1. Background
Many chemical substances such as medicines, detergents, cleaning substances, bleaches, adhesives, and kerosene are used in households in developing areas, which endanger families' health, especially children (1). Children's behavior is implicitly involved in investigating the current situation as part of their everyday life. They play, try to open holders, imitate what adults do, put things in their mouths, pour harmful substances onto their skin, and disperse them into their eyes. In growing steps, by doing so, they are discovering new things. These behaviors play as dangerous actions that can cause physical or physiological harm to the child (2). One of the health problems caused by such behavior is poisoning, which is always a part of human life, and the causes change over time (3). Toxic substances are potentially harmful materials that can often be harmful to the human body by being intentionally or accidentally ingested, inhaled, or presented through the skin (4). Data on the non-fatal effects of child poisoning are not readily available at this time, but they are equally worried because these effects are widespread and can be a lifelong burden for young victims (5). The World Health Organization (WHO) found that about 3,45,814 people died of accidental or intentional poisoning worldwide in 2004, of whom 13% were below 20 years (6). Acute poisoning is exposure to a poison on one occasion or during a short period. In this regard, it has been reported that the high prevalence of acute poisoning among children, especially in Iran, is due to their curiosity about tasting and ingesting toxic substances, especially children under the age of five (7). The incidence of poisoning in children and adolescents is high, with peaks in children aged 1 to 7 years (8), which occur primarily in the home and home surroundings and can be avoided with primary preventative measures (9).
Poisoning causes have changed due to lifestyle changes and economic conditions (3). In developing countries, including Iran, unawareness, inadequate public knowledge, and lack of poison control centers are the leading causes of higher mortality and morbidity in these patients (10). In this regard, Haghighat et al. (7) reported that poisoning is one of the most common causes of morbidity and mortality in the pediatric emergency department, leading to high social and economic burdens, especially in low socioeconomic societies. Various symptoms and signs of poisoning have been observed in various studies, but the most common symptoms are diarrhea, sensory organ changes, fever, cough, mouth discharge, vomiting, impaired consciousness, blood pressure, and heart rate (11). Moreover, various factors such as family size, socioeconomic status, childcare system, and safe toxin storage are sociodemographic factors that can substantially impact the prevalence of poisoning (12). Recognizing risk factors can be beneficial to prevent poisoning. For this, keeping toxic substances out of the reach of children can reduce child poisonings (13) and increase child attention and care if the family is large (14).
2. Objectives
Given the above materials and specific socio-cultural in the underdeveloped province of Sistan and Baluchistan, Iran, the present study aimed to assess pediatric poisoning due to chemical substances and related symptoms and factors.
3. Patients and Methods
A research project entitled “A Study of Causes of Poisoning in Children Admitted to the Emergency Department of Teaching Hospital of Ali Ebne Abitalib in Zahedan, Iran” submitted to the Children and Adolescent Health Research Center, belongs to the Zahedan University of Medical Sciences, Zahedan, Iran that approved in 2019. The project was conducted as a retrospective study in 2020. Early in 2021, data was collected from the medical record that found about 636 poisoned children. Of these poisoned children, all children who were poisoned by chemical substances such as medicinal substances, bites or stings, toxins, detergents, pipe adhesive, and kerosene were considered for the present study. After evaluating information for each poisoned child, those with missed data and higher than 18 years of age were excluded from the study. Other types of poisoning, such as poisoning due to narcotics and their derivatives, were also excluded from the study, and finally, 292 cases were entered into the study.
3.1. Ethical Consideration
The study was approved by the Zahedan University of Medical Sciences committee. Then after study approval, researchers were prepared a standardized form to extract necessary information from the patients’ profiles. The form consisted of information about the demographic and socioeconomic factors of the children's household, the poisoning reason, symptoms and signs at the time of admission, and the outcome. Demographic and economic information was; parents’ education and occupation, the number of children in the household, age, gender. The symptoms and signs at the time of admission to the emergency department were also extracted from the profiles and were changes in eye pupil, respiratory system problems, blood pressure, heart rate. The clinical factors such as discharge status from the hospital, admission to the intensive care units, and intention of the poisoning were also extracted from the profiles.
3.2. Statistical Analysis
Data were analyzed using SPSS 18 (SPSS Inc, Chicago, Ill, USA), considering mean and SD for descriptive statistics and Pearson's chi-squared test for inferential statistics to assess the association between two specific categorical variables. The level of significance was considered 0.05.
