1. Context
Transcranial electrical stimulation (tES) is a non-invasive brain-stimulating method, which involves sending a small amount of electricity via the scalp to the brain to influence the processing of the underlying cortical regions. In recent years, numerous studies have demonstrated that tES might be a highly effective method for enhancing cognitive abilities in language acquisition, memory retention, focus, and mental computation (1-3). Combining tES with mental stimulation and other approaches to improve cognition is a relatively recent innovation (4-7). The most common tES protocols include “transcranial direct current stimulation” (tDCS), “transcranial alternating current stimulation” (tACS), “transcranial pulsed current stimulation” (tPCS), and “transcranial random noise stimulation” (tRNS) (8).
Transcranial electrical stimulation is performed through two or more rubber electrodes placed on the scalp; thus, a conductive material such as gel or sponge soaked in salt solution is used. The electrodes are linked to a battery-operated generator that allows the user to control the stimulation's period and electrical level. The place or places of stimulation can be determined using the international Electroencephalography placement system of 10 - 20 points, or electric field modeling can be used (9). The active electrode is often attached to the target area, and the return electrode is placed on the opposite area above the eye socket or somewhere other than the head, such as the shoulder.
Over the past decade, there has been a meteoric rise in the number of specialists interested in tES as a potential supplementary or alternative method for treating mental health issues. Transcranial direct current stimulation is one of the most widely used tES protocols. Transcranial direct current stimulation consists of an anodic (positively charged) electrode and a cathodic (negatively charged) electrode to determine the effects of stimulation. Transcranial direct current stimulation involves the application of a steady flow of direct electrical current to the brain tissue via the electrodes to regulate the activity level of the neurons located beneath the electrodes. The anode is the entry point of the current into the body, whereas the cathode is the exit point from the body (10). Research on the motor cortex in animals has revealed that tDCS applied anodally enhances excitability while transcranial direct current stimulation applied cathodally lowers neuronal activity (11).
Transcranial direct current stimulation can induce enduring modifications in the cerebral cortex that persist beyond the stimulation period. The period of physiological reactions following stimulation is based upon the intensity and duration of current flow. Applying electrical current to the motor cortex leads to more robust and longer-lasting effects regarding motor-evoked potentials (MEP) when the intensity or duration of stimulation is increased (11-13). The typical current intensity used for tDCS to produce lasting effects is between 0.5 and 2 mA (1), and usual tDCS montages last for 10 to 20 minutes (14). This study aimed to review the effectiveness of tDCS for the treatment of various mental disorders, considering the importance of using tDCS for the treatment of mental illnesses.
2. Evidence Acquisition
This review is a narrative review performed using the results of previous relevant studies from 2000 to 2023. Relevant mesh terms were used in valid international databases, including Web of Science, Science Direct, Scopus, PubMed, and Google Scholar. Medical subject headings (MeSH) terms for searching include “transcranial electrical stimulation,” “transcranial direct current stimulation,” “(tDCS),” “non-invasive brain,” “mental disorders,” “psychiatric disorders,” “electroencephalography,” “transcranial magnetic stimulation,” “electric therapy” “autism spectrum disorder,” “obsessive-compulsive disorder,” “attention deficit hyperactivity disorder,” “social anxiety disorder,” “panic disorder,” “generalized anxiety disorder,” “fear circuit,” “trait anxiety,” “substance use disorder,” “major depressive disorder,” “dementia,” “working memory” and other similar words. Inclusion criteria were the use of tDCS exclusively for treating various psychiatric disorders. The results of 25 similar previous studies were finally used after considering the inclusion and exclusion criteria out of the 55 studies received. Treatment methods, including “transcranial alternating current stimulation” (tACS), “transcranial pulsed current stimulation” (tPCS), and “transcranial random noise stimulation” (tRNS), were excluded. In addition, studies with low sample sizes (such as case reports) and studies published in non-authoritative journals were excluded.
3. Results
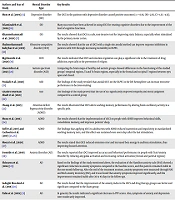
The effectiveness of tDCS for treating various mental disorders, including depressive disorder, obsessive-compulsive disorder (OCD), autism spectrum disorder (ASD), attention deficit hyperactivity disorder (ADHD), and anxiety disorders are shown in Table 1.
