1. Introduction
Behçet’s syndrome or Behçet’s disease (BD) is characterized by recurrent oral aphthae and any of the manifestations, including genital aphthae, ocular disease, vascular disease, skin lesions, gastrointestinal involvement, neurologic disease, or arthritis (1). The common site of genital ulcers is the scrotum in male patients and the vulva in female patients (2). The painful recurrence of genital ulcers in men or women can affect the quality of life of genital health (2). Genital ulcers are regarded as a major manifestation of BD. They are also the most specific (95%) mucocutaneous sign of BD and are observed in 50 - 85% of BD patients (3). Diagnosis is primarily based on the International Criteria for Behçet’s Disease (ICBD) derived from an evidence-based protocol (4). Herein, we report a case of atypical presentation of BD with a large severe acute genital ulceration to increase physicians’ awareness of this manifestation to avoid delay in diagnosis, the occurrence of severe complications, and the alteration of the quality of life.
2. Case Presentation
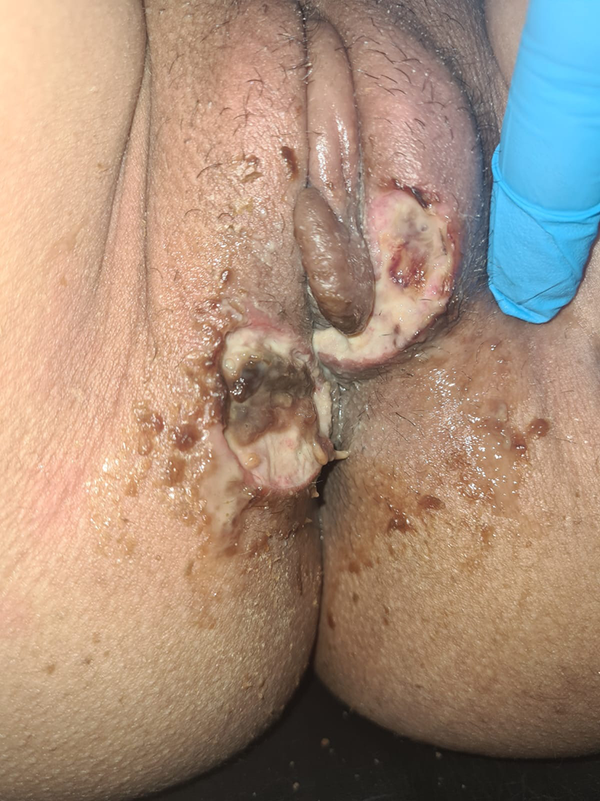
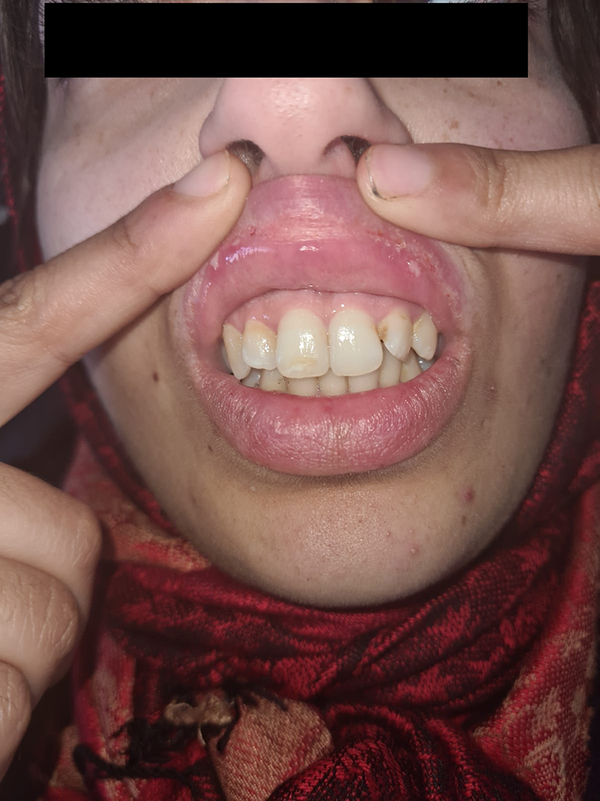
A 29-year-old unmarried woman with a history of recurrent oral aphthae presented to the dermatology department with a first episode of genital ulcer developed 2 weeks before admission, 3 months after unprotected sex with only one partner. It was treated as a sexually transmitted infection but without any improvement, and serological tests for syphilis, human immunodeficiency virus (HIV), and hepatitis B and C were negative. On clinical examination, there were two large painful ulcerations (Figure 1); the first one was oval and well-demarcated with a fibrinous and hemorrhagic center, located on the left labia majora; the second one was rounded and well-demarcated with a fibrinous center, located on the lower part of the right labia majora and the inner side of the right thigh, without inguinal lymphadenopathy or urethral discharge. There were also painful oral ulcers, rounded with a size of a few millimeters to 1 cm; they had well-defined margins, a white base, and surrounding erythema. (Figure 2) There were non-follicular pustules on the face (Figure 2) and limbs and painful edema on the left leg, with positive Homan’s sign.
