1. Background
Antibiotics inhibit the growth of or destroy microorganisms and have completely changed the present-day practice of medicine. Even lethal infections are readily treatable by new-generation antibiotics that have even improved other medical therapies like cancer chemotherapy and organ transplantation in children (1). Given the widespread therapeutic applications of antibiotics, their usage has now spread everywhere, leading to antibiotic resistance. So, it is critical to consider strict stewardship towards antibiotic use.
The easiest method to investigate prescription patterns is to carry out an audit on prescriptions to recognize commonly used antibiotics and drugs among various populations and identify polypharmacy as a serious emerging threat in the community. Auditing also reveals the use or misuse of medications with special reference to antibiotics (2). In addition, auditing helps in formulating and modifying treatment guidelines according to the needs of the population under study in order to restrict antibiotic over-prescription by physicians and nail antibiotic stewardship. It also helps to provide an evidence-based approach to judicious antimicrobial use (3).
In the present study, we aimed to audit the prescriptions of the referral patients coming to the outpatient pediatrics department of a tertiary care teaching hospital in Indore, wherein prescriptions were analyzed using pre-set parameters.
2. Objectives
To audit the patterns and quality of antibiotic prescription for children in the outpatient department (OPD).
3. Methods
This cross-sectional observational study was conducted in a tertiary care teaching hospital in central India from April 2018 to May 2019. The study was approved by the Institutional Ethics Committee, and written informed consent was obtained from participants’ parents.
One-thousand prescription sheets of pediatric patients aged 1 month to 15 years attended the outpatient department during the study period were selected. The health care providers writing the prescriptions were unaware of the audit. The first author collected prescription sheets and gathered patients’ demographics and drug-related information.
A pre-validated list of 12 essential parameters (Table 1) was used to assess the quality of the prescriptions audited. A pilot study was done to validate the selected parameters and the feasibility of the study, after which the audit was finalized and performed.
| Serial No. | Audit Parameters |
|---|---|
| 1 | Patient Name |
| 2 | Age |
| 3 | Date |
| 4 | OPD number |
| 5 | Diagnosis |
| 6 | Dose of drug |
| 7 | Route of drug administration |
| 8 | Frequency of drug administration |
| 9 | Duration of drug usage |
| 10 | Generic name |
| 11 | Legibility |
| 12 | Signature of the doctor |
One score was given to each correctly written parameter, delivering a total score of 12. The quality of prescriptions was categorized as either poor (score 0 - 4), average (score 5 - 8), or good (score 9 - 12).
The prescribing indicators of the world health organization (WHO) were used to analyze antibiotic prescribing patterns and five important areas regarding the appropriate use of medicines (4). The indicators with their reference values (5-7) included:
- Indicator 1: The average number of medicines prescribed per encounter (ref value < 2).
- Indicator 2: The percentage of medicines prescribed by generic name (ref value = 100%).
- Indicator 3: The percentage of encounters with an antibiotic prescribed (ref value < 30%).
- Indicator 4: The percentage of encounters with an injection prescribed (ref value < 20%).
- Indicator 5: The percentage of medicines prescribed from a list of essential medicines (ref value = 100%).
The indicator 3 was used to analyze antibiotic prescription by health care providers using the following formula.
% encounters = No. of clinical encounters with one or more antibiotics prescribed / Total number or encounters
Based on the qualification of prescribers, all audited prescriptions were categorized based on being ordered by Postgraduates in Pediatrics, MBBS, and AYUSH (an acronym for Ayurveda, Yoga and naturopathy, Unani, Siddha, and Homeopathy) incorporating six health fields, which is practiced in India and some of its neighboring Asian countries.
Data were entered in an excel sheet, and descriptive statistics and open-source Epidata software was used for statistical analyses.
4. Results
This prospective observational study was conducted from April 2018 to May 2019. During the study period, a total of 1000 prescription sheets were analyzed. Out of 1000 prescriptions, 830 (83%) were ordered by postgraduates in pediatrics, 130 (13%) by MBBS, and 40 (4%) by AYUSH doctors.
