwhile, the average out-of-pocket payment in the world and OECD countries is 18.5% and 20.2%, respectively (24, 25). In 2000-2015 in the eastern Mediterranean region, almost half of the health expenditures were financed by out-of-pocket payments (21). Therefore, it could be inferred that the out-of-pocket payments of the health expenditures in Iran are higher than the world and OECD average.
2. Objectives
The present study aimed to determine the risk of catastrophic health expenditures due to non-medical costs in the outpatients in Qazvin, Iran.
3. Methods
This cross-sectional survey was conducted on the outpatients and caregivers referring to the internists of Bu-Ali Sina and Velayat teaching hospitals in Qazvin, Iran. The study protocol was approved by the Research Ethics Committee of Qazvin University of Medical Sciences (code: IR-QUMS.REC.1396.20).
The sample size of the study was estimated using the Cochran formula based on the trend of the previous year (26). Based on statistical formulations, the sample size was determined to be 341 outpatients. The patients were selected via cluster sampling, and data were collected via sample rotation within one month (December 22, 2017-January 22, 2018) with a one-month recall period. Finally, 341 outpatients were randomly selected from those referring to the mentioned healthcare centers.
Data were collected using a researcher-made questionnaire and by the observation of the prescriptions of the selected patients. Initially, the validity of the questionnaire was confirmed by health service management professionals and physicians. Prior to data collection, a questionnaire was distributed among 30 outpatients in a pilot study, and the required data were collected after removing the defects.
Unlike family-centered studies, the current research was conducted from the perspective of the outpatients. The expenses that had been paid directly by the patients and their caregivers to receive health services were calculated and considered as out-of-pocket payment. Initially, the out-of-pocket expenditures of the patients and their caregivers were identified. The outpatient out-of-pocket expenditures included the out-of-pocket payments covering direct medical costs (costs of physician visits, medications, and laboratory or diagnostic tests) and non-medical costs (costs of transportation, residence, and food), which were paid by the patients and their caregivers. Notably, the share of insurance payments was excluded in the identification of the mentioned costs. In the present study, several steps were followed to determine whether the out-of-pocket payment costs could be catastrophic. One of the approaches that is applied to determine the threshold of CHEs is to calculate the ratio of out-of-pocket payments to the total income. In general, the reported thresholds in different studies are within the range of 2.5 - 15% (27).
Considering that Iran is a middle-income country (28), a threshold of 5% was set to determine whether payments were out-of-pocket for patients. The currency conversions were carried our based on the official exchange rate of December 22, 2017 (1$=34,214 Iranian Rials) (29).
3.1. Statistical Analysis
Data analysis was initially performed in Excel 2013 and SPSS version 21 using mean, median, and standard deviation. In addition, graphs and ratios were prepared.
4. Results
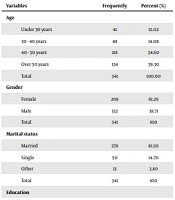
In total, 341 outpatients referring to the internal medicine clinics of Velayat Hospital and Bu-Ali Sina Hospital in Qazvin in 2017 were enrolled in the study. The mean age of the patients was 47.8 ± 13.7 years, and the highest and the lowest frequencies belonged to the age groups of 40-50 years (34.6%) and < 20 years (0.9%), respectively. The majority of the patients were female (61.3%) and married (81.5%). In terms of education level, the patients without a high school diploma had the highest frequency (67.7%). In addition, the majority of the examined outpatients were housewives (41.9%), and self-employed patients had the lowest frequency (2.3%). Approximately 89.5% of the patients had social security and health insurance coverage; among the insured patients, social security was most common, while Imam Khomeini Relief Foundation had the lowest frequency. Table 1 shows the demographic characteristics of the examined patients.