The D-dimer level was elevated, and a Doppler ultrasound revealed deep venous thrombosis of the right common femoral, femoral, and popliteal veins. The diagnosis of BD was made according to the ICBD based on the findings, including genital aphthosis (two points), oral aphthosis (two points), skin lesions (one point), and vascular manifestations (one point). The patient was treated with prednisone 40 mg/day and colchicine 1 mg/day, and the lesions developed well and healed within 2 weeks, leaving scarring lesions in the genital area.
3. Discussion
The BD is a vasculitis with multisystemic involvement of unknown etiology (1). It is ubiquitous but more common in the Mediterranean region and Japan (5). It mainly affects young and middle-aged adults, with no gender predominance. In the absence of a biological, histological, or radiological pathognomonic marker, the diagnosis is made based on clinical criteria (4). The ICBD is a point-based system used to diagnose the disease. The criteria included recurrent oral ulcerations observed by a physician or patient, occurring ≥ three times in a year (two points), recurrent genital ulcerations (two points), eye lesions (two points), skin lesions (one point), central nervous system involvement (one point), vascular manifestations (one point), oral aphthosis (two points), and genital aphthosis (two points). In the pathergy test, if used (one point), patients scoring ≥ four points are classified as having BD (4). Genital ulcerations, the most specific lesions of BD, occur in 50 - 85% of patients with BD. The ulcers resemble oral aphthae in appearance and are usually painful. Genital ulcers most commonly occur on the scrotum in men and the vulva in women. Recurrences are usually less common than with oral ulcers. Scarring is common with genital lesions. Scarring of the scrotum as a result of ulceration is rarely, if ever, observed in conditions other than BD (3).
Aldeen reported the case of a 19-year-old female with recurrent oral aphthosis for 3 years who was consulted for multiple tender punch-out genital ulcerations for 5 days. The pathergy test was positive, and the result of a skin biopsy from the ulcers was consistent with BD that developed well after treatment with prednisone 40 mg/day (6). Marfatia et al. reported the case of a 29-year-old male who was consulted for multiple orogenital aphthae developing for a year and a half and treated for uveitis. Syphilis serology and HIV test were negative, and BD was diagnosed according to the criteria, including oral aphthosis (two points), genital aphthosis (two points), and skin lesions (one point) (7). It is important to consider the possibility of BD as an etiology for genital ulceration, even in cases where the lesions appear suddenly and are severe, especially if other criteria of the disease are present. Recurrent genital ulceration is not always present in BD (8).
The treatment of genital ulcers depends on the severity of symptoms and the presence of other disease manifestations. For isolated lesions, topical corticosteroids are sufficient; for oral aphthae and genital ulcers that do not respond to topical therapy, systemic glucocorticoids are recommended (9). Colchicine or apremilast is recommended to prevent recurrent oral and genital ulcers (10). Other therapeutic options might also be prescribed, such as thalidomide, interferon alfa, cyclosporine, tumor necrosis factor-alpha inhibitors, and azathioprine, depending on the presence of other organ involvement (6).
During the initial evaluation of a patient with genital ulcers, they should be evaluated for the presence of a sexually transmitted infection. These infections are the most common cause of genital ulcer disease (GUD). In addition, genital ulcers increase the risk of contracting HIV. Empiric treatment is often initiated based on history taking and physical examination because test results are often not immediately available and/or some tests have low sensitivity. In some patients, the evaluation is negative, and/or they do not respond to empiric therapy. In these patients, further evaluation for less common sexually transmitted causes of GUD and non-sexually acquired causes of GUD, including BD, might be required (11).
3.1. Conclusions
Behçet's disease is a nonvenereal cause of genital ulceration. The disease is characterized by recurrent oral and genital ulcers, skin lesions, and ocular inflammation. Mucocutaneous lesions constitute the hallmark of the disease, and a high index of suspicion in a patient with these lesions might result in the early diagnosis, management, and prevention of complications.