1. Background
Cancer is the leading cause of death in developed countries and the second cause in developing countries (1). About 12.7 million new cancer cases are diagnosed yearly, 56% of whom occur in low- and middle-income countries (1-3). In addition, a significant number of these cancer cases involve children. In general, about 160,000 new cases of cancer in the world are diagnosed in children under 15 years old (3).
Cancer has socio-economic and psycho-social effects on children and their families (3), whose basic needs should be considered to achieve sustainable support for children with cancer and their parents (3-5). These needs and challenges include inadequate access to relevant information, stress, lack of financial resources to meet health needs, and inadequate nutrition (4).
International studies have shown the high prevalence of dental caries among children with cancer, and the most common dental treatments include preventive and restorative measures and removal of infectious foci (6). Poor oral hygiene can complicate oncology treatment and negatively affect the child’s health. Odontogenic infections can lead to widespread fatal infection in children undergoing chemotherapy or bone marrow transplantation (7).
Dental examination, treatment, and preventive measures, including removal of all potential sources of infection and counseling of the patient’s parents about prevention, should be performed before the onset of immunosuppressive periods as a result of chemotherapy treatment. This program should also be followed during treatment (8, 9). Parents of children with cancer need to be educated about the need for primary oral and dental care during treatment to prevent or at least reduce long-term complications (10).
Recently, the guidelines of the Multinational Association for Supportive Care in Cancer/International Society of Oral Oncology (MASCC/ISOO) indicate that the best way and the essential prescription is to prevent or manage oral mucositis, as the most common complication of treating these patients (11, 12).
Treating these patients requires a multidisciplinary team that includes a pediatric oncologist/hematologist, pediatrician, nutritionist, nurses, pediatric dentist, social workers, and the child’s parents. Proper communication with them should be ensured to improve the quality of care provided to the child (9, 13).
Parents of these patients are very conservative and usually do not follow a strict protocol. The parents’ primary concerns are the children’s illness and systemic health, so they focus on oral and dental hygiene and a healthy diet. These children also use drugs containing sucrose and high-calorie food supplements to increase energy levels, which can increase caries (14, 15).
Following a basic oral care strategy will prevent subsequent infections and bacteremia, which reduces the possibility of pain in the structures of the mouth and teeth as well as the side effects of chemotherapy on the soft tissue of the mouth and the duration of hospitalization and improves the quality of life and care provided to children undergoing chemotherapy (14).
Very limited studies have assessed parents’ awareness, attitudes, and oral healthcare practices regarding their child during chemotherapy and immunosuppression. Parents’ awareness and attitude affect their children’s oral and dental health, which will significantly impact the primary oral and dental health measures during chemotherapy and immunosuppression.
2. Objectives
The main goal of the current study was to determine the awareness and performance of parents of children with cancer regarding their oral and dental health.
3. Methods
This descriptive-analytical epidemiological study was conducted on parents of 3-13-year-old healthy and cancerous children in Ahvaz, Iran. This study was conducted after obtaining permission from the Ethics Committee of Ahvaz Dental School (IR.AJUMS.REC.1401.299) in the fall of 2022. The study population included parents with cancer and healthy children. Parents with cancer children (case group) were selected from those referred to the specialized oncology clinic of Shafa Hospital in Ahvaz. In addition, parents with healthy children (control group) were randomly selected from among those who referred to the children’s department of Ahvaz Dental School or other clinics and offices in the Ahvaz.
The study objectives were explained to the children's legal guardians, who participated in the study after obtaining consent. Exclusion criteria included age under three years, older than 13 years, and lack of consent from the child’s parents.
Due to the limited number of referrals to the specialized oncology clinic, the census method was used by the parents of all cancer children who had previously agreed to participate in the study (n = 110). Then, the control group was randomly selected with the same number as the case group (n = 110).
In this study, a researcher-made questionnaire was used as a measurement tool, which was designed based on Gupta et al. (16). The content validity of the questionnaire was confirmed by the qualitative method by experts, and the reliability of the questionnaire was evaluated by the test-retest method (agreement coefficient = 0.72). The questionnaire consisted of three parts, including demographic information, knowledge questions, and performance questions about oral and dental hygiene. In the demographic section, information about age, gender, place of residence, and parents’ education was collected. The awareness section consisted of ten questions based on which a score of one was assigned to the "correct" answer and zero to the "incorrect/I don’t know" answer. Therefore, the range of awareness scores is in the range of 0 to 10. The final part of the questionnaire contained eight questions about the evaluation of parents’ performance, which were in the form of two-choice questions: "yes" and "no." Finally, the results of this part are expressed as percentages.
