1. Background
Hemangioma is the most common benign tumor in childhood, with an overall prevalence of 2 to 3% in neonates, 10% in less than one-year-old children, and 22% to 30% in premature low birth weight infants (1-3). The definitive etiology of hemangioma remains unknown, although gestational age, gestational blood pressure, and birth weight have been reported to be associated with hemangioma (4). Many previous confusions about vascular lesions were related to their classification systems. In 1982, Mulliken and Glowacki classified congenital vascular moles into two main categories: hemangiomas and vascular malformations (5). In another classification system developed by Waner and Suen, hemangioma was classified as superficial hemangiomas (located in the papillary dermis), deep hemangiomas (located in the reticular dermis or subcutaneous tissue), and hybrid type (both superficial hemangiomas and deep hemangiomas) (6). Hemangioma is mainly characterized by the proliferation of endothelial cells and can be subdivided into the rapid proliferation phase (0 to 1 year), involvement phase (1 to 5 years), and involved phase (5 to 10 years) (7).
With the spontaneous return of hemangiomas, treatment choice is still controversial. These hemangiomas are not usually life-threatening or functional disabling but can cause various physiological problems due to deformities such as low self-esteem, impaired quality of life, and depression (8). Also, it seems that 40 to 50% of all hemangiomas that heal incompletely may accompany with some skin abnormalities such as telangiectasia, stippled scarring, anetoderma, or epidermal atrophy.
Also, delayed problematic hemangiomas can lead to major deformities or even life-threatening conditions. It is recommended to use active treatment instead of conservative observational measures to avoid the defects and deformities caused by the disease (8). With the advancement of modern technology, active therapies not only have specific therapeutic effects but also could improve the patient's quality of life (9). Recent treatments for neck and head hemangiomas mainly include medication, laser therapy, and surgery. Overall, the treatment approaches for hemangioma should be personalized depending on the initial symptoms, defects' severity, and the lesion's growing phase. There is no suitable "gold standard" treatment for all patients, and multidisciplinary management is often required for best performance (10).
The purse-string suture for surgical skin lesions was first introduced in 1985 (11). It is a technique for closing surgical sutures or postoperative circular lesions (12, 13). The proponents of this technique believe that this method is associated with less scarring, shorter wound healing time, faster homeostasis recovery, and ultimately improved beauty-related consequences than other suture closure methods. This method is also equal to other methods in cost-effectiveness (14). Regarding dermatological surgeries, various studies have been published on the benefits or limitations of the purse-string method, but there have been very few studies comparing the consequences of this method with other methods, such as laser coagulation. For example, due to its high effectiveness and low side effects, the 595-nm pulsed dye laser coagulation method has received much attention (15). This method has been widely used, especially in treating facial vascular malformations, which need to accelerate recovery, especially from an aesthetic point of view. However, epidermal burns, post-inflammatory pigment changes, and scarring are possible in such a procedure. What remains a fundamental question is the best repair method for surgical sutures after surgery for vascular lesions, including hemangioma. In this regard, which one can lead to the highest level of patient satisfaction: purse-string, coagulation use, or a combination of both? Apart from the role and effect of each treatment procedure, the ultimate goal of using such treatments is to improve the appearance of lesions, patients' satisfaction, and quality of life in the long term.
2. Objectives
The present study aimed to evaluate the outcome of different therapeutic procedures in patients suffering from facial vascular malformations regarding long-term satisfaction, quality of scars, and quality of life.
3. Methods
3.1. Study Population
This self-control before-after interventional case series study was conducted on consecutive patients with congenital vascular lesions, including hemangiomas or facial vascular malformations, referred to Al-Zahra Hospital in Isfahan, Iran, between 2017 and 2019. The inclusion criteria were the presence of congenital vascular lesions, including hemangiomas and vascular malformations, on the face in patients aged 20 to 50 years. In this regard, age under 20 or over 50 years, co-existence of other pathological inflammatory or infectious skin lesions, history of chronic diseases such as liver or kidney disease, a recent history of using corticosteroids or anti-inflammatory drugs, and a history of any therapeutic or aesthetic interventions on the face were the exclusion criteria.