4. Results
Of 292 children poisoned by chemical substances, 48.6% were girls. Table 1 shows a significant association between age and gender distribution (χ2 = 10.363, P = 0.006). Of 126 children aged younger than 5 years, 42.9% were girls. This trend was 41.1% and 62.4% in age groups of 5 - 10 years and > 10 years, respectively. Of the poisoned children, boys were more in number and in all age groups except the age group of > 10 years.
| Age Groups (y) | Sex | Total | χ2 | P | |
|---|---|---|---|---|---|
| Boy | Girl | ||||
| < 5 | 72 (57.1) | 54 (42.9) | 126 (100.0) | 10.363 | 0.006 |
| 5 - 10 | 43 (58.9) | 30 (41.1) | 73 (100.0) | ||
| > 10 | 35 (37.6) | 58 (62.4) | 93 (100.0) | ||
| Total | 150 (51.4) | 142 (48.6) | 292 (100.0) | ||
a Values are expressed as No. (%).
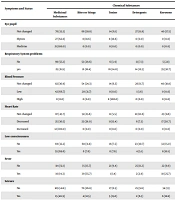
Table 2 shows that age (χ2 = 22.494, P = 0.013), self-poisoning (χ2 = 32.176, P < 0.001) had a significant association with the different types of chemical substances such that children in age groups < 5 and > 10 years mostly experienced poisoning by medicinal when children aged 5 - 10 years experienced bites or stings. Of 62 self-poisoning children, 62.9%, 16.13%, and 12.9% used medicinal toxins and kerosene, respectively. Of the six dead children, three, two, and one were due to kerosene, medicinal substances, and bites, respectively. Of those admitted to the ICU, 35.9%, 31.5%, and 13% were poisoned by medicinal substances, bites, and detergents, respectively. Of 84 children with two siblings, 48.8%, 31%, and 11.9% were poisoned by medicinal substances, bites, and kerosene substances, respectively. Of 55 poisoned children with fathers' jobs in governmental offices, most of them (45.5%) were poisoned by medicinal substances and about 30.9% by bites. Of 45 fathers with higher education, 40% had at least a child poisoned by medicinal, 28.9% had at least a child poisoned by bites substances. Of 71 mothers with governmental jobs, about 47.9%, 21.1%, and 14.1% had children poisoned by medicinal substances, bites, and kerosene, respectively. Furthermore, about 45.1%, 23.5%, and 15.7% of mothers with higher education had poisoned children with medicinal substances, bites, and kerosene, respectively.
| Symptoms and Status | Chemical Substances | Total | χ2 | P | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Medicinal Substances | Bites or Stings | Toxins | Detergents | Kerosene | Pipe Adhesive | |||||
| Eye pupil | 62.112 | < 0.001 | ||||||||
| Not changed | 76 (33.2) | 66 (28.8) | 14 (6.1) | 27 (11.8) | 40 (17.5) | 6 (2.6) | 229 (100.0) | |||
| Myosis | 27 (62.8) | 8 (18.6) | 8 (18.6) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 43 (100.0) | |||
| Medirias | 21 (100.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 21 (100.0) | |||
| Respiratory system problems | 74.319 | < 0.001 | ||||||||
| No | 99 (55.3) | 53 (29.6) | 6 (3.4) | 13 (7.3) | 5 (2.8) | 3 (1.7) | 179 (100.0) | |||
| yes | 25 (21.9) | 21 (18.4) | 16 (14.0) | 14 (12.3) | 35 (30.7) | 3 (2.6) | 114 (100.0) | |||
| Blood pressure | 134.109 | < 0.001 | ||||||||
| Not changed | 82 (36.9) | 54 (24.3) | 14 (6.3) | 26 (11.7) | 40 (18.0) | 6 (2.7) | 222 (100.0) | |||
