1. Background
Preeclampsia is a serious complication that affects 5% - 8% of pregnancies (1).
It is the third leading cause of maternal mortality in the world and second in Iran (2). According to the estimation by the World Health Organization, preeclampsia is responsible for 10% of maternal mortality, and in Asian women has worse pregnancy outcomes than the other countries (3, 4).
It is diagnosed with high blood pressure and proteinuria after the 20th week of gestation (5, 6).
Despite extensive research in recent decades, it seems impossible to prevent its occurrence (7, 8). The risk factors of preeclampsia can be found in the first pregnancy, chronic diseases, diabetes before pregnancy, kidney diseases, chronic hypertension, rheumatic disease, molar pregnancy, twin pregnancies, maternal infections, high maternal weight, family history of preeclampsia, history of preterm labor, and smoking (9, 10).
Various measures to prevent or modify the severity of preeclampsia such as low-salt diet, exercise, taking diuretics, low-dose aspirin, antihypertensive drugs, and fish oil are studied (11, 12).
Preeclampsia is complemented by vasospasm and endothelial stimulation leading to decreased organ perfusion (13). Therefore, magnesium sulfate is the effective medicine that may act as a vasodilator (14, 15).
Also, the antioxidants have good efficacies in the treatment of preeclampsia (16-18), and some studies show that herbal products, especially the ones with antioxidant activities, may be more congruent with the human nature and result in lower side effects and risk of preeclampsia (19, 20). According to the traditional knowledge, garlic may be effective in the treatment of preeclampsia; however, the efficacy is not established (21, 22). Garlic (Allium sativa L.), belonging to Alliaceae family, contains alliin and related derivatives such as allicin, polysulfides, ajoenes, mercaptanes, thioglycosides, thiosulfinates, and adenosine and can be used as some vitamins such as thiamine, niacin, and vitamin-C (23). However, garlic is a native of Middle-Asia and could be found worldwide. It is traditionally used as a treatment for respiratory (24, 25) and cardiovascular diseases; as well as glycemic control and has antineoplastic and antimicrobial properties (26-28).
In recent decades, many clinical studies were performed on the efficacy of garlic, and it was concluded that it decreases blood pressure and serum cholesterol, and is effective in the prevention and treatment of heart diseases, especially atherosclerosis (29). Also, genetics is a predisposing factor for preeclampsia and there is evidence that certain races are more exposed to this condition (30, 31).
2. Objectives
Therefore, according to the reports of studies on the high prevalence of preeclampsia in Turkmen women living in Gorgan, and the antihypertensive effect of garlic, the current study aimed at investigating the efficacy of cultivated garlic in Golestan province in decreasing the risk of preeclampsia in high-risk Turkmen pregnant women.
3. Methods
The current interventional, double-blind, randomized, clinical trial was conducted in health centers of Golestan province, Iran. Inclusion criteria were: primigravid women aged < 40 years, having normal blood pressure, and being high-risk for preeclampsia (first-degree family history of preeclampsia) and normoglycemic.
Women with hypersensitivity to garlic or drug consumption, the ones with underlying, heart, renal, and chronic pulmonary diseases, women with chronic hypertension, rheumatologic and thyroid diseases, placenta abruption, complete bed rest, twin pregnancy, history of preterm delivery, premature preterm rupture of membrane, gestational diabetes, anemia, and obesity were excluded.
For pregnant women without diabetes, average fasting blood sugar (FBS) levels vary between 60 and 95 mg/dL (32).
Gestational hypertension is defined by ACOG (American College of Obstetrics and Gynecology) guidelines as blood pressure ≥ 140 mmHg systolic or 90 mmHg diastolic taken twice, six hours apart, after 20th week of gestation when previous blood pressure was normal. Alternatively, a patient with a systolic blood pressure > 160 mmHg or diastolic blood pressure > 110 mmHg can be confirmed to have gestational hypertension (33).
Preeclampsia is defined by ACOG guidelines as meeting either of the above hypertension criteria with ≥ 300 mg protein excretion in a 24-hour urine (33).
The convenience sampling method was used to select 56 patients in each group with α = 0.05 and β = 0.2.
After the exclusions, a total of 112 pregnant women started the study. Participants were randomly allocated to receive either the garlic capsule (n = 56) or placebo (n = 56) for eight weeks. The study was performed according to the principles of the Declaration of Helsinki. The ethical committee of Islamic Azad University, Pharmaceutical Sciences Branch approved the study protocol and informed written consent was obtained from all participants; the study was also registered in the Iranian Registry of Clinical Trials (IRCT No. 2015053122490N1).
