1. Background
Vertical root fracture (VRF) is the worst kind of longitudinal fracture and often leads to tooth extraction (1). VRF is often caused by dental treatment following placement of pins and screws (2). The main risk factors for VRF include excessive cleaning and forming of the root canal, application of excessive lateral and vertical forces while filling the root canal, loss of moisture in teeth without pulp, over-preparation of the post space, excessive exertion of pressure in placing the post, loss of tooth integrity due to trauma and decay, excessive occlusal force especially on restored teeth, and occlusion-induced centrifugal forces (3).
VRF in root canal treated teeth significantly reduces long-term prognosis and eventually leads to extraction of the tooth (4). The most common radiographic features of VRF are:
1) Destruction of the crescent-shaped bone that contains combined periapical and perilateral radiolucency and is located on one or either sides of the root;
2) Lateral periodontal radiolucency along the root;
3) Or radiolucency angled from the bone crest that terminates along the root.
The definitive diagnosis is only possible by direct observation of the fracture line with or without surgical intervention (5). To date, the two-dimensional digital and conventional intraoral radiography has been the most common imaging modality for VRF detection. Fracture lines are only visible when radiation beam passes through them in parallel, and VRF may be overlooked when the beam does not pass through the fracture line tangentially (6). Since the beam often makes an angle with the fracture line, repeated radiographs at different angles are required, which requires an increase in patient's dose. Hence, conventional radiographs are far from ideal for VRF (7). In early stages, VRFs are hairline fractures that do not displace adjacent pieces, and are hardly detectable in intraoral images, until development of the soft tissue surrounding the root pieces that separates them (8). Both digital and conventional imaging systems have shown poor sensitivity in VRF detection. This limitation arises from several factors, including superimposition of adjacent anatomic structures, beam not parallel to fracture line, and producing two-dimensional images from three-dimensional objects (9). CBCT has significantly greater detection sensitivity than intraoral systems (10). The presence of a solid or metallic structure (with high density) can often create artifacts that appear as radiopaque and radiolucent strips on the image that mimic root fractures or cover fracture regions (11).
The inability of conventional imaging techniques to accurately show VRF in a non-destructive way stresses the importance of the alternative advanced imaging techniques that facilitate VRF analysis. In recent years, cone-beam computed tomography (CBCT) has (12) shown better performance in detecting VRF compared to conventional intraoral radiography, although CBCT has been shown to have a higher level of radiation than conventional radiographic techniques (13).
Generally, significant amounts of strip-like artifacts in the region can reduce diagnostic accuracy of images, or even make them unusable (14-17). Various ways have been suggested for reducing artifacts in CBCT (18). The present study aims to investigate whether using artifact-reduction option with higher image resolution increases diagnostic accuracy in the presence of high density materials such as prefabricated posts or not.
2. Objectives
This study compares diagnostic power of CBCT with and without artifact-reduction option in detecting VRF in roots with casting posts. Investigating artifact-reduction option can be helpful in detecting fractures adjacent to metallic and Gutta-Percha posts, and eliminating artifacts in the jaw region, and better detection of the width and length of the surrounding bones and their actual structure.
3. Materials and Methods
3.1. Material Preparation
This study was cross-sectional. Direct observation of CBCT images was carried out by three observers in two different with and without artifact reduction technique modes, and data was recorded. A total of 62 extracted human premolars without root fracture were evaluated via direct observation and staining with methylene-blue. Given the study type, minimum sample size in fracture and non-fracture groups was determined as 31 per group (62 samples in total). These teeth had been extracted due to periodontal problems or orthodontic treatments. Teeth were non-randomly selected according to inclusion criteria. In the 31 teeth with fracture that were included, the vertical fracture line created by the Instron machine ascertained the presence of a fracture, and this was confirmed by methylene-blue staining. Absence of a fracture in the 31 samples without fracture was confirmed by methylene-blue staining. Teeth deemed with calcification in root treatment were replaced by other eligible samples. Samples with fracture breaking into two under Instron machine pressure were excluded, and only samples with non-displaced fractures were included.