| Low | 42 (66.7) | 20 (31.7) | 0 (0.0) | 1 (1.6) | 0 (0.0) | 0 (0.0) | 63 (100.0) | |||
| High | 0 (0.0) | 0 (0.0) | 8 (100.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 8 (100.0) | |||
| Heart rate | 31.219 | 0.001 | ||||||||
| Not changed | 87 (43.7) | 51 (25.6) | 11 (5.5) | 21 (10.6) | 23 (11.6) | 6 (3.0) | 199 (100.0) | |||
| Decreased | 25 (30.5) | 23 (28.0) | 11 (13.4) | 6 (7.3) | 17 (20.7) | 0 (0.0) | 82 (100.0) | |||
| Increased | 12 (100.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 0 (0.0) | 12 (100.0) | |||
| Low consciousness | 37.629 | < 0.001 | ||||||||
| No | 69 (32.2) | 68 (31.8) | 16 (7.5) | 23 (10.7) | 32 (15.0) | 6 (2.8) | 214 (100.0) | |||
| Yes | 55 (69.6) | 6 (7.6) | 6 (7.6) | 4 (5.1) | 8 (10.1) | 0 (0.0) | 79 (100.0) | |||
| Fever | 71.113 | < 0.001 | ||||||||
| No | 114 (51.1) | 35 (15.7) | 21 (9.4) | 25 (11.2) | 22 (9.9) | 6 (2.7) | 223 (100.0) | |||
| Yes | 10 (14.3) | 39 (55.7) | 1 (1.4) | 2 (2.9) | 18 (25.7) | 0 (0.0) | 70 (100.0) | |||
| Seizure | 7.405 | 0.192 | ||||||||
| No | 109 (41.8) | 70 (26.8) | 17 (6.5) | 25 (9.6) | 34 (13) | 6 (2.3) | 261 (100.0) | |||
| Yes | 15 (46.9) | 4 (12.5) | 5 (15.6) | 2 (6.3) | 6 (18.8) | 0 (0.0) | 32 (100.0) | |||
| Vomiting and nausea | 56.61 | < 0.001 | ||||||||
| No | 93 (47.4) | 65 (33.2) | 12 (6.1) | 13 (6.6) | 10 (5.1) | 3 (1.5) | 196 (100.0) | |||
| Yes | 31 (32.0) | 9 (9.3) | 10 (10.3) | 14 (14.4) | 30 (30.9) | 3 (3.1) | 97 (100.0) | |||
| SPO2 | 100.973 | < 0.001 | ||||||||
| No | 48 (35.8) | 67 (50.0) | 0 (0.0) | 6 (4.5) | 8 (6.0) | 5 (3.7) | 134 (100.0) | |||
| Yes | 76 (47.8) | 7 (4.4) | 22 (13.8) | 21 (13.2) | 32 (20.1) | 1 (0.6) | 159 (100.0) | |||
| Total | 124 (42.3) | 74 (25.3) | 22 (7.5) | 27 (9.2) | 40 (13.7) | 6 (2.0) | 293 (100.0) | |||
a Values are expressed as No. (%).
Of 43 myosis pupils, 62.8%, 18.6%, and 18.6% were due to medicinal, beating, and toxin, respectively. Of 21 poisoned children with medirias, all were due to medicinal substances. Of the children, 114 had respiratory system disorders (RSD), in which 21.9%, 18.4%, 14%, 12.3%, 30.7%, and 2.6% were due to medicinal substances, bites, toxins, detergents, kerosene, and pipe adhesive poisonings. Therefore, RSD was associated with chemical poisoning materials (χ2 = 74.319, P < 0.001). Of 63 children with low BP, 66.7%, 31.7%, and 1.6% were due to medicinal substances, bites, and detergents, respectively, and from six children with high BP, all were due to toxins (χ2 = 134.11, P < 0.001). Heart rate in 12 and 82 poisoned children increased and decreased respectively such that all increased children were due to medicinal and from those who had a decrease in HR, 30.5%, 28%, 13.4%, 7.3%, and 20.7% were due to medicinal substances, bites, toxins, detergents, and kerosene. Of the children, 79 had low consciousness, of whom 69.6% were due to medicinal substances, 70 had fever, of whom 55.7% were due to bites, 32 had seizures, of whom 46.9% and 18.8% were due to medicinal substances and kerosene, 97 had vomiting and nausea, of whom 32% and 30.9% were due to medicinal substances and kerosene. Moreover, of the children, 159 had low SPO2, of whom 47.8 %, 13.8%, and 20.1% were due to medicinal substances, toxins, and kerosene (Table 3).
