1. Background
Vulvovaginal candidiasis (VVC) is a common vaginal infection among reproductive-aged women, and at least 70 - 75% of women experience this infection once in their life (1). The condition mainly results from Candida albicans, but other yeast species may also cause vaginitis (2). According to Narayankhedkar, vaginal candidiasis is the most prevalent infection among reproductive-aged women (3). Various factors influence the risk of VVC, including age, hygienic habits, a history of the disease, and immune system activity (4).
The most bothersome signs and symptoms of vaginal candidiasis are vulvar pruritus, pain, dysuria, redness, and swelling (5). Subjective symptoms, as well as clinical and laboratory examinations are used to diagnose VVC. The latter includes internal pelvic examination, taking a wet cotton smear, measuring vaginal pH, and vaginal discharge culture. The observer may see budding yeasts or hyphae after adding potassium hydroxide to the vaginal discharge (6).
Vulvovaginal candidiasis may cause recurrent infections in women and some complications in pregnant women, such as membrane premature rupture and preterm labor, and impose women to human immunodeficiency virus (HIV) (4).
Azole compounds, either taken orally or applied as vaginal cream or suppository, can be used to treat vaginal candidiasis (7). These medications can be administered as a single dose (fluconazole, 150 mg) or as 3- to 7-day regimens. Drug resistance; however, is a main concern when using antifungal medications (8). Also, antifungal medications may lead to allergic responses in some patients (9). Drug resistance may lead to the emergence of new fungi, making the therapeutic process even more difficult in the future (10). A previous study showed a recovery rate of 9 - 19% in the women who experienced recurrent C. albicans infections upon six months of continuous treatment with azole medications (11).
Several alternative and complementary treatments have been recently proposed for the treatment of vaginal candidiasis. Some of these alternative medications have antifungal effects that help restore the vaginal microbiota balance while some others have an inhibitory activity against the growth of vaginal microbiota. Substances such as boric acid, vinegar, garlic, and tea have received scientific attention in this regard (12).
Henna (Lawsonia inermis) is an evergreen plant originally obtained from the leaves of a tree with the same name in Egypt. This plant can bind with proteins and be used to dye hair and nail as well (13). Henna hexane extracts have shown antimicrobial effects against microorganisms such as streptococci, staphylococcus, and pseudomonas (14). A study by Suleiman and Mohamed showed that the ethanol and petroleum ether extracts of henna had antifungal activity against all yeast strains except for Pichia Fabianii (15). Along with this, we previously compared the antifungal effects of 4% henna extract with that of clotrimazole in a study on 35 female Wister rats and showed that the two compounds had similar effects (16).
2. Objectives
To the best of our knowledge, no study has yet evaluated the anti-candida effects of henna in humans. Therefore, this study was designed to compare the anti-candida activity of henna with that of clotrimazole in patients with vaginal candidiasis.
3. Methods
This was a parallel randomized controlled trial in which 80 women of reproductive age were recruited from two public health centers in Ahvaz, Iran. Data collection started in October 2019 and finished in December 2019.
Inclusion criteria were as follows: married and monogamous women with C. albicans, aged 18-45 years, and with basic literacy. Women with the following criteria were excluded from the study: having other types of vaginitis, being under medications such as antibiotics and corticosteroids for two weeks before the study, using antifungal drugs four weeks before the study, using any vaginal gel or suppository 48 hours before the study, using hormonal contraceptives, using herbal medicines during two weeks before the study, having vaginal bleeding and chronic diseases such as diabetes, cardiovascular and thyroid diseases, having any allergy to herbal medicines, being pregnant or at the breastfeeding period, having any abnormality in cervical opening, and experiencing stressful events during the month before the study. The eligible women admitted to two specified public health centers in Ahvaz, Iran, and suffering from C. albicans were recruited in this study.
3.1. Sample Size
The following formula was used for sample size calculation (17):
P1 = 0. 95, P2 = 0. 67
The calculated sample size was n = 35, and considering a 14% drop-out rate, 40 women were recruited in each group. The power of the study was set at 90%.
3.2. Drug Preparation
The leaves of the henna tree were obtained from a garden in Kerman, Iran. Then the henna leaves were dried and powdered. Ethanol 80% was added to the powder, and the mixture was kept for 72 hours. The maceration method was used for extraction. The extract was dried using a rotary and a freeze-dryer machine and kept away from light in the refrigerator until preparing the formulation. The herbal cream was prepared at a concentration of 1%. The produced vaginal creams were tested for uniformity, acidity, and dispersion. Clotrimazole 1% vaginal cream (Iran Farma Company) was purchased and inserted into tubes similar to those of henna vaginal cream. Clotrimazole was dyed using a material that was soluble in the water and oil phases. This dye (extracted from Annato plant) can be used in plant-derived and industrial formulations without causing any sedimentation or allergy. So, both the henna and clotrimazole creams had a similar color (orange-yellowish).