| Authors and Year of Study | Mental Disorder Type | Key Results |
|---|---|---|
| Mutz et al. (2019) (15) | Depressive disorder (DD) | The tDCS in the patients with depressive disorder caused positive outcomes (α = 0.95, OR = 2.65, CI = 1.55 - 4.55). |
| Eslamizadeh et al. (2016) (16) | DD | Many successes have been achieved in using tDCS for treating cognitive disorders due to the improvement of the level of cognitive functions. |
| Khanmohammadi et al. (2020) (17) | DD | The results showed that tDCS is a safe, non-invasive tool for improving static balance, especially when stimulated by the primary motor cortex. |
| Shahmohammadi Kaleybar et al. (2019) (18) | Obsessive-compulsive disorder (OCD) | The results showed that the use of tDCS with a single-site anodal method can improve response inhibition in patients with OCD through increasing excitability in DLPFC. |
| Rigi Kooteh et al. (2020) (19) | OCD | The results indicated that tDCS and emotion regulation can play a significant role in the treatment of drug addiction, especially in the prevention of relapse. |
| Ghoreishi et al. (2021) (20) | Autism spectrum disorder (ASD) | Comparing the brain maps of healthy and autistic groups showed differences in the functioning of the studied groups' temporal regions, T3 and T4 brain regions, especially in the frontal and occipital T regions between eyes open and closed. |
| Pouladi et al. (2020) (21) | ASD | The findings of the study revealed that anodal tDCS on the DLPFC in the left hemisphere can increase executive performance in decision-making |
| Ghadiri Sourman Abadi et al. (2021) (22) | ASD | The findings of the study proved that the use of tES significantly improved empathy and moral judgment compared to a control group |
| Chang et al. (2015) (23) | Attention deficit hyperactivity disorder (ADHD) | The results illustrated that tDCS alters working memory performance by altering brain oscillatory activity in a specific pole. |
| Munz et al. (2015) (24) | ADHD | The results showed that the implementation of tDCS on people with ADHD improves behavioral skills, consolidates memory, and improves patients' sleep. |
| Soff et al. (2017) and Cachoeira et al. (2017) (25, 26) | ADHD | The findings that applying tDCS to adolescents with ADHD reduced inattention and impulsivity in standardized working memory tests, and this effect was sustained even seven days after the last stimulation. |
| Moezzi et al. (2020) (27) | ADHD | The results stated that tDCS reduced omission error and increased beta energy in auditory stimulation, thus improving focused attention. |
| Ironside et al. (2019) (28) | Anxiety disorders (AD) | The results reported that tDCS improved accuracy and behavioral performance in people with Trait Anxiety Disorder by reducing amygdala activation and increasing cortical activation (frontal and parietal regions) |
| Shiozawa et al. (2014) (29) | AD | Based on the findings of the study mentioned above, the evaluation of the Hamilton anxiety scale (HAS) showed a significant reduction in anxiety symptoms compared to the baseline scores, and this pattern remained stable in the one-month follow-up. After the end of the treatment sessions, anxiety symptoms were measured through HAS and Beck anxiety inventory (BAI), and it was found that anxiety symptoms improved significantly, and this improvement remained stable after 30 to 45 days in the follow-ups. |
| Sadeghi Movahed et al. (2018) (30) | AD | The results found that the improvement of the anxiety index in the tDCS and drug therapy groups was better and significant compared to the Sham group |
| Palm et al. (2019) (31) | AD | In general, the results indicated a significant decrease in PPV scores. Also, symptoms of anxiety and depression were moderately improved. |
| Vafaye Sisakht and Ramezani (2017) (32) | AD | The results expressed that tDCS in the R-DLPFC region improved the mental health of veterans, and their psychological problems were resolved after treatment sessions. |
| Amini and Vaezmousavi (2021) (33) | AD | The results showed that tDCS is related to optimizing the performance of athletes in three effectiveness systems, including cognitive, psychological, and physiological performance. |
| Sarhadi et al. (2019) (34) | AD | The findings that combined treatment, including sertraline and tDCS, as an efficient and effective method in reducing the symptoms of post-traumatic stress disorder in veterans have significant effects. |
| Rigi Kooteh et al. (2019) (35) | AD | The findings showed that both tDCS and emotion regulation training had significant and long-term effects on reducing the desire to use drugs and fantasizing about drug use in drug-dependent patients. |
3.1. Depressive Disorder
It is estimated that depression affects > 300 million individuals worldwide, with an annual occurrence rate of 6.6% and a lifetime occurrence rate of 16.2% (36). This disorder has been introduced as the third essential cause of disability worldwide (37), and 15% of cases are associated with suicidal ideation and attempted suicide (38). Transcranial direct current stimulation uses anode stimulation on the left dorsolateral prefrontal cortex (L-DLPFC). Therefore, its purpose is to deal with the hypoactivity of this brain region and the subsequent hyperactivity in the brain's default mode network (39). Transcranial direct current stimulation elicits enduring alterations in neuronal plasticity via “N-Methyl-D-aspartate receptor-mediated pathways,” equal to the processes of long-term -potentiation and -depression (40). Further, tDCS has been linked to alterations in neurotransmitter levels (e.g., “serotonin” and “dopamine”) and the activity of vessels and astrocytes by affecting ion channels in the cell membrane and resulting in the redistribution of neurochemicals (41, 42). Mutz et al. compared the effectiveness and acceptability of brain stimulation without surgery for the treatment of major depressive disorder in adults and showed that tDCS in these patients caused positive outcomes (α = 0.95, OR = 2.65, CI = 1.55-4.55) (15). Eslamizadeh et al. reported many successes in using tDCS for treating cognitive disorders due to improving the level of cognitive functions (16). Moreover, Khanmohammadi et al. showed that tDCS is a safe, non-invasive tool to improve static balance, especially when the primary motor cortex is stimulated (17).
