1. Background
Postoperative pain has many adverse effects on the patient. If not controlled properly, it can lead to a wide range of problems, such as pneumonia, DVT, infections, cardiac ischemia, and skin ulcers, and may even become a chronic symptom (1).
The use of a pain pump is an appropriate method for relieving postoperative pain. Using opioids for pain control can cause a wide range of complications, such as nausea and vomiting, respiratory depression, sedation, and intolerance; in this regard, adjuvant drugs have been introduced to reduce the need for opioids and improve the quality of analgesia (2). They can be helpful, especially in patients with a history of narcotic use; they show little response to the opioids and, therefore, need a higher dose of the pain control drugs, which deteriorates the symptoms.
In general, the approach to the pain pump and multi-drug combination, which have fewer complications, has increased attention to adjuvant drugs (3).
Today, vein acetaminophen with apotel brand as an adjuvant drug is one of the most commonly used drugs to control pain in operating rooms and inpatients.
Furthermore, apotel is an antiemetic drug which acts by the prevention of the secretion of prostaglandins in the CNS; prostaglandins have a direct effect on the Temperature Control Center in the hypothalamus which in turn resulted in the reduction of the anti-inflammatory effects of the environment, as well as reduction of fever. Overall, apotel is used to control short-term pains with mild to moderate strength, especially after surgery, hyperthermia treatment, and emergency pain management (4).
Research shows that ketamine is a fast-acting anesthetic used for anesthetic, tranquil, and analgesic; it has high safety margins with an antagonistic effect on the NMDA receptor; the latter prevents CNS sensitivity to painful stimuli, and reduces in postoperative pain (5).
Ketamine has not been used for a long time for pain control, due to its possible complications, such as neurotoxicity, delirium, and its negative effects on memory. Owing to new studies which have clearly shown the mechanism of action and effects of relieving pain and analgesia at low doses, apotel is now considered again as the part of a multidrug approach in almost all surgical spectra (6-11). Postoperative pain can be a serious problem in patients undergoing spinal fusion surgery, because it may bring about extensive damage to the soft tissue, bones, and muscles.
The present study compared the analgesic efficacy and safety of intravenous ketamine infusion for pain management with intravenous infusion apotel in spondylolisthesis who underwent lumbar spinal fusion. The instrumentation was also evaluated (12).
2. Objectives
Accordingly, this study provides a comparative analysis of the effects of ketamine and apotel in pain pump on controlling the postoperative pain in posterior spine fusion surgery.
3. Methods
Approved by the Ethics Committee of Iran University of Medical Sciences under the register code of IRCT20190430043430N1, the present study was conducted under a double-blind randomized clinical trial environment.
It consisted of 72 patients hospitalized in 2018 for posterior spinal fusion surgery. The samples were selected through a convenient sampling technique. All the participants met the inclusion criteria.
To calculate the sample size, we used the formula provided by Kaur (13): assuming a difference of 2 in the VAS score of 6 hours after the surgery in the two groups (6 and 4) and the standard deviation of 3, alpha 0.05, and the test power of 80%, the below formula provided the sample size of 36 for each group.
Neither the evaluator nor the patients were aware of the type of intervention. The patients were randomly divided into two groups by a third person who was not familiar with the design selecting envelopes for the groups.
3.1. Inclusion Criteria
Participants’ age range of 20 - 50 years old, ASA2-1, non-addiction and non-smoking, BMI < 35. They were asked to sign the consent form.
3.2. Exclusion Criteria
Patients with a history of seizure, psychosis, and memory disorders were excluded from the study.
The included patients were subjected to general anesthesia under the anesthetic method with midazolam anesthesia 0.02 mg/kg and fentanyl 3 µg/kg; they underwent standard monitoring, including electrocar diogram pulse oximetry, and blood pressure measuring. Also, the patients were hydrated with an infusion of 5 mL/kg of 0.9% saline. The blood transfusions and fluid therapy were calculated via standard methods and induction with thiopental 5 mg/kg and cisatracurium 0.2 mg/kg and lidocaine 1 mg/kg and under maintenance with 100 µg/kg propofol and 0.1 µm fentanyl. In the operating room, after extubation, for the ketamin group, 0.2 mg/kg of ketamine per hour was infused by a pain pump. If the pain persisted, the dose was repeated; if persisted again, the pain was controlled by morphine. To identify the side effects of ketamine, midazolam was used. The pain score was recorded based on VAS criteria from 1 to 10 points. In the apotel group, apotel was used instead of ketamine. If the pain persisted, pethidine and morphine were used similar to those in the ketamine group.
The pain pump was adjusted to 4 CC infusion per hour. The total dose of opioids was recorded in 48 hours, considering the patients’ weight.
The outcome measures encompassed VAS, the severity of sedation, and the patients' satisfaction with the postoperative analgesia. Finally, at the times of 6, 12, 18, 24, and 48 hours after the surgery, the severity of pain was measured by the Visual Analogue scale (VAS) (14); the scores was recorded by a third person who was unaware of the study design. The severity of sedation was measured using the Ramasy score (15). Patients’ satisfaction with the postoperative analgesia was also measured.