3.2. Preparation of Samples
Trial group in the present in-vitro study consisted of 62 human premolars with no fracture. Samples were selected irrespective of the patient's age, gender, and reason for extraction. The extracted teeth were placed in the volatile disinfectant solution of 0.5% sodium hypochlorite (Golrang-Tehran-Iran) and their crowns were cut off from the cement-enamel junction (CEJ) using a micro-motor and metal disc to eliminate errors caused by enamel fracture (19). Then, all samples received root treatment and the root crowns were preflared by Gates Glidden No. 2 or 3 (Dentsply Maillefer, Ballaigues). All teeth received peripheral filing by 15 to 50 file (Dentsply Maillefer, Ballaigues. Switzerland) and the debris inside canals were removed by rinsing. After preparation, canals were filled by Gutta-Percha (Aria Dent, Tehran, Iran) and sealer (Dentsply Maillefer, Ballaigues. Switzerland). A week later, in preparation for the post space, all teeth were emptied by Pizzo No. 2 or 3 (Dentsply Maillefer, Ballaigues. Switzerland) to two-thirds of the root length. Periapical radiographic images confirmed suitability of the post spaces. Prefabricated bronze posts (Nordin, Chaily, Switzerland) were placed in the canals but were not cemented due to the likelihood of cement flow into the fracture line (19).
Each tooth was covered with a 2-3mm layer of red wax (Dentsply, DeTrey, Weybridge, UK), and mounted in separate blocks made from a mixture of gypsum and saw dust (to resemble the jaw trabeculation). This ensured absence of a gap in the root, easy removal of teeth from their blocks, and also avoided disintegration of pieces while creating fractures (8).
Vertical root fractures were created in 31 randomly selected teeth by an Instron machine (Zwcik/roell, GmbH & Co. KG, Germany). This system creates an increasing compressive force on the pin until the fracture sound is heard. Then, this force is immediately cut off according to the diagram on the system monitor. Samples from fracture group that split into two under Instron machine force were excluded and replaced by new eligible samples. As the control group, no fracture was created in the other 31 teeth.
During the study, all samples were kept in a hydrated medium, and removed only during construction of posts, fracturing roots, and preparing images.
3.3. Imaging Method
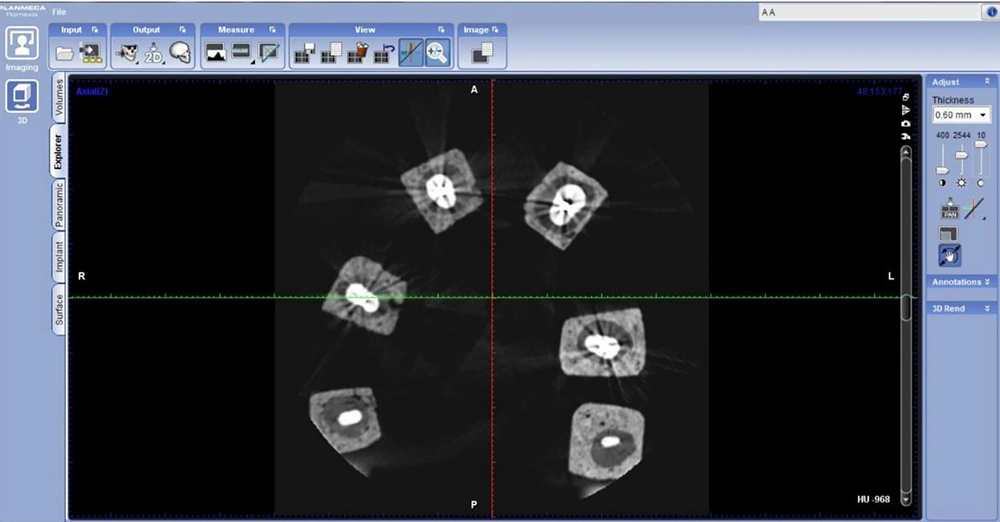
In preparation for CBCT images, the teeth were randomly divided into 11 groups consisting of 10 of six and one of two teeth. Six gypsum and sawdust blocks were placed on a sample similar to the jaw arch that was made from Putti on the chinrest of CBCT device (Promax3d, planmeca. Helsinki. Finland) and images were taken in two modes, with mild artifact reduction (AR) and without AR (Figure 1).