3.1. Intervention
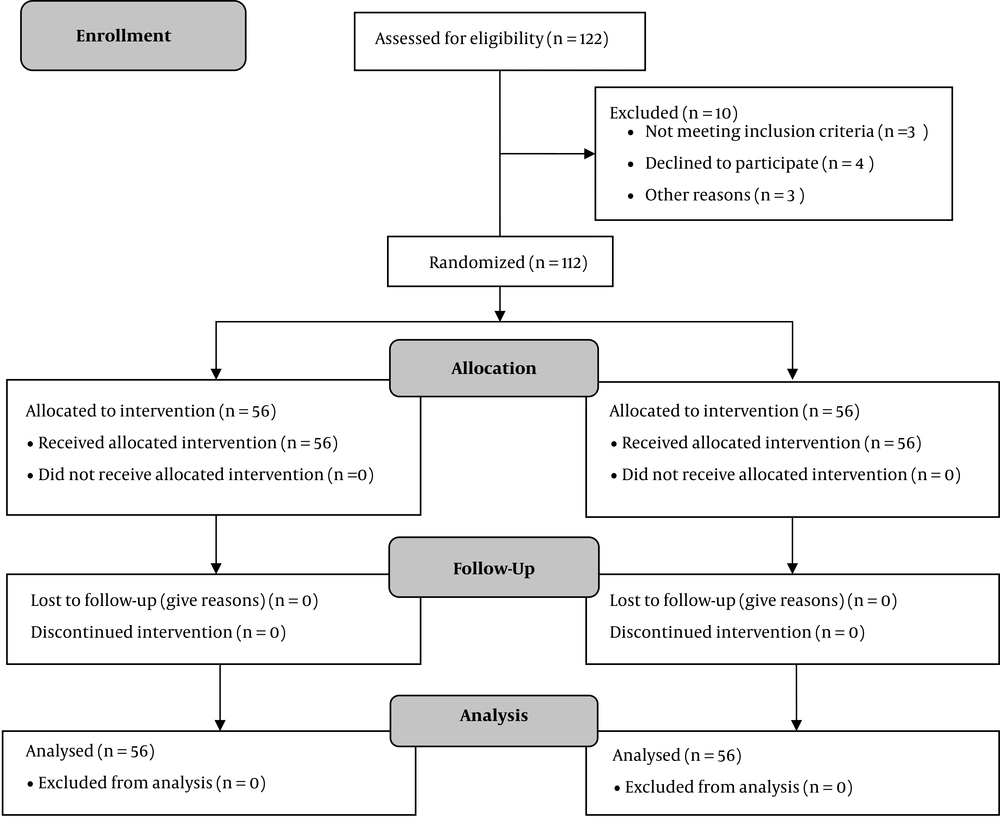
Primigravida Turkman pregnant women in the 3rd trimester of pregnancy were randomly assigned to receive either garlic capsule 800 mg/day or placebo capsule containing 1000 mg allicin per day (27) with the same color and shape. For random allocation, randomized block design, block size 4 (two alleles), was performed by someone other than researchers. Blood pressure, weight, and FBS were measured at three time points: at baseline as well as one and two months after the intervention. Participants with gestational age of 28 weeks were followed up for two months. The treatment continued for eight weeks. Study profile is displayed in Figure 1.
Garlic collected from Golestan Province was dried and then milled to provide garlic powder and prepare garlic capsules in the laboratory of Department of Pharmacology, Islamic Azad University, Pharmaceutical Sciences Branch.
These out comes measured at 3 time points: at the beginning, one, and two months after the intervention, and would be compared across the groups. In the studied samples, systolic and diastolic blood pressures were the primary outcomes, while FBS and weight gain were the secondary ones.
Physician and pregnant women were blind to the prescribed capsule. To resolve dropout problem, 10% higher than the calculated sample size was enrolled. The informed consent forms were signed by all subjects and the Declaration of Helsinki was respected throughout the study period; the drug costs were paid by authors.
Pregnancy weight data were taken from the clinical records of pregnant women. Demographic characteristics were collected by a trained midwife at the maternity clinic at baseline. Body weight was measured barefoot in the fasting state with minimal clothing, using a digital scale (Seca, Hamburg, Germany).
Systolic and diastolic blood pressures were measured via a sphygmomanometer (ALPK2, Zhejiang, and China) twice (in the first and second months after the intervention) by the trained midwife at the maternity clinic. Blood pressure was measured after 30 minutes resting in the sitting position for each patient. Patients were monitored for any symptoms of hypertension, proteinuria, weight gain, drug side effects, and other possible complications in each prenatal visit and no complications were reported.
3.2. Statistical Analysis
In the current study, data were analyzed using SPSS version 20. Data were expressed as mean ± standard deviation (SD) or number (%) where appropriate. Quantitative data were compared between the two groups using t test. Chi-squared test, when appropriate, was used to compare the variables. The Kolmogorov-Mirnov test was utilized to test the normality of quantitative data. Inter- and intragroup comparisons were performed for repeatedly measured quantitative data. P < 0.05 was considered statistically significant.