3.2. Surgical Procedures
The following surgical techniques were employed to improve the patients' lesions: purse-string methods, excision and graft, excision and flap, coagulation and cautery ablation with a catheter, and/or tissue expander and flap. Depending on the anatomical area of the lesion, one or more techniques were used to improve the lesions.
3.3. Study Tools and Measurements
Prior to surgery, baseline assessments, including gender, age, clinical and medical history, and status of the lesion (the size of the site involved and the location of the lesions according to facial beauty units), were done by interviewing and physical examination by two plastic surgeons (the study researcher and a non-intervening person) with an acceptable agreement between them (Kappa value of 0.86). Patients were fully explained how to perform the surgery, and their written consent was obtained. They were treated with one of three methods, including purse-string methods along with coagulation, excision and graft, and ablation catheter (although the type of surgery and the number of surgeries might differ for the patients).
Before surgery and at intervals of one week, three weeks, six weeks, three months, and six months after surgery, the subjects were evaluated in terms of (1) satisfaction with the aesthetic appearance of the scar assessed based on the Visual Analog Scale (VAS) ranged between 0 (completely dissatisfied) and 10 (completely satisfied); (2) the quality of scars caused by these treatments was assessed using the Stony Brook Scar Evaluation Scale (SBSES) (16) and interpreted by the two plastic surgeons. The SBSES was initially proposed in 2007 by Singer et al. and is a six-item ordinal wound evaluation scale developed to measure the short-term cosmetic outcomes of wounds five to 10 days after injury up to the time of suture removal. It incorporates the assessments of individual attributes with a binary response (1 or 0) for each, as well as overall appearance, to yield a score ranging from 0 (worst) to 5 (best) (17); (3) significant improvement of procedural outcome assessed based on patient-reported outcome measures (PROM) including five questions related to pain/discomfort, mobility, looking after myself, doing daily activities, and feeling worried. Each question was rated as 0 (no problem), 1 (some problem), or 2 (a lot of problems) (18); (4) the quality of life was assessed based on the 17-item Wound-QoL questionnaire, which includes items of physical disorder, local movement disorder, physical condition, psychological disorder, feeling of disability, daily activity disorder, social dysfunction, dependence on others, treatment disorder, and the financial burden (19). The items in this inventory ranged from 0 (not at all) to 1 (a little), 2 (moderate), 3 (quite a lot), and 4 (very much), and a higher total score indicated a poorer wound-related quality of life (20). The items of the questionnaire were structured in three subscales of "body" (items 1 to 5), "psyche" (items 6 to 10), and "everyday life" (items 11 to 16). Item 17 does not belong to either of the subscales. The total score ranged from 17 to 85; a higher score indicates a poorer quality of life (20).
Finally, the trend of changes in the scores during the six months of follow-up was evaluated and compared between different treatment techniques. The study was ethically approved by the ethics committee of Isfahan University of Medical Sciences (IR.NUI.MED.REC.1399.335)
3.4. Statistical Analysis
For statistical analysis, the data were presented as mean ± standard deviation (SD) for quantitative variables and were summarized by frequency (percentage) for categorical variables. Continuous variables were compared using t-test or Mann-Whitney test whenever the data did not appear to have normal distribution or when the assumption of equal variances was violated across the study groups. The trend of the change in the quantitative scores was assessed by the Repeated Measures ANOVA. P-values of ≤ 0.05 were considered statistically significant. SPSS version 23.0 for Windows (IBM, Armonk, New York) was used for statistical analysis.