| Variables and Groups | Chemical Substances | Total | χ2 | P | |||||
|---|---|---|---|---|---|---|---|---|---|
| Medicinal Substances | Bites | Toxins | Detergents | Kerosene | Pipe Adhesive | ||||
| Age groups (y) | 22.494 | 0.013 | |||||||
| < 5 | 48 (38.1) | 27 (21.4) | 10 (7.9) | 16 (12.7) | 22 (17.5) | 3 (2.4) | 126 (100.0) | ||
| 5 - 10 | 26 (35.1) | 29 (39.2) | 3 (4.1) | 5 (6.8) | 8 (10.8) | 3 (4.1) | 74 (100.0) | ||
| > 10 | 50 (53.8) | 18 (19.4) | 9 (9.7) | 6 (6.5) | 10 (10.8) | 0 (0.0) | 93 (100.0) | ||
| Sex | 6.372 | 0.272 | |||||||
| Boy | 57 (38.0) | 41 (27.3) | 12 (8.0) | 19 (12.7) | 18 (12.0) | 3 (2.0) | 150 (100.0) | ||
| Girl | 66 (46.5) | 33 (23.2) | 10 (7.0) | 8 (5.6) | 22 (15.5) | 3 (2.1) | 142 (100.0) | ||
| Discharge status from hospital | 14.066 | 0.17 | |||||||
| Good | 57 (42.5) | 37 (27.6) | 5 (3.7) | 14 (10.4) | 19 (14.2) | 2 (1.5) | 134 (100.0) | ||
| Satisfied | 65 (42.5) | 36 (23.5) | 17 (11.1) | 13 (8.5) | 18 (11.8) | 4 (2.6) | 153 (100.0) | ||
| Death | 2 (33.3) | 1 (16.7) | 0 (0.0) | 0 (0.0) | 3 (50.0) | 0 (0.0) | 6 (100.0) | ||
| ICU admission | 9.295 | 0.098 | |||||||
| No | 91 (45.3) | 45 (22.4) | 14 (7.0) | 15 (7.5) | 30 (14.9) | 6 (3.0) | 201 (100.0) | ||
| Yes | 33 (35.9) | 29 (31.5) | 8 (8.7) | 12 (13.0) | 10 (10.9) | 0 (0.0) | 92 (100.0) | ||
| Self poisoning | 32.176 | < 0.001 | |||||||
| No | 85 (36.8) | 73 (31.6) | 13 (5.6) | 22 (9.5) | 32 (13.9) | 6 (2.6) | 231 (100.0) | ||
| Yes | 39 (62.9) | 0 (0) | 10 (16.13) | 5 (8.1) | 8 (12.9) | 0 (0.0) | 62 (100.0) | ||
| No children in household | 18.116 | 0.053 | |||||||
| 1 | 53 (44.5) | 26 (21.8) | 7 (5.9) | 13 (10.9) | 15 (12.6) | 5 (4.2) | 119 (100.0) | ||
| 2 | 30 (33.3) | 22 (24.4) | 11 (12.2) | 11 (12.2) | 15 (16.7) | 1 (1.1) | 90 (100.0) | ||
| 3 | 41 (48.8) | 26 (31.0) | 4 (4.8) | 3 (3.6) | 10 (11.9) | 0 (0.0) | 84 (100.0) | ||
| Father occupation | 20.967 | 0.399 | |||||||
| Self job | 16 (35.6) | 8 (17.8) | 5 (11.1) | 6 (13.3) | 10 (22.2) | 0 (0.0) | 45 (100.0) | ||
| Worker | 23 (39.7) | 15 (25.9) | 4 (6.9) | 7 (12.1) | 8 (13.8) | 1 (1.7) | 58 (100.0) | ||
| Farmer | 26 (39.4) | 20 (30.3) | 4 (6.1) | 8 (12.1) | 8 (12.1) | 0 (0.0) | 66 (100.0) | ||
| Governmental job | 25 (45.5) | 17 (30.9) | 5 (9.1) | 0 (0.0) | 6 (10.9) | 2 (3.6) | 55 (100.0) | ||
| No governmental job | 34 (49.3) | 14 (20.3) | 4 (5.8) | 6 (8.7) | 8 (11.6) | 3 (4.3) | 69 (100.0) | ||
| Mother occupation | 12.485 | 0.642 | |||||||
| Housewife | 35 (49.3) | 18 (25.4) | 4 (5.6) | 8 (11.3) | 6 (8.5) | 0 (0.0) | 71 (100.0) | ||
| Governmental job | 34 (47.9) | 15 (21.1) | 6 (8.5) | 5 (7.0) | 10 (14.1) | 1 (1.4) | 71 (100.0) | ||
| Self job | 28 (36.4) | 20 (26.0) | 6 (7.8) | 8 (10.4) | 11 (14.3) | 4 (5.2) | 77 (100.0) | ||
| Ungovermental job | 27 (36.5) | 21 (28.4) | 6 (8.1) | 6 (8.1) | 13 (17.6) | 1 (1.4) | 74 (100.0) | ||
| Father education | 31.326 | 0.178 | |||||||
| Illiterate | 19 (40.4) | 11 (23.4) | 5 (10.6) | 4 (8.5) | 6 (12.8) | 2 (4.3) | 47 (100.0) | ||
| Primary (1 - 5) | 14 (25.9) | 22 (40.7) | 5 (9.3) | 3 (5.6) | 10 (18.5) | 0 (0.0) | 54 (100.0) | ||