| Variables | Frequently | Percent (%) |
|---|---|---|
| Age | ||
| Under 30 years | 41 | 12.02 |
| 30 - 40 years | 48 | 14.08 |
| 40 - 50 years | 118 | 34.60 |
| Over 50 years | 134 | 39.30 |
| Total | 341 | 100.00 |
| Gender | ||
| Female | 209 | 61.29 |
| Male | 132 | 38.71 |
| Total | 341 | 100 |
| Marital status | ||
| Married | 278 | 81.50 |
| Single | 50 | 14.70 |
| Other | 13 | 3.80 |
| Total | 341 | 100 |
| Education | ||
| Diploma & Under diploma | 293 | 85.92 |
| Associate | 24 | 7.04 |
| Licentiates and above | 24 | 7 |
| Total | 341 | 100 |
| Occupational status | ||
| Housewives | 143 | 41.94 |
| Retired/ pensioner | 23 | 6.74 |
| Employee | 18 | 5 |
| Unable | 14 | 4.11 |
| Self-employed | 8 | 2.35 |
| Others | 135 | 39.59 |
| Total | 341 | 100 |
| Insurance | ||
| Social security | 177 | 52 |
| Health insurance | 128 | 37.54 |
| Armed forces | 12 | 3.52 |
| Others | 24 | 7.04 |
| Total | 341 | 100 |
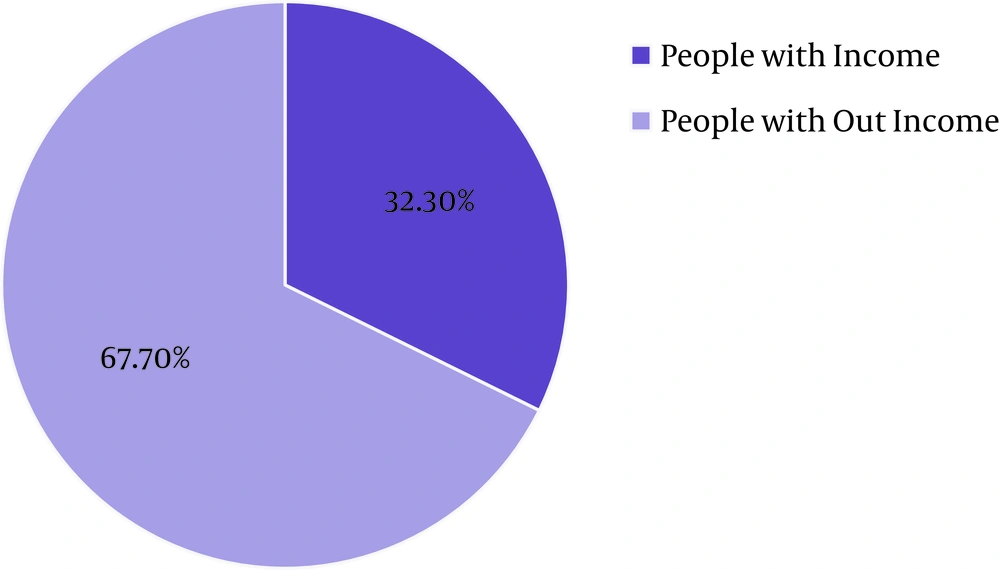
According to the information in Table 2 and Figure 1, the majority of the examined patients (67.7%) had no income.
| Income | Mean | Median | Standard Deviation |
|---|---|---|---|
| USD | 159.29 | 0 | 248.14 |
| Rls | 5,450,000 | 0 | 8,490,000 |
Table 3 shows the mean income of the outpatients with income.
| Income | Mean | Median | Standard Deviation |
|---|---|---|---|
| USD | 493.8 | 467.64 | 159.53 |
| Rls | 16,894,540 | 16,000,000 | 5,458,290 |
The direct expenditure of the studied patients encompassed both medical and non-medical costs. The mean out-of-pocket spending of the patients for direct medical and non-medical costs was estimated at 38 and 12 dollars, respectively, while the mean out-of-pocket spending of the patients for direct costs was 50 dollars. Therefore, it could be inferred that the out-of-pocket payment of the patients for direct medical costs constituted 75.8% of the total out-of-pocket payments for the direct costs. In other words, the out-of-pocket payments for the direct medical costs (receiving medical services and treatments) was higher in the present study. The mean direct costs represented the patients’ mean out-of-pocket payments incured for the patients by themselves or their caregivers (Table 4).
| Direct Costs | Mean | Median | Standard Deviation | OOP Ratio of Direct Costs |
|---|---|---|---|---|
| Medical | 75.8 | |||
| USD | 38 | 28 | 33 | |
| Rls | 1,300,000 | 960,000 | 1,120,000 | |
| Non-medical | 24.2 | |||
| USD | 12 | 6 | 21 | |
| Rls | 410,000 | 200,000 | 720,000 | |
| Total | 100 | |||
| USD | 50 | 34 | 54 | |
| Rls | 1,710,000 | 1,160,000 | 1,840,000 |
Table 5 shows the details of the out-of-pocket payments of the patients for direct medical services, such as physician visits, medications, and diagnostic/laboratory tests. According to the findings, the mean out-of-pocket payments for these costs were estimated at 1.98, 10.8, and 25.13 dollars, respectively. Meanwhile, the highest out-of-pocket payment belonged to diagnostic/laboratory test expenditures (50.3%).