Clotrimazole and henna tubes were coded by a pharmacologist (ZAH), and the person who administered the drugs (MY) was also unaware of the content of the tubes. To test for allergies, we first relied on the results of our previous study on the effects of henna on C. albicans in rats (15). In the present study, we first tested some of the creams on the hands of three participants; then, we asked them to test the cream on the outside of the vagina. After observing no allergic reactions, we started to apply the henna cream to the women in the intervention group. All the steps of preparation and coding of henna vaginal cream were carried out by a pharmacologist (ZAH). The herbarium code of this plant, which was acquired in our previous study (16), is JPS017114.
3.3. Measurements
The women referring to two public health centers in Ahvaz, complaining of the signs and symptoms of C. albicans, were assessed according to the mentioned eligibility criteria by a trained midwife who was not aware of the purpose of the study. At the first visit, a disposable speculum was inserted into the vagina without lubrication, and the signs of the disease were recorded into a checklist. Then two sterile cotton swabs were taken from the vaginal discharge. Vaginal pH was measured using a pH gauge paper. A pH less than 4 - 4.5 was regarded in the favor of C. albicans. Samples with higher pH values were excluded because this was an indication of mixed vaginitis. The first swab, which was kept in a sterile tube containing normal saline, was sent to the laboratory for culture. The Saber Dextrose agar culture medium was used to detect C. albicans.
In the laboratory, the samples were incubated in Saber Agar Dextrose supplemented with chloramphenicol at 30 - 37°C for 48 hours, and the colonies were counted using a microscope. Candida albicans was detected using the germ tube test, which is the golden diagnostic method for this yeast. The second sample was assessed in terms of lactobacillus using Gram staining. After obtaining definitive results from the laboratory regarding fungal growth and the confirmation of C. albicans, the women were asked to attend the clinic.
3.4. Randomization and Allocation Concealment
In this study, a random table produced by Microsoft Excel was used for randomization. The table was prepared by a statistician. According to the code (A or B) assigned, women with confirmed C. albicans infection were randomly allocated into one of the two groups of henna or clotrimazole vaginal cream.
For allocation concealment, completely identical cream tubes were prepared by a pharmacist and labeled by the code of A or B. Both the researcher and the participant were unaware of group allocations. During the study, no code was broken. The statistician was also blinded to group allocations until after analysis.
3.5. Intervention
All women with a confirmed C. albicans diagnosis received one applicator (5 gr) of either clotrimazole or henna vaginal cream for seven nights. The women were asked not to have a sexual relationship during the treatment period or use condoms in the case of sexual intercourse. In addition, health recommendations during treatment were given individually for each participant. The women were requested to avoid any vaginal douches and herbal medications during treatment. During treatment, the patients were followed up in terms of their compliance with the medication, as well as the side effects of the creams via the phone calls made by one of the researchers (MY).
3.6. Follow-up
The women were requested to attend the clinic after the completion of the treatment and two and four weeks afterwards for assessing the relapse. At these intervals, the women were evaluated with respect to the signs and symptoms of the disease, and all observations were recorded into a checklist. Also, a smear was obtained from the vagina, which was used for Gram staining, and the results were recorded into the checklist.
The initial diagnosis of candida and the results of treatment and relapse were evaluated according to clinical signs and symptoms, vaginal pH, laboratory observations, and culture outcomes. We also used a questionnaire to record the subjective symptoms of candidiasis, such as burning sensation, itching, discharge, irritation, and dyspareunia. The participants were asked to score the items from zero (not having the symptom) to three (having bothersome symptoms).
3.7. Statistical Analysis
All data were entered into SPSS version 22. The chi-square test and independent t-test were used for categorical and continuous data, respectively. Generalized estimating equations (GEE) were used to assess changes in the signs and symptoms of vaginitis at one, two, and four weeks after the intervention. A P value of < 0.05 indicated a statistically significant observation.
3.8. Ethical Considerations
The study was approved by the Ethics Committee of Ahvaz Jundishapur University of Medical Sciences (Ref Code: IR.AJUMS.REC.1394.616), and the protocol was registered in the Iranian Registry of Clinical Trials (Ref No: IRCT2016022119743N4). All the participants signed written informed consent before data collection, and the anonymity of the participants was observed.