| Secondary (6 - 8) | 25 (46.3) | 11 (20.4) | 2 (3.7) | 6 (11.1) | 9 (16.7) | 1 (1.9) | 54 (100.0) | ||
| High school (9 - 12) | 22 (44.0) | 9 (18.0) | 4 (8.0) | 5 (10.0) | 7 (14.0) | 3 (6.0) | 50 (100.0) | ||
| Diploma | 26 (60.5) | 8 (18.6) | 4 (9.3) | 3 (7.0) | 2 (4.7) | 0 (0.0) | 43 (100.0) | ||
| University degrees | 18 (40.0) | 13 (28.9) | 2 (4.4) | 6 (13.3) | 6 (13.3) | 0 (0.0) | 45 (100.0) | ||
| Mother education | 26.159 | 0.399 | |||||||
| Illiterate | 20 (43.5) | 16 (34.8) | 3 (6.5) | 1 (2.2) | 6 (13.0) | 0 (0.0) | 46 (100.0) | ||
| Primary (1 - 5) | 23 (47.9) | 13 (27.1) | 3 (6.3) | 4 (8.3) | 5 (10.4) | 0 (0.0) | 48 (100.0) | ||
| Secondary (6 - 8) | 27 (46.6) | 15 (25.9) | 5 (8.6) | 4 (6.9) | 7 (12.1) | 0 (0.0) | 58 (100.0) | ||
| High school (9 - 12) | 16 (44.4) | 6 (16.7) | 3 (8.3) | 5 (13.9) | 4 (11.1) | 2 (5.6) | 36 (100.0) | ||
| Diploma | 15 (27.8) | 12 (22.2) | 7 (13.0) | 7 (13.0) | 10 (18.5) | 3 (5.6) | 54 (100.0) | ||
| University degrees | 23 (45.1) | 12 (23.5) | 1 (2.0) | 6 (11.8) | 8 (15.7) | 1 (2.0) | 51 (100.0) | ||
The analysis revealed that poisonings due to medicinal items rose and fell over the years, with a peak in 2017 (70.7%) and 2020 (64.3%). Bites or stings had a decreasing trend over the years. Of 22 children poisoned by toxins, about 20.7% and 19.2% were in 2018 and 2016, respectively. Detergents had a constant trend overall but with fluctuations in the years peaked in 2018 (13.8%). Kerosene had a decreasing trend from 22.2% to 11.1% from 2014 to 2020, with a peak (22.2%) in 2014. Of six children poisoned by adhesives materials, two were poisoned in 2014, similar to 2016. Of 19 children poisoned in March, 36.8% and 31.6% were poisoned by toxins and kerosene, respectively. Of 29 children poisoned in April, 44.8% and 27.6% were due to medicinal substances and bites or stings, respectively. Of poisoned children in May, about 32.4% and 29.4% were due to bites or stings and medicinal substances, respectively. Of poisoned children in June, 47.4% and 33.3% were due to bites or stings and medicinal substances, respectively. Of 52 poisoned children in July, 46.2% and 30.80% were due to medicinal substances and bites or stings, respectively. Of 11 poisoned children in August, 54.5% and 27.30% were due to medicines and detergents, respectively. Of 13 children poisoned in September, 46.2% and 30.80% were poisoned by medicinal and kerosene, respectively. Of 11 poisoned children in October, 54.5% and 27.30% were due to medicinal substances and bites or stings, respectively. Of 12 poisoned children in November, 50% and 25.0% were due to medicinal substances and kerosene, respectively. Of 18 children poisoned in December, 61.1% and 22.2% were poisoned by medicinal substances and kerosene, respectively. Of 18 poisoned children in January, 50% and 16.7% were poisoned by medicinal substances and kerosene, respectively. Moreover, of 19 children poisoned in February, 57.9% were poisoned with medicinal substances and 10.5% with other materials except for toxins.