A simple random number generator was used for random allocations and measurements. Throughout the trial, researchers and nurses were blinded to the procedure wherever applicable. Moreover, the patients were allocated by a medical doctor who was not aware of the study design that was the one who recorded the variables and measurements.
3.3. Data Analysis
The data were analyzed running SPSS software. To report the quantitative variables, the mean ± SD was used. For the qualitative variables, the frequency and percent was used. For a comparative analysis of the quantitative variables in the two normally distributed groups, the t-test was utilized. For the qualitative variables, the chi-square test and nonparametric tests were used. In order to compare the changes in pain score in different postoperative hours in the two groups, repeated measures ANOVA test was used. A P value less than was considered significant.
4. Results
One pair of the samples with a total size of 72 patients, referred to the hospital in 2018 to undergo posterior spine fusion surgery, participated in the study. Half of the participants were assigned to the ketamine group and the other half were allocated to the apotel group.
The demographic data of the patients in the two groups are provided in Table 1. Accordingly, no significant differences were found in the two groups.
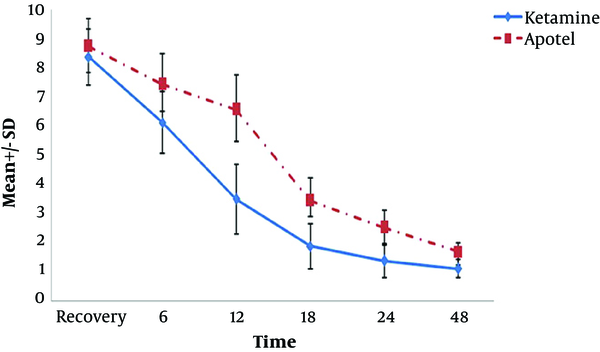
As shown in Figure 1, the mean score of the postoperative pain was lower in the ketamine group; this difference was statistically significant (P < 0.001).
According to Table 2, there was no significant difference between the postoperative pain score of the surgery in the two groups in recovery (P = 0.125). The post operative pain was significantly lower in the patients in the ketamine group than the apotel group (P < 0.001) at 6, 12, 18, 24 and 48 hours after the surgery.
| Variable | Apotel (N = 36) | Ketamine (N = 36) | P Value |
|---|---|---|---|
| Visual Analog scale | |||
| Recovery | 8.75 ± 0.9 | 8.38 ± 0.96 | 0.12 |
| 6 hour after operation | 7.44 ± 0.93 | 6.13 ± 1.07 | < 0.001 |
| 12 hours after operation | 6.58 ± 1.1 | 3.5 ± 1.2 | < 0.001 |
| 18 hours after operation | 3.44 ± 0.55 | 1.88 ± 0.78 | < 0.001 |
| 24 hours after operation | 2.52 ± 0.6 | 1.38 ± 0.59 | < 0.001 |
| 48 hours after operation | 1.69 ± 0.46 | 1.11 ± 0.31 | < 0.001 |
Visual Analog Scale in Terms of Two Groupsa
Table 3 shows that Ramsy score of the patients in two groups were not, significantly different (P = 0.16).
Table 4 shows the satisfaction rate of the patients with the analgesia in the two groups at 24 and 48 hours after the surgery. The satisfaction rate was significantly higher in the ketamine group than in the apotel group.
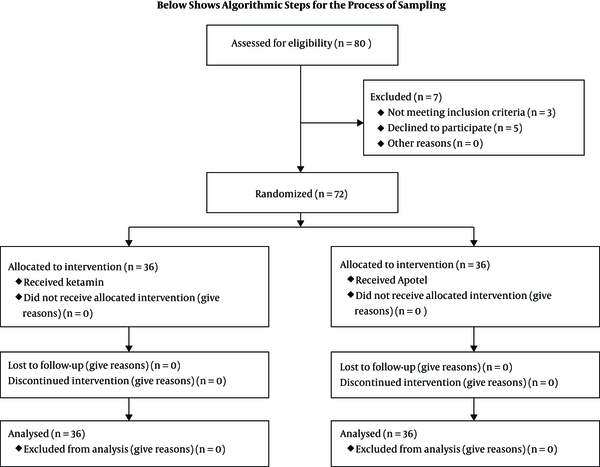
Nausea and vomiting, delusions, and other complications were not observed in any of the two groups. Figure 2 shows algorithmic steps for the process of sampling.
