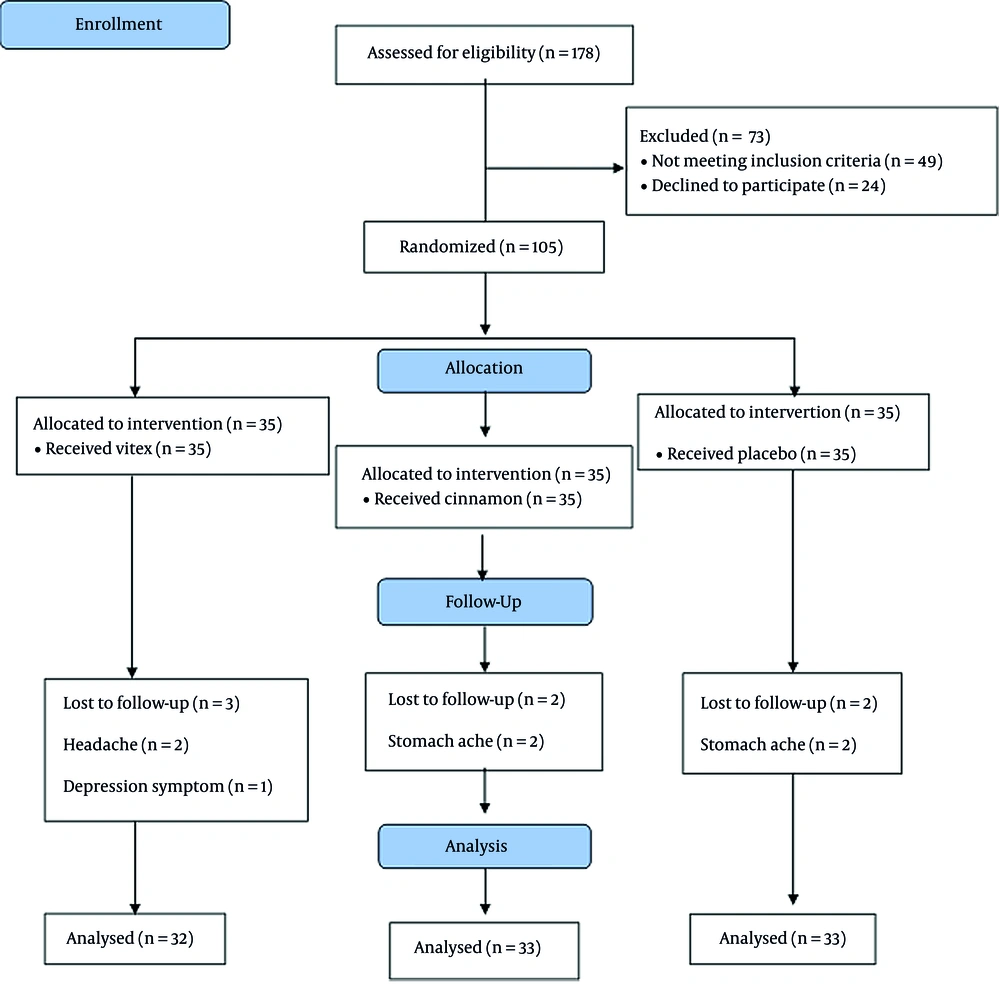
Some notable strengths of this study include using the random assignment method, blinding method, and careful phone call follow-up until two and three months after the intervention.
According to the presented data, cinnamon improved sexual function after three months. In this regard, the study by Safavi et al. showed that the total score of sexual function in women of reproductive age increased after two months of cinnamon drops (
23). There is no study about the effect of cinnamon on sexual function, so it was impractical to review our result and compare it to other studies. Nevertheless, few studies, including the study by Kianitalaei et al. in 2020, showed that alcea benefits the sexual function of postmenopausal women (
24). Also, in Malakouti et al.'s study, inhalation aromatherapy with a combination of lavender, fennel, geranium, and red rose improved the sexual function of postmenopausal women (
25). According to the results of these studies, it can be decided that medicinal plants can generally be effective for the sexual function of postmenopausal women.