4. Results
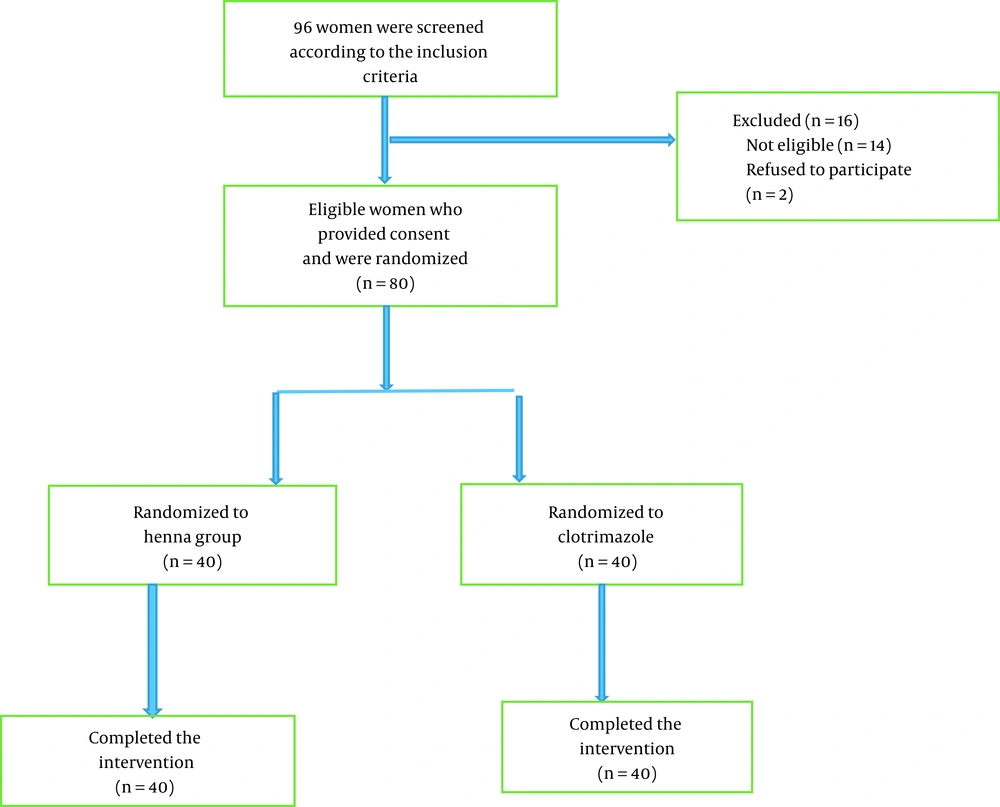
In this study, all of the 80 women recruited completed the study (Figure 1). The demographic characteristics of the participants are presented in Table 1. The mean ages of the women in the henna and clotrimazole groups were 31.4 ± 7.8 and 33.2 ± 8.5 years, respectively. The two groups did not have any significant difference regarding employment status, education level, economic status, and the number of coituses per week.
| Variables | Henna (N = 40) | Clotrimazole (N = 40) | P Value |
|---|---|---|---|
| Age (y) | 31.4 ± 7.8 | 33.2 ± 8.5 | 0.37 |
| Employment status | 0.30 | ||
| Housewife | 28 (70) | 31 (77.5) | |
| Employee | 12 (30) | 9 (22.5) | |
| Education | 0.38 | ||
| Under diploma | 20 (50) | 25 (62.5) | |
| Diploma | 8 (20) | 4 (10) | |
| Academic | 12 (30) | 11 (27.5) | |
| Economic status | 0.13 | ||
| Weak | 8 (20) | 4 (10) | |
| Moderate | 25 (62.5) | 33 (82.5) | |
| Good | 7 (17.5) | 3 (7.5) | |
| Number of coituses per week | 0.64 | ||
| 1 or less | 26 (65) | 23 (57.5) | |
| 2 | 5 (12.5) | 6 (15) | |
| 3 | 8 (20) | 9 (22.5) | |
| 4 or more | 1 (2.5) | 2 (5) |
aValues are expressed as mean ± SD or No. (%).