4. Results
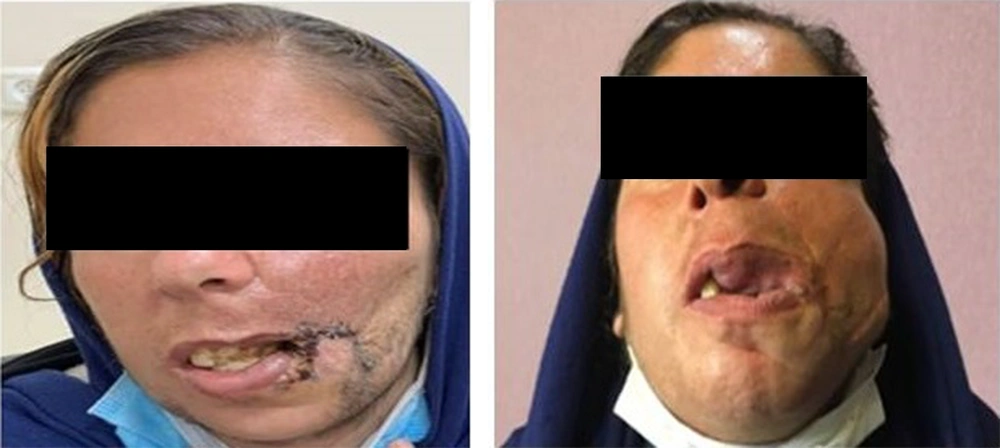
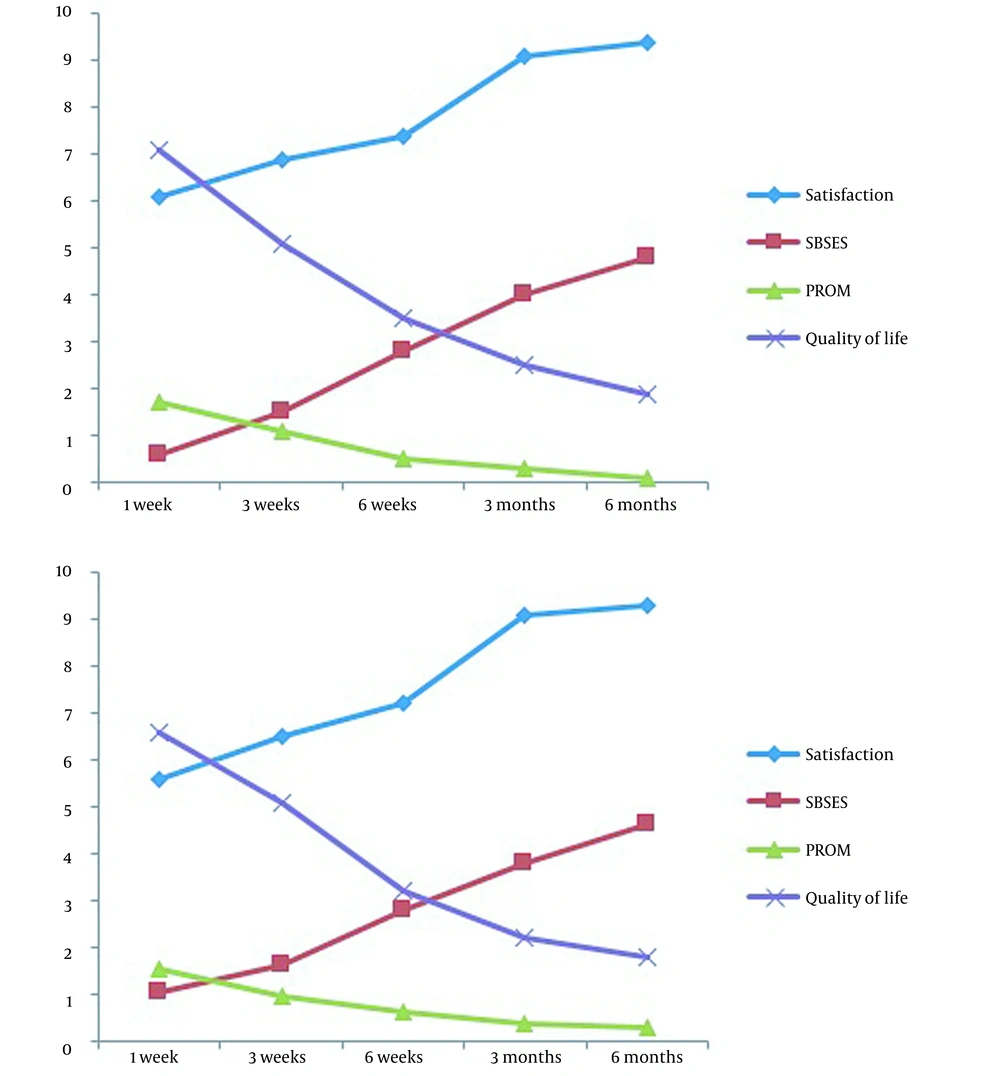
In total, 60 patients suffering from facial vascular lesions were evaluated. The average age of the participants was 30.43 ± 8.24 years, and 83.3% were female. The mean size of the lesions was estimated to be 15.48 ± 1.25 cm. Regarding the location of lesions, 38.3% were localized on the chin, 3.3% on the cheek, 23.3% on the forehead, and 5.0% on the ocular surface. As indicated in Figure 1, the sizes of scars were significantly reduced in all studied patients following the therapeutic, surgical procedures. Assessing the patients' satisfaction over time (Table 1) showed an upward trend from the first week of treatment until six months. In this regard, the mean satisfaction score in the first week was 5.68 ± 1.17, which significantly rose to 9.35 ± 0.71 six months after the therapeutic interventions. The assessment of the quality of scars by SBSES also revealed significant improvement in postoperative scars within the six months after treatment (Table 1). In this regard, we assessed different aspects of the six-month quality of scar that showed improvement in scar width less than 2 cm in all patients, flatting the lesions in 88.3%, the same color of the lesion with the surrounding skin in 91.7%, absent hatch/suture marks in 95.0%, and good overall appearance in 90.0% of the participants. In Table 1, the mean PROM score significantly reduced over time from 1.57 ± 0.5 at one week to 0.27 ± 0.44 at six months of initial treatments. In this regard, six-month PROM results showed no pain/discomfort condition in 98.3%, no problem in walking in 96.7%, no problem in self-care in 91.7%, proper daily activities in 90.0%, and complete lack of worry in 96.7%. Also, the assessment of the patient's quality of life using the Wound-QoL tool (Table 1) showed a significantly improved quality of life score, as the overall score significantly reduced from 67.63 ± 11.02 at one week to 18.85 ± 2.34 at six months after the initial treatment. The trends of the changes in all study parameters were found to be significant in both men and women. Using the multivariable linear regression models (Tables 2 - 4), the trend of the significant changes in all parameters related to scar healing was independent of baseline characteristics, including gender, age, size, and location of the lesions. In this regard, the changes in the study parameters were independent of patients' sex, similar in men and women (Figure 2).
| Parameter | 1 Week | 3 Weeks | 6 Weeks | 3 Months | 6 Months | P-Value |
|---|---|---|---|---|---|---|