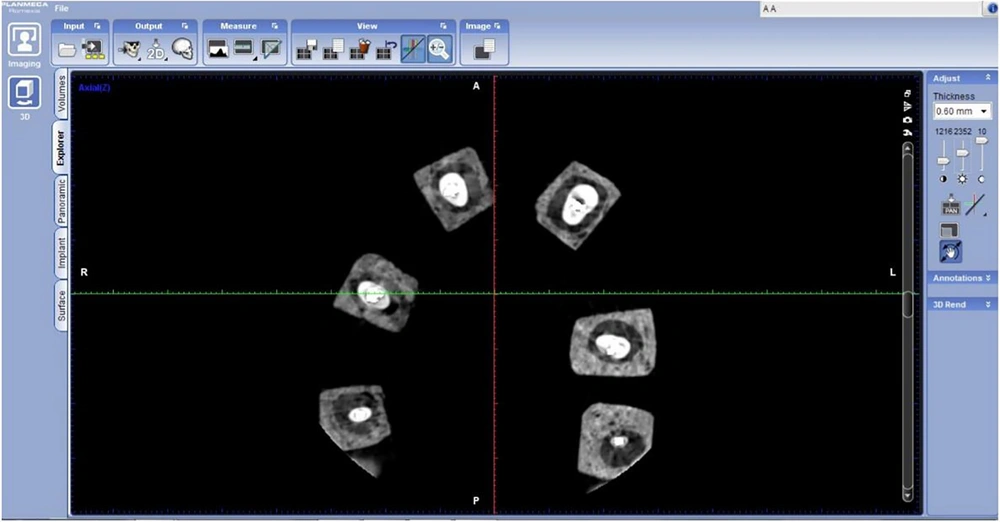
In promax3d system, AR has three options of low, mild and high. A total of 22 exposures were taken (Figure 2). Imaging was carried out in 8 × 8 cm2 field of view (FOV) at a voltage of 74 kvp, with slice thickness of 1mm, voxel size 0.15, and 12 mA, which was adjusted for each sample by the system. Axial, coronal and sagittal planes were analyzed.
3.4. Data Collection
Three maxillofacial radiologists who had no knowledge of the root groups assessed images for presence or absence of root fracture. All observers were blinded regarding all aspects of data gathering. They were able to adjust contrast and brightness of images when necessary with no time restriction. All images were reviewed on LG FLATRON W175s with a resolution of 1440 × 90 pixel, and Planmeca Romexis Viwer 3.0.1.R software (Helsinki, Finland). CBCT images were assessed in axial, coronal, and sagittal planes). Observers recorded their answers regarding probability of VRF as a five-option scale as follows:
1) Definitely no fracture
2) There is probably no fracture
3) Uncertainty about presence or absence of a fracture
4) There is probably a fracture
5) There is definitely a fracture
Observers recorded their detection according to this scale.
To apply the gold standard, teeth were removed from gypsum sawdust blocks, and examined for fracture by 1% methylene-blue staining and rinsing.
With a fracture present, the dye penetrated in the line of fracture was visible as a dark blue line on the surface of the root. Thus, presence or absence of vertical root fracture in samples was confirmed.
3.5. Analysis
To calculate the intra-observer coefficient, observers viewed the scanned images and re-identified fractures according to the mentioned five-option scale two weeks later, without knowledge about fractured samples.
Data were analyzed in SPSS for Windows version 16 (SPSS Inc., Released 2007, Chicago, IL, USA)
At first, the observers' diagnostic performance was determined separately (versus the gold standard) in each voxel size and accordingly, diagnostic indices were calculated. These indices included sensitivity, specificity, positive predictive value and negative predictive value. As the observers’ remarks on fracture were based on a five-option scale (including definite or probable presence or absence of fracture, as mentioned before), diagnostic indices could be calculated in two situations; first, considering definite cases only, and second, considering definite and probable cases together. Therefore, the indices included definite sensitivity (number of teeth diagnosed as definite fracture divided by the number of fractured teeth, based on gold standard), total sensitivity (number of teeth diagnosed as definite or probable fracture divided by the number of fractured teeth based on gold standard), definite specificity (number of teeth diagnosed as definite no-fracture divided by the number of intact teeth based on gold standard), total specificity (number of teeth diagnosed as definite or probable no-fracture divided by the number of intact teeth based on gold standard), definite positive predictive value (fractured teeth diagnosed as definite fracture divided by the number of teeth diagnosed as definite fracture), total positive predictive value (number of fractured teeth diagnosed as definite or probable fracture divided by the number of teeth diagnosed as definite or probable fracture), definite negative predictive value (number of intact teeth diagnosed as definite no-fracture divided by the number of teeth diagnosed as definite no-fracture), total negative predictive value (number of intact teeth diagnosed as definite or probable no-fracture divided by the number of teeth diagnosed as definite or probable no-fracture).