Table 2 shows the clinical signs and symptoms of candidiasis in the two groups of henna and clotrimazole. In the henna group, 82.5% of the participants had a severe burning sensation before the intervention, but after four weeks of the intervention, 92.5% of them were free of burning in comparison with 45% in the clotrimazole group. After four weeks of treatment and regarding itching, discharge, irritation, and dyspareunia, 87.5%, 90%, 95%, and 90% of the women in the henna group had none of these symptoms compared to 5%, 37.5%, 52.5%, and 27.5% in the clotrimazole group, respectively (P < 0.001).
| Variables | Henna (N = 40) | Clotrimazole (N = 40) | ||||||
|---|---|---|---|---|---|---|---|---|
| Baseline | 1 Week After Intervention | 2 Weeks After Intervention | 4 Weeks After Intervention | Baseline | 1 Week After Intervention | 2 Weeks After Intervention | 4 Weeks After Intervention | |
| Burning | ||||||||
| None | 36 (90) | 36 (90) | 37 (92.5) | 3 (7.5) | 18 (45) | |||
| Mild | --- | 4 (10) | 4 (10) | 3 (7.5) | --- | 26 (65) | 34 (85) | 20 (50) |
| Moderate | 7 (17.5) | --- | --- | --- | 11 (27.5) | 11 (27.5) | 6 (15) | 2 (5) |
| Severe | 33 (82.5) | --- | --- | --- | 29 (72.5) | --- | --- | --- |
| Itching | ||||||||
| None | 0 | 28 (70) | 34 (85) | 35 (87.5) | 0 | 4 (10) | - | 2 (5) |
| Mild | 1 (2.5) | 11 (27.5) | 6 (15) | 5 (12.5) | 1 (2.5) | 29 (72.5) | 34 (85) | 32 (80) |
| Moderate | 11 (27.5) | 1 (2.5) | --- | --- | 13 (32.5) | 7 (17.5) | 6 (15) | 6 (15) |
| Severe | 28 (70) | --- | --- | --- | 26 (65) | 0 | 0 (0) | --- |
| Discharge | ||||||||
| None | 0 | 38 (95) | 37 (92.5) | 36 (90) | 2 (5) | - | 15 (37.5) | |
| Mild | 1 (2.5) | 2 (5) | 3 (7.5) | 4 (10) | 2 (5) | 30 (75) | 35 (87.5) | 22 (55) |
| Moderate | 31 (77.5) | --- | --- | --- | 20 (50) | 8 (20) | 5 (12.5) | 3 (7.5) |
| Severe | 8 (20) | --- | --- | --- | 18 (45) | --- | --- | --- |
| Irritation | ||||||||
| None | 17 (42.5) | 37 (92.5) | 34 (85) | 38 (95) | 5 (12.5) | |||
| Mild | 13 (32.5) | 3 (7.5) | 6 (15) | 2 (5) | 9 (22.5) | 27 (67) | 36 (90) | 21(52.5) |
| Moderate | 10 (25) | --- | --- | --- | 17 (42.5) | 8 (20) | 4 (10) | 16 (40) |
| Severe | --- | --- | --- | --- | 14 (35) | --- | - | 3 (7.5) |
| Dyspareunia | ||||||||
| None | 37 (92.5) | 34 (85) | 36 (90) | |||||
| Mild | 6 (15) | 3 (7.5) | 6 (15) | 4 (10) | 5 (12.5) | 4 (10) | --- | 11 (27.5) |
| Moderate | 29 (72.5) | --- | --- | --- | 28 (70) | 24 (60) | 36 (90) | 25 (62.5) |
| Severe | 5 (12.5) | --- | --- | --- | 7 (17.5) | 12 (30) | 4 (10) | 4 (10) |
aUsing the chi-square test, the differences between the two groups were not significant at the baseline (P > 0.05), but there were significant differences at 1-, 2-, and 4-week after the intervention (P < 0.001).
bValues are expressed as No. (%).
Table 3 shows colony formation, the number of lactobacillus, and vaginal pH in the participants of the two study groups before and after the intervention using the GEE test. The means (SD) of colony formation were 290.85 (47.35) and 265.12 (37.46) in the henna and clotrimazole groups, respectively, at the baseline, which reduced to zero and 25.45 (25.09) at the 4th week of the intervention (P < 0.001).