| Mean satisfaction score | 5.68 ± 1.17 | 6.57 ± 0.98 | 7.20 ± 0.87 | 9.08 ± 0.86 | 9.35 ± 0.71 | < 0.001 |
| Mean SBSES score | 0.98 ± 0.85 | 1.62 ± 0.66 | 2.78 ± 0.64 | 3.82 ± 0.59 | 4.67 ± 0.51 | < 0.001 |
| Mean PROM score | 1.57 ± 0.50 | 0.98 ± 0.56 | 0.60 ± 0.55 | 0.38 ± 0.49 | 0.27 ± 0.44 | < 0.001 |
| Mean QOL score | 67.63 ± 11.02 | 51.47 ± 10.28 | 32.95 ± 8.02 | 23.05 ± 4.76 | 18.85 ± 2.34 | < 0.001 |
The Trend of Changes in Parameters Related to Postoperative Outcomes
| Source | Type III Sum of Squares | Mean Square | F | P-Value |
|---|---|---|---|---|
| Intercept | 50.859 | 50.859 | 47.366 | 0.000 |
| Gender | 0.079 | 0.079 | 0.074 | 0.787 |
| Age | 1.009 | 1.009 | 0.940 | 0.337 |
| Size | 1.959 | 1.959 | 1.825 | 0.182 |
| Location | 2.242 | 2.242 | 2.088 | 0.154 |
Six-Month Postoperative Changes in Stony Brook Scar Evaluation Scale Score in Patients Suffering from Hemangioma Independent of Baseline Variables
| Source | Type III Sum of Squares | Mean Square | F | P-Value |
|---|---|---|---|---|
| Intercept | 2.463 | 2.463 | 3.555 | 0.045 |
| Gender | 0.033 | 0.033 | 0.048 | 0.828 |
| Age | 0.030 | 0.030 | 0.044 | 0.835 |
| Size | 0.007 | 0.007 | 0.010 | 0.922 |
| Location | 0.116 | 0.116 | 0.168 | 0.683 |
Six-Month Postoperative Changes in Patient-Reported Outcome Measures Score in Patients Suffering from Hemangioma Independent of Baseline Variables
| Source | Type III Sum of Squares | Mean Square | F | P-Value |
|---|---|---|---|---|
| Intercept | 9447.280 | 9447.280 | 54.955 | < 0.001 |
| Gender | 74.724 | 74.724 | 0.435 | 0.512 |
| Age | 650.798 | 650.798 | 3.786 | 0.057 |
| Size | 375.485 | 375.485 | 2.184 | 0.145 |
| Location | 92.411 | 92.411 | 0.538 | 0.467 |
Six-Month Postoperative Changes in Quality of Life Scores in Patients Suffering From Hemangioma Independent of Baseline Variables
5. Discussion
At the beginning of the study, we hypothesized that lesions and malformations such as facial vascular malformations due to hypervascularity leave far fewer scars after surgery and repair. Therefore, patient satisfaction and quality of life will improve optimally compared to other lesions. In this regard, we assessed six-month postoperative outcomes (regardless of the type of procedure) in terms of patients' satisfaction with the procedure, patients' viewpoints on his/her appearance and daily activities, quality of the postoperative scar, and patient quality of life. We found considerable improvements in all postoperative outcome-related parameters following surgical approaches. In other words, apart from baseline characteristics of patients and lesions (size or location) and procedural characteristics, these lesions were significantly