SPSS software version 24 was used for data analysis. Calculating the average and variance of the awareness and performance scores was used to describe the data. In the following, the Kolmogorov-Smirnov test was utilized to evaluate the normality of the distribution of the studied variables, and the t-test of independent groups (or in the non-parametric mode, the Mann-Whitney U test) was used for the inferential analysis of the awareness and performance scores between the two groups. Pearson’s correlation coefficient and regression analysis were applied to evaluate the relationship between awareness level and performance. This study considered the significance level of P < 0.05 for all statistical tests.
4. Results
Out of 220 parents studied, 105 (47.7%) had male, and 115 (52.3%) had female children, and the average age in both studied groups was approximately seven years. Considering the necessity of homogenizing the samples selected from the two studied groups, the results showed no significant difference between the two groups regarding the average age distribution of children (Table 1). The results showed a significant difference between the two groups regarding awareness in some of them (Table 2). In addition, the results showed that the level of awareness of people in different dimensions was not the same, and the highest awareness score was related to the question "the best means of oral and dental hygiene," and 91.4% of the studied people answered this question correctly. In addition, the lowest awareness was related to the question "the most important time to clean the teeth" when only 25% of people chose the correct answer to this question.
| Groups | No. | Mean ± SD | Min | Max | T | P-Value |
|---|---|---|---|---|---|---|
| Healthy children | 110 | 7.155 ± 2.16 | 3 | 14 | 0.370 | 0.712 |
| Children with cancer | 110 | 7.018 ± 3.21 | 3 | 15 | ||
| Total | 220 | 7.086 ± 2.73 | 3 | 15 | - | - |
| Question and Groups | Option"A" | Option "B" | Option"C" | Option "D" | Correct Answer |
|---|---|---|---|---|---|
| 1. The leading cause of tooth decay? | |||||
| Options | Sweet and sticky material | Fruits and vegetables | Dairy products | I do not know | |
| Healthy | 86 (78.2) | 0 (0) | 0 (0) | 24 (21.8) | 86 (78.2) |
| Cancer | 97 (88.2) | 0 (0) | 1 (0.9) | 12 (10.9) | 97 (88.2) |
| 2. The best tool for maintaining oral health? | |||||
| Options | Toothbrush and dental floss | Mouthwash | Chewing gum | I do not know | Correct answer |
| Healthy | 102 (92.7) | 6(5.5) | 0 (0) | 2 (1.8) | 102 (92.7) |
| Cancer | 99 (90) | 9 (8.2) | 1 (0.9) | 1 (0.9) | 99 (90) |
| 3. The best tool to clean between the teeth? | |||||
| Options | Toothbrush | Dental floss | Toothpick | I do not know | Correct answer |
| Healthy | 20 (18.2) | 90 (81.8) | 0 (0) | 0 (0) | 90 (81.8) |
| Cancer | 34 (30.9) | 67 (60.9) | 8 (7.3) | 1 (0.9) | 67 (60.9) |
| 4. The most crucial time to clean teeth? | |||||
| Options | Before going to bed at night | After every meal | After breakfast | I do not know | Correct answer |
| Healthy | 35 (31.8) | 50 (45.5) | 22 (20) | 3 (2.7) | 35 (31.8) |
| Cancer | 20 (18.2) | 87 (79.1) | 0 (0) | 3 (2.7) | 20 (18.2) |
| 5. The proper time to change the toothbrush? | |||||
| Options | Three months | One year | Six months | I do not know | Correct answer |
| Healthy | 72 (65.55) | 1 (0.9) | 31 (28.2) | 6 (5.5) | 72 (65.55) |
| Cancer | 65 (59.1) | 3 (2.7) | 27 (24.5) | 15 (13.6) | 65 (59.1) |
| 6. Probability of caries after frequent consumption of sweet snacks between meals? | |||||
| Options | Yes | No | I do not know | - | Correct answer |
| Healthy | 91 (82.7) | 2 (1.8) | 17 (15.5) | - | 91 (82.7) |
| Cancer | 83 (75.5) | 4 (3.6) | 23 (20.9) | - | 83 (75.5) |
| 7. Does cancer affect gum health? | |||||
| Options | Yes | No | I do not know | - | Correct answer |
| Healthy | 39 (35.5) | 5 (4.5) | 66 (60) | - | 39 (35.5) |
| Cancer | 49 (44.5) | 6 (5.5) | 55 (50) | - | 49 (44.5) |
| 8. Do cancer treatment drugs affect patients’ gum health? | |||||
| Options | Yes | No | I do not know | - | Correct answer |
| Healthy | 20 (18.2) | 3 (2.7) | 87 (79.1) | - | 20 (18.2) |
| Cancer | 38 (34.5) | 18 (16.4) | 54 (49.1) | - | 38 (34.5) |
| 9. Is compliance with oral and dental health during cancer treatment effective during the disease? | |||||
| Options | Yes | No | I do not know | - | Correct answer |
| Healthy | 39 (35.5) | 5 (4.5) | 66 (60) | - | 39 (35.5) |
| Cancer | 51 (46.4) | 14 (12.7) | 45 (40.9) | - | 51 (46.4) |
| 10. Does fluoridated toothpaste help keep teeth healthier? | |||||
| Options | Yes | No | I do not know | - | Correct answer |
| Healthy | 82 (74.5) | 5 (4.5) | 23 (20.9) | - | 82 (74.5) |
| Cancer | 58 (52.7) | 9 (8.2) | 43 (39.1) | - | 58 (52.7) |
a Values are expressed as No. (%).
