1. Introduction
Discoid lupus erythematous (DLE), the most common form of chronic cutaneous lupus erythematous is characterized by patches of persistent erythema, adherent scaling, follicular plugging and, in later stages scaring and atrophy (1, 2).
These lesions persist for years and tend to expand slowly. Biopsy of DLE lesions shows hyperkeratosis, follicular plugging, and atrophy of the epidermis; hydropic degeneration of basal keratinocytes; and a mononuclear cell infiltrate adjacent to epidermal, adnexal, and micro vascular basement membranes (3). Treatment is focused on control of local cutaneous disease and consists mainly of photo protection and topical treatment with glucocorticoids, immune modulators including Elidel and Protopic, intra-lesional glucocorticoids and oral medications including antimalarials, Thalidomide and Dapsone. If local therapy is ineffective, use of aminoquinoline antimalarials may be indicated (4, 5).
High power lasers including PDL have been used for treatment of chronic refractory lesions of discoid lupus erythematous since 1986 (6). We herein report, the first case of DLE treated with specific low-level laser therapy.
2. Case Prtesentation
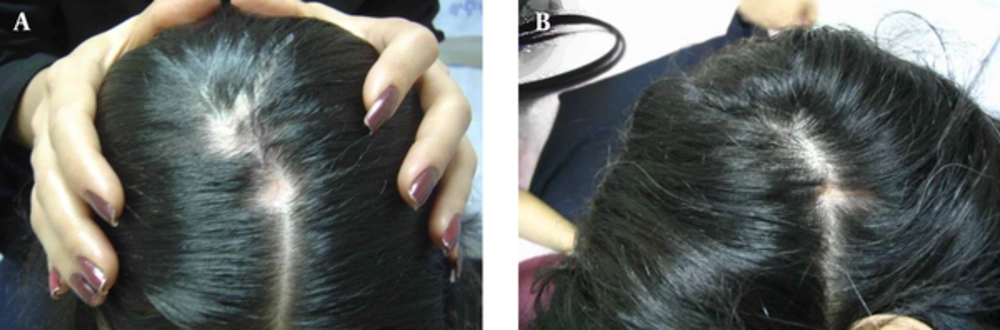
The case was a 33-year-old female with six years history of DLE, who was referred to the laser clinic of Milad hospital (2009) with acute flare of skin lesions since seven months ego. She had four lesions (three with local alopecia, scaling and itching and one with atrophy) on the scalp (Figure 1A).
The histological examination of lesions supported the clinical diagnosis of DLE. Serological investigations for antinuclear antibodies, anti Ro/SS-A antibody, erythrocyte sedimentation rate (ESR), rheumatoid factor (RF) were negative. However, anti ds-DNA antibody was positive. The patient showed no signs of underlying systemic illness manifestations. Her skin lesions were under control with standard therapies including local corticosteroids and antimalarial drugs (hydroxychloroquine 200 mg/day) for several months, however after withholding antimalarial drugs because of pregnancy and breastfeeding period, the lesions flared up during and subsequent to pregnancy. Intra-lesional injections of corticosteroids (diluted triamcinolone acetate, 4 mg/mL) and antimalarial therapy were started. However, there was no response from skin lesions on the scalp during about seven months of corticosteroid oral therapy.
We used a combination of low-level laser therapy using local irradiation of lesions with infrared and red light diode laser (830 nm, 200 mw; and 630 nm, 20 mw, respectively; each 6J/cm2; Mustang 2000, Moscow, Russia) in addition to intravenous red light laser (655 nm, 2 mw for 20 minutes). Intravenous laser therapy was done using a fiber optic laser conduit inserted via a needle placed on the forearm in median cubital vein. We also used laser acupuncture with infrared diode laser (1 J/cm2 Mustang 2000, Moscow, Russia) for LI-11, LI-4, SP-6, PC-6, ST-36 and GB-34 points. All three methods of laser therapy (local irradiation, intravenous laser and laser acupuncture) were done every other day. Corticosteroid was discontinued because of its inhibitory effect on laser therapy, but the patient continued using hydroxychloroquine. After five sessions of treatment, the beneficial effects started to appear as reduction in itching and disappearing of erythema, and after 10 sessions, itching of the lesions discontinued. During the one-month follow up, the patient was symptom free and medications were discontinued. Three months later, the patient had itching at the same affected area. The LLLT with the same protocol was done for 12 sessions (phase 2).
3. Discussion
Through a total of 27 sessions of treatment, the lesions improved completely with highly satisfactory results; and one month after LLLT, as the patient was symptom free, drug-therapy was continued. Alopecia resolved completely and the atrophic lesion improved moderately (Figure 1B). After three months, the lesions flared up again with itching and scaling. A second therapeutic course was done using the same protocol for 12 sessions. During the one-year follow up after the second treatment course, there was no recurrence without any medication.