4. Results
The current study was performed on 112 women (with a first-degree family history of preeclampsia). Demographic and medical characteristics of both groups are presented in Table 1. In both groups, the blood pressure was in normal range.
| Measurements at Baseline | Garlic | Placebo | P Value |
|---|---|---|---|
| Weight, kg | 59.27 ± 4.88 | 62 ± 4.93 | 0.004 |
| Systolic blood pressure, cmHg | 9.79 ± 0.78 | 9.74 ± 0.88 | 0.736 |
| Diastolic blood pressure, cmHg | 6.14 ± 0.4 | 6.16 ± 0.41 | 0.818 |
| FBS, mg/dL | 75.43 ± 4.12 | 74.02 ± 4.66 | 0.93 |
| Age, yr | 38.75 ± 0.88 | 38.79 ± 0.73 | 0.871 |
aValues are expressed as mean ± SD.
As observed in Table 1, there was no statically significant difference between the two groups, except in weight at baseline. The mean age of all participants was 38.77 ± 0.809 years ranging from 37 to 40.
The changes of systolic blood pressure between the garlic and placebo groups in the first and second months of follow-up were not significant (P = 0.51, P = 0.40, respectively).
Table 2 displayed no changes in FBS level between the two groups; in other words, FBS in the two groups did not change over time.
| Variable/Month | Group | P Value* | |
|---|---|---|---|
| Garlic | Placebo | ||
| Weight gain | |||
| 1 | 1.71 ± 0.59 | 1.96 ± 1.34 | 0.510 |
| 2 | 3.8 ± 0.74 | 3.5 ± 0.92 | 0.406 |
| Systolic blood pressure | |||
| 1 | 9.5 ± 0.63 | 9.6 ± 0.61 | 0.34 |
| 2 | 9.37 ± 0.67 | 9.6 ± 0.62 | 0.529 |
| Diastolic blood pressure | |||
| 1 | 6 ± 0.18 | 6 ± 0 | 0.317 |
| 2 | 6 ± 0.29 | 6 ± 0 | 0.154 |
| FBS, mg/dL | |||
| 1 | 76 ± 3.7 | 75 ± 3.3 | 0.217 |
| 2 | 76 ± 4.2 | 75 ± 2.8 | 0.847 |
aValues are expressed as mean ± SD.
Weight changes were not significant in the first and second months after the intervention in both groups (P > 0.05).
After the intervention, the blood pressure and FBS of both groups were in the normal range. The data showed that the blood pressure was in the normal range even after two follow-ups. In other words, preeclampsia was not reported in any of the groups.
5. Discussion
According to the current study, the administration of 800 mg/day of garlic capsules during the 3rd trimester of pregnancy in the high-risk women for preeclampsia (with a positive family history of preeclampsia) did not reduce the systolic and diastolic blood pressures and there was no significant difference between the placebo and intervention groups over time. The current study findings were consistent with those of the study by Ziaei and et al.; they found no significant differences in the means of systolic and diastolic blood pressures between the two groups. Also, in the intervention group, there was no significant difference in the means of total cholesterol, high-density lipoprotein (HDL), low-density lipoprotein, and triglyceride before and after the experiment (27). A systematic review showed no difference between the two groups of garlic and control in developing the risk of gestational hypertension or preeclampsia. The complaints of undesirable odor in the garlic group were reported more than the other group (23).
Li et al., in a systematic review of 16 articles on the garlic effects on blood pressure changes showed that garlic can reduce blood pressure in the hypertensive and elevated systolic blood pressure cases, but had no effect on normal subjects. The administration of garlic reduced the total cholesterol, triglycerides, and HDL (34). Some studies provided insufficient evidence of the effect of garlic on hypertension, hypercholesterolemia, cancer, colds, peripheral arterial disease, and preeclampsia compared with placebo (34-36).
Some researchers describe that consumption of garlic had an antihypertensive effect in both human and animals; however, this effect was slight (37-39). But in the current study, in both groups, the systolic and diastolic pressure changes were not significantly different during the two follow-ups. It seems that garlic consumption was not effective in reducing the blood pressure in the pregnant women with a positive family history of preeclampsia. According to the findings of other studies, garlic was effective in reducing FBS (40, 41), but in the present study, the changes of FBS had no significant difference between the garlic and placebo groups during the two follow-ups.
5.1. Conclusions
The changes of systolic and diastolic blood pressure between the two groups of garlic and placebo were not significant after one and two months of intervention; it seems that administration of garlic to high-risk pregnant women was not effective in decreasing blood pressure. Therefore, it does not prevent preeclampsia in patients with a positive family history of preeclampsia.
Further studies should be conducted to identify the proper dose and duration of garlic use, and its effect on different ethnics and races in different physiological and pathological conditions.
5.2. Limitations
Small sample size had the risk of selection bias and limited generalizability. Also, since the study included the pregnant women with first-degree family history of preeclampsia (sister or mother), it was not possible to assess the effect of garlic consumption on preeclampsia or other biomarkers of systemic inflammation and oxidative stress. In addition, the beneficial effects of the maternal garlic supplementation on the biochemical indicators of newborns were not assessed.