| Variables | Henna (N = 40) | Clotrimazole (N = 40) | P Value |
|---|---|---|---|
| Colony formation | |||
| Before intervention | 290.85 (47.35) | 265.12 (37.46) | 0.51 |
| 1 week after intervention | 0.00 (0.0) | 32.10 (32.08) | < 0.001 |
| 2 weeks after intervention | 0.00 (0.0) | 5.77 (12.19) | < 0.001 |
| 4 weeks after intervention | 0.00 (0.0) | 25.45 (25.09) | < 0.001 |
| Lactobacillus | |||
| Before intervention | 10.1 (9.1) | 12.8 (9.0) | 0.57 |
| 1 week after intervention | 64.0 (14.6) | 19.6 (15.0) | < 0.001 |
| 2 weeks after intervention | 75.4 (13.0) | 14.6 (15.6) | < 0.001 |
| 4 weeks after intervention | 88.8 (11.1) | 16.8 (14.8) | < 0.001 |
| Vaginal pH | |||
| Before intervention | 3.7 (0.38) | 3.8 (0.40) | 0.39 |
| 1 week after intervention | 3.5 (0.28) | 3.9 (0.60) | < 0.001 |
| 2 weeks after intervention | 3.4 (0.41) | 3.5 (0.15) | < 0.001 |
| 4 weeks after intervention | 3.6 (0.16) | 4.2 (0.59) | < 0.001 |
Abbreviation: pH, Potential of hydrogen.
aValues are expressed as mean (SD).
bThe GEE test was used to analyze data.
The mean of lactobacillus colonies significantly increased in the henna group compared to the clotrimazole group (P < 0.001). Also, vaginal pH decreased significantly in the henna group compared to the clotrimazole group (P < 0.001). None of the participants complained of any side effect in the henna or clotrimazole group.
5. Discussion
This study was designed to compare the effects of the ethanolic extract of henna and clotrimazole vaginal cream on vaginal candidiasis symptoms. In comparison to clotrimazole, our results showed that the henna cream could significantly reduce the signs and symptoms of vaginal candidiasis. In this regard, burning sensation, itching, discharge, irritation, and dyspareunia decreased in around 90% of the participants in the henna group, while clotrimazole could alleviate these symptoms in only 45%, 5%, 37.5%, 52.5%, and 27.5% of the women, respectively. According to our results, henna was more effective than clotrimazole in decreasing colony formation. Also, the reduction in vaginal pH was more pronounced in the henna group compared to the clotrimazole group. This was the first report on the impact of henna on C. albicans in humans. We previously investigated the effects of henna on vaginal candidiasis in rats, and our results showed that the effects of 4% henna vaginal cream were similar to that of clotrimazole (16). Other studies have evaluated the effects of henna on C. albicans in vitro. For example, Nawasrah et al. combined henna with acrylic resin denture and found that the combination significantly inhibited C. albicans proliferation (18). In their study, Singhal et al. compared the effects of pomegranate and henna on C. albicans and found that the effects of henna were superior to that of pomegranate in terms of controlling candidiasis in vitro (19). Rahmoun et al. also found that the ethanolic extract of Algerian L. inermis (150 µg/mL) had antifungal activity (20). The antifungal activity of the ethanolic extract of henna was also reported by Suleiman and Mohamed in an in vitro study (15). The results of our study are consistent with those of the above-mentioned studies. It has been shown that the antimicrobial effects of henna leaves result from its 0.5-1.5% lawsone content, a compound showing dyeing properties (20). The antifungal effects of henna may also be attributed to lawsone in henna leaves (21). Yoshijima et al. suggested that the hydrophilic materials of henna could reduce C. albicans adherence to any surface (22). The antifungal effects of some species of henna, such as Sudanese henna, have been attributed to their naphthoquinone content (23).
The results of the present study showed that colony formation reduced in both of the study groups (i.e., henna- and clotrimazole-treated); however, the number of colonies reached zero only in the henna group after treatment. Also, vaginal pH reduced, and the mean number of lactobacillus increased significantly in the henna group compared to the clotrimazole group, according to the GEE test. We could not find any study evaluating the effects of henna on lactobacillus colony formation. However, YİĞİT, in his study, found that Lawsonia inermis had the highest antifungal activity against 68 clinical candida strains, including C. albicans (24), which was similar to our observation. Other studies have shown that henna has the ability to disintegrate fungal membranes and enzymes, which can alter the cell membrane arrangement and morphology of fungi (20, 25).
5.1. Limitations
This is the first study on the effects of henna on vaginal candidiasis in humans. Other studies have assessed the effects of this herb in vitro or on animals. Despite certain strengths, this study has one main limitation. For assessing the subjective symptoms of vaginal candidiasis, we relied on the responses of the participants, which may have been affected by the recall bias.
5.2. Conclusions
The results of this study showed that henna vaginal cream significantly reduced the subjective symptoms of vaginal candidiasis, colony formation, and vaginal pH and increased lactobacillus formation. Further clinical trials are recommended to obtain the most effective dose of the henna vaginal cream and to investigate its efficacy in women with recurrent vaginal candidiasis.