5. Discussion
Both haphazard and intentionally, poisonings are the leading causes of mortality and morbidity common in the pediatric population, highlighted in children younger than 5 years, particularly in boys (15). The present study revealed that children aged 5-10 years experienced poisoning with bites and stings when others were poisoned by medicinal substances. Boys were more when girls were increased among medicinal and self-poisonings. About 92 children were admitted to the PICU because of severe poison, who mainly were without siblings and had parents with non-governmental jobs and low education.
Azab et al. (16) assessed poisoned children and found, those younger than 6 years were more, about 11% were 6 - 12 years, and 37% were > 12 years. They also found that haphazard poisoning represented 68.5% of the ingestions; however, among adolescents, 84.1% of ingestions were self-poisonings. Lee et al. (17) led an investigation on poisoned children under 18 years and found that boys and young children were higher in number. Saikia et al. (9) investigated that of the poisoned children, about 77.8% were aged 1 - 5 years and 65.5% were boys. Vilaça et al. (18) found that 72.5% were < 4 years and 55% were boys. They also reported that of the accidental poisonings, about 90% occurred at home.
Tobaiqy et al. (19) revealed that most children in their study were aged 5 years or younger. Accidentally poisonings occurred in 56.5% of observed cases, in which 52.2% occurred in younger than 5-year-old children. Of 7.20% of deliberate, intentional poisonings, almost 92.8% occurred at home. All the results from the mentioned studies are somehow comparable with the results of the present study with a little difference in age group categorization, but with consensus in this fact that, overall, more poisoned children are boys or young. Nevertheless, self-poisoning was more in girls, especially in adolescents. Alghadeer et al. (4) found that medicinal items were the most common causes of poisoning, followed by chemical materials, more common in children under 2 years of age. In the present study, the medicinal items were one type of chemical materials, and the results were incomparable status. Azab et al. (16) found that the most frequent medicinal items were pain killers, anti-fever, and medicine for rheumatism in all age groups. In their study, the most common nonmedicinal substances were corrosives in preschool children and pesticides in adolescents. In their study, only 3% of the poisoned children died. Saikia et al. (9) found that more poisonings were accidentally due to ingested chemical substances that usually occurred at home (85.6%) and in surroundings (11.8%). Vilaça et al. (18) found that 82.7% of poisonings occurred via the oral ingestion route, of which 36.5% were due to medicinal substances and 29.4% were due to detergents. In their study, only one child died. Sunilkumar and Parvathy (15) considered poisonings by kerosene. They reported from other studies that kerosene was the commonest of the poisoning in Malaysia and Nigeria. Another study demonstrated that kerosene poisonings occurred accidentally (20).
Tobaiqy et al. (19) found that medicines such as paracetamol, anticonvulsants, and other central nervous system-acting medicines were the most common substances of poisoning in children. They also found that the most common route of poisoning was oral ingestion, and only one death was recorded.
Amorim et al. (21) analyzed poisoned children under 12 years old from 2012 to 2014 and found that more than half were due to chemical substances and bites or stings. In their study, accidental poisoning was 92.2% and mainly occurred at home. Of all the death cases, six were by chemicals and two by scorpion bites. Alghadeer et al. (4) reported that the main route of poisoning was oral. Among the chemicals materials, pesticide products were involved in 39.6% of the cases, followed by detergents items in about 25.9%. Muller and Desel (3) found that most intoxications with medications were due to substances affecting the central nervous system. In the study by Lee et al. (17), medicinal ingestion was the leading cause of poisoning, and pesticide was the most common nonmedicinal poison ingested. Sharma et al. (22) found that the most common substance for poisonings was organophosphorus, followed by bites, medicinal substances, and kerosene. Children can also get organophosphate poisoning by consuming contaminated food or water. The most common unintentional exposure routes are breathing and skin contact. The present study found that 14 (4.8%) of poisoned children accidentally (7 children) and intentionally (7 children) were due to organophosphate that all discharged from the hospital. Studies (23, 24) have reported that poisonings with organophosphate were more than other poisoning substances, whereas other studies (25, 26) reported a lower percentage of organophosphate poisoning cases. Kasiri et al. (27) found that the high incidence of pesticide poisoning was attributed to organophosphate (19.4%). Organophosphate compounds are consumed in most poisoning cases, usually used to commit suicide, as investigated in India (84.3%) (28).