improved from the first weeks of the treatment intervention. This confirms that for treating such postoperative lesions, especially scars after surgery, there is no need to use further reconstructive interventions or readmit the patients. In addition, considering the importance of these scars from a psychological point of view and their potential impact on patients' mood characteristics, it seems that treating these lesions with primary minimal invasive measures can be effective in the shortest possible time on psychological aspects and dissatisfaction with the treatment procedure. In a similar observation by Cheng et al. in 2019 (21), surgical excision of skin hemangioma and subcutaneous tissue could lead to no appearance of surgical site infection, nerve injury, mortality, sepsis, septic shock, or bloodstream infections. As Demiri et al. in 2001 (22) showed, although facial hemangiomas might cause significant functional disturbance or severe psychological distress, surgical excision early surgery could provide active treatment with excellent results and minimal morbidity. In another experiment by Li et al. (23) on patients who underwent surgical excision of upper and lower lip hemangiomas, it was found that the procedure was accompanied by minimal complications and a high degree of parent satisfaction. Early conservative and even invasive treatments may prevent symptoms and functional problems arising from proliferative lesions in such tumors, especially facial types that have annoying appearances. Various therapeutic approaches have been developed in this regard, but these methods are not very acceptable due to severe procedural complications such as ulceration, sclerotic scaring, tissue atrophy, or radionecrosis. We could also show that common treatments, including purse-string methods, coagulation, excision and graft, and ablation catheter, lead to favorable outcomes regarding appearance and physical and psychological sequels. Nevertheless, in general, we believe that the main reason for the surgical recovery in these lesions is their vascularity. In fact, it will be possible to repair the lesion faster due to the faster rate of endothelial production of anti-inflammatory factors and tissue repair in such lesions.
5.1. Conclusions
Different surgical techniques can achieve favorable postoperative outcomes in patients suffering from facial vascular malformation, independent of the patient's baseline characteristics and procedural techniques. This improvement can be obtained in different aspects, including patient satisfaction with cosmetic consequences, functionality, quality of scars, and patient quality of life.