1. Background
Burnt wound is an injury, especially burned by fire, heat, caustic agents, electricity or radiation (1). It can be classified into epidermal, partial thickness and full thickness burn wound (2). Incidence rate of burn injuries is approximately 1.25 million cases per year in the United States (3). The prevalence of burning in third world countries is several times more than Europe and North America in which are also more severe (4). Infection due to new strains of drug resistant bacteria is the major impediment topical factor in healing process and also prolongs treatment period (5, 6). Improving the methods of wound healing, tissue repairing and decreasing the time of hospitalization offer tremendous opportunities to enhance the quality of life for burnt patients (7).
Silver sulfadiazine (SSD) was introduced in 1970s as an antibacterial agent for topical treatment of burns and wounds (8). SSD cream has broad spectrum antimicrobial activities. It has been shown to inhibit bacteria resistant to other antimicrobial agents. SSD cream, although being effective, causes some systemic complications including neutropenia, erythema multiform, crystalluria and methemoglobinemia (9). Although SSD has been the standard treatment of burn wound in hospital, alternative treatment for burnt wound that is cheaper and locally available is still needed (10).
Visceral fat of goat mixed with barley seed ash (Vf-BS) has been used in Iranian traditional medicine in the treatment of wounds and burns. Traditional use of this natural product is recommended in some region of Fars province, southern Iran. It could be considered as a valuable cost benefit wound healing agent.
Barley (Hordeum vulgare L) belongs to the grass family, Poaceae (Gramineae). It is the fourth most important cereal crop in the world (11). Barley grain is an excellent source of dietary fibers and other bioactive constituents, such as protein and complex carbohydrates and a good source of certain vitamins and minerals. Furthermore, barley contains many other compounds including simple phenolic acids, flavonoids and lignans, all of which have good antioxidant properties (12, 13).
Visceral fat tissue refers to the ectopic fat depots surrounding the internal organs and is often used synonymously for intra-abdominal fat (14). In general, visceral fat depots in goats consist mainly of saturated fatty acid (SFA), monounsaturated fatty acid (MUFA) and small amounts of polyunsaturated fatty acid (PUFA) (15).
2. Objectives
Today, there is growing interest towards clinical application of natural drugs in healing of burn wounds; therefore, the present study was designed to compare the healing effects of traditional preparation with SSD on type II superficial skin burning in rats.
3. Materials and Methods
3.1. Chemicals
All the chemicals were of analytical grade. Silversulfadiazine cream was purchased from Sobhan Company (Iran). Visceral fat prepared from fat around the intestine of goats was obtained from slaughterhouses in shiraz.
3.2. Drug Preparation
Six-rowed barley grains (Hordeum Vulgare.L) were collected from Nourabad Mamasani region in northwest of Fars province, Iran. The grains were identified at the Herbarium of Department of Pharmacognosy, School of Pharmacy, Shiraz. The barley grains were burned by indirect heat, at 160oC for 30 minutes and then were powdered. Visceral fat of goat was heated very slowly by indirect heat to be melted. Then burnt powder and oil was mixed in proportion of 1 to 2 respectively, and it was shaken to produce a uniform suspension. Finally, this cream was sterilized.
3.3. Experimental Animals
60 Male albino Wister rats with mean body weight of 250 - 300 g and 5 - 6 months old were obtained from the Laboratory Animal breeding and maintenance Center of Grash Medical Faculty, Iran. Rats were randomly divided into four groups, each group contained fifteen animals. They were kept in polycarbonate cages under standard condition (temperature 24 - 28oC, relative humidity 60 - 70% and 12-hour dark-light cycle) and fed with standard pelleted diet and water ad libitum. All experimental protocols involving animals were reviewed and approved by the Local Animal Ethics Committee guideline for use of experimental animals.
3.4. Burn Wound Model
The back of rats was shaved with a sterilized razor blade. Following this procedure, the animals were returned to their cages for 24 hours to reduce swelling caused by shaving. A method described by Kaufman et al. was used for induction of burns (16).
The rats were initially anesthetized with single intramuscular injections of 6 mg/kg xylazine hydrochloride (Rompun, Bayer, 23.32 mg/mL) and 85 mg/kg ketamine hydrochloride (Ketalar, Parke-Davis, 50 mg/mL). The skin of animals’ back prepared with 10% antiseptic povidone-iodine solution (Kim-Pa, Poviiodeks, 10% povidone-iodine). Then second-degree burn was created by a metal cylinder (1.5 cm ID, self-made) immersed in boiling (100oC) water for three minutes and maintained on the back of rats for three seconds. All animals were resuscitated immediately with lactate Ringer’s solution (2 mL/100 g of body weight) intraperitoneally. Finally, each animal was placed in a separate cage. To avoid variations between experiments, the same researcher induced all burns.