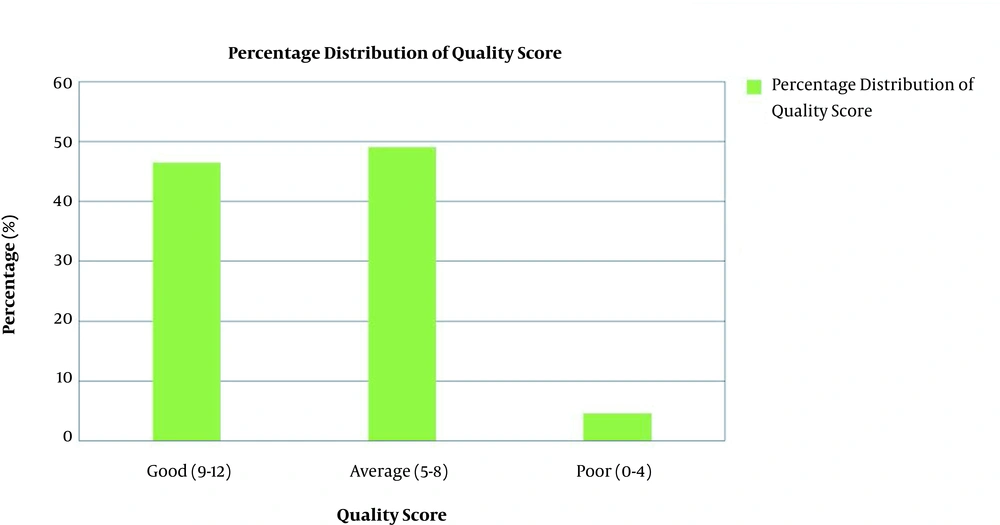
The distribution of audit parameters has been shown in Table 2. Out of 1000 prescriptions, 490 (49%), 464 (46.4%), and 46 (4.6%) had average, good, and poor qualities, respectively (Figure 1).
| Audit Parameters | Yes | No |
|---|---|---|
| The patient’s name | 98.1 | 1.9 |
| Age | 88 | 12 |
| Date | 87.2 | 12.8 |
| Opd number | 58.1 | 41.9 |
| Diagnosis | 27 | 73 |
| Dose | 89 | 11 |
| Route | 68 | 32 |
| Frequency of drug | 90.3 | 9.7 |
| Duration of drug | 86.4 | 13.6 |
| Legibility | 54.2 | 45.8 |
| Generic name | 29.3 | 70.7 |
| Signature of the doctor | 62 | 38 |
a Values are expressed as percentage.
According to the WHO core prescribing indicators (Table 3), the average number of the medicines prescribed per encounter was 3.5 (ref value < 2), indicating polypharmacy. The percent of the medicines prescribed by generic names was 27.3% (ref value 100%). The ratio of encounters with an antibiotic prescribed was 65% (ref value < 30%), and the percentage of encounters with an injection prescribed was 6% (ref value < 20%). Finally, the rate of prescription from a list of essential medicines was 15% (ref value 100%).