Lubrication and sexual satisfaction scores increased in the cinnamon group, while a study by Safavi et al. in 2018 also showed that two months of cinnamon drops increased lubrication and sexual satisfaction in women of childbearing age (
23). Also, in the study by Taavoni and Haghani in 2014, the results showed that aphrodite improved the sexual satisfaction of postmenopausal women, which was also statistically significant (
26).
In the present study, other areas of sexual function for the cinnamon and placebo groups, namely sexual desire, orgasm, arousal, and intercourse pain, did not improve significantly. One study showed that aphrodite improved sexual desire and orgasm in postmenopausal women after four weeks of intervention (
27). Also, a study by Safavi et al. in 2018 showed that rose, ginger, and cinnamon drops improved sexual desire, orgasm, arousal, and intercourse pain in women of childbearing age (
23). According to the results obtained in the present study and the research mentioned above, it can be concluded that cinnamon generally improves sexual function. The different results observed for each domain could be due to differences in sample size, instruments to measure sexual function, prescribed doses of drugs, drug preparation methods, or target groups.
Vitex can improve sexual function after three months. In this regard, Sadeghi et al. showed that vitex improves sexual function in postmenopausal women (
28). Mazaro-Costa also stated that plants such as vitex, fennel, ginkgo,
Tribulus terrestris, red clover, black cohosh,
Angelica archangelica, hops, and ginseng, according to a search in the PubMed database, have the greatest impact on the reproductive system of menopausal women and improve sexual function (
8). Contrary to the results of our study, van Die et al. showed that after 16 weeks of consuming vitex, the sexual function of postmenopausal women did not improve (
29). Also, Naseri et al. could not obtain any significant improvement in the sexual function of postmenopausal women after eight weeks of vitex consumption (
30).
However, it should be noted that the tools used in these two studies are different from the present study. In the study by van Die et al. (
29), vitex tablets were used for the intervention, and in the study by Naseri et al., the sample size (26 in each group) and the dose used for the intervention (30 mg of vitex) were less than in the present study. As a result, due to the lack of sufficient studies and contradictory results, it is not possible to comment definitively on the effectiveness of vitex on the sexual function of postmenopausal women.
The sexual desire and arousal domains in the vitex group were the only domains that showed significant improvement. Similarly, a 2002 study by Lucks et al. found that vitex oil improved sexual desire in postmenopausal women (
31). These results are also evident in a 2005 study by Smolinski et al., in which sexual desire improved in postmenopausal women 16 weeks after consuming vitex (
32). Another study by Heirati et al. showed that the difference between the vitex and placebo groups was not significant in any domain, but there was a significant difference in the overall sexual function mean score, so the intervention group had a higher score than the placebo group after 16 weeks (P < 0.05) (
33).
Side effects included headache in two participants and depressive symptoms in one participant of the vitex group, and stomachache in the cinnamon (two participants) and placebo (two participants) groups. Also, two participants in the cinnamon group stated that taking the capsules caused vaginal spotting, but they did not stop taking the capsules. Participants with side effects were referred to a health center physician and psychologist.
Different side effects reported in studies on cinnamon and vitex can be due to differences in drug preparation, target groups, intervention doses, consumption methods, duration of use, and research methods.
Like Farahmand and Ramezani Tehrani's study, this study showed that appropriate plants could effectively treat sexual disorders; however, more studies in this field are needed (
34).
There were also limitations to this research, including the fact that the subjects avoided expressing sexual problems or unusual sexual relations due to cultural reasons and the subject's sensitivity. Subjects were assured that the completed questionnaires and their information would remain confidential. Stress and anxiety of subjects while taking the capsules due to COVID-19 and the subsequent negative impact on study results was another limitation of this study.
5.1. Conclusions
Cinnamon and vitex improved sexual function in menopausal women. More studies in this field may be conducted to introduce them as an appropriate herbal remedy for older women.