3.5. Treatment and Assessment of Healing Process
Control group: The burned areas in this group received no treatment.
Normal saline group: immediately after burning, normal saline was applied topically onto the surface of burn areas, twice a day for 14 consecutive days.
Silversulfadiazine group: immediately after burning, SSD cream was applied topically onto the surface of burn areas, twice a day for 14 consecutive days.
Traditional preparation group: immediately after burning, traditional preparation was applied topically onto the surface of burn areas, twice a day for 14 consecutive days.
The burn wound site was photographed with a digital camera (Sony Cybershot DSC-P72) on days 1, 4, 9 and 14. Based on images obtained from the digital camera, the wound area was measured with Image processing software (Digimizer 4.1.1.0, persianGFX.com).
The evaluated surface area was then used to calculate the percentage of wound contraction, tacking the initial size (measured on day one) of the wound as 100% using the following formula (17).

For microscopic studies, five rats from each group were killed on 4th, 9th and 14th days of experiment, and then burned area with a little normal skin was sampled. These tissue samples were kept in 10% neutral buffered formalin solution and sent to pathologic laboratory of veterinary medicine, Shiraz University of Medical Sciences. After fixation in formalin solution, the skin tissues were embedded in paraffin, cut into 5 μm sections, stained with hematoxylin and eosin dye. Stained slides were observed for re-epithelization, collagen content, inflammatory changes, polymorphonuclear cells, vacuolization and fibroblast. All slides were observed under light microscope (Olampus, Japan).
3.6. Statistical Analysis
The percentage of wound contraction was analyzed by statistical package SPSS 18.0 for Windows (IBM Company). Statistically, all data were expressed as mean ± S.D. Differences between groups in different days were estimated using One-way ANOVA analysis of variance. Statistical significance was considered at P < 0.05.
4. Results
No mortality was seen in animals during the study. The results of the burned area measurement are shown in Table 1, Figures 1 and 2. General parameters for the evaluation of wound healing, histopathological examination and measurement of the wound area were used.
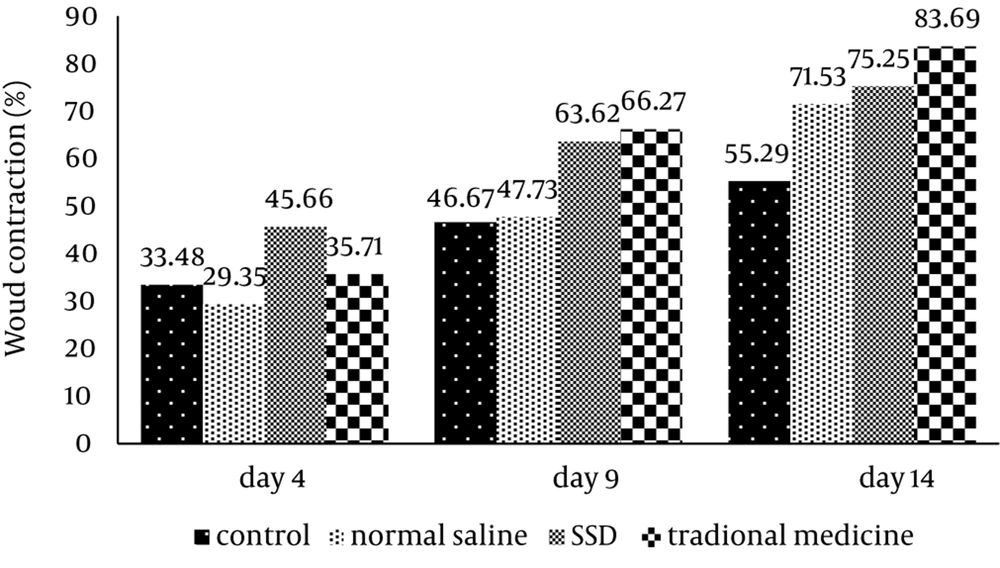
On day 1, the average diameter of wound in all groups was almost similar and there was no significant difference between these groups (P < 0.05). On 4th day, the size of wound was decreased in all groups but the percentage of wound contraction in SSD group was significantly greater than other groups (P < 0.05). On 9th day of trial, the wound area was lower significantly in all groups compared with 4th day. Furthermore, wound contraction in SSD and traditional preparation groups were significantly greater than control and NS groups, but there was no significant difference between SSD group and traditional preparation group. On 14th day, as shown in Table 1, rats treated with NS, SSD and traditional preparation exhibited a significant (P < 0.05) reduction in the size of wound compared with the control group. Additionally, the percentage of wound contraction in the traditional medicine group was significantly greater than other groups (Figure 1).