| WHO Core Prescribing Indicators | Reference Value | Observed Value |
|---|---|---|
| The average number of medicines prescribed per counter | < 2 | 3.5 |
| The percentage of medicines prescribed by generic names | 100 | 27.3 |
| The percentage of encounters with an antibiotic prescribed | < 30 | 65 |
| The percentage of encounters with an injection prescribed | < 20 | 6 |
| The percentage of medicines prescribed from a list of essential medicines | 100 | 15 |
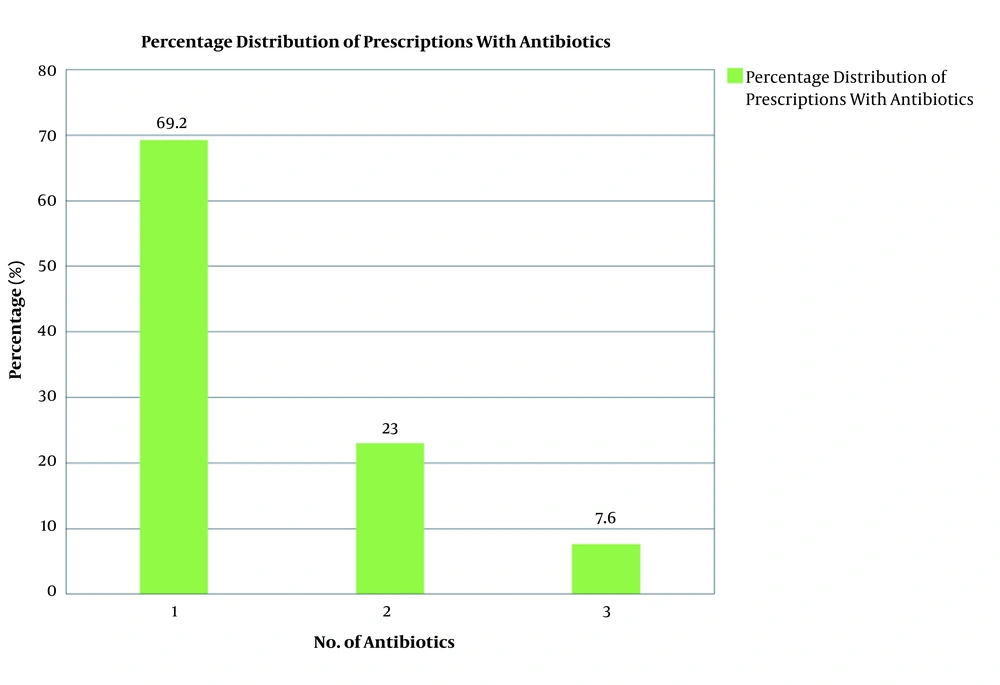
Out of 1000 prescriptions, 650 (65%) had one or more antibiotics prescribed, of which 450 (69.2%) had one antibiotic, 150 (23%) had two antibiotics, and 50 (7.6%) had three antibiotics (Figure 2).
Regarding the qualifications of the prescribes of encounters with an antibiotic prescribed, 63% were postgraduates in pediatrics, 70% were MBBS physicians, and 90% were AYUSH doctors (ref value < 30%).
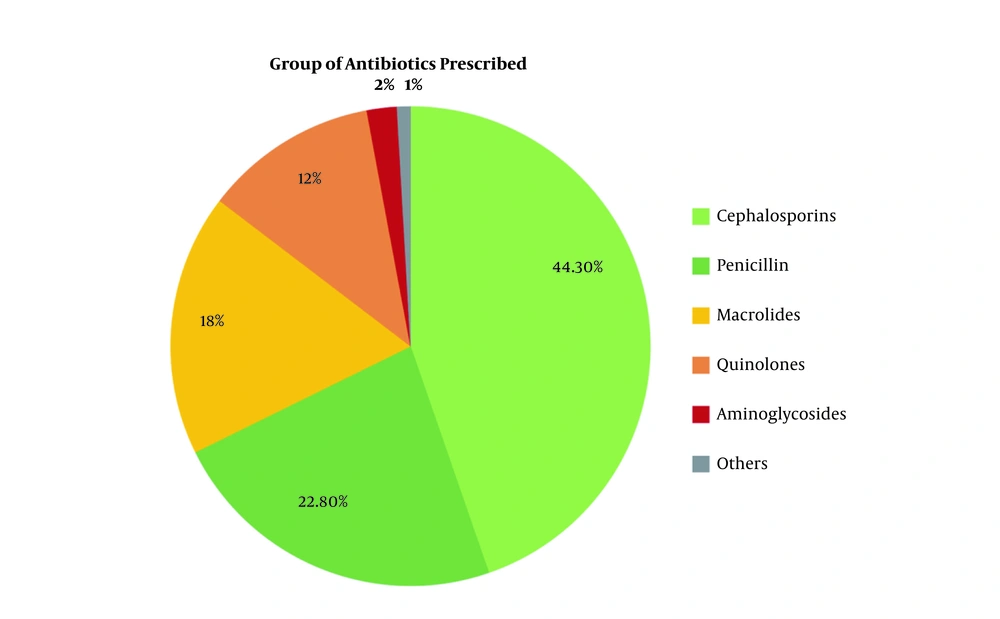
Out of 1000 prescriptions, antibiotics were prescribed in 650. The total number of antibiotics used in these prescriptions was 900, indicating the prescription of more than one antibiotic in many sheets. Cephalosporins (443, 44.3%) were the most common group of the antibiotics prescribed, followed by penicillin (228, 22.8%) (Figure 3).