Direct non-medical costs included transportation, residence, and food of the patients and their caregivers, which were calculated to be 9.06, 0.78, and 2.19 dollars, respectively. In other words, the transportation costs had the highest share (18.2%) of the out-of-pocket payments for the direct non-medical costs. In addition, the sum of the direct costs represented the total out-of-pocket payments of the patients and their caregivers.
| Direct costs | Parameters | Mean | Median | Standard Deviation | OOP Ratio of Direct Costs |
|---|---|---|---|---|---|
| Medical | Visit | 4 | |||
| USD | 1.987 | 1.228 | 1.052 | ||
| Rls | 68,000 | 42,000 | 36,000 | ||
| Drug | 21.5 | ||||
| USD | 10.814 | 8.768 | 11.399 | ||
| Rls | 370,000 | 300,000 | 390,000 | ||
| Laboratory & diagnostic tests | 50.3 | ||||
| USD | 25.136 | 21.336 | 27.182 | ||
| Rls | 860,000 | 730,000 | 930,000 | ||
| Non-medical | Transportation | 18.2 | |||
| USD | 9.061 | 4.676 | 13.737 | ||
| Rls | 310,000 | 160,000 | 470,000 | ||
| Reside | 1.5 | ||||
| USD | 0.789 | - | 5.553 | ||
| Rls | 27,000 | - | 190,000 | ||
| Food | 4.5 | ||||
| USD | 2.192 | - | 5.846 | ||
| Rls | 75,000 | - | 200,000 | ||
| Total | 100 | ||||
| Total direct costs | USD | 49.980 | 36.535 | 43.842 | |
| Rls | 1,710,000 | 1,250,000 | 1,500,000 |
Finally, the total out-of-pocket payment of the studied outpatients was estimated at 49.97 dollars, and the highest out-of-pocket payments were for diagnostic/laboratory tests, medications, and transportation costs.
| Without Non-Medical Costs | With Non- Medical Costs | |
|---|---|---|
| Mean of total sample income | X =38/159.29 = 0.23 | X = 50/159.29 = 0.31 |
| Mean of patients with income | X = 38/493.8 = 0.076 | X = 50/493.8 = 0.10 |
The ratio of the out-of-pocket payments to the income of the patients was also calculated, and it was determined whether the patients’ out-of-pocket payments were catastrophic. As mentioned earlier, the threshold of the CHEs was set at 5%. According to the obtained results, the rate of exposure to CHEs was 31%, and the ratio of the out-of-pocket payments to the income of the patients with income was 10%. (Table 6)
5. Discussion
In the current research, the mean out-of-pocket payment per outpatient was calculated within a one-month period based on the share of the direct medical and non-medical costs using a novel approach. The main difference of our study with similar studies is that due to the shift in the perspective of the family unit from multidimensional families to individuals across various countries, costs and incomes are calculated per person rather than on a household basis. In order to meet the research objectives, questions were addressed regarding the out-of-pocket payments for direct medical and non-medical costs, rate of patients’ exposure to CHEs, and impact of direct non-medical costs on the patients’ exposure to CHEs.
According to statistics, the costs of out-of-pocket health expenditures in Iran was more than twice the global average in 2016 (23). In official statements, out-of-pocket expenditures generally represent patients’ out-of-pocket payments for receiving diagnostic and treatment procedures. In addition to direct medical costs, direct non-medical costs are thoroughly paid by patients or their caregivers, which significantly increase patients’ out-of-pocket payments (5).
In the current research, the out-of-pocket payments of the patients were calculated contrary to the traditional approach and most of the similar studies considering the out-of-pocket payments for direct medical and non-medical costs. According to the obtained results, the out-of-pocket direct medical costs constituted a major share compared to the non-medical costs. Consistently, Bahmei et al. also reported that direct medical costs were higher than direct non-medical costs (30), whereas Wagner et al. stated that direct non-medical costs were higher than direct medical costs (31). The main caused of increased direct medical costs has been shown to be the higher costs of diagnostic tests compared to other costs. In a study by the WHO, most out-of-pocket payments were for the costs of medication (32). Some of the discrepancies in this regard could be attributed to the differences in the sample populations (inpatient/outpatient), type of diseases, study design, and items considered in the classification of direct medical and non-medical costs. Most findings have confirmed that the share of direct medical costs is higher than non-medical costs, while these categories of costs cannot have the same share in healthcare expenditures. Therefore, further investigations are required.