Discoid lupus erythematous is a chronic inflammatory skin condition notorious for causing disfiguring scars and alopecia. Since 1986, lasers have been introduced as an alternative treatment approach for refractory skin lesions of DLE (6-8). However, lasers already been used for treatment of these lesions have been high power lasers with varying amount of adverse effects (9) (Table 1).
| Year | Authors | Indications | Type of Laser | Response | Reported Side-Effects |
|---|---|---|---|---|---|
| 1986 | Henderson et al. | DLE | CO2 | Dramatic clinical and cosmetic improvement | Splotchy hypo pigmentation |
| 1988 | Zachariae et al. | DLE | Argon | Highly satisfactory | Slight scarring and an insignificant pigmentation |
| 1996 | Nurnberg et al. | DLE | argon | Dramatic impact in contrast to untreated lesions | Hypo pigmentation |
| 2000 | Kuhn et al. | DLE | argon | Complete resolve | No short-term side-effects |
| 2001 | Tremblay JF, Carey W | DLE | Erbium: YAG | Remarkable cosmetic improvement | No side-effects during two years |
| 2003 | Baniandres et al. | DLE, CLE | FDPL, LDPL | An average improvement in over 60% of patients | Transient hyper pigmentation, light scarring |
Treatment of Discoid Lupus Erythematous With Laser; Review of the Literature
The primary concept for use of lasers in treating these lesions was the coagulative ability of high power lasers for blood vessels ablation and vaporization of lesions in the affected areas (6, 10, 11). However, the fact has been neglected that these lesions are sensitive to high power light irradiations such as long-standing sun exposure, UVA or UVB irradiations (7) and high power laser irradiation can also proceed the activity of disease along with other side effects such as hyper and hypo pigmentation of the lesions because of exceedingly coagulated vessels in the region and the resulting superficial ischemia.
Rather, it seems that photosensitivity of these lesions depends on various factors especially presence of some autoantibodies such as anti Ro/SS-A autoantibody (12). However, none of the previous reports have emphasized the presence of such antibodies before starting the treatment with laser irradiation.
Presence of discoid skin lesions in the process of lupus seems to be an immunological process with mononuclear cell infiltrate adjacent to epidermal, adnexal, and micro vascular basement membranes and immunoglobulins and complement deposits at the basement membrane zone in about 90% of cases (3).
One of the most important functional aspects of laser therapy is photobiostimulation effects of low-level lasers on various biological systems especially immunological system, which is based on the effects of low intensity lasers, often described as lasers with less than 500 mw average power (13-17).
Low-level laser irradiation is characterized by its ability to induce non-thermal, non-destructive photo biological process, which is collectively referred to as “biomodulation” (18). Biomodulation by low level laser therapy (LLLT) has become popular as a therapeutic modality for the acceleration of wound healing and the treatment of inflammation (19). It is important to differentiate between LLLT and high-intensity laser treatment, in which heat and thermal cell damage are generated. The exact mechanism by which LLLT works is yet to be understood. However, apparently there is no linear relationship between the wavelength or dosage of LLLT and the type of photochemical reaction that it causes; depending on the target cell’s physiologic status, light irradiation seems to induce either stimulatory or inhibitory effects (18).
On the other hand, LLLT appears to have immunomodulatory potential. Dyson et al. (20) investigated the effect of several energy densities of LLLT on human T-lymphocyte proliferation in vitro. Mitogen-treated cell proliferation was inhibited by all the energy densities. Interestingly, non-stimulated cells were only inhibited by higher densities in the range of 10.8 - 13.2 J/cm2, while lower densities actually stimulated their proliferation (1.2 - 3.6 J/cm2). In another study, Dima et al. (21) investigated the effects of low-level laser (GaAlAs diode laser; 830 nm) on serum opsonic activity. They found that LLL irradiation had no effects on serum opsonic activity, but significantly higher values were observed at the highest dose tested (60 mw for one minute) in the absence of myeloperoxidase (MPO) inhibitor NaN3.
To the best of our knowledge, this is the first case report on the use of LLLT for the treatment of DLE. Our case, although flared after three months of withholding laser therapy, showed initial improvement without serious side effects, after six years of persistent refractory lesions and re-improvement of the lesions subsequent to second phase of therapy, fell us in doubt if we could use low-level laser therapy alone in place of drug-therapy in such refractory cases of discoid lupus erythematous, successfully. Overall, after about one year of the second therapeutic phase, the patient is still well without any medication. This encourages us to propose further clinical trials to determine the efficacy of this new modality of treatment for discoid lupus erythematous.