3.2. Obsessive-Compulsive Disorder
Obsessive-compulsive disorder is a mental disorder in which a person repeatedly experiences specific thoughts (called obsessions) or feels the need to repeatedly perform specific actions (called compulsions), leading to distress or disturbance in the person's general functioning (43). Many studies, including neuropsychological function, structural-functional neuroimaging, and also therapeutic studies, have implicated the potential role of functional disorder of neural circuits in OCD. In addition, abnormalities of the cortical-subcortical circuit of the brain have been introduced as one of the prominent abnormalities of physiology pathology in OCD (44). Obsessive-compulsive disorder is considered a chronic and debilitating mental disorder with an estimated lifetime prevalence of 1 - 3% (45, 46), which accounts for approximately 2.5% of all disabilities worldwide and is among the top 20 leading causes of disease-related disability in people aged 15 - 44 years (47). According to the present search, the number of studies related to the application of tDCS for treating OCD is very limited. Overall, three studies have stimulated the dorsolateral prefrontal cortex (DLPFC), and the sample size of these studies is too small to discuss their effectiveness (48-50). However, the studies mentioned above have indicated that using different stimulation parameters, such as anodal and cathodal stimulation of the L-DLPFC and bilateral stimulation of the DLPFC, significantly improved OCD symptoms (48-50). Similar to transcranial magnetic stimulation (TMS) studies, the role of tDCS targeting the DLPFC is limited to reducing anxiety and accompanying depressive symptoms (51). Shahmohammadi Kaleybar et al. showed that using tDCS with a single-site anodal method can improve response inhibition in patients with OCD through increasing excitability in DLPFC (18). In addition, Rigi Kooteh et al. reported that tDCS and emotion regulation can play a critical role in treating drug addiction, especially in relapse prevention (19).
3.3. Autism Spectrum Disorder
Autism spectrum disorder is a complicated neurological condition that has become increasingly prevalent. In addition, ASD is marked by lifelong impairments in communication and interactions and restricted and repeated behavior habits. Typically, these difficulties substantially disrupt an individual's daily activities early in the developmental stage (52). A variety of cognitive and verbal disabilities, sensory abnormalities, and behavioral symptoms characterize ASD. The exact causes and mechanisms behind ASD are not yet fully understood, but some suggested factors include the brain being more effective on the right side, an imbalance between inhibitory and excitatory processes, abnormal connections within the brain, changes in developing synaptic connections, and dysfunction in the mirror neuron system (53).
There is no specific treatment for ASD, but non-invasive brain stimulation interventions, particularly tDCS, have become increasingly popular in recent years due to their ease of use. So far, tDCS has only been marginally and inconsistently used for patients with ASD (54). Some studies on the use of tDCS for ASD treatment have shown that this therapeutic technique improves social cognition (55, 56), executive functions (57, 58), verbal skills (59), and stereotyped behaviors of ASD patients (60, 61). Ghoreishi et al. showed that between eyes open and eyes closed by comparing the brain maps of healthy and autistic groups, and there are differences in the functioning of the temporal regions, T3 and T4 brain regions of the studied groups, especially in the frontal and occipital T regions (20). Pouladi et al. showed that anodal tDCS on the DLPFC in the left hemisphere can increase executive performance in decision-making (21). Ghadiri Sourman Abadi et al. reported that using tES significantly improved empathy and moral judgment compared to a control group (22).