According to the results of the present study regarding direct non-medical costs, commuting costs were observed to be higher than other costs. In the study by Powel et al., direct non-medical costs were reported to be lower than direct medical costs. Furthermore, the results of the mentioned study indicated that commuting costs were higher than the costs of accommodation and food (33). Therefore, it could be inferred that patients must pay out of their pockets for transportation services to reach their medical center of choice and may overlook their other essential needs (e.g., food) as they are forced to pay for direct non-medical costs. Notably, access to healthcare services is an important issue in the discussion of direct non-medical costs since the availability of more services decreases these costs. Moreover, these costs may vary in the case of inpatients.
According to the results of the present study, the patients' out-of-pocket payments were catastrophic in different situations. A large portion of the patients' income was reported to be allocated to health services and treatment, thereby leading to CHEs. In addition, the patients with no income were more likely to experience CHEs. In fact, direct medical costs caused 23% of all the examined patients and 8% of the patients with income to face CHEs.
The findings of the current research demonstrated that the out-of-pocket payments for direct non-medical costs (costs of medical transportation, accommodation, and food) increased the CHEs by up to 8%. In line with this finding, Shrime et al. also confirmed the effects of direct non-medical costs on the exposure of patients to CHEs (34). On the other hand, Anderz et al. did not consider direct non-medical costs in the calculation of CHEs (35).
Direct medical costs (i.e., healthcare costs) are the 'tip of the iceberg' when it comes to the costs of medical services imposed on patients. In contrast, direct non-medical costs may be invisible to health care policymakers and decision-makers. Depending on the type of diseases and patient conditions, direct non-medical costs may be large or small, while non-medical costs increase the out-of-pocket payments, thereby increasing the CHEs.
Although all the patients were covered by insurance in the present study, they still had out-of-pocket payments for healthcare services. Therefore, it could be concluded that insurances have literally failed to cover the needs and costs of patients. In fact, insurance services must adequately and fully cover a wide range of the medical needs of their clients. Furthermore, the high costs and poor performance of supplementary insurances may be the reasons behind patients’ lack of interest in purchasing these services. According to Zhang et al., the shallow coverage of outpatient care is a major issue in the healthcare system (36). Although private and public insurance covers more than 90% of Iranians, studies have shown that more than 50% of health expenditures are paid out-of-pocket (22).
5.1. Limitations of the Study
- The impossibility of patient follow-up and lack of accurate data on their costs; to resolve this issue, the patients' recent prescriptions were reviewed, and if a drug or test was prescribed and cost information was not available, the cost would be extracted based on the prescriptions.
- In all cost studies, there is a reminder bias or a reminder error, which cannot be reduced to zero. By designing appropriate questions, categorizing questions, consulting professors about designing the questions, detailing the questions, asking and interviewing the patients, and viewing the patients' prescriptions, we attempted to minimize the reminder bias.
5.2. Recommendations
- Calculation of out-of-pocket payments by dividing direct (medical and non-medical) and indirect costs using the same method in the patients with different diseases (inpatient and outpatient) in diverse geographical areas to determine the dominate share of each cost;
- It is recommended that similar studies be performed on both public and private sectors for the comparison of the results.
- It is recommended that similar studies be performed on the elderly and housewives who do not have income and are in a more vulnerable position when it comes to CHEs.
- Due to the individualistic view of family relations, it is recommended that individuals be examined rather than families for the reconsideration of CHE-related approaches.
5.3. Conclusion
Considering the national policy concerning the shift from inpatient services to outpatient services, it is anticipated that high out-of-pocket payments will cause severe issue for both the health system and patients in the coming years. Moreover, the high direct medical costs that are paid by outpatients out of their pockets require strong and coherent policies for the determination of the patients’ share. With the occurrence of illnesses, patients incur direct and indirect medical costs. Therefore, policymakers and decision-makers must consider direct non-medical and medical costs since direct non-medical costs add to the overall out-of-pocket payment of patients and increase the risk of CHEs.