Regarding symptoms and signs due to poisonings, Saikia et al. (9) found that 1.3% had diarrhea, 7.8% were in altered sensorium, 3.9% had fever, 10.5% had cough, 24.2% presented with excessive secretions from the mouth, 20.3% had vomiting without blood staining, and 7.8% had blood-stained vomiting was their chief complaint. Moreover, in their study, the mucosal injury was observed in 26.8% of the cases. However, Alghadeer et al. (4) reported that poisoned children were most asymptomatic. Sunilkumar and Parvathy (15) reported that the common symptoms in poisoned children were vomiting and nausea in 80.2%, coughing in 82.4%, fever in 69.2%, tachypnoea in 25.3%, restlessness in 23.1%, drowsiness in 12.1%, cyanosis in 1.1% and there were no symptoms in 17.6% of children. The present study showed that pupils changed due to medicinal substances, bites or stings and toxins, not by kerosene or detergents substances or pipe adhesive. RSD happened due to medicinal substances, bites, toxins, detergents, kerosene, and pipe adhesive. The blood pressure as a vital sign was due to medicinal, bitten, and detergent materials, and from those who had high blood pressure was due to toxins. Heart rate changes were due to medicinal substances, bites, toxins, detergents, and kerosene. Low consciousness was another vital sign, mostly was due to medicinal poisonings. In short, the other signs such as fever, seizures, vomiting, and nausea were due to bites, medicinal substances, and kerosene. Low SPO2 was due to medicinal toxins and kerosene. Different poisoning materials shared all the above signs, and perhaps it would be related to the age of the children and the dose of poisoned materials.
Dayasiri et al. (29) conducted a study to identify the risk factors of demographic and socioeconomic effects on poisonings and found that from accidental poisonings and among children aged 1 - 5 years, the majority were belonged to lower socioeconomic status (79.1%) and were from rural areas. They also reported that the most substantial risk factors were inadequate knowledge, employed mothers, lack of family support, and unsafe storage place to keep poisonous materials. Poisoning is a severe preventable health problem worldwide, especially in developing countries.
The present study revealed that most of the cases were discharged from the hospital with good or satisfactory status when only six children died due to medicinal substances, bites or stings, and kerosene. The same results were observed by Farag et al. (30) that most of the poisoned children were discharged with complete recovery, and Seif et al. (31) and Gheshlaghi et al. (32) found similar results. These studies reported that no fatalities were found during hospitality. This can be explained that most cases were mild, with an early arrival to the poisonings center, so that has been reported that early arrival is a reason for better outcomes (33).
Farag et al. (30) found that the number of poisoned children varied from one season to another, highest in summer and lowest in autumn. Agarwal et al. (34) and Sobeeh et al. (35) found similar results that the peak of poisoning was in summer can be referred to several factors such as cleaning houses with different detergents. Another reason could be more usage of pesticides due to the increasing presence of insects and pests in this season (36). Studies in Iran and Saudi Arabia showed the peak incidence of poisonings in autumn (32, 37). On the other hand, in a Turkish study, most cases were in spring (38). The present study showed that children poisoned by medicinal items approximately had the highest frequency in all months of the year. It is inferred from the present study and the other mentioned studies that kerosene is more frequent in the cold months, November and December.
A limitation of this study was that it was conducted in one emergency department, which cannot be a comprehensive picture of the pediatric poisoning trends.
5.1. Conclusions
The present study concluded that among the poisoned children, boys were more than girls and that self-poisoning was more in girls, especially at older ages. In medicinal substances and kerosene, girls were more than boys, more frequented by bites, stings, toxins, and detergents. All the symptoms and signs of poisoning were observed in medicinal substances and bites. Poisoned children by medicinal substances were high in all months of the year, kerosene was frequented more in the cold months, and detergent items and bites were more in summer. There is a need for further prospective studies to provide a clearer picture of the different aspects of poisoning and lead to preventive measures that are more comprehensive implementable and programs.