To compare the diagnostic efficacy of CBCT with AR versus CBCT without AR technique option, all diagnostic indices (including definite and total sensitivity, specificity and positive and negative predictive values) were compared between two techniques separately. For this purpose, each index was calculated when the radiologist used AR technique or did not; then two groups (each group included results of three radiologists evaluations, with and without AR option) were compared (using U Mann-Whitney test). Also, inter-observer and intra-observer reliabilities were assessed using agreement coefficient.
Definite VRF was considered when the radiolucent line extended from the external border of the tooth to pulp chamber in all three axial, coronal, and sagittal planes. While probable VRF was considered when the line could not be detected in any of the three multiplanar images (axial, coronal or sagittal) or detected in just one of them.
Scientific honesty in assessing the results was observed, care was taken in proper use of equipment, and consideration was given to the welfare of the study team to avoid their discomfort.
4. Results
Because of using Instron device, fractures could happen in all directions (not only linear or regular). As we mentioned before, we included only 31 teeth with vertical fractures and the other ones were excluded. A total of 11 images were prepared from 62 teeth, and assessed by three maxillofacial radiologists. Half of the samples were with vertical root fractures (VRF) (n = 31), and half without, which were randomly arranged in 10 blocks of 6 and one block of 2. The performance of the three observers in regard to presence and absence of artifact reduction is mentioned in Table 1.
| Detection indices/Observer and option | Definite specificity, % | Total specificity, % | Definite sensitivity, % | Total sensitivity, % | Definite negative predictive value, % | Total negative predictive value, % | Definite positive predictive value, % | Total positive predictive value, % |
|---|---|---|---|---|---|---|---|---|
| First observer/without AR | 54.83 | 93.54 | 74.2 | 83.9 | 94.44 | 85.3 | 95.83 | 92.85 |
| Second observer/without AR | 77.41 | 83.9 | 45.2 | 71 | 77.41 | 74.28 | 100 | 84.61 |
| Third observer/without AR | 38.7 | 87.1 | 54.83 | 67.74 | 85.71 | 79.4 | 100 | 84 |
| First observer/with AR | 58.1 | 80.7 | 71 | 80.7 | 90 | 80.64 | 91.66 | 80.64 |
| Second observer/with AR | 83.9 | 83.9 | 41.93 | 64.51 | 81.25 | 72.22 | 92.85 | 83.33 |
| Third observer/with AR | 54.83 | 80.7 | 61.3 | 71 | 100 | 75.75 | 100 | 84.61 |
Abbreviation: AR, artifact reduction
4.1. Sensitivity
Mean definite sensitivity was 58.07 ± 14.77 without AR option and 58.06 ± 14.78 with AR option, and Mann-Whitney showed no significant difference between two modes (P = 0.997).
Mean total sensitivity was 74.2 ± 8.56 without AR option, and 72.06 ± 8.15 with AR option, and Mann-Whitney showed no significant difference between two modes (P = 0.825) (Table 2).
| Without AR | With AR | |
|---|---|---|
| Definite sensitivity | 58.07 ± 14.77 | 58.06 ± 14.78 |
| Total sensitivity | 74.2 ± 8.56 | 72.06 ± 8.15 |
Abbreviations: AR, artifact reduction; SD, standard deviation
aValues are expressed as mean ± SD.
4.2. Specificity
Mean definite specificity was 56.96 ± 19.44 without AR option and 65.6 ± 15.93 with AR option, and Mann-Whitney showed no significant difference between these two groups (P = 0.840).