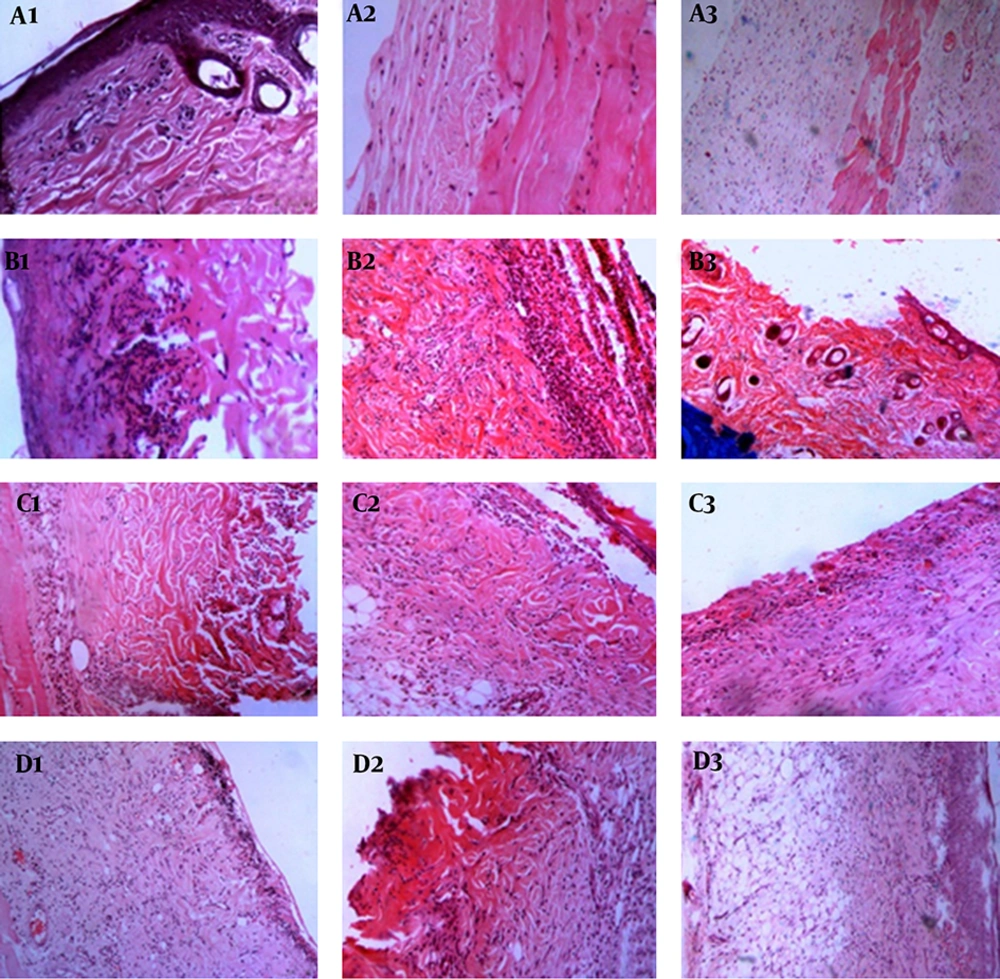
Histopathologic evaluations on fourth day after injury, severe inflammation and crust formation in all the experimental groups were seen. In addition, angiogenesis was observed in the traditional medicine group except these findings.
On 9th day in both control and normal saline groups, severe inflammation and mild angiogenesis were seen. In SSD and traditional preparation groups, acute inflammatory cell infiltration and granulation tissue formation were observed.
On 14th day, collagen deposition was observed in both control and normal saline groups (Figure 2). In SSD group, collagen deposition and chronic inflammatory cell infiltration were observed and in the traditional preparation-treated group, collagen deposition and epidermal regeneration were seen.