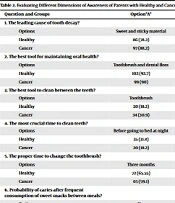
The results related to the awareness section showed that the average awareness score of parents of healthy children was 5.96 (out of 10) and 5.70 (out of 10) for parents of cancer children. Parents of healthy children had higher levels of awareness of oral and dental health, but no significant differences were observed between healthy children and cancer children (P = 0.313) (Table 3). The results related to measuring the practice of the studied parents regarding compliance with oral and dental health and the effects associated with the frequency of respondents related to each question were presented in Table 4. The results showed a significant difference between parents of healthy and cancer children in all areas except the answer to the question "Have you ever received nutrition advice from a pediatrician or nutritionist?" regarding "practice." The results of parents’ practice showed that the average practice score of parents of healthy children was equal to 4.26 (out of 8) and 2.97 (out of 8) for parents of cancer children. The parents of healthy children had higher levels of performance compared to parents of cancer children regarding oral and dental health, and this difference was significant (P < 0.001) (Table 5).
| Groups | No. | Mean ± SD | Median | Min | Max | P-Value |
|---|---|---|---|---|---|---|
| Parents of healthy children | 110 | 5.96 ± 1.88 | 6 | 1 | 10 | 0.313 |
| Parents of cancer children | 110 | 5.70 ± 1.92 | 6 | 1 | 9 |
| Question and Parents Groups | Yes | No | Chi-square Statistic | P-Value |
|---|---|---|---|---|
| 1. Does your child brush their teeth day and night? | 4.02 | 0.045 b | ||
| Healthy | 88 (80) | 22 (20) | ||
| Cancer | 75 (68.2) | 35 (31.8) | ||
| 2. Do you have a history of using fluoride for your child? | 4 | 0.045 b | ||
| Healthy | 35 (31.8) | 75 (68.2) | ||
| Cancer | 22 (20) | 88 (80) | ||
| 3. Do you do periodic dental examinations of your child? | 26.69 | <0.001 b | ||
| Healthy | 81 (73.6) | 29 (26.4) | ||
| Cancer | 43 (39.1) | 67 (60.9) | ||
| 4. Do you follow the preventive recommendations of the treatment staff? | 14.47 | <0.001 b | ||
| Healthy | 93 (84.5) | 17 (15.5) | ||
| Cancer | 68 (61.8) | 42 (38.2) | ||
| 5. Does your child frequently use snacks and sweet drinks between main meals? | 10.66 | 0.001 c | ||
| Healthy | 14 (12.7) | 96 (87.3) | ||
| Cancer | 34 (30.9) | 76 (69.1) | ||
| 6. Have you ever received nutritional advice from a pediatrician or nutritionist? | 2.20 | 0.138 | ||
| Healthy | 27 (24.5) | 83 (75.5) | ||
| Cancer | 37 (33.6) | 73 (66.4) | ||
| 7. Have you taken your child to the dentist for examination/follow-up treatment? | 43.75 | 0.001 c | ||
| Healthy | 77 (70) | 33 (30) | ||
| Cancer | 28 (25.5) | 82 (74.5) | ||
| 8. Did you follow your child’s oral care instructions during or after treatment? | 23.54 | 0.001 c | ||
| Healthy | 54 (49.1) | 56 (50.9) | ||
| Cancer | 20 (18.2) | 90 (81.8) |
a Values are expressed as No. (%).