Mean total specificity was 88.16 ± 4.88 without AR option and 81.76 ± 1.84 with AR option, and Mann-Whitney showed no significant difference between these two groups (P = 0.184) (Table 3)
| Without AR | With AR | |
|---|---|---|
| Definite specificity | 56.96 ± 19.44 | 65.6 ± 15.93 |
| Total specificity | 88.16 ± 4.88 | 81.76 ± 1.84 |
Abbreviations: AR, artifact reduction; SD, standard deviation
aValues are expressed as mean ± SD.
4.3. Positive Predictive Value
Mean definite positive predictive value was 98.6 ± 2.42 without AR option, and 94.8 ± 4.54 with AR option, and Mann-Whitney showed no significant difference between them (P = 0.200).
Mean total positive predictive value was 87.13 ± 4.91 without AR option, and 82.83 ± 2.04 with AR option, and again Mann-Whitney showed no significant difference between them (P = 0.105) (Table 4).
| Without AR | With AR | |
|---|---|---|
| Definite positive predictive value | 98.6 ± 2.42 | 94.8 ± 4.54 |
| Total positive predictive value | 87.13 ± 4.91 | 82.83 ± 2.04 |
Abbreviations: AR, artifact reduction; SD, standard deviation
aValues are expressed as mean ± SD.
4.4. Negative Predictive Value
Mean definite negative predictive value was 85.83 ± 8.5 without AR option, and 90.41 ± 9.4 with AR option, and Mann-Whitney showed no significant difference between them (P = 0.875). Also, mean total negative predictive value was 79.6 ± 5.5 without AR option, and 76.16 ± 4.21 with AR option, and Mann-Whitney showed no significant difference between these values (P = 0.738) (Table 5).
| Without AR | With AR | |
|---|---|---|
| Definite negative predictive value | 85.83 ± 8.5 | 90.41 ± 9.4 |
| Total negative predictive value | 79.6 ± 5.5 | 76.16 ± 4.21 |
Abbreviations: AR, artifact reduction; SD, standard deviation
aValues are expressed as mean ± SD.
Generally, Mann-Whitney test was used to compare with and without AR options, which showed no significant difference between these two modes in any of the detection indices (including definite and total detection sensitivity, definite and total detection specificity, definite and total positive predictive values, and definite and total negative predictive values) (all Ps > 0.05).
4.5. Reliability
The intra-observer reliability was assessed using weighted kappa coefficient. They were 0.4, 0.55, and 0.45 for three radiologists (mean weighted kappa equal to 0.47) when they did not use AR option, whereas, they were 0.6, 0.7, and 0.4 (mean weighted kappa equal to 0.57) when radiologists used AR option. No significant difference was found between different AR modes.
Mean inter-observer reliability coefficient (weighted kappa) was 0.50 with AR option and 0.51 without AR option, which were both moderate, with no significant difference between them. The inter-observer reliability coefficient was poor.
5. Discussion
Various studies have reported low sensitivity for conventional radiographic VRF detection (25% - 47%) (20). Software capabilities in digital radiography have not been able to enhance this sensitivity (18). CBCT superiority over other imaging modalities in detection of VRF has been demonstrated. There are fewer artifacts in CBCT compared to CT system. However, these artifacts still occur in the presence of radiopaque materials such as metal post that could cause false positive and negative results (19). Given the limitations in previous studies, the few reports provided, and the effect of a post on VRF detection accuracy, the present study investigated the effect of presence and absence of AR option in Promax CBCT imaging system (Planmeca, Helsinki, Finland) on VRF detection accuracy.
In the present study, observers reported the results according to a 5-point scale; therefore, the results were in the form of definite and total sensitivity and specificity. In definite sensitivity and specificity, observers had a definite view about presence or absence of a fracture. However, in total sensitivity and specificity, possible detection and definite cases were considered. Positive predictive value shows probability of being ill when the result is positive, and it is found from the ratio of actual positive over sum of positive and false, and in the present study its value was not significantly different between with and without AR modes. Also, negative predictive value shows probability of not being ill when the result is negative, and it is found from the ratio of actual negative over sum of negative and false, and its value was not significantly different between with and without AR modes. However, given that predictive value is dependent on the prevalence of disease, which was randomly chosen in the present study (50%), it is possible that predictive value is not much reliable.