A1) Control group in day 4, A2) Control group in day 9, A3) Control group in day 14, B1) Normal saline group in day 4, B2) Normal saline group in day 9, B3) Normal saline group in day 14, C1) Silver sulfadiazine group in day 4, C2) Silver sulfadiazine group in day 9, C3) Silver sulfadiazine group in day 14, D1) Traditional medicine group in day 4, D2) Traditional medicine group in day 9, D3) Traditional medicine group in day 14.
| Groups | 1st day | 4th day | 9th day | 14th day |
|---|---|---|---|---|
| Control | 14.7302 ± 1.13 | 9.738 ± 0.154 b, c | 7.764 ± 0.785 b, c | 6.450 ± 0.486 b, c, d |
| Normal Saline | 14.910 ± 0.982 | 10.423 ± 0.955 b | 7.995 ± 0.104 b, c | 4.140 ± 0.523 c, e |
| Silversulfadiazine | 15.037 ± 1 .6197 | 8.169 ± 0.986 c, d, e | 5.596 ± 0.597 d, e | 3.574 ± 0.441 c |
| Traditional Medicine | 14.985 ± 1.108 | 9.716 ± 0 .715 b | 5.236 ± 0.611d, e | 2.341 ± 0.665 b, d, e |
The Average of Wound Area on Different Days Based on mm2 a
5. Discussion
Burn remains a major public health issue all over the word, especially in developing countries. Burn wounds are painful maladies and entail a complex healing process (9, 18). The final aim of burn management and therapy is wound healing and epithelization as soon as possible to prevent infection and reduce functional and aesthetic after effects (8, 19). Wound healing is a collaborative process involving a variety of cells and matrix components interacting continually towards a common goal (20) This process is characterized by three stages of inflammation, proliferation and remodeling. The proliferative phase typically demonstrates angiogenesis, collagen deposition, granulation tissue formation, epithelialization and wound contraction (21).
Barley grain contains a number of components associated with health benefits including tocotrienol, lignan, phytoestrogen, phenolic compounds and phytic acid (22, 23). Barley is a folk remedy for bronchitis, burns, cancer, catarrh, chest, chilblains, cholecystosis, cholera, cough, debility, diarrhea, dyspepsia, fever, inflammation, measles, phthisis, puerperium, sores and urogenital ailments (24).
In the current study, there was a significant difference regarding mean percentage of wound contraction between days 4, 9 and 14 of experiment in all groups. Nevertheless, most wound contraction was seen in traditional preparation group. The results indicated that both traditional preparation and SSD significantly (P < 0.05) promoted wound contraction and shortened epithelization period. However, the traditional cream seemed to be more effective. These results here are also supported histologically by increased collagen deposition, angiogenesis and minimal inflammation in rats treated with traditional cream compared to other groups. Many studies have been performed to evaluate wound healing potential of natural products.
Yaman et al. assessed the healing effects of Nigella sativa and silversulfadiazine on burn wound in rats. Histopathological examination was used to evaluate the healing effects. They reported that using NS and SSD cream are effective in healing burn skin wounds in the rat model (25).
In another study, Nikzad et al. investigated the effects of Arnebia leaf on healing process of second-degree burn. This study showed that Arnebia leaf did not have any effect on healing of second-degree burn wounds in rats (26).
In another research, Shokouhi-Sabet-Jalali et al. revealed that topical honey in treatment of burn compared with normal saline accelerated the healing process and had valuable antimicrobial effect in promoting recovery of this kind of wound (27).
It has been established that visceral fat induces nitric oxide synthase (28, 29).This enzyme generates nitric oxide (NO) from amino acid L-arginine. NO has antibacterial properties and plays a critical role in many phases of wound healing (30, 31). Furthermore, main fatty acids of visceral fat of goat are C18:1, C18:0, C16:0, C14:0, C16:1, C10:0 and C12:0. They are useful as a nutritional source, solvent, vehicle and stabilizer of administered products and form a protective barrier for the skin. Besides being important in processes of cellular inflammation, they have a great capacity of tissue regeneration and antimicrobial activity (32, 33). It may be the mechanism that links visceral fat to wound healing. These results are in agreement with those of Cardoso and Souza. They studied the effects of polyunsaturated fatty acids on diminishing wound area and demonstrated that PUFAs may play an important role in wound healing (32).
Furthermore, some ingredients in the barley seed ash might be responsible for wound healing. Finally, this study affirmed that the mixture of visceral fat and barley seed ash as a traditional cream accelerated wound healing and wound contraction and promoted epithelization. According to the obtained results, beneficial effects of this traditional preparation in the healing of superficial skin wounds are comparable with SSD in rats. The present study indicated that this preparation could be applied in the treatment of burns and may be an alternative to the use of SSD and other routine treatments.