b There is a significant difference at α = 0.05.
c There is a significant difference at α = 0.01.
| Groups | No. | Mean ± SD | Median | Min | Max | Mann-Whitney U Test | P-Value |
|---|---|---|---|---|---|---|---|
| Parents of healthy children | 110 | 4.26 ± 1.43 | 4 | 1 | 7 | 6.046 | < 0.001 |
| Parents of cancer children | 110 | 2.97 ± 1.69 | 3 | 0 | 8 |
5. Discussion
This study evaluated the level of awareness and practice of parents of cancer and healthy children regarding oral and dental health. The results showed that the parents’ awareness of the control group was higher than the case group, but this difference was insignificant. Three of the ten questions on awareness dealt with cancer or drugs used to treat it on the health of teeth and gums. Parents of children with cancer had more awareness than the control group in all three questions. However, more education and information should be provided to parents due to parents’ lack of information about the effect of the disease itself or the drugs used.
The most significant percentage difference in answering the awareness questions was related to "the best tool for cleaning between the teeth" (81% of the control and 60% of the study group). Therefore, according to the results and the high prevalence of interdental caries among children, the parents of children with cancer should be given the necessary training for correctly and regularly using dental floss to prevent interdental caries.
The lowest percentage of correct answers among the questions related to essential brushing time for the child was 31.8% for the control and 18.2% for the case group. As saliva secretion decreases during the night, the cleansing property of saliva, which is considered the essential property of saliva, also decreases, and the risk of caries increases. Therefore, the most crucial time to brush teeth should be after eating at night and before the child sleeps. Following this principle can effectively reduce caries and improve children’s oral health.
In questions related to practice, parents of healthy children had better practice than parents of cancer children, which was even significant. Special attention should be paid to the education of the parents of these children regarding oral and dental health instructions considering dental and gum problems in children with cancer, the impact of the disease and the drugs used for the mouth and teeth of these children, and the importance of maintaining oral health.
About 75% of children in the cancer group brush their teeth during the day and night, while this rate was 88% for children in the control group, which was statistically significant. Gupta et al. compared the performance of parents of children undergoing chemotherapy regarding oral and dental health. The amount of brushing of children with cancer was similar to that of the present study, and 74% of them brushed their teeth during the day and night (16). This rate was reported as much as 66.2% in Alkhuwaiter (17), but there was no control group in the mentioned study, and the sample size was smaller than in the present study.
Evaluation of parents’ practice showed that the practice index in cases of history of fluoride use, periodical dental examinations, following preventive recommendations, dental visits, and carrying out oral health care instructions in the parents of children with cancer was significantly lower than the control group.
Only 25.5% of children with cancer have ever had a dental visit. Ali and Nurelhuda reported that almost all children with leukemia (93.1%) never experienced a dental visit during their lifetime. Since most of the mothers in the present study were illiterate, the low percentage of dental visits can result from parents’ lack of awareness in this field (18). Gupta et al. also indicated that only 87% of parents of Indian patients took their children to a dental visit (16). Based on Pedrosa et al., 41.1% of children with cancer have never visited a dentist. Among the people who had a dental consultation, only 16% of the consultations were for preventive treatment (19).
The use of snacks and sweet drinks between main meals in children with cancer was significantly more than in healthy children. In addition, the rate of receiving nutritional advice from pediatricians or nutritionists in the group of children with cancer was higher than that of healthy children, but this rate was insignificant.
5.1. Limitations
The limitation of this study was that children with the same socio-economic status and children with similar oral and dental health status were not compared. In addition, more studies should be conducted with a larger sample size and similar oral health guidelines. In addition, some studies need to be performed to separate different types of cancer in children because different kinds of cancer may have different effects on oral and dental lesions and, subsequently, on oral and dental hygiene.
5.2. Conclusions
Based on the results, the awareness and practice of the parents of children with cancer is insufficient regarding their children’s oral and dental health, probably due to the lack of education and information to the parents. Increasing parents’ information about children’s oral health through educational classes, dental and nutritional counseling sessions, brochures, and pamphlets is possible. In addition, children with cancer should be referred to the dentist based on a coherent and regular schedule for preventive and therapeutic measures.