5. Discussion
In this observational study, we assessed the quality of antibiotic prescribing patterns and prescription writing by child healthcare providers. The quality of the prescriptions was found to be good (46.4%) and average (49%) in most encounters, while it was poor at 4.6%. The average number of the medicines prescribed per encounter was 3.5, indicating polypharmacy. Only 27.3% of the medicines had been prescribed by their generic names. The percentage of encounters with an antibiotic prescribed was 65%, indicating a very high antibiotic usage by the health care providers.
Neha et al. (8), in their prescription-audit study involving 100 in-patient prescriptions, found nine prescriptions as semi-rational and 91 as rational. This high rate of rational drug usage was likely to be a result of regular update and supervision by the teaching faculties of the department. In a similar audit study by Ahsan et al. (9) based on WHO core indicators, authors reported the use of 4.02 drugs per prescription with 39.01% of the prescriptions containing antibiotics. They also reported that 79.2% of the prescriptions had medications from the list of essential drugs, which was higher than that of our study. This variation in the results of different studies may be explained by different levels of awareness among drug prescribers, the availability of various medicines in a specific area, and differences in the epidemiology of diseases in different regions.
Our study showed that 65% of the audited prescriptions contained antibiotics. The use of more than one antibiotic was relatively common (23 and 7.6% for two and three antibiotics, respectively). Harshal N Pise et al. (2015), in a study in Maharashtra (10), reported that 60.6% (110/182) of audited prescriptions contained antibiotics, with most of them containing two antibiotics (48.58%, n = 77/182). The excessive and simultaneous prescription of more than two antibiotics in a single sheet by outdoor patients necessitates the need for developing and following rational antibiotic prescription policies.
In our study, cephalosporins (44.3%) were the most common group of the prescribed antibiotics, followed by penicillin (22.8%). A study by Hussain et al. (11) in rural health care centers showed the use of penicillin in 31.7% of prescriptions, followed by quinolones and cephalosporins. This difference can be attributed to variations in the populations studied, the number of prescriptions audited, and the prescriber groups’ qualifications. Differences in prescribing patterns can also be attributed to variations in the availability of drugs in local markets, as well as the policies of medical representatives.
Many antibiotics in our study were prescribed by MBBS and AYUSH doctors, who are the first point of contact for many sick children. So, it is important to consider training courses, regular updates, and timely feedback by competent agencies for these practitioners. Our observations also revealed that outpatient training at the postgraduate level was effective in decreasing the indiscriminate use of medicines, especially antibiotics.
The major limitation of our study was that the analysis was confined to a particular geographic region and the duration of the study was only one year. As the study was performed at a single public sector teaching hospital, most of the prescriptions were for the children of the economically poor class of the society.
5.1. Conclusion
There is room for the improvement of prescription writing quality. Antibiotic prescription by health care providers, especially AYUSH doctors, needs to be supervised, given that many of these practitioners intend to prescribe antibiotics. Auditing prescriptions over a longer period of time and in different regions will produce better-quality data which can pave the path for formulating effective policies to establish antibiotic stewardship.
5.2. Recommendations
- Developing antibiotic stewardship programs at various levels of health care is the need of the hour.
- Periodic prescription audits should be regularly conducted by competent authorities to ensure rational antibiotic use.