5. Discussion
Uncontrolled pain can influence the patient and cause various short-term and long-term problems, such as poor patient satisfaction, development of chronic pain syndromes, delayed postoperative recovery and patient mobilization, vein thrombosis, pulmonary embolism, psychological trauma, and ischemia. The most important finding of the present meta-analysis was that the intravenous ketamine infusion was associated with a significant reduction of postoperative pain compared with apotel infusion (P < 0.001). There was no significant difference between age, sex, BMI, underlying diseases, smoking in patients with posterior spinal fusion surgery in the two groups of ketamine and apotel. The minimum and maximum age were 15 and 69 years, respectively. The mean age of the patients was 6.63 ± 13.18 years in the apotel group and 43.83 ± 11.39 in the ketamine group. The finding showed no significant difference between the two groups in terms of age (P = 0.14). Out of 36 patients in the apotel group, 14 cases were women, and 22 were men. There were ten women and 26 men in the ketamine group. Furthermore, there was no significant difference between the two groups in terms of gender (P = 0.474). The results showed that the postoperative pain at 6, 12, 18, 24 and 48 hours after the surgery in the ketamine group was significantly lower than that of the apotel group. Also, the pain in both of the groups significantly decreased during recovery to 48 hours after the surgery. The rate of satisfaction with the analgesia in the patients, 24 and 48 hours postoperatively, in the ketamine group was significantly better than the apotel group. However, there was no significant difference between the Ramsy score of the patients in the two groups.
No adverse effects of nausea, vomiting, delusion, and other complications were found in ketamine and apotel groups.
The incidence of the pain in the patients undergoing posterior spine infusion surgery was relatively common; however, it was necessary to use a more extensive range of postoperative analgesic methods. Therefore, it is necessary to consider the conventional methods of postoperative analgesia (1, 2).
According to some reviews, the administration of ketamine and apotel can help control the amount of the pain after various surgeries (13, 16-18). T the best of our knowledge, no study has yet compared ketamine infusion pumps and applet fusion pumps for pain control after posterior spine fusion surgery. Kaur et al. (13) showed that the pain score in the first six hours after surgery in patients with open-ended cholecystectomy, under general anesthesia in low-dose ketamine infusion (0.2 mg/kg) during the surgery, was less than normal saline infusion (control group). At 12 and 24 hours after the surgery, there was no significant difference between the two groups. Morphine consumption in the ketamine group was lower than that in the control group. None of the patients had side effects, and the incidence of nausea and vomiting and satisfaction was similar in both groups.
A study by Faiz et al. (19) concluded that the pain level of the patients undergoing hysterectomy surgery, based on VAS criteria for recovery and 4, 6, 12, and 24 hours after the surgery in the group of 15 mg/kg venotic acetaminophen, was lower than 0.15 mg/kg ketamine group. This inconsistency could be due to the difference in the design and the type of surgery in the two studies. While in other studies with results consistent with the present study, there has been no significant difference between the Ramsy score of the patients in recovery and 4, 6, 12, and 24 hours after the surgery regarding side effects such as nausea and vomiting, respiratory problems; the drowsiness was not significantly different between the two groups.
Pestieau et al. (18) showed that pain, sedation score, and postoperative opioid use in pediatric patients with scoliosis in posterior spine fusion surgery in a low dose ketamine infusion group was similar with those in the saline group. Despite the insignificance of difference, Kim et al. (4), the results showed that the pain level was less than normal saline within 1 - 48 hours based on VAS in the patients undergoing surgery due to posterior spine inflammation in either ketamine (2 µg/kg/min or µg/kg/min 1, after a 0.5 to 0.5 µg/kg/min bolus dose). Moreover, there was no difference between the patients receiving ketamine and normal saline in terms of patient satisfaction and side effects. Hadi et al. (17) showed that pain levels were significantly lower in patients who received intravenous ketamine (1 µg/kg/min) 6, 12, and 24 hours after microedisecctomy in the ketamine recipient group (1 µg/kg/min) during and after the surgery. Also, pain in both groups of ketamine was lower than the normal saline group. The incidence of complications of nausea and vomiting in the control group was more than that of the two groups of ketamine. In a study by Mahmoodiyeh et al. (20) whose results were inconsistent with our results, the pain levels were observed in the patients undergoing surgery based on VAS criteria in recovery at 2, 6, and 12 hours, postoperatively, The controls were given fentanyl/ketamine (12 mg/kg and 3.6 mg/kg, respectively), and for the case group, fentanyl /paracetamol (12 mg/kg and 10 mg/kg, respectively) were used, applying by infusion pump. Only at 24 hours was postoperative pain in the paracetamol group less than in the ketamine group. However, there was neither significant difference nor side effects between hemodynamic changes in recovery and 2, 6, 12, and 24 hours after the surgery.
Ketamine has been used as a general anesthetic and analgesic for various pain conditions in the last few decades. Since Foster and Fagg reported the discovery of the NMDA receptor in 1987, ketamine has been used as a potentially antihyperglycemic agent due to its actions as a non-competitive NMDA receptor antagonist. However, given the adverse effects of its complications, the drug remains controversial (21).
The most blatant limitation in this study was the fact that the surgery should have been conducted by one surgeon, and with the same method, but it was not possible to do at this center.
5.1. Conclusions
The use of ketamine infusion pump is more effective than apotel infusion pump for controlling the postoperative pain in posterior spinal fusion surgery.