High sensitivity means actual positive values compared to actual positives detected plus false negatives, and recognition of most lesions or problems, which are VRFs in this case. In the present study, total detection sensitivity was 74.2 ± 8.56 without AR option, and 72.06 ± 8.15 with AR option, which was higher in without AR option mode, but not statistically significantly. In a study conducted by Melo et al. (16), total detection sensitivity and specificity reduced in the presence of a post, but this reduction was not significant. In a study carried out by Costa et al. (19), CBCT image was accurate in detecting horizontal root fracture without posts. The VRF detection sensitivity and specificity reduced by presence of post.
The low levels of sensitivity and specificity in the present study appear to have been caused by the presence of a bronze post in the root canal.
With no AR option, the sensitivity found in the present study was less than that in a study performed by Bechara et al. (20), which could have been affected by the observers’ detection power or the mount materials (In Bechara et al. study, samples were mounted on a bovine rip bone, and in the present study puttii was used). Moreover, in the study conducted by Bechara et al., broken samples were glued together by methyl-methacrylate adhesive, which could have affected detection sensitivity and specificity, and the teeth had received root canal treatment and had Gutta-Percha. On the other hand, in the present study, root-treated teeth with prefabricated posts were used, which could be the reason for lower sensitivity and specificity. This requires further studies. In the present study, the overall sensitivity was higher without AR option compared to the with AR option, but the difference was not significant. Whereas, in the study carried out by Bechara et al., sensitivity was significantly higher without AR option in Promax system. The higher detection system specificity suggests fewer false positive cases. In the present study, total detection specificity was 88.16 ± 4.88 without AR, and 81.76 with AR, so it was higher without AR but not significantly. These values were also lower compared to studies that did not use a post. This was due to beam hardening caused by high density metallic posts and the scattering caused by radiopaque materials and their induced artifacts. Artifacts can appear as lines or twilight areas around the filling materials similar to fracture lines, and thus cause false positive and negative results (21). Specificity was higher in the present study compared to a study performed by Bechara et al., when AR option was used in Promax system, but without AR option the result was close to that found in study conducted by Bechara et al. without much difference. This may have been due to the difference between the two studies in the way fracture was created, since in a study conducted by Bechara et al., fractures were created manually using a hammer, which may have created greater gaps between separated pieces of tooth after fracture. Moreover, in their study, detection of fracture was carried out in teeth with filling and without a post, which seems to be the cause of the difference in the results. Estrela et al. (22) investigated the effect of type of posts on the amount of artifact created, and reported the most amount of artifacts in castings of gold alloys and silver alloy and the least in carbon fiber posts. In the present study, bronze (copper and zinc alloy) posts were used, which was not investigated in the study conducted by Estrela et al. However, this shows that the amount of artifact is affected by the post material, which can also affect the detection accuracy. According to a study conducted by Ferreira et al. (23), detection sensitivity and positive predictive value are higher in fiber resin posts than titanium posts. Therefore, the post material could be considered as one of the reasons for lower detection accuracy in the present study. According to a study performed by Ozer et al. (24), the gap between VRF pieces affects detection accuracy of CBCT. Ozer et al. studied the detection accuracy of CBCT and digital radiography in detecting VRF, and concluded that CBCT is more accurate than digital radiography in detecting all VRF thicknesses, and VRF was most detectable when the gap between fracture pieces was 0.4 mm. Hence, non-displaced and hairline fractures can affect interpretation of the results. Mild fractures with no displacement of fracture pieces are usually not detectable with intraoral radiography, and sometimes fracture lines cannot be seen even in CBCT scans (23).Given the intra-observer results, indicating low reliability coefficient (first, second, and third observer: 40%, 55%, and 45% without AR option, and 60%, 70% and 40% with AR); such low coefficients seem to have been caused by metallic artifact in teeth with posts.
In conclusion, according to the results, sensitivity, specificity, and positive and negative predictive values in detecting root fracture in teeth with prefabricated posts were affected by the use or non-use of AR option, but with no significant difference between them. This could have been due to the presence of artifacts produced by posts. According to previous studies, this option can only be used for better resolution, but it has no effect on the detection accuracy. Moreover, the poor inter and intra-observer reliability agreement coefficients suggests that these poor coefficients are caused by the presence of posts in the canal and metallic artifact.