3.4. Attention Deficit Hyperactivity Disorder
Attention deficit hyperactivity disorder is a disorder of neural development, which can be identified by symptoms of disinterest, excessive levels of hyperactivity, and impulsivity that are not acceptable for the individual's maturity. In addition, ADHD prevalence in childhood is 7%, and it is often associated with other disorders such as stubbornness-disobedience, Tourette syndrome, anxiety, and mood disorders (62). Drug treatment of ADHD is mainly performed by stimulant drugs (for example, methylphenidate), serotonin reuptake inhibitors, and norepinephrine (atomoxetine). This type of treatment can worsen the patient's condition in some situations, which can induce adverse reactions, including a reduced desire to eat, sleep disturbances, migraines, nausea, and impaired maturation. Consequently, there is a substantial requirement for innovative techniques in ADHD treatment. As tDCS is known to enhance cognitive abilities like awareness and memory, it could be an effective therapeutic method. The initial investigation examined the impact of tDCS on the ability to consciously recall information in individuals diagnosed with ADHD (63, 64). Transcranial direct current stimulation is a neurological treatment technique that introduces a direct and weak current to cortical areas and facilitates or inhibits spontaneous neural activity (65). Chang et al. found that tDCS alters working memory performance by changing brain oscillatory activity in a specific pole (23). Munz et al. concluded that implementing tDCS in people with ADHD improves behavioral skills, consolidates memory, and improves patients' sleep (24). Soff et al. and Cachoeira et al. reported that applying tDCS to adolescents with ADHD reduced inattention and impulsivity in standardized working memory tests, which was sustained even seven days after the last stimulation (25, 26). Overall, the analyzed data from the studies showed that tDCS has the potential to decrease symptoms ADHD symptoms and enhance mental processes in individuals diagnosed with ADHD. Moezzi et al. stated that tDCS reduces omission error and increases beta energy in auditory stimulation, thus improving focused attention (27).
3.5. Anxiety Disorders
Maladaptive neural plasticity is one of the essential pathological mechanisms affecting anxiety disorders (66). Transcranial direct current stimulation may be a valuable tool to counter patterns of maladaptive neuroplasticity with pathological hypoactivity/hyperactivity modulation of the DLPFC in relevant clinical populations (28, 67). Ironside et al. showed that tDCS improved accuracy and behavioral performance in people with trait anxiety disorder by reducing amygdala activation and increasing cortical activation (frontal and parietal regions) (28). In Shiozawa et al., a middle-aged woman received a course of 10 stimulation meetings administered once daily, five times per week, over two weeks. The stimulation involved the application of cathodal stimulation with an intensity of 2 mA to the right dorsolateral prefrontal cortex (R-DLPFC). Based on the findings, the Hamilton Anxiety Scale (HAS) evaluation indicated a notable decrease in anxiety symptoms compared to the initial scores. This reduction in anxiety symptoms remained consistent during the one-month follow-up period (29). Shiozawa et al. conducted the first case study on the application of tDCS to a middle-aged woman with generalized anxiety disorder. Cathodal electrical stimulation was performed for 15 consecutive sessions daily on R-DLPFC. The anode was also placed on the deltoid muscle of the opposite shoulder, and the stimulation intensity was equal to 2 mA. After the end of the treatment sessions, anxiety symptoms were measured through HAS and Beck Anxiety Inventory (BAI), and it was found that anxiety symptoms improved significantly, and this improvement remained stable after 30 to 45 days in the follow-ups (29). In Sadeghi Movahed et al., 18 patients with generalized anxiety disorder were randomly divided into three groups. The first group (6 people) was exposed to tDCS with 2 mA cathodal conditions on R-DLPFC, the second group was treated with medication (6 people), and the third group was exposed to Sham stimulation (6 people). Next, the anxiety symptoms of all three groups were measured by HAS in the pre-test and post-test steps. The results of the mentioned study showed that the anxiety index improvement in the tDCS and drug therapy groups was better and significant compared to the Sham group (30). Palm et al. examined eight pilots suffering from paroxysmal positional vertigo (PPV) who were exposed to tDCS to modulate the symptoms related to the disease (dizziness/numbness) by this method. Anodal electrical stimulation with 2 mA was applied on R-DLPFC daily for five consecutive days to perform the mentioned study. In general, the obtained results showed a significant decrease in PPV scores. Furthermore, symptoms of anxiety and depression were moderately improved (31). Vafaye Sisakht and Ramezani reported that tDCS in the R-DLPFC region improved veterans' mental health, and their psychological problems were resolved after treatment sessions (32). Amini and Vaezmousavi showed that tDCS is related to optimizing the performance of athletes in three effective systems, including cognitive, psychological, and physiological performance (33). Sarhadi et al. indicated that combined treatment, including sertraline and tDCS, as an efficient and effective method of reducing the symptoms of post-traumatic stress disorder in veterans has significant effects (34). Rigi Kooteh et al. found that both tDCS and emotion regulation training had significant and long-term impacts on reducing the desire to use drugs and fantasizing about drug use in drug-dependent patients. In other words, combined treatment can significantly reduce the desire to use drugs in drug addicts, and starting treatment with emotion regulation training followed by tDCS can lead to better results (35).
4. Conclusions
Based on the findings, tDCS was adequate for the treatment of various mental disorders, including depressive disorder, obsessive-compulsive disorder, autism spectrum disorder, attention deficit hyperactivity disorder, and anxiety disorders. In addition, tDCS could improve the symptoms of each of the aforementioned mental disorders. Limited studies have been conducted to evaluate the effectiveness of tDCS for some mental disorders. Therefore, the results of some studies need to be reassessed to achieve reassuring conclusions.